Accelerated Esthetic Dental Results Using an Interdisciplinary Approach
Abstract: Traditionally, achieving case acceptance in situations that involve orthodontics has been challenging for clinicians, especially among adult male patients. In recent years, surgically accelerated orthodontics has emerged as an alternative approach for patients who might otherwise avoid treatment or choose a compromised form of treatment due to esthetic concerns about wearing traditional braces. In this case report, use of an interdisciplinary approach that combined Kois diagnostic principles with Accelerated Osteogenic Orthodontics™ (AOO™) and lingual braces resulted in a successful restoration while maintaining satisfactory esthetics during treatment.
Dentists often struggle to achieve case acceptance involving orthodontics, particularly in adult males.1 The case presented herein demonstrates a successful, predictable outcome for a patient who had rejected traditional orthodontics. Use of an interdisciplinary approach that combined Kois diagnostic principles (Kois Center, www.koiscenter.com) with Accelerated Osteogenic Orthodontics™ (AOO™) (Wilckodontics, Inc., www.wilckodontics.com) and lingual braces would provide an excellent restorative result without sacrificing esthetics during treatment.2
Orthodontics with surgical acceleration has become an invaluable tool in expediting orthodontic treatment. It enables the clinician to achieve movement that had previously been very difficult without orthognathic jaw surgery3 and helps increase patient acceptance of orthodontia.4
Clinical Case Overview
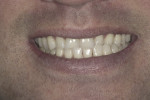
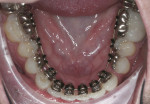
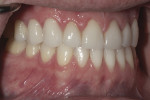
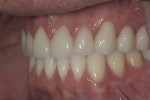
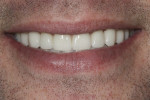
Patient History and Chief Complaint: The patient was a 33-year-old man who presented to the office with a chief concern of chipping front teeth and a visible crossbite (Figure 1). He was aware that orthodontics would be necessary; however, he was apprehensive about his appearance during the treatment and wanted to avoid labial braces.
There were no contraindications to either dental treatment or use of AOO.5 The patient was in good health and had routinely received periodic cleanings every 6 to 12 months. He had previously consulted with 16 different specialists and general dentists. Treatment plans presented to him had included a Le Fort I maxillary advancement, labial orthodontics, and clear aligners. He expressed unease with those plans, which he felt did not address his chief concerns.
Diagnostic Findings
Oral cancer screening was performed with no abnormal findings. Additionally, the patient had no history of sleep-related airway issues or sleep bruxism and had a Mallampati grade 1 airway.
Periodontal: The examination revealed good oral hygiene and some mild gingivitis. Periodontal pocket measurements did not exceed 4 mm, and the patient was classified as AAP type 1 periodontitis. Alveolar bone levels were optimal with no bone loss. The patient’s biotype was classified as thin, and gingival scallop was high.6
Risk: Low
Prognosis: Excellent
Biomechanical: There were no caries and no signs of erosion. The full-coverage crown on tooth No. 19 exhibited marginal microleakage and was, therefore, considered questionable. All other existing restorations were classified as acceptable.
Risk: Moderate
Prognosis: Good
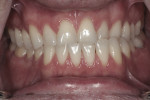
Functional: The patient had a class 3 skeletal and dental relationship. Teeth Nos. 10 through 12 and 21 through 23 were in crossbite. These teeth exhibited class 1 mobility as a result of primary occlusal traumatism. There were no joint noises, nor was there any muscle tenderness. The joints exhibited a normal response to loading. Responses given in the patient’s dental history indicated that the wear was currently active. The patient also reported that he had more than one bite, and had a mild parafunctional habit of nail biting. Teeth Nos. 6 through 10 and 23 through 27 had mild to moderate attrition. The functional diagnosis was determined to be a constricted envelope of function due to the findings of primary occlusal trauma and severe attrition of the anterior teeth.
Risk: Moderate
Prognosis: Fair
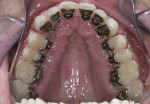
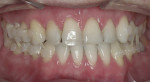
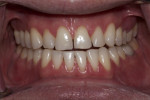
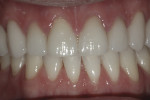
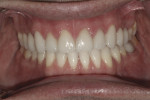
Dentofacial: Dentofacial risk is based on the amount of tooth and gingiva revealed by the patient both in full smile and repose.7 The patient’s lip measured 23 mm and elevated approximately 8 mm in full smile. In repose, approximately 2 mm of tooth structure was visible. These measurements fall within normal limits of an adult male in the third decade of life,8 for whom it is expected that the lip will lengthen by 1 mm each decade throughout his lifetime.9 Although gingival display was minimal, the interdental papillae were visible at full smile (Figure 2). For this reason, the dentofacial risk was classified as moderate. The prognosis was poor due to the broken down dentition (Figure 3).
Risk: Moderate
Prognosis: Poor
Treatment Goals
Treatment goals addressed the patient’s chief concern—chipping front teeth and a visible crossbite—through an interdisciplinary approach that reduced functional risk without increasing periodontal or biomechanical risk.10 These goals were achieved in a fast and esthetic manner that was acceptable to the patient while accomplishing an optimal outcome with a natural appearance.
Treatment Plan
Using an interdisciplinary approach, it was determined that the patient would be well served with lingual braces (Incognito™, 3M Unitek, www.3Munitek.com), in conjunction with AOO. By planning the AOO in conjunction with the lingual braces rapid tooth movement would be achieved while addressing the patient’s esthetic concerns. Transitional bonding would be placed during orthodontic treatment to improve esthetics and facilitate communication between the orthodontist and restorative dentist. Following orthodontia, necessary restorative dentistry would be completed to restore the tooth structure lost to functional attrition.
Treatment Details
Planning and Delivery of Braces
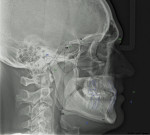
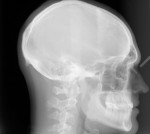
Mounted diagnostic casts, a full-mouth series of x-rays, a cephalometric radiograph (Figure 4), a dentofacial analyzer transfer, a panoramic radiograph, and diagnostic photographs were taken. Referrals were made for orthodontic and surgical consultations.
Polyvinyl siloxane (PVS) impressions were taken, and a prescription was developed for Incognito lingual braces. The setup was reviewed and approved by the general dentist and orthodontist. Six weeks after the impressions, the customized braces and wires were returned and delivered to the patient.
Surgical Phase
Seven days after the placement of braces, the surgical phase of treatment was completed under intravenous sedation. Interdental circumscribing cuts and corticotomies were performed, and a mix of 50% demineralized freeze-dried bone allograft (DFDBA) and 50% BioOss® (Geistlich Biomaterials, www.bio-oss.com) grafting material was placed over the cortical bone. 4-0 Gore-Tex® sutures (W.L. Gore & Associates, Inc., www.goremedical.com) were placed in an interrupted fashion (Figure 5 and Figure 6). Postoperatively, the patient was placed on amoxicillin 500 mg TID for 7 days and pain medications as needed.
Orthodontic Phase
With AOO, minimal movement occurs in the first 4 weeks, but very rapid movement occurs from month 1 to month 6. This period is known as regional acceleratory phenomenon (RAP).11 This physiological process can be described as “bone matrix transportation” and occurs subsequent to the demineralization of the alveolar housing in response to osseous insult.12 Patients are instructed to avoid NSAIDs for 6 months, as the anti-inflammatory effect negatively influences the RAP.13 The patient was seen every 2 weeks to monitor the progress of the orthodontics and for necessary wire changes. Periodontal maintenance was performed every third month.
Tooth movement was accelerated by use of class 3 elastics with composite buttons. At 10 weeks, enough overjet was achieved to allow placement of transitional composite bonding to repair the incisal edges previously damaged through functional wear (Figure 7 and Figure 8). This achieved an improvement in appearance by creating symmetrical teeth while giving the orthodontist a specific guide to the planned restorative endpoint. The orthodontist could then use either the free gingival margin or the incisal edges to line up the teeth. Moreover, orthodontic extrusion of teeth Nos. 24 and 25 was completed with enameloplasty to improve esthetics and to avoid the need for restoring those teeth.
Total orthodontic treatment spanned 8 months. Upon removal of braces (Figure 9), the patient was placed in retention with an Essex-type retainer and was referred to the general dentist for restorative treatment.
Post-Orthodontic Diagnostics
One week after the braces were removed, PVS impressions, bite records, photographs, and dentofacial analyzer records were taken, and a diagnostic wax-up was created. During this diagnostic process, ideal gingival zeniths were noted, and it was determined that tooth No. 13 was indicated for esthetic crown lengthening. After close analysis of intraoral photography, scarring from the periodontal/osseous surgery was visible near the area of the papilla.
Periodontal Surgery and Shade Selection
The patient was appointed with the general dentist for periodontal surgery, where gingival zeniths were optimized, the necessary crown lengthening was completed using a closed technique14 on tooth No. 13, and the area of scarring was abraded with a coarse diamond. Shade selection was performed and noted to be 3R1.5 gingival and 2R1.5 incisal (Vita 3D Master® Shade Guide, Vident, vident.com.).
Restorative Phase
Five weeks after the removal of the lingual braces and approximately 9 months after the start of orthodontics (Figure 10), restorative dentistry was initiated. In order to maintain the ideal spacing that had been created by the orthodontist, immediate preparation of anterior teeth and the nonfunctional cusps of two of the premolars was completed.15 A stabilization period of a minimum of 2 months is advised in cases involving intrusion or extrusion of the incisors or molars and in cases with unstable occlusion.16
Prior to the restorative appointment, a matrix was fabricated from the diagnostic wax-up using PVS putty with a light-body PVS reline (Sil-Tech®, Ivoclar Vivadent, www.ivoclarvivadent.com). Anesthesia was achieved with three carpules of 4% septocaine, and the matrix was tried in to confirm fit. The teeth were then spot-etched, primed, and bonded. The matrix was filled with bis-acrylic composite (Protemp™, 3M ESPE, www.3MESPE.com) in a bleach shade and placed intraorally for 2 minutes. The putty was then removed and preparations were done through the mock-up into enamel. This technique allows for conservative preparation by eliminating unnecessary removal of tooth structure.17 Bonding the mock-up assures that it does not fall off during preparation.
A full-arch impression was taken with PVS (Aquasil™, DENTSPLY Caulk, www.caulk.com), and bite registration was obtained (Blu-Bite®, Henry Schein, www.henryschein.com). Temporization was done using the same matrix as the mock-up and A1 Protemp provisional material. The temporaries functioned as a trial smile for the coming weeks. No adjustments were necessary to the provisional because the patient was satisfied with the appearance and function. The stability from splinting nine temporaries together was deemed sufficient to maintain tooth position, so no additional retention was used for this patient while he wore the temporaries. However, providing extra-coronal retention during the temporary phase is generally advised to maintain interproximal contacts and tooth position. An Essex-style retainer made on a model of the diagnostic wax-up provides added assurance that the final restorations will have predictable interproximal contacts at delivery. Retention is necessary for final restorations,18 as the ideal spacing achieved orthodontically can be difficult to maintain.
Pressed e.max® (Ivoclar Vivadent) ceramic restorations were fabricated with a V1 ingot and cut back and layered with e.max Ceram™ (Ivoclar Vivadent) porcelain impulse powders to mimic the appearance of the patient’s natural dentition (Figure 11 through Figure 13).
The final restorations were placed 3 weeks later (Figure 14). A 4th generation bonding protocol was used with translucent RelyX™ Veneer Cement (3M ESPE), a light-cured bonding agent. A new retainer was fabricated at the time the restorations were placed, and the patient was advised to wear the retainer every night for 12 months.17 After delivery, the occlusion was adjusted so the central incisors had little functional contact and functional canine guidance was present on the highly polished e.max porcelain of adequate thickness (Figure 15).
Conclusion
Esthetic and rapid dental therapy can be completed with the use of orthodontics. The total treatment time in this case was less than 11 months—much less time than traditional modalities of therapy typically require. During treatment, the patient’s esthetic requirements were met with lingual braces and the placement of transitional bonding.
Surgically accelerated orthodontics proved to be an ideal approach for this patient, who may have otherwise avoided treatment altogether or chosen a compromised form of treatment due to his esthetic concerns about wearing traditional braces. This treatment modality has the potential to increase treatment acceptance for a population demographic that has historically rejected traditional orthodontics due to length of treatment time and the appearance of braces. Creating beautiful smiles is among the most gratifying things dentists facilitate, and the hope is that this approach will increase treatment acceptance by using an orthodontic method that is fast, safe, and esthetically pleasing.
Through an interdisciplinary approach, this patient’s functional risk was decreased while functional and dentofacial prognoses were improved without increasing either the periodontal or biomechanical risk. Most importantly, the expectations of this patient were met, giving him a natural smile in a timely manner (Figure 16).
Acknowledgments
The author wishes to acknowledge the contributions of orthodontist Shawn Miller, DDS, MS, Orange, California; periodontist Marlene Miller, DMD, MMedSc, Tustin, California; dental technician Wayne Payne, CDT, AAACD, Payne Dental Laboratory, San Clemente, California; and William J. Spath, DDS, father and mentor.
References
1.Tuominen ML, Tuominen RJ. Factors associated with subjective need for orthodontic treatment among Finnish university applicants. Acta Odontol Scand. 1994;52(2):106-110.
2. Muir JC. Lingual orthodontic appliances: invisible braces. N Z Dent J. 1991;87(388):57-59.
3. Criteria for Orthognathic Surgery. Rosemont, IL: American Association of Oral and Maxillofacial Surgeons; 2008:3.
4. Bell WH, Finn RA, Buschang PH. Accelerated orthognathic surgery and increased orthodontic efficiency: a paradigm shift. J Oral Maxillofac Surg. 2009;67(10):2043-2044.
5. Roblee RD, Bolding SL, Landers JM. Surgically facilitated orthodontic therapy: a new tool for optimal interdisciplinary results. Compend Contin Educ Dent. 2009;30(5):264-275.
6. Bakeman EM, Kois JC. Maximizing esthetics/minimizing risk: the line of predictable success. Inside Dentistry. 2005;1(1):16-24.
7. Kois J. New challenges in treatment. Journal of Cosmetic Dentistry. 2011;27(1):110-123.
8. Peck S, Peck L, Kataja M. Some vertical lineaments of lip position. Am J Orthod Dentofacial Orthop. 1992;101(6):519-524.
9. Rifkin R. Facial analysis: a comprehensive approach to treatment planning in aesthetic dentistry. Pract Periodontics Aesthet Dent. 2000;12(9):865-871.
10. Wennström JL. Mucogingival considerations in orthodontic treatment. Semin Orthod. 1996;2(1):46-54.
11. Frost HM. The biology of fracture healing. An overview for clinicians. Part 1. Clin Orthop Relat Res. 1989;248:283-293.
12. Wilcko MT, Wilcko WM. The Wilkcodontics Accelerated Osteogenic Orthodontics (AOO) Technique: An Overview. Orthotown. 2011;July/August:36-48.
13. Nowzari H, Yorita FK, Chang HC. Periodontally accelerated osteogenic orthodontics combined with autogenous bone grafting. Compend Contin Educ Dent. 2008;29(4):200-206.
14. Sonick M. Periodontal plastic surgery II: esthetic crown lengthening. Inside Dentistry. 2007;3(9):64-72.
15. Moon JE, Kim SH, Han JS, et al. Esthetic restorations of maxillary anterior teeth with orthodontic treatment and porcelain laminate veneers: a case report. J Adv Prosthodont. 2010;2(2):61-63.
16. Amato F, Mirabella AD, Macca U, Tarnow DP. Implant site development by orthodontic forced extraction: a preliminary study. Int J Oral Maxillofac Implants. 2012;27(2):411-420.
17. Magne P, Magne M. Use of additive waxup and direct intraoral mock-up for enamel preservation with porcelain laminate veneers. Eur J Esthet Dent. 2006;1(1):10-19.
18. Clark JD, Kerr WJ, Davis MH. CASES—clinical audit; scenarios for evaluation and study. Br Dent J. 1997;183(3):108-111.
About the Author
Andrew Spath, DDS
Lecturer
UCLA School of Dentistry
Los Angeles, California
Private Practice,
Newport Beach, California