Use of a Resin-Modified Glass-Ionomer (RMGI) Liner in Conservative Direct Treatment of Deep Caries
Abstract:
Liners and bases are a class of dental materials that provide added protection for the health and well-being of a tooth being restored. They help prevent postoperative sensitivity resulting from an incomplete dentinal seal. Some practitioners use them, while others choose not to. In this case report, a resin-modified glass-ionomer (RMGI) liner was utilized in deep restorations on premolars that had old, existing amalgam restorations and were experiencing microleakage and sensitivity problems. The materials and technique used allowed for conservative treatment while delivering an esthetic and functionally pleasing result.
Among clinicians who use dental liners and bases when restoring a tooth, there is a considerable range of opinions and practices. Anecdotally, the author has observed practitioners who opt to place a liner under nearly every posterior restoration, believing that it is simple insurance against hypersensitivity and recurrent decay. Recent research has questioned this practice, finding that a resin-modified glass-ionomer (RMGI) liner did not reduce postoperative sensitivity for moderate-depth Class I and II restorations.1 However, the study did not examine the effect of liners on deeper restorations or the considerable amount of existing evidence on that topic that supports their use.
This article will explore the rationale behind the use of liners/bases, the materials currently available, and the data in favor of them, as well as present a case in which a liner was utilized in the treatment of deep recurrent caries. Although liners may not be necessary in every restoration, data shows that they can be very effective in cases where their use is warranted.
Why Use a Liner?
There are a variety of views and approaches when it comes to either using or not using dental liners and bases for tooth restoration. A clinician’s decision is often made based on the depth of the restoration and the proximity to the pulp. If no liner or base is used on larger, deeper restorations, patients might sometimes experience postoperative sensitivity due to pulpal inflammation, and restorations can exhibit microleakage and stress fractures over time. Prevention of postoperative sensitivity is one of the most notable reasons why dentists use liners, as its occurrence not only impacts a patient’s quality of life but can also adversely affect his or her judgment of the dentist’s skill. Liners can also be used to manage the stress put on the tooth due to polymerization shrinkage of composite materials, as their low modulus can help distribute forces more evenly along the walls of a preparation.2
A simple protocol to follow can be based on the size and depth of the restoration. For shallow to normal restorations, a base or liner is usually not needed if proper bonding techniques are followed. Often, a simple flowable composite is placed first and used more as an “adaptive” initial composite layer. When exercising this option, the dentist must ensure that the field remains free of contamination during application of both the adhesive and the flowable. The use of the flowable as a liner actually relies on the adhesive as the desensitizing agent; therefore, if the bonding step is not performed correctly the restoration will be vulnerable to the same sensitivity as it would be if no liner were used at all. Despite this caveat, flowable materials have the advantages of good adaptation, ease of injection, and a wide variety of shade choices, which is important when esthetics are a high priority.3
Deeper, larger restorations with recurrent decay typically require some form of proper liner or base. When there is a true pulp exposure, bioactive products, ie, those that have the capacity to interact with living tissue or systems, can be considered. These are placed directly over the exposure to stimulate secondary dentin growth. For many years calcium hydroxide was used for pulp capping. This material protects the pulp from thermal insult and stimulates the formation of new dentin. Calcium hydroxide, however, has been declining in popularity since at least the mid-1990s,4 as this material will dissolve if exposed to leakage; therefore, clinicians often opt for an alternative liner material. Resin bioactive products (eg, TheraCal LC®, BISCO, Inc., www.bisco.com; Pro-Root® MTA, DENTSPLY Tulsa Dental Specialties, www.tulsadentalspecialties.com) are often considered as a liner in pulp exposure cases, as they provide immediate bond and sealing properties. These resin-modified bioactive products contain calcium silicate and may be considered a new generation of liners called resin-modified calcium silicates (RMCSs). Their significant calcium release creates an alkaline environment stimulating hydroxyl-apatite and secondary dentin formation within affected tissues.5,6
For deeper restorations that are close to the pulp but where no pulp is exposed, an RMGI liner is a primary option. These materials are dimensionally very stable, they bond to dentin, and release fluoride. They also reduce stress on the tooth and can inhibit microleakage. Glass-ionomer (GI) and RMGI liners are perhaps what many dentists envision first when they consider using a liner. Published research has demonstrated a variety of positive results for RMGI liners, and opinion leaders have echoed their approval.3,7 In one study comparing Class I restorations lined with an RMGI liner and dentin adhesive versus dentin adhesive alone, severity and frequency of sensitivity was found to be less in the RMGI group at both 24 hours and seven days,8 a critical time period for the patient’s judgment of the comfort of the restoration.
RMGI liner has also been shown to be an effective tool to combat microleakage,9-18 which is one of the most frequently occurring problems for a restoration. Microleakage can lead not only to postoperative sensitivity, but also marginal discoloration and recurrent caries, as well as periodontal disease, which can eventually necessitate endodontic treatment.19
The following case demonstrates the use of an RMGI liner in deep restorations on teeth that had already been suffering from microleakage and sensitivity.
Case Presentation
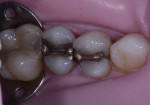
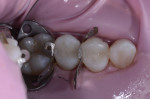
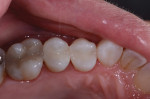
The patient, a 52-year-old woman, presented with sensitive amalgam restorations on two premolars (Figure 1). She stated the amalgams had been placed when she was a teenager, and she reported sensitivity to cold on both teeth, as well as biting pain on the first premolar. Examination revealed a crack on the mesial aspect of the first premolar as well as gray staining and generalized microleakage around both restorations. While an indirect restoration may have been a possibility for the second premolar, it was determined that both teeth could be treated with direct restorations. The patient agreed to this course of treatment due to both time and cost advantages.
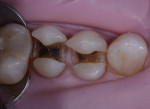
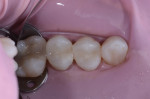
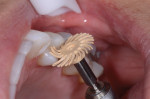
The patient was anesthetized with Septocaine® (Septodont, www.septodontusa.com), and a rubber dam was placed. A Zeiss medical microscope (Zeiss, www.zeiss.com) was used to aid vision during the procedure. An A-dec electric handpiece (A-dec Inc., us.a-dec.com) and a diamond bur were used to remove the amalgam restorations (Figure 2). Stain and affected dentin were removed as much as possible, leaving preparations that reached nearly to the pulpal floor. The preparations were cleaned and dried, with the surfaces left slightly moist. A glass-ionomer liner/base (Vitrebond™ Plus Light Cure Glass Ionomer Liner/Base, 3M ESPE, www.3MESPE.com) was dispensed onto a mixing pad and the paste and liquid components were mixed together for 15 seconds until they reached a smooth consistency and glossy appearance (Figure 3). (Author note: GC Fuji LINING™ LC [GC America, Inc., www.gcamerica.com] would also have been an appropriate choice for this case.) The liner/base material was applied to the deepest areas of the dentinal floor and kept short of the mesial and distal gingival cavosurface margins. The liner was then light-cured for 20 seconds.
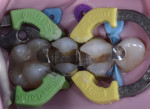
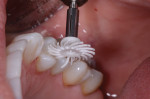
A matrix system (Triodent Sectional Matrix System, Triodent, www.triodent.com) was placed around the teeth, and total etching was performed with a 35% phosphoric acid solution (Ultra-Etch®, Ultradent Products, Inc., www.ultradent.com) (Figure 4). Universal adhesive (Scotchbond™ Universal Adhesive, 3M ESPE) was scrubbed into the preparations for 20 seconds, and excess adhesive was removed with a dry microtip. The preparations were then air-dried for 15 seconds until there was no movement of the adhesive, and the teeth were light-cured for 10 seconds (Figure 5).
A layer of flowable restorative (Filtek™ Supreme Ultra Flowable Restorative, 3M ESPE) in an A3 opaque shade was then placed in the bottom of the preparations to block out the appearance of the dark dentin (Figure 6). The layer of flowable composite was cured, and a “ramp style” build-up was then performed with layers of packable restorative. Composite was placed first on the buccal wall and light-cured (Figure 7); this was followed with another layer on the lingual wall (Figure 8). Separate curing of the buccal and lingual layers helped reduce the c-factor, which can be an issue if the layers are cured in bulk.20
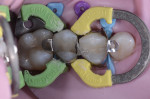
To begin basic contouring, the matrix rings and wedges were removed but bands were left in place to protect the adjacent teeth (Figure 9). The bands were removed after basic contouring (Figure 10). The rubber dam was then removed, and the occlusion was checked. Final finishing and polishing was completed with finishing and polishing wheels (Sof-Lex™, 3M ESPE), progressing from beige to white (Figure 11 and Figure 12).
The final results were highly esthetic and comfortable restorations (Figure 13). At her 4-week follow-up appointment the patient reported that she had no sensitivity and the bite felt great. The materials and technique used in this case allowed the teeth to be treated conservatively while still delivering a patient-pleasing result.
Discussion and Conclusion
In the case presented, the depth of the preparations as well as the pre-existing sensitivity were both strong indicators of a need for a liner. While there was no pulp exposure, the restorations were deeper than average and had recurrent decay. Although the long-term success of the treatment will only be seen with time, the use of an RMGI liner provided the assurance of extended fluoride release and protection against microleakage. The availability of a reliable treatment to protect against sensitivity and microleakage contributed to the decision to restore this case conservatively with direct restorations and an RMGI liner. These benefits, combined with the fact that the patient reported no sensitivity at follow-up, are signs that bode well for this treatment modality in the future.
This case demonstrates a successful outcome using a simple and predictable clinical workflow. While dental treatments and procedures are never completely predictable, clinicians should strive to have a protocol in place that provides an evidence-based guideline for effective decision-making when it comes to liners and bases.
Disclosure
The author has no financial affiliation with any of the products mentioned in this article.
About the Author
John F. Weston, DDS
Owner/Director, Scripps Center for Dental Care,
La Jolla, California
References
1. Strober B, Veitz-Keenan A, Barna JA, et al. Effectiveness of a resin-modified glass ionomer liner in reducing hypersensitivity in posterior restorations: a study from the practitioners engaged in applied research and learning network. J Am Dent Assoc. 2013;144(8):886-897.
2. Tolidis K, Nobecourt A, Randall RC. Effect of a resin-modified glass ionomer liner on volumetric polymerization shrinkage of various composites. Dent Mater. 1998;14(6):417-423.
3. Christensen GJ. Preventing postoperative tooth sensitivity in class I, II and V restorations. J Am Dent Assoc. 2002;133(2):229-231.
4. Weiner RS, Weiner LK, Kugel G. Teaching the use of bases and liners: a survey of North American dental schools. J Am Dent Assoc. 1996;127(11):1640-1645.
5. Colon P, Bronnec F, Grosgogeat B, Pradelle-Plasse N. Interactions between a calcium silicate cement (Biodentine) and its environment [abstract]. J Dent Res. 2010;89(spec iss B). Abstract 401.
6. Gandolfi MG, Suh B, Taddei P, et al. Chemical-physical properties of TheraCal pulp-capping material [abstract]. J Dent Res. 2011;90(spec iss A). Abstract 2521.
7. Christensen GJ. Should;resin-based composite dominate restorative dentistry today? J Am Dent Assoc. 2010;141(12):1490-1493.
8. Akpata ES, Sadiq W. Post-operative sensitivity in glass-ionomer versus adhesive resin-lined posterior composites. Am J Dent. 2001;14(1):34-38.
9. Holtan JR, Nystrom GP, Douglas WH, Phelps RA 2nd. Microleakage and marginal placement of a glass-ionomer liner. Quintessence Int. 1990;21(2):117-122.
10. Sidhu SK, Henderson LJ. In vitro marginal leakage of cervical composite restorations lined with a light-cured glass ionomer. Oper Dent. 1992;17(1):7-12.
11. Tsunekawa M, Usami Y, Iwaku M, et al. A new light-activated adhesive cavity liner: an in vitro bond strength and microleakage study. Dent Mater. 1992;8(5):296-298.
12. Wieczkowski G Jr, Yu XY, Joynt RB, Davis EL. Microleakage evaluation in amalgam restorations used with bases. J Esthet Dent. 1992;4(2):37-40.
13. Youngson CC, Holguin SM. Early in vitro marginal microleakage associated with different lining materials under Class II amalgam restorations. Eur J Prosthodont Restor Dent. 1992;1(2):73-77.
14. Robchinsky J, Donly KJ. A comparison of glass-ionomer cement and calcium hydroxide liners in amalgam restorations. Int J Periodontics Restorative Dent. 1993;13(4):378-383.
15. Mason PN, Ferrari M. In vivo evaluation of glass-ionomer cement adhesion to dentin. Quintessence Int. 1994;25(7):499-504.
16. Marchiori S, Baratieri LN, de Andrada MA, et al. The use of liners under amalgam restorations: an in vitro study on marginal leakage. Quintessence Int. 1998;29(10):637-642.
17. Howdle MD, Fox K, Youngson CC. An in vitro study of coronal microleakage around bonded amalgam coronal-radicular cores in endodontically treated molar teeth. Quintessence Int. 2002;33(1):22-29.
18. Wibowo G, Stockton L. Microleakage of Class II composite restorations. Am J Dent. 2001;14(3):177-185.
19. Murray PE, About I, Franquin JC, et al. Restorative pulpal and repair responses. J Am Dent Assoc. 2001;132(4):482-491.
20. Clark DJ. Reclaiming endodontics and reinventing restorative, part 2. Dent Today. 2010;29(11):156,158-161.