Clinical Case Report Anterior Wear: Orthodontic and Restorative Management
John C. Kois, DMD, MSD; Brett C. Filder, DDS, MSD
Background
Age at Initial Presentation: 34
Initial Presentation: March 2003
Active Treatment Completed: June 2006
Medical History
The patient presented with an unremarkable medical history, except for exercise-induced asthma. He was a healthy male taking no medications and therefore had no medical contraindications for treatment.
Dental History
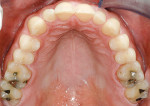
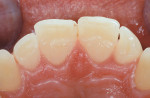
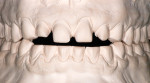
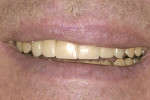
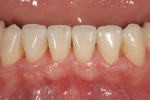
The patient presented with several concerns about his dental health. Most significantly, he was embarrassed to smile and his maxillary anterior teeth were “thinning” and chipping on the edges. These problems continued even though he was wearing a nightguard. He had experienced jaw problems for the past 10 years, including difficulty opening widely. He estimated having tension headaches once a month for 2 to 3 days and also described awakening with some teeth feeling sore. In addition, he was frustrated with his previous dental care because attempts to equilibrate his teeth had made him worse. He said his posterior teeth did not touch unless he clenched his teeth. When he removed his nightguard in the morning, he felt only his anterior teeth contact (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5, Figure 6, Figure 7, Figure 8, Figure 9, Figure 10, Figure 11).
Diagnostic Findings
Temporomandibular Joints (TMJ):
- Maximal opening 44 mm with normal range of movement and no deviation upon opening
- Bilateral joint sounds noted, Grade 1
- Load test negative
- Immobilization test negative
Extraoral: Within normal limits. Cancer screening negative.
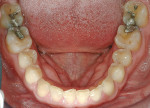
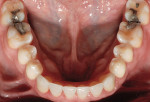
Intraoral: Bilateral mandibular lingual tori—approximately 10 mm x 5 mm (Figure 6).
Diagnosis
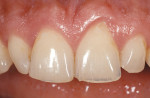
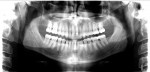
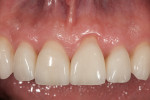
Periodontal: Mild chronic periodontitis, AAP type II. Probing depths were within normal limits without bleeding on probing. Bone support was within 2 mm of the cementoenamel junction (CEJ) without any infrabony defects. The gingival architecture was symmetrical except in regard to tooth No. 9, which had 2-mm apical recession (Figure 8).
Biomechanical: No caries, minimal erosion occlusal surface Nos. 19 and 30 (Figure 4, Figure 5 and Figure 6).
Functional: Moderate attrition lingual Nos. 6 to 11 and moderate attrition incisal/facial Nos. 22 to 27. Evidence for constricted chewing pattern and nocturnal bruxism (Figure 9, Figure 10, Figure 11).
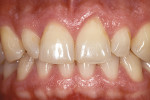
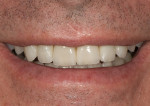
Dentofacial: Medium lip dynamics, unacceptable diastemas, maxillary tooth size discrepancies, acceptable color (Figure 3).
Risk Assessment
An individual risk assessment is critical to determine the most appropriate treatment plan, although there can be multiple treatment options. Only when the composites of the diagnostic categories are considered simultaneously and risk is reduced or prognosis is improved can interdisciplinary treatment be rendered successfully with the most promising survival probabilities.
Dentofacial: Moderate risk because of the medium lip dynamics, incomplete tooth display, and inability to display the gingival architecture. Exceeding the patient’s vision was more likely and less difficult (Figure 1, Figure 2, Figure 3).
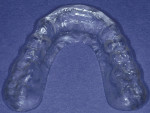
Functional: Moderate-to-high risk because of the combination of constricted chewing pattern and nocturnal bruxing. This required management of the occlusion to minimize ongoing friction and provide nighttime protection with appliance therapy for life (Figure 5, Figure 6, and Figure 9, Figure 10, Figure 11).
Biomechanical: Low risk because of no caries within 3 years, minimally restored teeth without structural compromises, and no shared risk factors. The patient was caries resistant (Figure 4).
Periodontal: Low risk because of slight bone loss and no shared risk factors for bone loss. The patient was resistant to periodontal disease (Figure 4).
Concerns
- How could the anterior teeth be managed to reduce the functional risk?
- How could his esthetic concerns be achieved without increasing the biomechanical risk? Reducing more tooth structure for restorative materials would remove more tooth structure than the patient may lose in his lifetime even without treatment. A key concern prior to initiating treatment was the fremitus on the anterior maxillary teeth. Increasing the horizontal parameter of overjet was expected to relieve the constricted envelope of function. The overjet change was more important for allowing normal function despite the increase in visual vertical display and increase of overbite relationship of anterior incisors. The vertical parameter of overbite was less a concern of function and more a concern of esthetics. Increased overbite as well as overjet was expected to result in improved esthetic and functional goals of treatment.
Treatment plan
Treatment options and goals were discussed with the patient. The patient’s primary objectives were to manage the continued loss of anterior tooth structure, improve esthetics, and eliminate the existing symptoms. To minimize the compromises to the healthy teeth that did not require restorative dentistry and to limit the restorative treatment to only the anterior teeth, orthodontics would be essential. Then occlusal management commensurate with veneers Nos. 6 to 11 and Nos. 22 to 27 would be accomplished.
Phase I: Orthodontics
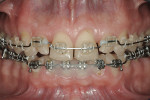
A complete facial evaluation and cephalometric analysis were made to create the proper space appropriation for normal tooth proportions and more favorable root inclination to reduce the interincisal angle. This was necessary to allow the mandibular anterior teeth to be repositioned behind the maxillary anterior teeth to minimize friction during chewing and to improve the esthetic outcome. To determine the magnitude of the movement necessary, the mandibular orthopedic reference position needed to be established. Following the use of the Kois Deprogrammer and the deprogramming protocol, it was determined that centric relation was actually anterior to the initial MIP. When a stable centric relation was confirmed, the incisal edge of the maxillary anterior teeth would need to be positioned 3 mm facially. In addition, the tooth position had to satisfy the functional concerns for anterior guidance by allowing space for the restorative material with minimal-to-no-further tooth preparation. Therefore, the mandibular anterior teeth also needed to be aligned and intruded (Figure 12 and Figure 13).
Phase II: Restorative
Following orthodontic therapy, 6 months of stabilization was necessary to allow for the mobility to resolve. During this time, it was necessary to maintain the anterior open bite with retainers. The patient was then equilibrated in the adapted centric posture position, Dawson Classification II, retaining the anterior open bite. The lingual of the maxillary anterior teeth would be managed with veneers Nos. 6 to 11 and the incisal edges of the mandibular incisors with veneers Nos. 22 to 27. The remaining tooth preparation was designed to meet the needs of the tooth by replacing the missing tooth structure for esthetics, not the needs of the restorative material (Figure 14). Otherwise, traditional tooth preparation would have unnecessarily increased the amount of tooth reduction and increased the biomechanical risk. Final impressions were made using a dual-phase, single-stage technique with light and putty viscosity vinyl polysiloxane (Impressiv, Cosmedent® Inc, Chicago, IL) according to the manufacturer’s instructions. Pro-visional restorations for Nos. 6 to 11 were made chairside with a methyl metharylate temporary crown-and-bridge resin) (DENTSPLY Caulk, Milford, DE) using an eggshell and subsequent direct reline (Figure 15). The provisional restoration for Nos. 22 to 27 was made chairside directly, using a Bis-GMA (Integrity®, DENTSPLY Caulk). The Kois Dento-facial Analyzer System (Panadent® Corp, Grand Terrace, CA) was used to communicate essential functional and esthetic parameters for the mounting of the maxillary provisional cast (Figure 16 A and Figure 16B, Figure 17A and Figure 17B, Figure 18A and Figure 18B). Jaw relation records were made in the MIP (which, following the equilibration, was now coincident with the mandible in adapted centric posture) using Jet Bite (Coltène/Whaledent Inc, Cuyahoga Falls, OH). Records, casts, final impressions, and digital photographs were transferred to the laboratory technician for the fabrication of the maxillary and mandibular anterior veneers. The platform on the articulator served as the natural head posture reference to ensure the symmetry of the incisal edge plane and horizontal and vertical tooth positions (Figure 16 A and Figure 16B, Figure 17A and Figure 17B, Figure 18A and Figure 18B). The veneers were luted, using the following adhesively retained protocol: The teeth were microabraded with 27-µm aluminous oxide with a PrepStart™ (Danville Engineering, Inc, San Ramon, CA) at 40 p.s.i., 0.015 tip. The teeth were etched with 37% phosphoric acid for 15 secs, and three layers of an unfilled adhesive resin (One-Step, Bisco Dental Products, Inc, Richmond, Canada) were applied and light-cured. The internals of the veneers were etched with HF acid, cleaned, silanated (3M Primer, 3M™ ESPE™, St. Paul, MN), and thoroughly dried. All veneers were luted with a photo-activated resin (RelyX™ Veneer, 3M ESPE, shade translucent) and cured with an LED light source (Figure 19, Figure 20, Figure 21, Figure 22, Figure 23, Figure 24, Figure 25). Following minor occlusal adjustment, a maxillary occlusal nightguard was fabricated (DB’s Dental Lab, Peters, MO) and seated.
Commentary
The final result exceeded the patient’s expectations (Figure 26 and Figure 27). By understanding the patient’s individual risk factors, treatment was designed to reduce or minimize any additional risk to the entire dentition. Alternative treatment options to manage the occlusal concerns with orthodontics could have been accomplished by increasing the occlusal vertical dimension. This would have created longer anterior teeth, which would have led to a less favorable esthetic outcome. Without orthodontics, increasing the occlusal vertical dimension would have required full-mouth rehabilitation. This would entail including all the posterior teeth, which would not otherwise be necessary and would have increased the biomechanical risk. Only the anterior teeth that were compromised by attrition and developmentally and esthetically compromised required restoration. All the necessary tooth preparation was kept in enamel, which further minimized additional biomechanical risks. Tooth preparation margin location was also maintained supragingivally, which did not contribute to any periodontal risks. The occlusal management resolved all the TMD symptoms from the constricted chewing pattern and eliminated the concerns of friction contributing to ongoing tooth structure loss. The nightguard, however, is still required to protect the restorations following any episodes of nocturnal bruxism. The patient is also on a 6-month recare interval for maintenance. The only anticipated liability is the restorations, ie, chipped porcelain, and not the remaining teeth. In conclusion, the patient’s periodontal and biomechanical prognosis remains good and has not changed. The dentofacial and functional prognoses were elevated from poor to good, provided the patient continues to wear the nightguard.
Acknowledgment
Laboratory support and ceramics by Leon Hermanides, Protea Dental Studios, Redmond, Washington.
Disclosure
Dr. Kois has a financial interest in the Panadent Dentofacial Analyzer.
About the Authors
John C. Kois, DMD, MSD; Director
Kois Center
Seattle, Washington
Private Practice
Tacoma, Washington
Brett C. Filder, DDS, MSD
Private Practice
Bellevue, Washington