Full-Mouth Rehabilitation of a Patient with Crohn’s Disease
David A. Cauble, DMD
Abstract
In this case, the patient's ultimate goal was to achieve a long-term functional chewing system that was esthetically pleasing and resilient to the potentially debilitating effects of Crohn's disease. The majority of the patient's risk was biomechanical, which proved to be a precursor to his functional and esthetic issues. The occlusal dysfunction was attributed to his loss of posterior support.
Background
Age at Initial Presentation: 42
Initial Presentation: January 2007
Active Treatment Completed: January 2010
Medical History
The patient presented with a significant history of Crohn’s disease, diagnosed when he was 13 years old. At age 15 he reported continual low-grade infections of the bowel requiring the administration of antibiotics for the next 5 years. During this time he was also on a high-caloric diet in an effort to maintain adequate weight. During these teenage years malnutrition became an issue and he recounted having an emaciated appearance, which prevented him from wanting his school picture taken. In 1998 complete bowel obstructions began reoccurring until 2001, when resection surgery of the bowel was necessary. At this time he was placed on Prednisone for the next year as well as Remicade administered intravenously for the next 3 years. In 2004 the patient had another obstruction of the bowel and was again placed on Prednisone and intravenous Remicade administered once every 8 weeks until present. The patient reported that between 1990 and 2004 he was in constant pain that was at times totally debilitating. Stomach pain would regularly keep him in bed.
Dental History
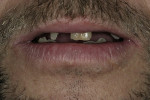
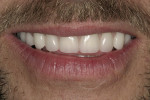
The patient presented with the following chief concern: "I want my teeth removed or repaired to give me a bite that works and lasts" (Figure 1). He felt embarrassed when he smiled because of his missing and broken teeth, and was looking for a long-lasting natural-looking solution that would be effective in chewing his food. The patient had recently been to several dentists within the community to discuss treatment options. In the past 12 years his dental health had rapidly declined as the negative effects of Crohn’s disease advanced. He had seen his susceptibility to tooth decay increase, ultimately leading to tooth loss.
Diagnostic Findings
Temporomandibular Joints: Maximum opening was 49 mm within normal range of movement. There was no deviation upon opening. Minor bilateral popping sounds were found. Findings from the load test of the joint were negative; immobilization test was positive.
Extraoral: The patient presented with an uneven occlusal plane; 7 mm of the maxillary central incisor displayed in a full smile with normal upper lip mobility and lip length. A scar on the lower left border of the lip was noted with slight residual swelling and minor immobility of the lower lip (Figure 2).
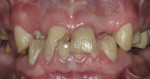
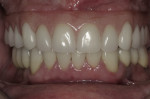
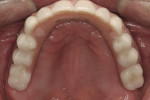
Intraoral: The patient had many missing and fractured teeth, with existing anterior teeth showing signs of moderate attrition and erosion (Figure 3, Figure 4 and Figure 5). There were many direct composite restorations restoring areas of decay and fracture, and exposed dentin on lower incisors. Active decay was noted on teeth Nos. 2, 6, 7, 8, 11, 13, 14, 21, 22, 27, and 28. Existing full-coverage restorations had active decay and/or questionable margins. Probing depths were within normal limits. There were several isolated areas with probing depths of 4 mm, with most areas not probing more than 3 mm. There were also some isolated areas of bleeding on probing with firm and salmon pink tissues.
Occlusal Notes
The patient had Class 1 malocclusion, lacking any posterior support because of tooth loss due to decay and infection. All existing teeth except for the lower incisors were biomechanically compromised with active decay. His lower anterior teeth had moderate attrition with exposed dentin, and occlusal vertical dimension was collapsed. Centric relation was not coincident with maximum intercuspal position.
Radiographic Assessment
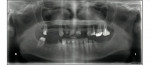
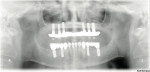
Pulpal pathology was noted on teeth Nos. 8 and 31 as well as failed root canal on No. 13. Mild bone loss was noted in all edentulous areas due to tooth loss (Figure 6).
Diagnosis
Periodontal: Mild chronic periodontitis, AAP Type II.
Biomechanical: Caries was present on all remaining dentition except for the lower incisors. All remaining dentition was biomechanically compromised with restorative work, most of which was failing. Moderate wear due to attrition and some evidence of erosion was noted on the incisal surfaces of teeth Nos. 22 to 27 and lingual surfaces of teeth Nos. 8 and 9. Pulpal pathology was noted on teeth Nos. 8, 13, and 31.
Functional: Occlusal dysfunction.
Dentofacial: Generalized missing, fractured, and discolored teeth. The mandibular incisal edge position was deficient due to wear.
Medical: Crohn’s disease.
Risk Assessment
The individual risk assessment was an invaluable tool in deciding an effective course of treatment. Only after thorough collection of dental and medical histories could risk factors be assessed and a treatment plan developed that would accomplish the patient’s request to lower biomechanical risk and improve function and esthetics.
Periodontal: Low
Biomechanical: High
Functional: High
Dentofacial: High
Prognosis
The overall prognosis of this debilitated dentition was considered poor to hopeless without treatment. No treatment and continued progression of multiple disease factors combined with the negative impact of Crohn’s disease were the contributing factors to such a negative prognosis. With treatment, by eliminating the most biomechanically compromised dentition and maintaining the least biomechanically affected dentition, a fair to good prognosis could be expected. Periodontally, this patient had minimum risk. Full and partial coverage restorations would protect remaining teeth from further decay and erosive factors as well as provide the ability to restore the occlusion in a stable bilateral balanced position.
Concerns
- How would the patient’s risk assessment modify the treatment planning strategy?
- How aggressive an approach would be appropriate—in regards to tooth removal—to provide the patient with the most predictable treatment?
- What occlusal vertical dimension would be appropriate for this patient? How would this vertical dimension be established? Once established, how would it be maintained throughout treatment?
- What would be the best sequence of events to maintain the best control of the case?
Treatment Goals
- Control the patient’s disease.
- Restore the shape/position of the upper and lower teeth and place implants appropriately.
- Establish a balanced occlusion.
- Make his teeth whiter.
Treatment Plan
Treatment options were discussed with the patient. The patient’s primary objectives were to achieve a dentition that was less prone to biomechanical failure while taking his medical condition into account. He wanted a functional bite and whiter teeth. Understanding the importance of good oral hygiene and realizing the risk factors associated with his disease he wanted to preserve his teeth but not as a compromise to the overall result. He was amenable to, and even prepared to, lose his remaining dentition, if necessary. Because of the extensive biomechanical risk of the majority of the dentition, maintaining the most compromised teeth was not recommended. His remaining teeth Nos. 6, 9, and 11 were in an acceptable position in the face, which was helpful in determining future tooth position and deciding how much of an increase in the vertical dimension of occlusion would be needed. A full-mouth rehabilitation focusing on the patient’s treatment goals was offered to the patient.
Phase I: Disease Control Phase
Reviewing the high biomechanical risk of the majority of the upper dentition as well as the lower posterior dentition, and taking into account the unpredictability of the patient’s medical condition, all remaining upper teeth and lower posterior teeth were removed. At the time of removal bone grafting was done to preserve the ridge as well as enable key locations to have implants placed at a later date. An upper immediate complete denture and a lower removable partial denture were fabricated at an increased vertical dimension of occlusion. A 6-mm increase in occlusal vertical dimension in the anterior was accomplished in the interim dentures. Minor caries control was done on the lower canines, oral hygiene instruction was given, periodontal prophylaxis was performed, and a home-care regimen with a caries reduction protocol was prescribed (CariFree®, Oral BioTech LLC, www.carifree.com).
Phase II: Surgical Phase
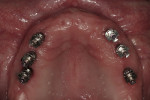
After a 6-month healing period in an immediate upper denture establishing the correct esthetic and functional tooth position, the denture was duplicated and a radiographic guide was fabricated with markers at tooth positions 3, 5, 6, 11, 12, and 14 on the maxillary arch and 19, 21, 28 and 30 on the mandibular arch (Figure 7). A surgical guide was then fabricated and implants were placed (Straumann USA LLC, www.straumann.us) (Figure 8). The patient healed in his provisional dentures for another 5 months.
Phase III: Restorative Phase
The patient’s objective was to have a fixed dentition. After esthetic evaluation it was determined that upper lip support was not needed from the flange of a prosthesis. It was decided that a fixed hybrid prosthesis would be the treatment of choice. Esthetic goals were already achieved in the provisional dentures as were the functional goals with the increase in the occlusal vertical dimension. The various phases of complete denture fabrication were followed to the completion of the upper arch prosthesis (Figure 9). Implant-supported porcelain-fused-to-metal (PFM) bridges were fabricated on the lower posterior quadrants. Lower canines were designed for PFM restorations and lower incisors were designed for all-ceramic, core-supported zirconia restorations (Lava™, 3M ESPE, www.3MESPE.com). Final impressions were made using a dual-phase, single-stage technique with light body and putty-viscosity polyvinyl siloxane (Impressiv, Cosmedent, Inc, www.cosmedent.com) according to manufacturer’s instructions (Figure 10). Provisional restorations for teeth Nos. 22 to 27 were made chairside directly with a Bis-acrylic composite temporary crown and bridge (Luxatemp, DMG America, www.DMG-america.com). The Kois Dento-Facial Analyzer System (Panadent Corporation, www.panadent.com) was used to communicate functional and esthetic parameters for the mounting of the upper occlusal wax rim. Records, casts, and final impressions were transferred to the laboratory technicians for the fabrication of the definitive restorations. The lower implant-supported restorations were cemented with Premier® Implant Cement™ (Premier Dental, www.premusa.com), and the PFM and zirconia restorations were cemented with a self-adhesive resin-luting cement (RelyX™ Unicem, 3M ESPE) according to the manufacturer’s instructions (Figure 11).
Phase IV: Maintenance Phase
The patient was scheduled to return for postinsertion recare every 4 months.
Commentary
By carefully evaluating the patient’s individual risk factors medically, biomechanically, and functionally an appropriate treatment plan was designed and carefully carried out in the clinic. The treatment addressed his chief concern of his unpredictable health, inability to chew his food, and poor appearance. The final result exceeded the patient’s expectations (Figure 12, Figure 13, Figure 14, Figure 15 and Figure 16).
The patient’s ultimate goal was to achieve a long-term functional chewing system that was esthetically pleasing and resilient to the potentially debilitating effects of Crohn’s disease. The majority of the patient’s risk was biomechanical, which proved to be a precursor to his functional and esthetic issues. His occlusal dysfunction was attributed to his loss of posterior support.
In an effort to achieve the most predictable result with regard to all risk factors, the most biomechanically compromised teeth were eliminated and replaced with implant-supported restorations. The joint was positioned in a more favorable orthopedic position (centric relation), and he was restored with a bilateral balanced occlusion. The postoperative functional diagnosis was acceptable and the preoperative high-risk biomechanical and dentofacial concerns were lowered significantly.
Acknowledgments
Oral surgery-implant placement and bone grafting by Todd A. Schock, DMD, MD; fixed hybrid prosthesis by Ruth Bourke BSc; ceramics by Colin Gibb, CDT
About the Author
David A. Cauble D.M.D.
Private Practice
Bend, Oregon