Controlling the Periodontal-Restorative Interface to Provide Esthetic Dentistry for an Esthetically High-Risk Patient
Abstract: This case involved a young female patient with anterior wear and a high lip line and thin tissue biotype. An organized approach was carried out to diagnose the esthetic problems so that a multidisciplinary treatment plan could be devised. The comprehensive plan included occlusal analysis and equilibration to establish maximum intercuspation in harmony with centric relation, correction of gingival levels, feldspathic porcelain restorations, and teeth bleaching. The case demonstrates technological advances and improvement in dentistry’s understanding of the science of color and dental ceramics.
Achieving predictable esthetic dentistry in a patient with anterior wear is demanding by itself. However, when this is compounded by a high lip line and thin tissue biotype, the case becomes complex and challenging. Establishing definitive goals at the very beginning with such patients and following an organized flowchart of procedures aimed at achieving the final esthetic result is essential.
The case discussed in this article required several areas of treatment—occlusal correction, management of the periodontal-restorative interface, and smile design in keeping with the patient’s youth and beauty. Primarily, its completion highlights the significance of diagnosis and analysis as well as extrapolation of all data gained to synergistically achieve form, function, and beauty.
Technological advances and improvement in dentistry’s understanding of the science of color and dental ceramics enables clinicians to offer appropriate treatment modalities. Some of these modalities may not necessarily use contemporary techniques and materials; rather, sometimes older, well-established techniques should be considered, especially when conservation of tooth structure is important.1
Initial Presentation/Clinical Findings
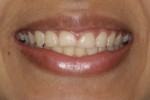
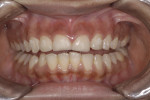
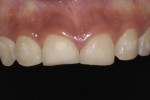
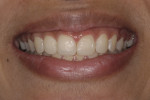
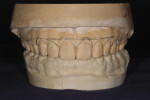
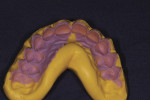
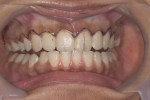
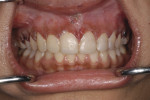
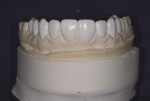
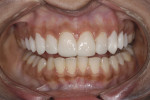
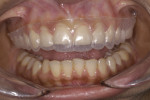
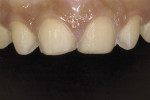
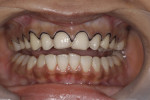
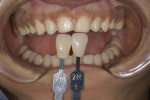
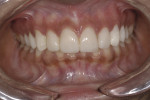
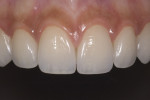
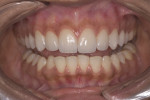
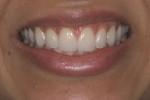
This young female patient was unhappy with her smile because she said her front teeth looked short (Figure 1 through Figure 4). She had received orthodontic treatment for the maxillary dentition, but the incisal edges of the anterior teeth were attrited, resulting in short, square-shaped clinical crowns. The overall effect was an unesthetic smile. Thus, the patient sought an opinion on the feasibility of designing her smile.
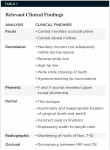
An organized approach was carried out to diagnose2 the esthetic problems so that a multidisciplinary treatment plan could be devised. The relevant clinical findings are listed in Table 1.
Risk Assessment
For an accurate risk assessment, a systematic approach to periodontal, biomechanical, functional, and dentofacial analysis was carried out.3
Periodontally the patient was “low” risk, as there was minimal or no bone loss consistent with American Academy of Periodontology (AAP) classification. Biomechanically the patient was at “moderate” risk; although there was no decay, structurally there was wear on the anterior teeth, with shortened roots on teeth Nos. 7 through 10. Functionally the patient was at “moderate” risk, because there was some occlusion discrepancy between centric relation (CR) and maximum intercuspation (MIP), as well as mild wear on a few posterior teeth. Dentofacially the patient had a “high” risk rating, as there was maximum tooth display and moderate but variable gingival display due to her high upper lip line.
Comprehensive Treatment Plan
Based on these esthetic goals, a comprehensive treatment plan was devised and presented to the patient. The plan could be summarized as follows:
• occlusal analysis and equilibration to establish MIP in harmony with CR to prevent further wear of anterior teeth and have a stable occlusion in the long term
• correction of gingival levels of teeth Nos. 4 through 13 to achieve correct proportions on treated teeth
• feldspathic porcelain restorations on teeth Nos. 4 through 13
• bleaching of lower teeth
Treatment Steps
Diagnostic Esthetic Preview
The first step was to determine the incisal edge position of teeth Nos. 4 through 13. The final restored length of maxillary incisors is affected by various factors, including the lower lip position during smiling, the lip positions at rest and in repose, upper lip characteristics, soft-tissue characteristics, the envelope of function, and facial proportion.4 Apart from determining the incisal length, determination of the horizontal position of the incisal edge is crucial and must accommodate the patient’s envelope of function and neutral zone.5
Teeth Nos. 6 through 11 were etched with 32% phosphoric acid for 20 seconds, and were washed and dried prior to application and curing of the bonding agent (Adper™ Single Bond 2, 3M ESPE, www.3MESPE.com). A2 body shade composite resin (Filtek™ Z350 XT, 3M ESPE) was used to buildup the incisal lengths on these teeth. The shaping of the direct resin was performed, with the author/clinicians mindful of the incisal embrasure forms and axial inclinations of maxillary anterior teeth. The cured mock-up resin was shaped with carbide burs (Safe End, SS White Burs, Inc., www.sswhiteburs.com) and carefully finished and polished to get the incisal plane of upper teeth in harmony with the smile line (Figure 5).
Phonetic guidelines (“F” and “V” sounds) were used to confirm the length and profile of the incisal edge of teeth Nos. 8 and 9. However, several teeth still appeared short in length in proportion to their width. Since the final incisal edge position was now determined, the next step was to calculate the ideal overall lengths needed to create a pleasing smile. This would help the clinicians determine the degree of correction of gingival levels of teeth Nos. 4 through 13 that would be needed. An elastomeric impression of this mock-up was taken using a putty-wash technique to make accurate casts on which measurements could be carried out.
The mesiodistal width of teeth Nos. 8 and 9 was 9 mm. Thus, their ideal length had to be close to 11.2 mm.2,6 This value was used as a guideline to mark a point on the gingival tissues at 11 mm from the incisal edges of mocked-up teeth Nos. 8 and 9 on the stone model. The proposed gingival outline was prepared on the stone model from teeth Nos. 4 though 13. A mock gingival surgery was performed on this cast (Figure 6), and an index was made over it with silicone putty and light-body material. The gingival outline of this silicone putty was trimmed precisely along the scallop of the proposed gingival outline from teeth Nos. 4 though 13. This would now be used as a surgical guide (Figure 7) by the periodontist.
Occlusal Equilibration
Study casts were used on a semi-adjustable articulator with the necessary face-bow and centric records. The patient was deprogrammed and a centric record was taken at a slightly increased vertical dimension of occlusion to prevent tooth contact from deflecting the mandible away from CR. Occlusal equilibration was carried out to remove interfering contact points from inclines of posterior teeth that were responsible for deflecting the mandible forward, thus causing anterior wear.5
Diagnosis for Corrections of Gingival Levels
The surgical guide fabricated from the impression of the mock-up was used to transfer the markings of proposed gingival levels onto the patient’s mouth. A surgical marker was used for this purpose. Next, the clinicians had to decide whether gingival resection alone or a combination of osseous resection along with gingival resection would be needed to achieve a stable soft-tissue level.
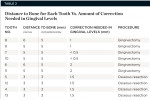
The patient was anesthetized, and a periodontal probe was used to measure the sulcus depth and to sound bone on mid-facial and interdental areas of each tooth. On average, a 1-mm increase in length was needed for teeth Nos. 9 and 10, and a 2-mm increase in length was needed for Nos. 6 and 11. Teeth Nos. 4, 5, 12, and 13 required correction of gingival levels by about 1.5 mm each. Teeth Nos. 7 and 10 needed less than 0.5-mm correction (Table 2).
The distance to bone for Nos. 6 through 11 was sufficient to allow required surgical excision of gingival tissues and still be left with at least 3 mm to bone so that the excised gingival tissue would not rebound, as sufficient biologic width would be maintained.7,8
Teeth Nos. 4, 5, 12, and 13 had a distance of only 3 mm to bone. Hence, to correct the gingival levels on these teeth by 1.5 mm, it was necessary to raise a flap and take the bone down by 1.5 mm so that sufficient biologic width would be maintained as the soft and hard tissue healed.7 Armed with this information, the surgical correction of gingival levels on all teeth was initiated in the same visit.
Surgical and Laser-Assisted Gingival-Level Correction
An 810-nm diode laser was used to carry out the gingivectomy on teeth Nos. 6 through 11 under local anesthesia (Figure 8 and Figure 9). The power setting used was 1.4 watts in continuous mode. Intermittent irrigation with chilled saline was done to prevent heat concentration in the tissues. Care was taken to achieve the desired gingival levels and zeniths as per guidelines set for esthetic rehabilitation.9 A minor correction of gingival levels of Nos. 7 and 10 was carried out with the diode laser.
An internal bevel incision was performed for teeth Nos. 4 and 5. This incision was made in such a way that 1.5 mm of gingival tissue would be excised subsequently after the sulcular incision was completed. Once the required tissue was excised, a full-thickness microflap was raised for only these two teeth. The reflection was just enough to visualize the bone. The palatal tissues were not reflected.
A carbide round bur was used at slow speed with copious irrigation to trim the bone by 1.5 mm so the distance from the new free gingival margin to the bone would be almost 3 mm as healing occurred. Smoothening of the trimmed bone was accomplished, and the creation of positive bone architecture was verified. A 5-0, undyed monofilament suture was used to provide microsutures to close the wound. A similar surgical procedure was then carried out for teeth Nos. 12 and 13.
Frenectomy was performed with the diode laser, as the labial frenal attachment was located more coronally between teeth Nos. 8 and 9.
Wax-Up and Provisionals
An elastomeric impression with putty silicone was taken of the upper arch with corrected gingival levels 10 days after these levels were surgically altered. The proposed final lengths of all teeth from Nos. 4 through 13 were elaborated for the laboratory.
Three weeks later, a full-contour wax-up (Figure 10) with “prep”’ guides and a clear silicone index fabricated on the waxed-up model were received. This silicone index would be used to carry material onto the teeth for direct fabrication of provisionals intraorally.
At 4 weeks after gingival correction, the patient was scheduled for fabrication of the first set of provisional restorations. Protemp™ 4 temporization material (3M ESPE) was loaded on the silicone index generated from the wax-up model and placed in the mouth on teeth Nos. 4 through 13, which were spot-etched and bonded. The excess material was carefully peeled off and removed with a #12 blade. Carbide finishing burs (Safe End Kit, SS White Burs, Inc.) were used to remove excess resin at the margins.
The provisional restorations (Figure 11) were assessed in the patient’s smile for all smile design principles and phonetic guidelines. Occlusion was verified in centric and eccentric positions to confirm the final goals. An impression of the approved provisional in the mouth was taken to provide a guide for the laboratory, and a surface sealing agent (BisCover™ LV, BISCO Inc., www.bisco.com) was applied on the surface of the provisionals and light-cured.
The patient was asked to maintain good oral hygiene and report for a check-up after 4 weeks. She was also instructed to bleach her lower teeth by following a home-bleaching regimen with 22% carbamide peroxide gel (NiteWhite® ACP, Philips Oral Healthcare, www.philipsoralhealthcare.com).
Eight weeks10 after the surgical manipulation of the gingival tissues, the clinicians decided to schedule her for preparations and definitive impressions of teeth Nos. 4 through 13.
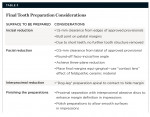
Tooth Preparation Design
The esthetically and functionally approved provisionals in the patient’s mouth determined the final volume of the restoration, so it was decided to cut back these provisionals using round burs of known diameter to achieve the desired clearance on the labial and incisal aspects. This approach for preparation of teeth makes it possible to conserve more enamel, and as a consequence, allows better bonding, biomechanics, and esthetic restorations.11
Two silicone putty indexes were made of the approved provisional in the patient’s mouth. These indexes were cut back in a notebook fashion to enable the clinicians to check for adequate clearance on the labial and incisal aspect during preparation. The horizontally sectioned notebook silicone matrix generated from approved provisionals and the transparent vacuum-pressed vinyl sheet (Figure 12) was used to confirm that adequate and uniform space for ceramic was available on the facial and incisal aspects. The final tooth preparation (Figure 13) considerations are listed in Table 3.
Definitive Impressions
Number 000 knitted cord impregnated with 25% buffered aluminum chloride was packed in the gingival sulcus of teeth Nos. 4 through 13. Minimal pressure was exerted to avoid damage to the connective tissue attachment, which could lead to an unpredictable healing response from the delicate gingival tissues. This cord is left in the gingival sulcus of anterior teeth for 10 minutes. The sulcus depth was used as a guide to decide the depth of margin placement.12 The gingival retraction was done mainly to deflect the gingival tissues from the prepared teeth so as to make space for the low-viscosity elastomers and to provide a dry working area with little sulcular fluid (Figure 14). The clinical goal was to keep the final margins of the preparation equi-gingival without dropping them further apically, as intracrevicular margins were not desired.13
Custom light-cured trays were fabricated with 2 mm of uniform space within them to accommodate the final polyether impression material. A layer of polyether adhesive was applied. Before the impression, the teeth were copiously irrigated with water and all retraction cords were removed. The teeth were then dried and isolated, and the impression material (polyether) was syringed onto the prepared teeth surfaces and within the deflected gingival crevice. The custom tray loaded with the material was placed in position in the patient’s mouth. The material was allowed to completely set, then was removed and disinfected before being sent to the laboratory. A stick bite record and photograph were taken to assist the ceramist with orientation of the upper cast. Stump shades (Figure 15) were recorded. The lower cast would be mounted with a centric record taken at the existing vertical dimension of occlusion.
The prepared teeth were then dried and spot-etched and bonded. The clear silicone matrix generated from the wax-up was loaded with temporization material (Protemp 4) and placed over these teeth. The excess provisional material was carefully cleaned from all areas, especially the gingival embrasures, with a #12 blade and carbide finishing burs (Safe End Kit). The photographs and impressions of final provisional restorations (Figure 16) were sent to the laboratory for reference.
Work Authorization for the Laboratory
The laboratory was informed regarding the color of the final light-cure resin cement that would be used. This would help in planning the color of layering powders.
The final target shade of the veneers in this case was 2M1 of the Vita® 3D-Master® shade guide (Vident, www.vident.com). A very subtle increase in chroma on cervical of teeth Nos. 6 and 11 was desired. The incisal translucency was to be significant but not overbearing.
In the laboratory, the study model of the provisionals was mounted against the opposing teeth, and a silicone putty index was formed to the incisal edges as well as the labial contours. This index helped the ceramist in planning the build-up of the final porcelain restorations. Platinum foil technique was used to fabricate the final feldspathic veneers. The ceramist decided to use the “contact lens” effect at the gingival margin of the preparations to create an illusion of a “disappearing” margin. It was based on this effect that all margins on the teeth had been left clinically equi-gingival (Figure 17).
Trial of Final Veneers
After removal of the provisionals, the veneers were checked for fit one by one and then checked together to verify the contact points. A transparent glycerin gel (Liquid Strip, Ivoclar Vivadent, www.ivoclarvivadent.com) that mimics the transparent shade of luting resin cement was used to try out the veneers.
Preparing the Surfaces for Bonding
Bonding techniques play a crucial role in the survival rates of ceramic veneers.6 Bonding of all 10 veneers should be carried out at one time, as bonding individual veneers could lead to difficulty in seating subsequent veneers after one is bonded. The preparation sequence of surface treatments for both the veneer and tooth are listed in Table 4.
Transparent light-cured resin cement (Variolink N Base, Ivoclar Vivadent) was loaded on all the veneers. A catalyst was avoided because dual-curing was unnecessary due to the relative thinness of the veneers. The long-term color stability of veneers bonded with light-cured resin cements has been shown to be better14 as compared to dual-cured cements.
Starting with teeth Nos. 8 and 9, each veneer was slowly seated with gentle finger pressure along the insertion axis. The gross excess cement was eliminated with the tip of a microbrush wetted with unfilled resin. Digital pressure and cleanup of excess resin were alternately repeated. This was continued until all the veneers were completely seated and no excess cement could be provoked. A clean sable hair brush was used to eliminate any final residue of cement.
All veneers were now “tack”-cured for 5 seconds on labial surfaces. A sharp #12 blade was then used to carefully cut off any gross bits of partially cured resin cement overlying the margins. The retraction cord was gently and carefully removed. Next, light-curing of palatal margins of all veneers was done for 90 seconds, followed by curing of buccal surfaces for 60 seconds. Final polymerization of marginal areas was performed after covering the composite with a layer of glycerin gel. Excess resin cement was removed with a #12 blade. Interproximal excess was removed, and contact between adjacent veneers was cleaned with a proxy disc. This was followed by use of medium-grit abrasive strip to smoothen any resin left over. Dental floss was used to check the patency and tightness of each contact area. Intraoral x-rays were taken to verify the absence of excess cement residue.
The occlusion was verified to ensure that all centric contacts were harmonized, and lingual surfaces were polished with a fine football diamond and rubber points. Light supporting contacts were maintained on anterior teeth. The anterior guidance was checked to make sure that equal pressure was exerted on teeth Nos. 8 and 9 during protrusive excursions. Working side canines and lateral incisors conformed to the planned occlusal design and took the load in lateral excursive movements, thereby discluding all other teeth.5 Fine Astropol (Ivoclar Vivadent) points were used to sequentially polish the margins. The patient was given a nightguard to protect the ceramic restorations. The postoperative photographs depict a satisfied patient (Figure 18 through Figure 22).
Conclusion
The management of the periodontal-restorative interface is challenging when the patient presents with a high lip line and thin tissue biotype. Careful selection of materials and protocols is of utmost importance to blend the restorations near the cervical areas so that the margins are clinically imperceptible. This must be achieved conservatively, keeping principles of smile design and occlusion in mind.
Feldspathic ceramic materials have again become an integral part of contemporary cosmetic dentistry. These handcrafted ceramic masterpieces are in stark contrast to the rapid development of computer-aided manufacturing/computer-aided design (CAD/CAM) technologies, which currently dominate publications and lectures.15
Acknowledgments
The author wishes to acknowledge Michael Sesemann, DDS, FAACD, for being a wonderful mentor, and Prashant Hatkar, MDS, for infusing positive energy in his life. He also acknowledges the contributions of the following dental team members: Bhakti Tunkiwala, MDS, for laser-assisted surgery on teeth Nos. 6 through 11; Sushrut Prabhudesai, MDS, for the periodontal-plastic procedure on the premolars; and Erik Haupt of Haupt Dental Lab, Brea, CA, for the ceramics.
References
1. Bakeman EM, Goldstein RE, Sesemann MR. Responsible esthetics: Is there a return to conservative esthetic dentistry? Inside Dentistry. 2010;6(6):36.
2. Fradeani M. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Vol 1. Chicago, IL: Quintessence Publishing; 2004.
3. Kois JC. New challenges in treatment planning: Incorporating the fundamentals of patient risk assessment—Part 2. Journal of Cosmetic Dentistry. 2011:27(1):110-121.
4. Hess LA. Altering the incisal edge position for optimal function and esthetics. VISTAS Complete and Predictable Dentistry. 2010;3(2 suppl):4-13. https://supp.cdeworld.com/courses/4442. Accessed October 22, 2012.
5. Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:227-230.
6. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Berlin, Germany: Quintessence Publishing; 2002.
7. Kois JC. Altering gingival levels: the restorative connection, Part I: biological variables. J Esthet Dent. 1994;6(1):3-9.
8. Nevins M, Mellonig JT, eds. Periodontal Therapy: Clinical Approaches and Evidence of Success. Vol I, 1st ed. Chicago, IL: Quintessence Publishing; 1998.
9. Chu SJ, Tan JH, Stappert CF, Tarnow DP. Gingival zenith positions and levels of the maxillary anterior dentition. J Esthet Restor Dent. 2009;21(2):113-120.
10. Pontoriero R, Carnevale G. Surgical crown lengthening: a 12-month clinical wound healing study. J Periodontol. 2001;72(7):841-848.
11. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-18.
12. Spear F. Using margin placement to achieve the best anterior restorative esthetics. J Am Dent Assoc. 2009;140(7):920-926.
13. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994.
14. Kano P, Baratieri LN, Gondo R. Ceramic restorations: updates and concepts for esthetic rehabilitation. QDT. 2010;33:199-209.
15. Hein S, Geller W. The platinum foil technique: history, indication, fabrication, and fit. QDT. 2011;34:25-39.
About the Author
Aliasger Tunkiwala, BDS, MDS
Private Practice
Mumbai, India