A Conservative Esthetic Alternative to Full-Coverage Crowns
Abstract:
Porcelain veneers have long been a popular restorative option that have evolved into a well-accepted treatment that can be fabricated in various ways. Onlays are another common treatment modality used in contemporary dentistry to restore large areas of decay and to replace old restorations. With the availability of newer high-strength materials such as lithium disilicate and processing technologies like CAD/CAM and heat pressing, dental professionals are now able to produce highly esthetic, high-strength restorations that blend seamlessly with the natural dentition while also withstanding posterior occlusal forces. This has resulted in innovative methods of providing minimally invasive dentistry. One such approach is a combination restoration which, as demonstrated in this case report, can be used as an alternative to coverage crowns to restore damaged posterior teeth.
In contemporary restorative dentistry, there are several ways for clinicians to enhance the shape, color, or position of teeth, and, moreover, various materials and processing methods are available to fabricate restorations. Choices include veneers, onlays, and a restorative technique that combines the former two options and is described in the case presented.
Veneers
One of the most utilized options for achieving lasting esthetic correction has been the porcelain veneer. Porcelain veneers have been used for various indications, including the restoration of teeth that are intrinsically or extrinsically discolored, teeth that require slight occlusal adjustment, and those that are fractured, traumatized, and/or worn. Depending on the severity of the discoloration or deformity, the veneer preparation will be more or less aggressive. Sometimes the preparation will extend around the entire tooth for what is considered a full veneer or 3/4 veneer, but most commonly the preparation is for a facial veneer, as veneers are rarely indicated for placement beyond bicuspids.
Having been available for more than 35 years, veneers have transitioned from being brittle structures with high failure rates to a well-accepted treatment that can be fabricated in a number of ways.1 First generations of veneers were made from materials that proved clinically unacceptable, including large-particle composites, methyl methacrylate, and shell veneering systems. In 1975, porcelain bonding was developed and, subsequently, feldspathic porcelain became the material of choice.2 By 1983, the dental profession had discovered the benefits of bonding porcelain to etched enamel, and this method became the standard of care due to the strength and clinical longevity lent to veneers by the simple change in bonding procedure.3,4
Today’s veneers are fabricated either from advanced formulations of ceramic material—including leucite-reinforced feldspathic porcelain and lithium disilicate—or composites with very small particles like microhybrids and nanohybrids. Composite veneers can be fabricated directly or indirectly, depending on the indication. Direct veneering is accomplished by carefully layering and light-curing composites. However, fabricating the restorations indirectly through heat pressing results in restorations that demonstrate exceptional characteristics, exhibiting wear resistance similar to enamel, wear compatibility with the opposing dentition, marginal integrity, good proximal contacts, excellent esthetics, and sufficient strength for the posterior portion of the mouth.5
Ceramics have gained popularity due to advances in material science. No all-ceramic veneering system is indicated for all clinical situations, but the most commonly used material for high-strength, esthetic restorations in recent years has been lithium disilicate due to its mechanical characteristics and optimal translucency. Translucency equates to heightened esthetics, which is the primary reason for choosing all-ceramic restorations.6 Ceramic veneers can be computer-assisted design/computer-assisted manufacture (CAD/CAM)-milled and sintered from blocks, or heat-pressed from ingots. Milled veneers are generally indicated for areas where lower occlusal forces are expected, because they are weaker than their pressed counterparts (approximately 360 MPa for milled restorations versus 400 MPa for pressed restorations).7 However, the pressed restorations can be used even in the posterior region. Whether milled or pressed, all-ceramic veneers contribute to marginal integrity, low marginal discoloration, low failure rates, and optimal esthetics,8 with the only drawback seeming to be a lower wear compatibility with the opposing teeth.9
Onlays
Another restorative modality is the onlay, which is used in contemporary dentistry to restore large areas of decay. Onlays are also used to replace old restorations, whether they are defective amalgam fillings, old cast-gold onlays, porcelain fused to metal (PFM), or fabricated from some other material. As with veneers, the aggressiveness of the preparation design depends largely on the severity of the damage to the tooth being restored.
Onlay restorations have been documented extensively since the late 1800s. Materials used for their fabrication have primarily been gold, porcelain, and composites. Gold was the material used most often for onlays until the 1980s, when a swift rise in the price of gold made large gold restorations uneconomical.10 The enduring use of gold for onlay procedures can be attributed to its ease of manipulation,11 excellent adaptation, superior marginal fit, and clinical longevity. The drawbacks of gold are expense and the fact that it is not tooth-colored; therefore, it is a less desired option by today’s esthetically conscious patients.10
Composites are also commonly used in contemporary dentistry to form onlays, although this was once a contraindication for these materials. First-generation composites lacked adequate mechanical properties and wear resistance to be suitable for onlay restorations,12 demonstrating high rates of attrition, abrasion wear, marginal degradation, polymerization shrinkage, and poor adhesion. Newer-generation composites reflect the improved material science that overcame many of the problems of early composites, offering higher filler-to-matrix ratios that enhanced the mechanical properties.13 The ability to limit preparation design and use better refractory die and heat-press processing technologies also greatly improved these restorations by providing improved marginal integrity, adhesion, strength, and esthetics.14,15
Ceramic onlays may be CAD/CAM-milled or heat pressed. Like other all-ceramic restorations, they have seen a dramatic improvement during the years of their clinical use due to material science improvements. Ceramics formulated with feldspathic porcelain, mica-filled glass, leucite-reinforced ceramics, or lithium disilicate are all used in today’s metal-free restorations with high success rates.16 The improved ceramics in onlay restorations allow conservative preparation designs similar to those that can be achieved with other materials and restorations. These ceramics produce restorations that are highly translucent—and, therefore, highly esthetic—and that have excellent marginal integrity and enhanced proximal contacts, demonstrate minimal wear, and do not fracture or abrade opposing teeth.17
Combination Approach
Traditionally, if a patient requires restorative work in the posterior region, conventional thought has been to treatment plan full-coverage restorations, such as crowns. The trend in recent years has been “minimally invasive” dentistry, which means preserving as much tooth structure as possible whenever feasible. This inherently signifies moving away from procedures, such as crown placement, that require destruction of sound enamel and dentin if other, less invasive options are available and will be equally effective. One technique originally developed to veneer the facial of posterior teeth and combine an occlusal onlay was first published by one of the present authors (REG) nearly 20 years ago. The technique used feldspathic porcelain and, according to Goldstein, it never caught on mainly because of fear of fracture in the posterior with the then-available materials and bonding techniques.18
With the availability of newer high-strength materials like lithium disilicate and processing technologies like CAD/CAM and heat pressing, dental professionals are now able to offer patients highly esthetic, high-strength restorations that not only blend seamlessly with the natural dentition, but that also can withstand even posterior occlusal forces. As a result, these restorative materials can be used in innovative ways to provide the minimally invasive dentistry that today’s patients demand.
One such approach is a veneer-onlay combination restoration. Generally a monolithic structure fabricated from lithium disilicate, this restoration is a hybrid of an onlay with an extended buccal veneer surface for use in bicuspid regions where there is mostly enamel to bond to. The authors fabricate onlays from feldspathic porcelain, especially if the anterior teeth will likewise be veneered with feldspathic porcelain. In the authors’ experience, there has been a less than 1% failure rate annually when this type of restoration is fabricated for bicuspids if sufficient enamel is present for bonding. Additionally, thus far, there has not been a single documented restoration failure for molars fabricated from monolithic lithium disilicate (IPS e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com), even when bonded to dentin. This restorative option requires a much less invasive preparation than a full-coverage crown but provides the same structural benefits.19 Simultaneously, with the components of an onlay and veneer, a combination restoration enhances the strength and esthetics of the remaining tooth.20 For patients presenting with wear, decay, or occlusal problems in posterior teeth, this treatment option will be less invasive, more readily repairable, less technique-sensitive to attain adequate bonding, and will leave more sound tooth structure remaining if further treatment is required in the future.
The following case demonstrates how these combination restorations can be used as an alternative to full-coverage crowns to restore damaged posterior teeth.
Case Presentation
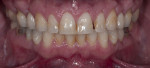
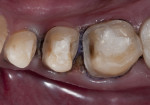
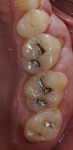
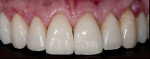
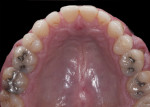
The patient presented with several primary concerns, chief among them being mainly esthetics. He did not like the color, size, or shape of his teeth (Figure 1) and wished to have the diastemas closed between teeth Nos. 10 and 11. He was also concerned about what he called the “volume” of his smile and wanted to widen his arch form to have a fuller smile. During the dental examination, it was determined the patient had mild incisal and occlusal wear and mild generalized recession, with localized moderate recession on maxillary first molars. Most of his posterior teeth had small to medium amalgam restorations with recurrent caries. There were also PFM restorations on teeth Nos. 18 and 29. All the maxillary anterior teeth and several mandibular anterior teeth had interproximal composite restorations that were discolored.
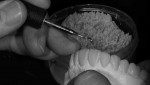
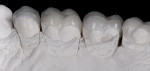
A design wax-up was completed to a new form based on the patient’s desires and the Adobe® Photoshop Smile Design technique21 (Figure 2). The plan was to slightly open or restore vertical dimension for several reasons: 1) to restore the missing cusp height from wear; 2) to avoid increasing the overbite and overjet relationship; and 3) to create restorative space to minimize the amount of tooth structure removal for restoration and ideal esthetics. From the design wax-up, clear matrices were fabricated and used to create a bonded functional esthetic prototype (BFEP)22 out of a special injectable composite (Reveal™, BISCO Inc., www.bisco.com), with the new tooth form, color, and increased vertical dimension (Figure 3). The increased vertical dimension of occlusion would create additional posterior interocclusal space for restorative purposes. The patient wore the BFEP for 3 months to verify esthetic acceptance and functional tolerance prior to irreversible tooth alteration. With this technique, which involves interimly restoring the case with composite, it is possible to then treat the case segmentally, if necessary.
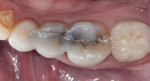
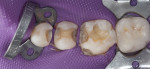
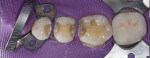
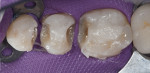
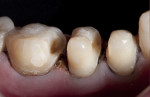
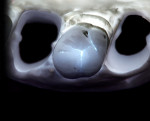
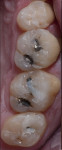
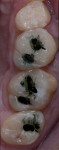
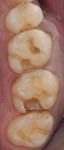
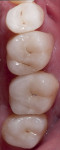
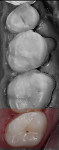
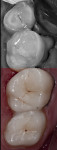
During the preparation appointment, preparations were done through the bonded composite based on first creating enough space for the minimal thickness of the chosen material, then managing the esthetic desires, and then removing old restorative material and any caries that may be present. A decision must be made as to whether it is necessary to “block out” a defect or undercut with composite (Figure 4 through Figure 7), and at a minimum the dentin is sealed. After transillumination was performed to diagnose crack lines, preparations were finalized with the primary goal of minimizing healthy tooth structure removal (Figure 8 and Figure 9). If significant areas of dentin are exposed during final preparation the dentin would be resealed. Impressions are made either conventionally or digitally, and then temporary restorations are fabricated using standard techniques with a bis-acryl material. It is important to note that a separator must be used on the tooth so the bis-acryl does not bond to the active bonding surface on the sealed dentin. A small area in the center of the tooth can be left without the separator so that the bis-acryl will bond to the “spot,” which is referred to as reverse spot bonding.
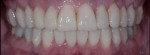
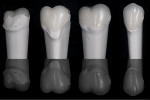
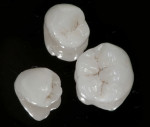
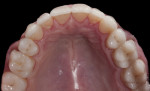
The laboratory then fabricated the combination restorations (Figure 10 through Figure 14) from the material of choice. The authors typically use e.max on molars due to its impressive success track record, but occasionally feldspathic porcelain is chosen—especially if there is still appreciable enamel on the tooth and bicuspids are being treated along with anterior porcelain veneers. The authors still prefer total-etch using a 4th generation adhesive, but there is promising short-term data on the so-called “universal” adhesives, which can be used in a “self-etch” mode. Figure 15 through Figure 29 show the maxillary arch esthetically and functionally restored with anterior porcelain veneers and posterior porcelain combination restorations.
Conclusion
In modern dentistry, materials and fabrication processes have advanced to a point where there is little that can’t be accomplished restoratively, even in the posterior region. Both chairside and through the laboratory, highly esthetic, high-strength restorations are becoming more cost-effective and are able to be more quickly fabricated. The veneer-onlay combination restoration is a good example of how dentistry has applied current science to clinical situations to provide patients with better dentistry, following the industry trends of minimally invasive and highly esthetic restorations.
About the Authors
Edward A. McLaren, DDS, MDC
Professor
Founder and Director
UCLA Post Graduate Esthetics
Director
UCLA Center for Esthetic Dentistry
Founder and Director
UCLA Master Dental Ceramist Program
UCLA School of Dentistry
Los Angeles, California
Private Practice limited to Prosthodontics and Esthetic Dentistry
Los Angeles, California
Johan Figueira, DDS
Faculty, UCLA Center for Esthetic Dentistry
UCLA School of Dentistry,
Los Angeles, California
Ronald E. Goldstein, DDS
Clinical Professor of Oral Rehabilitation
College of Dental Medicine
Georgia Regents University
Augusta, Georgia
Adjunct Clinical Professor of Prosthodontics
Henry M. Goldman School of Dental Medicine
Boston University
Boston, Massachusetts
Adjunct Professor of Restorative Dentistry
University of Texas Health Science Center
San Antonio, Texas
Private Practice
Goldstein, Garber, and Salama
Atlanta, Georgia
References
1. Larson, TD. 25 years of veneering: what have we learned? Northwest Dent. 2003;82(4):35-39.
2. Rochette AL. A ceramic restoration bonded by etched enamel and resin for fractured incisors. J Prosthet Dent. 1975;33(3):287-293.
3. Calamia, JR. Etched porcelain facial veneers: a new treatment modality based on scientific and clinical evidence. NY J Dent. 1983;53(6):255-259.
4. Calamia JR. Clinical evaluation of etched porcelain veneers. Am J Dent. 1989;2(1):9-15.
5. Touati B, Aidan N. Second generation laboratory composite resins for indirect restorations. J Esthet Dent. 1997;9(3):108-118.
6. Heffernan MJ, Aquilino SA, Diaz-Arnold AM, et al. Relative translucency of six all-ceramic systems. Part I: core materials. J Prosthet Dent. 2002;88(1):4-9.
7. Ivoclar Vivadent. IPS e.max Scientific Report: Vol. 1 2001-2011. https://www.ivoclarvivadent.us/en/ips-emax-scientific-report. Accessed March 16, 2015.
8. Christensen GJ, Christensen RP. Clinical observations of porcelain veneers: a three-year report. J Esthet Dent. 1991;3(5):174-179.
9. Suputtamongkol K, Anusavice KJ, Suchatampong C, et al. Clinical performance and wear characteristics of veneered lithia-disilicate-based ceramic crowns. Dent Mat. 2008;24(5):667-673.
10. Powers JM, Sakaguchi RL. Craig’s Restorative Dental Materials. 12th ed. St. Louis, MO: Mosby Elsevier; 2006.
11. Wolf BH, Walter MH, Boening KW, Schmidt AE. Margin quality of titanium and high-gold inlays and onlays—a clinical study. Dent Mater. 1998;14(5):370-374.
12. Asmussen E. Clinical relevance of physical, chemical, and bonding properties of composite resins. Oper Dent. 1985;10(2):61-73.
13. Miara P. Aesthetic guidelines for second-generation indirect inlay and onlay composite restorations. Pract Periodontics Aesthet Dent. 1998;10(4):423-431.
14. Baratieri LN, Ritter AV, Perdigão J, Felippe LA. Direct posterior composite resin restorations: current concepts for the technique. Pract Periodontics Aesthet Dent. 1998;10(7):875-886.
15. Robbins JW, Fasbinder DJ, Burgess JO. Fundamentals of Operative Dentistry: A Contemporary Approach. Chicago, IL: Quintessence Publishing; 1996.
16. Della Bonna A, Kelly JR. The clinical success of all-ceramic restorations. J Am Dent Assoc. 2008;139 suppl:8S-13S.
17. Ozyoney G, Yon Koglu F, Tagtekin D, Hayran O. The efficacy of glass-ceramic onlays in the restoration of morphologically compromised and endodontically treated molars. Int J Prosthodont. 2013;26(3):230-234.
18. Goldstein R. Etched porcelain restorations: veneers and inlays/onlays. In: Esthetics in Dentistry. 2nd ed. Vol 1. Hamilton, Ontario, Canada: B.C. Decker Inc.; 1998.
19. Chun YH, Raffelt C, Pfeiffer H, et al. Restoring strength of incisors with veneers and full ceramic crowns. J Adhes Dent. 2010;12(1):45-54.
20. Meyer A Jr, Cardoso LC, Araujo E, Baratieri LN. Ceramic inlays and onlays: clinical procedures for predictable results. J Esthet Restor Dent. 2003;15(6):338-351.
21. McLaren EA, Culp L. Smile Analysis: The Photoshop Smile Design Technique: Part 1. Journal of Cosmetic Dentistry. 2013;29(1):94-108.
22. McLaren EA. The Bonded Functional Esthetic Prototype: Part 2. Inside Dentistry. 2013:9(5)84-92.