There Is More to Front Teeth Than Looks Alone: Diagnosis and Treatment Planning
Treating Dentist: Joyce L. Bassett, DDSAdjunct Faculty, Senior Dental Student Esthetic Continuum, A.T. Still University, Arizona School of Dentistry, Mesa, Arizona;Private Practice, Scottsdale, Arizona
Background
Age at Initial Presentation: 26
Initial Presentation: December 8, 2008
Active Treatment Completed: May 12, 2009
Medical History
The female patient had a history of an anxiety disorder and gastrointestinal symptoms. She was taking Lexapro® daily for anxiety symptoms and Levsin® prn to control her stomach pain.
Dental History
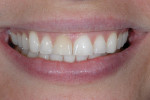
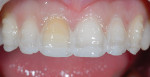
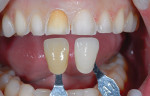
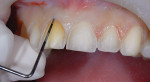
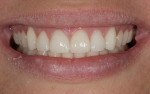
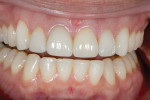
The patient presented seeking a cosmetic solution to her smile. Her last dental examination was 2 years earlier, and she had a history of trauma to her right central incisor. She reported intermittent pain and a sense of "tiredness" on the left side of her face. She was embarrassed to smile due to her "dark front tooth" and had noticed the edges were "chipping and thinning" (Figure 1 and Figure 2).
Diagnostic Findings
Extraoral: Normal.
Intraoral: Normal. Findings from the cancer screening were negative.
Temporomandibular Joints: Within normal limits. Maximum interincisal opening was 55 mm. No deviation or pathologic joint sounds were noted. Findings from the load and immobilization tests were negative.
Occlusal Notes
The patient had a Class 1 dental relationship.
Radiographic Assessment
The right central incisor had a questionable periapical lesion.
Diagnosis
Periodontal: Mild, chronic periodontitis, AAP Type I. There was no bleeding on probing, and the depths were within normal limits. Bone support was within 2 mm of the cementoenamel junction without infrabony defects. The gingival architecture was symmetrical. No pathologic mobility was present.
Biomechanical: Caries and minimal erosion were present on the occlusal surfaces of teeth Nos. 18 and 19. The central incisors exhibited combination lesions of erosion and abrasion at the incisal edges. The right central incisor had possible periapical pathology.
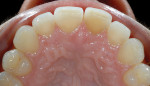
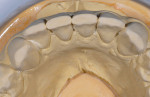
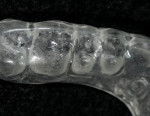
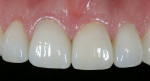
Functional: The patient presented with minimal attrition on the surfaces of teeth Nos. 5, 13, 20, 21, and 28. Moderate attrition with an erosive component appeared on the palatal/incisal surfaces of teeth Nos. 8 and 9. This cupping indicated that the chemical aspect was outpacing the frictional damage (Figure 3). The frictional issue was the causal agent of the diastema between the central incisors. Teeth Nos. 6, 7, 10 to 12, and 22 to 27 exhibited moderate attrition (Figure 4). Parafunctional activity was evident, and the patient experienced pain in the left masseter.
Dentofacial: Gingival tissue levels on the lateral incisors were not harmonious. The patient exhibited a high smile line, and the right central incisor appeared dark. There was a diastema between the central incisors.
Medical: Within normal limits.
Risk Assessment
An individual risk assessment is critical for determining the most appropriate treatment plan. There can be multiple treatment plans but only one diagnosis. The goal is to decrease the risk and increase the prognosis with the proposed treatment plan.
Periodontal: Low risk because there was no evidence or risk factors for bone loss.
Biomechanical: Moderate risk because of the amount of active attrition, erosion, and caries, and the need for endodontic intervention on the central incisor.
Functional: High risk because of the combination of occlusal dysfunction and parafunction.
Dentofacial: High risk because the patient exhibited high lip dynamics, high gingival scallop, thin biotype, and excessive tooth and gingival architecture display. Restoration margin placement and shade matching of the dark tooth would be more challenging. Exceeding the patient's expectation can be complicated when all aspects of the smile show.
Prognosis
Periodontal: Good
Biomechanical: Fair
Functional: Poor
Dentofacial: Poor
Concerns
1. How can the occlusion be managed to reduce the functional risk?
2. How can the parafunctional habits be handled in order to provide longevity to the final porcelain restorations?
3. How can esthetics be achieved without increasing the biomechanical risks?
4. Can the posterior dentition be equilibrated to allow the patient to feel posterior bilateral contacts simultaneously, thus attaining a "home position"?
5. Can the dark tooth be masked with porcelain and match the adjacent veneer?
6. Can the dark stump under the gingival margin of the right central incisor be masked, or will it show through the patient's thin biotype?
Treatment Goals
1. Maintain provisional and final restorations that do not break, chip, or debond.
2. Perform predictable minimally invasive preparation design of the anterior dentition.
3. Meet the patient's esthetics goals.
4. Increase the functional prognosis by equilibrating the dysfunction and making the patient aware of her parafunctional habits.
5. Determine the appropriate length, angle of guidance, overjet, and overbite.
Treatment Plan
The proposed treatment plan began with a periodontal referral for crown lengthening so the zenith on both lateral incisors would be equal, an orthodontic referral to correct the mandibular teeth rotations, and an endodontic referral for the right central incisor.
The patient refused to see the periodontist and orthodontist but agreed to have the endodontic phase completed. She did not want internal bleaching.
Phase I
1. Kois deprogrammer
2. Functional analysis
3. Equilibration
Phase II
1. Zoom power bleaching would be performed on all teeth not receiving porcelain restorations.
2. Records would be taken for a diagnostic wax-up.
3. Teeth Nos. 6, 7, and 9 to 11 would receive veneers. A crown would be placed on tooth No. 8, and incisal composites would be put on teeth Nos. 12 and 22 to 27. Teeth Nos. 18 and 19 would receive occlusal composites, and teeth Nos. 13, 14, 20, and 21 would be recontoured.
Phase III
The bruxism appliance would be fabricated.
Functional Analysis
The patient exhibited generalized wear facets on the incisal edges of many teeth (Figure 5 and Figure 6). It was necessary to see if these clinical findings correlated with the mechanics of occlusion. A Kois deprogrammer was fabricated to erase the engrams, break the feedback loop, halter muscle activity, and establish therapeutic position location (centric relation [CR]). The patient was instructed to wear this appliance as much as possible with the exception of eating and lifestyle interruptions.
This appliance has one anterior point of contact and separates the posterior teeth by 1 mm to 1.5 mm. When the patient removes the appliance, he or she should put teeth together and note the first two teeth that contact (centric occlusion). When this point of contact is duplicated consistently in the same location with no lateral movement, the patient is deprogrammed and ready for a CR bite record. This appointment occurs 1 week later, and the patient is instructed to wear the deprogrammer. The CR record is taken with the deprogrammer in the mouth. A functional analysis is performed and the feasibility of occlusal correction is determined.
In this patient, centric occlusion, which is the first point of contact in CR, was posterior to the maximum intercuspal position (MIP). This constituted occlusal dysfunction. The treatment was to correct the position of the posterior teeth by performing an occlusal equilibration using the deprogrammer 4 weeks later.
Restorative
New records were taken, and a diagnostic wax-up with preparation and provisional matrixes were fabricated. To assure appropriate but minimal reduction, the provisional matrix was loaded with a bis-acrylic composite. Composite prototypes were added to the facial surface of the maxillary anterior dentition. This allowed the patient to preview the esthetics and guide modifications in shape, fullness, and length. This facilitated appropriate preparation to assure maximum esthetics with minimum reduction.1 The patient evaluated the length and fullness; modifications were made until the patient approved this (Figure 7). Depth cut guides were then used across the facial prototypes and removal of 2 mm of incisal composite from the definitive patient-approved incisal edge was performed (Figure 8). The remaining composite prototype was removed, and the marks left by the depth cutter guided the definitive veneer preparation. The desired final color of the restoration and the underlying stump shade were the determining factors in the amount and depth of axial reduction.
A minimal preparation of 0.3 mm of facial reduction is necessary for a one-shade shift. The medium preparation of 0.5 mm can provide a two- to three-shade shift. A deep preparation of 1 mm is necessary to obtain a difference in color of three shades or more2 (Figure 9). In general, a depth of 0.2-mm space is needed to change the hue of the tooth by one shade.
It was necessary to remove 1 mm of facial dentin in the preparation design on the upper left central incisor to create space for restorative material with a four-shade shift stump. On evaluation of the palatal, there was a large endodontic access preparation, and a full cohesively designed crown preparation was performed.
Probing of the labial gingival sulcus revealed a space of less than 3 mm before the bone was sounded (Figure 10). This reflected a high risk of biologic width violation, dictating that the preparation margin must remain at the free gingival margin.3-5 The probe could be visualized when being used because a thin biotype was present. Expasyl® (Kerr, https://www.kerrdental.com) hemostatic atraumatic cord-free retraction was placed and rinsed. Impressions, facebows, and bites were recorded. A bis-acrylic composite (Venus® Temp C&B, Heraeus, https://www.heraeus-dental.com) was loaded into the provisional matrix. Composite prototypes were fabricated and luted with a combination of spot-etching and bonding with veneer cement (RelyX™, 3M ESPE, https://www.3mespe.com) in the tooth center. TempBond™ (Kerr) clear cement was employed at the periphery of the restorations and light-cured (Figure 11). The patient was dismissed but returned 20 mins later with the anterior prototypes fractured at both lateral incisors (Figure 12). The parafunctional habits of abnormal posturing and protrusive bruxism were occurring at a frequency during the day that was not appreciated until the provisionals were placed. A key concern was identifying the daytime parafunctional bruxism that happened subconsciously, and educating the patient on this destructive pattern.
An acrylic was placed on the anterior ramp of the patient's deprogrammer 4 mm high to prevent contact of the lower teeth against the maxillary provisionals (Figure 13). The patient was instructed to wear the deprogrammer during the day as a reminder to keep her lower incisors away from the incisal edges of her maxillary dentition. During this time, her occlusal diagnosis and treatment plan were reviewed. In occlusal dysfunction, the treatment was to steepen the angle of guidance and increase the interincisal angle. This was performed as part of her original provisionals. In parafunction, the treatment was to flatten the angle of guidance, eliminate excursive interferences, minimize lateral contacts, and shallow the cuspid guidance. Modifications to the composite prototypes were made until the final provisional restorations accomplished these parameters. The patient began weaning herself from the daytime deprogrammer. After 30 days with no breakage or loosening of the provisionals, a record and photographs were taken and sent to the ceramist to serve as a template for fabricating the final prosthesis. The delivery appointment entailed a try-in, evaluation of the esthetics, and cementation of the six porcelain-bonded restorations. The patient wore a nighttime appliance as instructed. Two years after treatment, no pulpal pathology, delaminations, or chipping was clinically appreciated. On periodontal recall, she was directed to bring her appliance, which displayed occlusal streaks and grooves (Figure 14).
Summary
When treating high-risk parafunctional cases, patient compliance and understanding of the disease is paramount in the success and longevity of the restorations. Controlling the patient's expectations for augmenting the length and blocking out the dark color was accomplished (Figure 15, Figure 16, Figure 17 and Figure 18).
Acknowledgments
The concepts in this article are the teachings of the Kois Center. The author thanks Brad Patrick of Patrick Dental Studio for the ceramic artistry discussed in this article.
References
1. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):17-18.
2. Gurel G. The Science and Art of Porcelain Laminate Veneers. Chicago, IL: Quintessence; 2003:241-251, 261-276.
3. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
4. Kois JC. Altering gingival levels: the restorative connection. Part 1. Biologic variables. J Esthet Dent. 1994;6(1):3-9.
5. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontal. 1992;63(12):995-996.