Soft-Tissue Risk Assessment in Esthetic Restorative and Implant Dentistry: Smile Analysis, Gingival Esthetics, and Dental Implant Report
Eduardo R. Lorenzana, DDS, MS
Abstract
Thorough diagnosis of the esthetic requirements and ramifications of restorative and implant dentistry in the esthetic zone requires a standardized, methodical approach. Examination of the periodontal and peri-implant tissues is an essential component of this approach because overall gingival display, soft-tissue position and volume, and papilla quantity and quality can exert significant influence on overall implant position as well as the overall esthetic outcome. This article aims to present a method that can be used in daily clinical practice to consistently evaluate and document a patient's esthetic requirements. Smile analysis and smile design principles are used to identify relationships between a patient's face, smile, periodontium, and natural dentition in preparation for any periodontal–restorative or implant-supported reconstruction where esthetics is a priority. Periodontal plastic surgery concepts and techniques that may have intimate and/or complementary effects on the proposed restorative treatment plan are presented in an effort to shed light on the demands that each patient's smile and soft-tissue characteristics exert on overall esthetics.
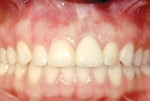
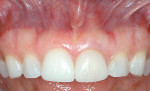
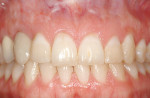
Clinical evaluation of risk in esthetic implant dentistry has been the subject of much discussion in the literature as the prevalence of implant-based reconstruction in the esthetic zone has risen.1-4 It is generally accepted by most clinicians that adequate soft-tissue quantity and quality is a prerequisite for a successful restoration, implant-supported or otherwise.5-8 Yet esthetic risk extends beyond the implant site, and undiagnosed and/or untreated soft-tissue deficiencies in the surrounding dental and periodontal structures can have just as much of a detrimental effect on the esthetic outcome as those directly associated with the dental implant unit itself (Figure 1). In other words, any assessment of risk involving implant dentistry can begin with the unit to be replaced, but it certainly cannot end there. Clinicians who fail to diagnose common deficiencies, such as an aberrant frenum, loss of attached gingiva, excessive gingival display, gingival asymmetry, gingival recession, alveolar ridge deficiencies, and loss of interdental hard/soft tissue, are risking an inadequate esthetic outcome.9 Periodontal plastic surgery concepts and techniques have evolved through research and clinical experience to address many of the aforementioned soft-tissue deficiencies, and their application to dental implant-based reconstruction can prove essential to achieving a satisfactory overall esthetic result.10,11
Research has shown that a person's smile has a significant effect on perceptions of one's attractiveness, personality, intelligence, and overall happiness.12,13 Therefore, the impact of treatment to be performed in the esthetic zone should not be taken lightly. Certainly one of the many challenges in any practice setting is the development of a systematic process for the documentation of clinical information critical to the formulation of a comprehensive esthetic treatment plan. For those clinicians unfamiliar with overall esthetic analysis and available soft-tissue enhancement techniques, this process can seem overwhelming. Surgical and prosthetic reconstruction in the esthetic zone is a process that requires close interaction between restorative and surgical professionals. Because most periodontal plastic surgery and dental implant patients originate with their restorative dentist, it is important that the restorative dentist be well versed on key esthetic variables and available surgical techniques to better prepare the patient for the surgical consultation. Such preparation cannot be underestimated, and the enhanced communication gives the patient further confidence in the restorative–surgical team.
This article presents a clinical risk assessment report, entitled the Smile Analysis, Gingival Esthetics, and Dental Implant Report (Figure 2), which serves as a diagnostic template or form that improves communication within the periodontal–restorative team. This report aims to assist any clinician seeking a greater awareness of smile analysis and gingival esthetics and how they complement conventional restorative and esthetic implant-based reconstructions. By providing a template for systematic documentation of each patient's clinical presentation, clinicians will be able to make an accurate assessment of esthetic risk and use it to formulate a comprehensive, customized treatment plan.
Smile Analysis, Gingival Esthetics, and Dental Implant Report
The origins of this report are found in a desire to formulate a concise yet thorough way to gather and share information on patients seeking periodontal and/or dental implant treatment impacting their esthetics. Its purpose is to incorporate an overall esthetic analysis14,15 and comprehensive assessment of common soft-tissue deficiencies16 with dental implant treatment planning. This serves to highlight the importance and impact of a thorough esthetic and soft-tissue analysis on dental implant therapy. The last point is of particular importance because the health, position, contour, form, quantity, quality, and color of the gingiva, central to the practice of periodontics, is also critical to the practice of implant dentistry, particularly in the esthetic zone.
Patient Information
Documentation of the patient's overall medical history is part of any practitioner's routine initial examination, so this report includes it in summary form only. Key questions, such as smoking habits and the need for premedication in accordance to physician's orders, are included for the purpose of communication with other members of the periodontal–restorative team and are not meant to supercede a comprehensive medical history questionnaire and thorough review with the patient. Central to any interview with a patient seeking treatment is documentation of the patient's chief complaint. Failure to address the main reason the patient sought treatment is a common criticism, and while further examination may elicit other, perhaps more pressing needs, these additional findings should be presented in the context of the patient's chief complaint. Finally, the question of time constraints can be an important factor when discussing treatment options and can help temper unreasonable expectations of treatment propagated by popular media.17,18
Facial Analysis
Facial analysis begins with the establishment of certain lines of reference. Deviations from the norm in how these reference lines relate to one another are the first step in diagnosing functional and esthetic discrepancies. The interpupillary line is generally accepted as the key horizontal plane of reference, but care should be taken in the establishment of the horizontal plane of reference because the interpupillary line is not always parallel to the horizon line (Figure 3).15 In the event that the interpupillary line and the horizon line fail to coincide, the patient and clinician together should decide on which line to base their horizontal frame of reference.19 The parallelism of the lip/incisal lines (and eventually the gingival line) is compared with the interpupillary line to document horizontal discrepancies in the patient's facial profile and possible divergence in the occlusal plane.20
The facial midline, as denoted by tracing a line through the glabella, the tip of the nose, the philtrum, and the tip of the chin, provides the vertical line of reference for the face and is perpendicular to the interpupillary or horizon line.15,21 Deviations of the facial midline are common, particularly in the midface region, but these are secondary to the parallelism of the horizontal reference lines, which provide the compositional cohesiveness that anchors pleasing facial esthetics (Figure 4).15,22 The key dental frame of reference, the facial midline, establishes or re-establishes the interincisal line.20 Deviations to either side of the midline should be noted, as well as lack of verticality of the interincisal line, which can draw unwanted attention to discrepancies in the patient's smile (Figure 5).19
Equal apportionment to the three major areas of the face as delineated by the hairline, the ophriac (eyebrow) line, the interalar line, and the tip of the chin is the key to a well-proportioned facial profile (Figure 6).15,20 Undoubtedly, the focus of the restorative team is on any deficiency in the lower third of the face, denoting a loss of vertical dimension to the occlusion. Recapturing the verticality of the lower third of the patient's face should be the focus of any analysis of facial proportionality.20
Smile Analysis
During smile analysis, the focus is on the elements that contribute to what is considered to be an esthetic smile. What exactly constitutes "esthetic" has been shown to be in the eye of the beholder19,23 and subject to outside influence, particularly from the popular media.18,24 Therefore, the documentation of the elements noted herein always needs to be tempered with the patient's expectations and opinion of what looks natural to them. It is also important to note that the dental office is not an environment most naturally suited to the analysis of the smile in the sense that a dental examination is seldom a relaxing experience for most patients. Therefore, an effort must be made to keep the atmosphere informal and friendly, so the patient feels comfortable and able to smile more freely, engaging all of the facial muscles involved in the act of smiling. A significant amount of information useful to an esthetic analysis can be gleaned during informal conversation when patients have let down their guard and are least aware that observations about their facial and perioral structures are being made.25
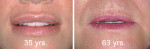
The first two notations in the Smile Analysis section involve recording the amount of central incisor display with the lips at rest and the amount of gingiva displayed at full smile. Incisal edge display with the lips at rest has been reported to range from 1 mm to 5 mm, with a normal range considered to be 2 mm to 4 mm for women and 1 mm to 3 mm for men.26,27 Vig and Brundo26 reported a mean incisal display for women of 3.4 mm vs 1.91 mm for men, and greater numbers for young patients (3.37 mm) vs middle-aged patients (1.26 mm). Several authors also have reported that these numbers generally decrease with advancing age, primarily caused by loss of muscle tone and incisal wear (Figure 7).27-29
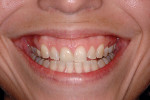
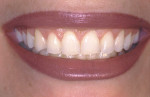
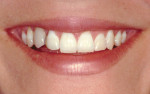
The aforementioned informal, conversational part of the exam is quite useful when attempting to record the amount of gingiva displayed at full smile. Most authors concur that gingival display in excess of 3 mm to 4 mm is considered un- esthetic.15,25,30 However, the significance of how much gingival exposure is too much depends on the patient and the clinician involved, with a range of acceptance from 1 mm to 4 mm.19,23 It appears that while there is such a thing as "excessive" gingival display, oftentimes the effect of the "gummy smile" can be mitigated by ensuring that the size and proportionality of the teeth displayed within the smile are as close to ideal as possible (Figure 8).
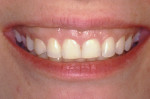
Next, the length of the upper lip, measured from the base of the nose to the inferior border of the upper lip, is recorded, with average measurements between 20 mm and 22 mm in women and 22 mm and 24 mm in men.31 Again, this measurement tends to increase as a patient ages, with increases in length reported up to 2 mm and concomitant decreases in maxillary central incisor display.29,22 A visual analysis of the height of the lip line also is recorded as low/medium/high (Figure 9). A low lip line exposes no more than 75% of the anterior teeth; a medium lip line exposes 75% to 100% of the anterior teeth, including interdental papillae; and a high lip line exposes the complete clinical crowns of the anterior teeth, with accompanying gingival tissue of varying height.32 The presence or absence of a midline deviation also is recorded in the manner described previously.
Visual determination of a cant or inclination to the occlusal plane is made in conjunction with noting the relationship of the upper incisal edges to the inferior commissural line. These annotations, taken together with the facial analysis of the interpupillary/horizon line, help identify any discrepancies of the occlusal plane (Figure 10). A significant inclination to the occlusal plane, if visually recognized, must be confirmed through the analysis of study casts mounted on a semi-adjustable articulator using a facebow transfer.33-36 The patient and restorative team should be prepared for multidisciplinary treatment, possibly requiring orthodontics, orthognathic surgery, and/or full-mouth rehabilitation. Care must be taken not to overtreat slight deviations from the horizontal plane, as these can be quite indispensable to the patient as part of his or her identity or personality.15,19
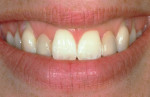
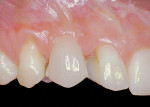
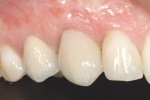
Finally, biotype determination is made by noting whether the patient displays a thick or thin biotype and whether the contour is flat or scalloped. Biotype is defined as a variation in tissue morphology because of tooth form.37-39 Many authors have correlated biotype with a difference in severity of periodontal signs and symptoms38,40,41 but, recently, biotype has emerged as an important factor in assessing risk in peri-implant esthetics.1-4,42-46 The prevailing concept regarding biotype and peri-implant esthetics is that a thin biotype is more prone to recession and loss of papilla height (Figure 11), while a thick biotype is more resistant to recession, yet scars more easily when incised vertically and is prone to increased pocket formation (Figure 12).1,2,45,46 Recent data has cast doubt on the likelihood of increased recession in thin-biotype patients, with proper three-dimensional implant position, particularly in the buccolingual aspect.47 However, being aware of the patient's biotype still can affect many esthetic variables including choice of implant components,4 soft-tissue grafting,48-50 esthetic crown lengthening,51 and three-dimensional implant position.3,4,47,51 Its inclusion in several of the aforementioned published esthetic risk analyses1-4,45 validates the importance of biotype classification in a thorough periodontal and peri-implant soft-issue risk assessment.
Gingival Esthetics
The portion of the report devoted to gingival esthetics focuses on the most common periodontal plastic surgery procedures likely to impact restorative outcomes: crown lengthening, soft-tissue augmentation, papilla augmentation, and ridge preservation/augmentation. Each section guides the clinician in obtaining the relevant clinical information necessary for interdisciplinary communication and execution, thereby minimizing esthetic risk and ensuring a successful outcome.
Crown Lengthening
Crown lengthening procedures traditionally have been applied in situations requiring additional tooth structure for restorative procedures, such as subgingival caries and fractures. The classic crown lengthening procedure involves gingivectomy and osseous recontouring to re-establish the biologic width at a more apical position.52-54 Authors have reported a minimal requirement of 3 mm to 5 mm of healthy supracrestal tooth structure to allow completion of restorative procedures.55-57 When crown lengthening is being considered in the esthetic zone because of a clinical observation of excessive gingival display, analysis of the functional and esthetic impact of the proposed procedure is indicated.
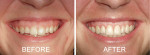
From the steps previously taken in the facial and dental analysis sections, a clinician should have been able to deduce the etiology of the excessive display, which can include altered passive eruption, vertical maxillary excess, short/hyperactive upper lip, dentoalveolar extrusion, or some combination thereof.52,58 Figure 13, Figure 14 and Figure 15 show a typical application of the crown lengthening section of the report as well as the before and after photographs of the corresponding patient.
Soft-Tissue Grafts
This section documents the locations where grafting is required and the relevant clinical information (ie, amount of recession, keratinized gingiva, total attachment loss), as well as the expected root coverage, and if a restoration is planned. Free epithelialized autogenous soft-tissue grafts are used primarily for extension of the zone of attached keratinized gingiva,59 but their use in root-coverage procedures60,61 has given way to the use of connective tissue grafting techniques because of the technique's improved predictability, esthetics, and versatility, and its diminished postoperative morbidity.62-67 The advent of allogeneic donor tissue and growth factors has resulted in many options for both clinicians and patients, depending on the clinical needs and limitations.68-71 Figure 16, Figure 17 and Figure 18 show a typical application of this section of the report and the corresponding clinical case.
Reduced Papilla Height/Volume
Using the guidelines set forth in the literature by Tarnow and colleagues71-72 and Choquet and colleagues,73 the papilla section of the report aims to systematically record the relevant factors affecting the height and volume of the interdental papilla. The position of the roots, interproximal bone height, location of contact points, volume of soft tissue, and need for orthodontics is recorded. Figure 19, Figure 20 and Figure 21 show an interdisciplinary case where a previous periodontal abscess and malpositioned teeth had resulted in a deficiency of the interdental papilla between teeth Nos. 8 and 9. After consultation with an orthodontist, the interdental area was grafted in a manner described by Azzi and colleagues,74 using autogenous connective tissue. Four weeks after the procedure, orthodontic treatment was begun to rotate and align the anterior teeth. Along with periodic adjustments, interdental stripping was performed to broaden the contact points and minimize the interdental spaces. Figure 22 shows the anterior teeth 2 years after tissue grafting and orthodontic treatment.
Ridge Preservation/Augmentation
This section includes information necessary to facilitate communication between the periodontal–restorative team when tooth removal is part of the treatment plan. Because loss of a tooth in the esthetic zone has the potential to be psychologically traumatic for a patient, coordination between the surgeon and restorative dentist to address not only the functional aspect of the planned treatment, but also the esthetic and psychological aspects, is paramount. The priority among these aspects is the manner in which the edentulous area will be provisionalized—removable partial denture, fixed partial denture, or implant-supported restoration. After the type of provisional is determined, the pontic design is determined and noted on the report as well as the need for future reshaping and timing of the definitive restoration.
Myriad techniques have been reported in the literature for ridge preservation75-77 and ridge augmentation,78-80 as well as the use of ovate pontics in conventional restorative and implant-supported reconstructions.81-83 It is not the objective of this article to review or comment on these techniques, but instead to emphasize the communication between team members to achieve the desired outcome.
Dental Implants
Documentation of clinical data relevant to the edentulous sites begins with noting the type of implant-supported restoration planned and a basic visual site evaluation. More definitive site evaluation needs to follow to confirm the clinical findings, including the use of study casts, diagnostic wax-ups, templates, and advanced radiography such as tomograms or computed tomography scans.84-86 The type of augmentation expected also is noted, along with the need for additional periodontal plastic surgery procedures including, but not limited to, crown lengthening and gingival grafting.
Case Report
A 35-year-old woman with a noncontributory medical history was referred for implant-supported replacement of a resin-retained fixed partial denture spanning teeth Nos. 5 through 7. The findings of the smile analysis, gingival esthetics, and dental implant sections of the report are shown in Figure 23. The patient's chief complaint was that her bridge of 15+ years was finally failing, and she could see that it was fractured and her teeth discolored from several attempts to repair and maintain the bridge. Initial facial analysis revealed her interpupillary line was generally parallel to her lip and incisal lines, but a 1.5-mm left incisal midline deviation from her facial midline was discovered. Her facial thirds were judged to be proportional.
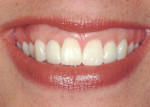
Smile analysis revealed 4 mm of incisal display with the lips at rest and 0 mm of gingival display (but papilla exposure) during full smile. Upper lip length was 20 mm and her lip line was judged to be medium (Figure 24). Her occlusal plane was judged to be generally parallel to the interpupillary line, with a reversed relationship to the lower lip at teeth Nos. 6 and 7. The patient attributed this to intrusion of tooth No. 7 after attempts to expose and guide the eruption of tooth No. 6. Finally, her tissue biotype was categorized as thick/scalloped.
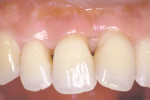
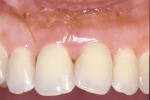
In the full retracted anterior view (Figure 25), aside from the planned replacement of tooth No. 6 with an implant, several soft-tissue abnormalities were noted that could have an effect on the overall esthetic result. Among these, a discrepancy was noted in the tissue heights on teeth Nos. 7 and 10, with No. 7 positioned further apically because of the aforementioned intrusion. The proposed remedy was crown lengthening of tooth No. 10 and orthodontic extrusion of tooth No. 7, which was declined by the patient. A related observation was the papilla deficiency between teeth Nos. 6 and 7 where orthodontics could have aided in improved root position, interproximal bone position, and soft tissue position, but again, the patient ruled out orthodontics. Additional findings included marginal tissue recession on tooth No. 5, where a full-coverage restoration was planned, as well as the need for soft- and hard-tissue augmentation on the facial of tooth No. 6 to eliminate the need for a ridge lap, augment the implant site, and simulate a root prominence (Figure 26).
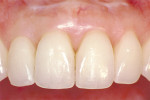
The information gathered during the examination was used to formulate the treatment plan, including implant placement and ridge augmentation at site No. 6, crown lengthening of tooth No. 10, the repositioning of the flap of tooth No. 5 coronally, and papilla augmentation between teeth Nos. 6 and 7. Additional restorative procedures included provisionalization of tooth No. 5, a bonded resin restoration on the distal of tooth No. 7, and guided tissue shaping to create the desired emergence profile and interdental papilla before taking the final impression. Figure 27, Figure 28 and Figure 29 show the final results.
Discussion
There are certain general esthetic objectives that are universal: that the smile should expose minimal gingiva, that the gingival contour should be symmetric and in harmony with the upper lip, that the incisal edges should generally follow the contour of the lower lip, that the anterior and posterior segments should be in harmony, and that the teeth should be of normal length.52 Guidelines like these are excellent, but the periodontal–restorative team attempting to follow these guidelines needs a way to collect and organize the raw clinical data necessary to help formulate a cohesive treatment plan that addresses the chosen esthetic objectives. The use of the report detailed herein is but one way to try to help clinicians accomplish that goal in a more organized and deliberate fashion. By presenting this report, it is hoped that it will be a relevant starting point for those seeking such a resource.
The reconciliation of esthetic and gingival analyses with dental implant treatment is one of the most important aspects contained herein, because this is a rapidly developing focus of research and clinical practice, and because patients are more educated than ever before about dental treatment and are more demanding in their expectations. When confronted with the loss of a tooth or teeth within the esthetic zone, they seek the replacement of that unit in the most natural way possible. The management of the peri-implant soft tissues has been described as a "balancing act" between the periodontal implant surgeon and the restorative dentist in the service of both the patient's expectations and the biological realities of predictable treatment results.87 By incorporating dental implant treatment considerations intimately into smile analysis and gingival esthetics concepts and techniques, it is expected that a more comprehensive view of periodontal plastic surgery and dental implant treatment emerges and becomes the standard of care in the clinical setting.
References
1. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001;22(3):199-206.
2. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-900.
3. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19(Suppl):43-61.
4. Martin W, Morton D, Buser D. Pre-operative analysis and prosthetic treatment planning in esthetic implant dentistry. In: Buser D, Belser U, Wismeijer D, eds. ITI Treatment Guide, Vol. 1. Implant Therapy in the Esthetic Zone: Single Tooth Replacements. Chicago, IL: Quintessence; 2007:9-24.
5. Belser UC, Bernard JP, Buser D. Implant-supported restorations in the anterior region: prosthetic considerations. Pract Periodontics Aesthet Dent. 1996;8(9):875-883.
6. Belser UC, Buser D, Hess D, et al. Aesthetic implant restorations in partially edentulous patients—a critical appraisal. Periodontol 2000. 1998;17:132-150.
7. Maynard JG Jr, Wilson RD. Physiologic dimensions of the periodontium significant to the restorative dentist. J Periodontol. 1979;50(4):170-174.
8. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
9. Miller PD Jr. Regenerative and reconstructive periodontal plastic surgery. Mucogingival surgery. Dent Clin North Am. 1988;32(2):287-306.
10. Miller PD Jr, Allen EP. The development of periodontal plastic surgery. Periodontology 2000. 1996;11:7-17.
11. Israelson H, Plemons JM. Dental implants, regenerative techniques, and periodontal plastic surgery to restore maxillary anterior esthetics. Int J Oral Maxillofac Implants. 1993;8(5):555-561.
12. Otta E, Folladore Abrosio F, Hoshino RL. Reading a smiling face: messages conveyed by various forms of smiling. Percept Mot Skills. 1996;82(3 Pt 2):1111-1121.
13. Beall AE. Can a new smile make you look more intelligent and successful? Dent Clin North Am. 2007;51(2):289-297.
14. Fradeani M. Esthetic Rehabilitation in Fixed Prosthodontics. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Chicago, IL: Quintessence; 2004:323-334.
15. Chiche GJ, Pinault A. Artistic and scientific principles applied to esthetic dentistry. In: Chiche GJ, Pinault A, eds. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence; 1994:13-32.
16. McGuire MK. Periodontal plastic surgery. Dent Clin North Am. 1998;42(3):411-465.
17. Theobald AH, Wong BK, Quick AN, et al. The impact of the popular media on cosmetic dentistry. N Z Dent J. 2006;102(3):58-63.
18. Crockett RJ, Pruzinsky T, Persing JA. The influence of plastic surgery "reality TV" on cosmetic surgery patient expectations and decision making. Plast Reconstr Surg. 2007;120(1):316-324.
19. Kokich VO Jr, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. J Esthet Dent. 1999;11(6):311-324.
20. Facial analysis. In: Fradeani M. Esthetic Rehabilitation in Fixed Prosthodontics. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Chicago, IL: Quintessence; 2004:34-61.
21. Moskowitz M, Nayyar A. Determinants of dental esthetics: a rationale for smile analysis and treatment. Compend Contin Educ Dent. 1995:16(12):1164-1186.
22. Ahmad I. Geometric considerations in anterior dental aesthetics: restorative principles. Pract Periodontics Aesthet Dent. 1998;10(7):813-822.
23. Pinho S, Ciriaco C, Faber J, et al. Impact of dental asymmetries on the perception of smile esthetics. Am J Orthod Dentofacial Orthop. 2007;132(6):748-753.
24. Geron S, Atalia W. Influence of sex on the perception of oral and smile esthetics with different gingival display and incisal plane inclination. Angle Orthod. 2005;75(5):778-784.
25. Dentolabial analysis. In: Fradeani M. Esthetic Rehabilitation in Fixed Prosthodontics. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Chicago, IL: Quintessence; 2004:62-114.
26. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
27. Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning—Part I. Am J Orthod Dentofac Orthop. 1993;103(4):299-312.
28. Qualtrough AJ, Burke FJ. A look at dental esthetics. Quintessence Int. 1994;25(1):7-14.
29. Fudalej P. Long-term changes of the upper lip position relative to the incisal edge. Am J Orthod Dentofacial Orthop. 2008;133(2):204-209.
30. Allen EP. Use of mucogingival surgical procedures to enhance esthetics. Dent Clin North Am. 1988;32(2):307-330.
31. Peck S, Peck L. Facial realities and oral esthetics. In: McNamara JA, ed. Esthetics and the Treatment of Facial Form. Craniofacial Growth Series, Vol. 28. Ann Arbor, MI: Center for Human Growth and Development, University of Michigan; 1993:97.
32. Tjan AHL, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51(1):24-28.
33. Schillingburg HT Jr, Hobo S, Whitsett LD. Fundamentals of Fixed Prosthodontics. 2nd ed. Chicago, IL: Quintessence; 1981:55-78.
34. Schallhorn RG. A study of the arbitrary center and the kinematic center of rotation for face-bow mountings. J Prosthet Dent. 1957;7:162-169.
35. Teteruck WR, Lundeen HC. The accuracy of an ear face-bow. J Prosthet Dent. 1966;16(6):1039-1046.
36. Whitsett LD, Shillingburg HT Jr, Keenan MP. Modifications of a new semi-adjustable articulator for use with a caliper style ear face-bow. J Calif Dent Assoc. 1977;5(4):32-38.
37. Seibert JS. Surgical management of osseous defects. In: Goldman HM, Cohen DW, eds. Periodontal Therapy. 5th ed. St. Louis, MO: CV Mosby; 1973:765-766.
38. Weisgold A. Contours of the full crown restoration. Alpha Omegan. 1977;7(3):77-89.
39. Kay HB. Esthetic considerations in the definitive periodontal prosthetic management of the maxillary anterior segment. Int J Periodontics Restorative Dent. 1982;2(3):44-59.
40. Seibert JS, Lindhe J. Esthetics and periodontal therapy. In: Lindhe J, ed. Textbook of Clinical Periodontology. 2nd ed. Copenhagen: Munksgaard; 1989:477-514.
41. Olsson M, Lindhe J. Periodontal characteristics in individuals with varying form of the upper central incisors. J Clin Periodontol. 1991;18(1):78-82.
42. Becker W, Ochsenbein C, Tibbetts L, et al. Alveolar bone anatomic profiles as measured from dry skulls. Clinical ramifications. J Clin Periodontol. 1997;24(10):727-731.
43. Kan JY, Rungcharassaeng K. Site development for anterior single implant esthetics: the dentulous site. Compend Contin Educ Dent. 2001;22(3):221-232.
44. Kan JY, Rungcharassaeng K, Umezu K, et al. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):557-562.
45. Sclar AG. Systematic evaluation of the esthetic patient. In: Sclar AG. Soft Tissue and Esthetic Considerations in Implant Therapy. Chicago, IL: Quintessence; 2003:24-29.
46. Fugazzotto PA. Treatment options following single-rooted tooth removal: a literature review and proposed hierarchy of treatment selection. J Periodontol. 2005;76(5):821-831.
47. Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Impl Res. 2008;19(1):73-80.
48. Kan JY, Rungcharassaeng K, Lozada JL. Bilaminar subepithelial connective tissue grafts for immediate implant placement and provisionalization in the esthetic zone. J Calif Dent Assoc. 2005;33(11):865-871.
49. Beagle JR. Developing keratinized mucosa around non-submerged ITI dental implants. Part II: the subepithelial connective tissue graft. Implant Realities. 2003;1(3):22-24.
50. Silverstein LH, Lefkove MD. The use of the subepithelial connective tissue graft to enhance both the aesthetics and periodontal contours surrounding dental implants. J Oral Implantol. 1994;20(2):135-138.
51. Lorenzana ER, Gillespie JG, Martin W, et al. Altered passive eruption in conjunction with implant placement in the esthetic zone. Implant Realities. In press.
52. Allen EP. Surgical crown lengthening for function and esthetics. Dent Clin North Am. 1993;37(2):163-179.
53. Gargiulo AW, Wentz FM, Orban BJ. Dimensions and relation of the dentogingival junction in humans. J Periodontol. 1961;32:261-267.
54. Vacek JS, Gher ME, Assad DA, et al. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent. 1994;14(2):154-165.
55. Ingber JS, Rose LF, Coslet JG. The "biologic width"—a concept in periodontics and restorative dentistry. Alpha Omegan. 1977;70(3):62-65.
56. Rosenberg ES, Garber DA, Evian CI. Tooth lengthening procedures. Compend Contin Educ Dent. 1980;1(3):161-172.
57. Wagenberg BD, Eskow RN, Langer B. Exposing adequate tooth structure for restorative dentistry. Int J Periodontics Restorative Dent. 1989;9(5):322-331.
58. Dolt AH 3rd, Robbins JW. Altered passive eruption: an etiology of short clinical crowns. Quintessence Int. 1997;28(6):363-372.
59. Sullivan HC, Atkins JH. The role of free gingival grafts in periodontal therapy. Dent Clin North Am. 1969;13(1):133-148.
60. Miller PD Jr. Root coverage using a free soft tissue autograft following citric acid application. Part I: technique. Int J Periodontics Restorative Dent. 1982;2(1):65-70.
61. Holbrook T, Ochsenbein C. Complete coverage of the denuded root surface with a one-stage gingival graft. Int J Periodontics Restorative Dent. 1983;3(3):8-27.
62. Allen AL. Use of the supraperiosteal envelope in soft tissue grafting for root coverage. II. Clinical results. Int J Periodontics Restorative Dent. 1994;14(4):302-315.
63. Levine RA. Covering denuded maxillary root surfaces with the subepithelial connective tissue graft. Compend Contin Educ Dent. 1991;12(8):568-572.
64. Harris RJ. Root coverage with connective tissue grafts: an evaluation of short- and long-term results. J Periodontol. 2002;73(9):1054-1059.
65. Wennström JL. Mucogingival therapy. Ann Periodontol. 1996;1(1):671-701.
66. Lorenzana ER, Allen EP. The single-incision palatal harvest technique: a strategy for esthetics and patient comfort. Int J Periodontics Restorative Dent. 2000;20(3):297-305.
67. Lorenzana ER, Rees TD, Hallmon WW. Esthetic management of multiple recession defects in a patient with cicatricial pemphigoid. J Periodontol. 2001;72(2):230-237.
68. Allen EP. AlloDerm: an effective alternative to palatal donor tissue for treatment of gingival recession. Dent Today. 2006;25(1):48-52.
69. Cummings LC, Kaldahl WB, Allen EP. Histologic evaluation of autogenous connective tissue and acellular dermal matrix grafts in humans. J Periodontol. 2005;76(2):178-186.
70. McGuire MK, Scheyer ET. Comparison of recombinant human platelet-derived growth factor-BB plus beta tricalcium phosphate and a collagen membrane to subepithelial connective tissue grafting for the treatment of recession defects: a case series. Int J Periodont Restorative Dent. 2006;26(2):127-133.
71. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996.
72. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
73. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
74. Azzi R, Etienne D, Sauvan JL, et al. Root coverage and papilla reconstruction in class IV recession: a case report. Int J Periodontics Restorative Dent. 1999;19(5):449-455.
75. Keith JD Jr, Salama MA. Ridge preservation and augmentation using regenerative materials to enhance implant predictability and esthetics. Compend Contin Educ Dent. 2007;28(11):614-21.
76. Iasella JM, Greenwell H, Miller RL, et al. Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. J Periodontol. 2003;74(7):990-999.
77. Fiorellini JP, Nevins ML. Localized ridge augmentation/preservation. A systematic review. Ann Periodontol. 2003;8(1):321-327.
78. von Arx T, Buser D. Horizontal ridge augmentation using autogenous block grafts and the guided bone regeneration technique with collagen membranes: a clinical study with 42 patients. Clin Oral Implants Res. 2006;17(4):359-366.
79. Proussaefs P, Lozada J. Use of titanium mesh for staged localized alveolar ridge augmentation: clinical and histologic-histomorphometric evaluation. J Oral Implantol. 2006;32(5):237-247.
80. Buser D, Dula K, Hess D, et al. Localized ridge augmentation with autografts and barrier membranes. Periodontol 2000. 1999;19:151-163.
81. Orsini G, Murmura G, Artese L, et al. Tissue healing under provisional restorations with ovate pontics: a pilot human histological study. J Prosthet Dent. 2006;96(4):252-257.
82. Kan JY, Rungcharassaeng K, Kois JC. Removable ovate pontic for peri-implant architecture preservation during immediate implant placement. Pract Proced Aesthet Dent. 2001;13(9):711-715.
83. Spear FM. Maintenance of the interdental papilla following anterior tooth removal. Pract Periodontics Aesthet Dent. 1999;11(1):21-28.
84. Higginbottom FL, Wilson TG Jr. Three-dimensional templates for placement of root-form dental implants: a technical note. Int J Oral Maxillofac Implants. 1996;11(6):787-793.
85. Garber DA, Belser UC. Restoration-driven implant placement with restoration-generated site development. Compend Contin Educ Dent. 1995;16(8):796-804.
86. Van Assche N, van Steenberghe D, Guerrero ME, et al. Accuracy of implant placement based on pre-surgical planning of three-dimensional cone-beam images: a pilot study. J Clin Periodontol. 2007;34(9):816-821.
87. Levine RA. Soft tissue considerations for optimizing implant esthetics. Functional Esthetics & Restorative Dentistry. 2007;1(2):54-62.
About the Author
Eduardo R. Lorenzana, DDS, MS
Adjunct Assistant Professor, Graduate Periodontics
The University of Texas Health Science Center
San Antonio, Texas
Private Practice
San Antonio, Texas