Trends in Dentistry 2021
Making sense of unusual times for clinicians
Jason Mazda
Predictability is one of the primary goals that dental professionals strive to achieve, not only in clinical cases but in the operation of their businesses as well. Unfortunately, as we approach the 2-year anniversary of when the COVID-19 pandemic hit the United States, unpredictability reigns supreme. Dental practices across the country have been busy as patients returned to their chairs with more disposable income, but will it last? Adoption rates for certain technologies continue to climb, but dentists are still closely monitoring costs and, in some cases, limiting capital investments. And amid these and other pandemic-related concerns, dentistry is facing its own unique challenges in dealing with the staffing shortages that have plagued the country as a whole.
Inside Dental Technology has always believed that keeping a finger firmly on the pulse of the clinical side of the profession can help dental laboratory professionals better develop and adapt their own strategies, both at the bench and at the desk. In that spirit, our annual Trends in Dentistry feature presents carefully collated data from Inside Dentistry readership surveys on various aspects of the profession, including business, clinical, product, and collaboration trends, as well as select data from other sources.* "We could spend a week discussing what all of this means," says Inside Dentistry Editorial Advisory Board member Roger P. Levin, DDS, CEO of the Levin Group. Indeed, the discussion will continue beyond these pages—you're invited to a free live streaming CE event, "Trends: The Inside Look with Dr. DiTolla and Friends," on Wednesday, December 8, from 6 PM to 8 PM ET.
*All data are from Inside Dentistry surveys unless otherwise indicated.
Business Is Good
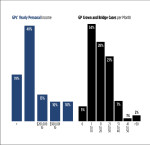
Approximately 81% of the general practitioners (GPs) who responded to this year's Inside Dentistry survey reported a personal yearly income of $100,000 or higher, with 19% at $300,000 or higher. Those numbers are up from 73% and 14%, respectively, last year. Approximately 50% of responding GPs indicated that they are treating more than 75 total patients per week, compared with 43% last year, and about 59% reported that they treat more than 10 new patients per week, which is the same percentage as last year.
The American Dental Association's Health Policy Institute (HPI) found that 100% of the practices that responded to its October 2021 survey were open, with 65% reporting "business as usual." Anecdotally, many dentists say that the peaks and valleys that were predicted a year ago have not materialized and that business has been steadily strong. That business has trickled down to many laboratories. "I was skeptical as to the future of our business and our niche implant solution," says Inside Dental Technology Editorial Advisory Board member Arian Deutsch, CDT, Owner of Deutsch Dental Arts in Sun City West, Arizona. "Instead of being slow, we are busier than ever before. The full-arch implant rehabilitations market is booming."
Levin cautions, however, that it may not last. "We are in an altered business universe," he explains. "Most practices are very busy due to what I call the ‘pandemic effect.' This will not last more than 6 to 18 months. Many people are not spending in traditional places, so they have more money for dentistry. But dentists should not assume that this will continue."
Pandemic factors aside, Levin notes that, per the Levin Group's statistical analysis, a large percentage of practice owners are not making as much money as they could or should be. "Any dental practice owner with a pretax personal income below $250,000 should absolutely overhaul his or her practice," Levin says. "The average retirement age of a dentist is about 72 and rising. Five years from now, I believe that it will be 74 or 75, in part because of student loan debt. You need to get a return on your education."
According to HPI, as of October, 20% of dentists had raised fees to maintain financial sustainability, 6% downsized their teams, 12% reduced team hours, and 9% borrowed money from a bank. In addition, 38% of dentists who responded to HPI's survey reported that they felt very confident in the recovery of their practices, whereas 36% reported that they felt somewhat confident, 14% indicated neither confident nor skeptical, and 12% reported that they were somewhat or very skeptical.
One key way for a practice to increase its production is to maximize case acceptance for complex treatment plans. Approximately 44% of responding GPs reported that no more than half of their complex treatment plans are accepted. "Most practices are very successful with simple treatment plans, but their acceptance rates fall off dramatically as the size of the case and the fee for the case increase. It is not that they cannot perform complex treatments clinically, but rather that they cannot sell them," Levin says. "We are entering a new era in dentistry with dental insurance reimbursements dropping and volume in some practices dropping. As dentistry becomes more competitive, achieving higher acceptance rates for larger cases is an excellent way to increase practice production."
One hindrance to progress is a staffing shortage. The HPI survey found that 24% of dentists "definitely" planned to hire more staff by early January and that 25% indicated "maybe." However, about 9% of the responding dental hygienists surveyed by HPI and the American Dental Hygienists' Association were not working as of August, with 74% of them reporting that they left their positions voluntarily.
"We believe that this is a staffing crisis," Levin says," and that it will last for at least 5 to 8 years. Our shortage is worse than those of many other industries due to several factors, including the formal qualifications required for dental hygienists and certified assistants, competition from other industries that pay more and offer better benefits, the fact that more women are leaving the workforce than men during the pandemic, and the training challenges brought on by advancements in technology."
Clinical Progress
A rise in cosmetic dentistry has been one of the dominant themes of the pandemic.
"Suddenly, people care about their teeth more," says Inside Dentistry Restorative Section Editor Amanda N. Seay, DDS, a private practitioner in Mount Pleasant, South Carolina. "Maybe it is because they are seeing themselves on the computer screen more than they ever have before. What I find interesting is that, in previous cosmetic consultations, patients always showed me pictures of themselves smiling and discussed ways to improve their smiles. More recently, there has been a big push for clear aligner therapy and whitening; people are saying that they don't like what they see while they are talking, which is very different."
Despite a number of new delivery models for clear aligner treatment, some of which involve third-party laboratories, 62% of dentists surveyed reported that clear aligners should only be handled in person, 21% indicated that certain at-home aligner services that involve clinician partners are beneficial options, and 17% noted that, in general, at-home services expand access to care and are a good option for patients. "It is a marketplace that probably will not go away, but dentistry is not a commodity—time, skill, and judgment are elements that are missing from these direct-to-consumer services," Seay says. "Services that involve in-person visits along with ‘virtual care' do work, but how simplified do we need to make things? Are we really the generation that cannot even visit the dentist one or two times for orthodontic treatment?"
Among other procedures, approximately 60% of GP respondents reported that they perform more than 10 crown and bridge cases per month, and 56% indicated that they place implants—down from 76% and 69%, respectively, last year. And of the GP respondents in practice for 10 years or less, only 40% reported that they place implants.
"You might think that young graduates would want to jump right into placing implants, but that comes with becoming a seasoned practice owner or practitioner who can afford to acquire the necessary education," Seay says. "That also goes for clear aligners, digital smile design, and more—practitioners slowly incorporate those services. Surgery is one of the last ones, typically, because the necessary CE and training take more time."
Approximately 33% of the GPs indicated that they treat sleep apnea patients. Seay says that area continues to evolve as more is understood about airway management. "There is still so much confusion in the science and literature of sleep," she says. "Sleep issues and airway issues are completely different. Putting appliances in patients' mouths is not really fixing the problem. When you treat the airway, you are moving the anatomy—the teeth, tongue, jaw, and facial structures. This is a big paradigm shift in how we think as clinicians. More of us are learning; however, it is hard to say whether the field is growing because there are two segments: dentists who are shifting their focus from sleep to airway and dentists who are primarily only providing sleep appliances to these patients."
Collaboration Through Communication
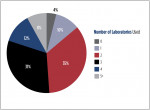
Advances in communication technology have enabled dentists to be more connected than ever with laboratories, and as a result, collaboration is as important as ever in providing optimal patient care on restorative cases. Approximately 72% of the respondents who do indirect restorative work reported that they exclusively use outside laboratories, 4% employ a dental technician or technicians, 16% mill restorations themselves, 2% use 3D printers to fabricate models and other products but do not mill restorations, and 11% do analog laboratory work. Among the respondents who use outside laboratories, 53% use three or more, and only 9% reported that any of their laboratory work is done overseas, which is down from 12% last year.
"The pandemic probably contributed to less work being sent overseas," says Inside Dental Technology Editorial Advisory Board member Gregg A. Helvey, DDS, CDT, a private practitioner and adjunct associate professor at the Virginia Commonwealth University School of Dentistry. "That would have changed my thinking if I had been sending work overseas."
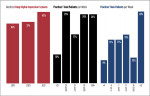
Approximately 64% of respondents reported that it is either paramount or very important to use a laboratory whose technicians graduated from an accredited dental technology program, whereas 27% indicated that it is somewhat important, and 9% indicated that it is not important. A clear trend exists in which more experienced dentists are more likely to place an importance on graduation from an accredited program. Among those who reported that it is paramount or very important, 68% were in practice more than 20 years, 59% for 11 to 20 years, 55% for 6 to 10 years, and 50% for 5 years or less.
"Veteran dentists have experienced situations when the laboratory has helped them, as well as situations when the laboratory has not helped, so we appreciate being able to depend on someone with more education in the dental field," says Helvey, who does most of his own laboratory work but works with an outside partner for zirconia, dentures, partial dentures, and aligners. "Newer dentists, as they try to keep up with the newest technology, may place more value on a laboratory's ability to help with software as opposed to more of an engineering or mechanical approach to making a good restoration, but experience and exposure often change that."
Deutsch notes that even though a sizable portion of dentists appreciate formally educated technicians, problems persist in that area of the profession.
"Our clients definitely place value on working with a technical team that is well educated in their craft," Deutsch says. "I do find that many dentists, however, do not fully understand the challenges that technicians face in terms of getting educated as dental technology programs continue to close their doors across the country. If they knew that many of their own state dental associations fight against requiring a CDT-designated technician to be employed at a dental laboratory in their state, we might start to see some support from individual clinicians."
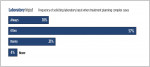
Effective collaboration, particularly for complex and/or esthetic cases, involves more than just high-quality work. The communication is critical. Approximately 75% of the total respondents and 89% of those in practice for 10 years or less reported that they always or often solicit the laboratory's input when treatment planning complex cases.
"When I prepare teeth for restorations such as anterior veneers, I am already thinking about the laboratory work involved," Helvey says. "How will I get porcelain from the front to the back without making any changes that would cause fracture points in the ceramic? Do I have enough clearance? In an ideal world, all dentists would learn that perspective in dental school; however, at the very least, communicating with the laboratory early in a case is important."
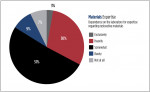
Relatedly, about 33% of the responding dentists indicated that they depend heavily or exclusively on their laboratories for expertise regarding restorative materials, and 51% indicated that they depend on them somewhat.
"Valuing and considering the laboratory's technical expertise is extremely important, but this can be a double-edged sword," Deutsch says. "Many times, there is almost too much reliance on the technician's expertise in treatment planning. There is a need for balance. I have seen some laboratories engage in what I feel is an ‘enabling' approach—catering to every whim of the dentists and in many cases overstepping their legal boundaries on chairside conversions, placing multi-unit abutments during surgery, etc. I have always wanted to empower my clients to take ownership of their practices, their clinical work, and their knowledge so that they can become better clinicians and have a well-rounded understanding of restorative steps, techniques, and materials. At the end of the day, clients who are empowered by their technical teams become very cohesive and appreciative in the long term."
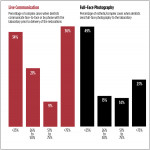
Despite the heavy dependence on laboratories in so many cases, only about 46% of the respondents reported that they communicate face-to-face or by phone with the laboratory prior to the delivery of restorations for more than half of their complex cases.
"In-person communication is the most effective, followed by video chat and then phone conversations, so I would like to see that number higher," Deutsch says.
Regarding visual communication, 37% of the total respondents reported that they send full-face photographs of the patient to the laboratory for more than half of their esthetic or complex cases, whereas 49% reported that they do so less than one-quarter of the time.
"The laboratory really cannot evaluate the mid-face cant with just a photograph from nose to chin," Helvey says. "The midline profile needs to run all the way from chin to forehead. If the laboratory only has a model, they have no choice but to orient it so the maxillary canines are at an equal level, even though they usually are not. All of the other interproximal lines are based off the mid-face cant. Without a facebow or full-face portrait, you tie the hands of the technician; it is like asking them to match a shade off a stone model."
Newer dentists do trend toward increased communication. Approximately 52% of those in practice for 10 years or less reported sending full-face photographs for more than half of their esthetic or complex cases, which is contrasted by those with more than 10 years of experience, of which only 33% reported sending full-face photographs.
"That number should be much higher," Deutsch says. "Both dental laboratories and dentists need to do better. The way we have addressed it is by requiring photographs with cases and firmly refusing any case for which the dentist is not willing to provide photography. In this day and age, there is no excuse to not provide photographs with a case."
Product Progress
The pandemic's impact on purchasing has been wide ranging. Since the unprecedented shutdown in early 2020, budgets have certainly come under greater scrutiny, but in many cases, technology can offer solutions to pandemic-related issues. In 2019, 53% of the responding dentists reported that they spent more than 10% of their yearly practice budget on new technology. That number jumped to 56% last year before falling to 47% this year. Among the respondents in practice for 5 years or less, only 42% reported that they spend more than 10% of their budget on new technology. This is down from 73% last year—an indicator that newer dentists with tight budgets may have felt the squeeze more than others.
At the same time, 43% of this year's respondents report that they use digital impression systems, which is up from 37% last year and 36% in 2019 (notably, Inside Dentistry's surveys are conducted via email and thus likely target a more tech-savvy segment). "Many more people are starting to see the ROI on intraoral scanners," says Inside Dentistry Editorial Advisory Board member Chad C. Duplantis, DDS, a private practitioner in Fort Worth, Texas.
Approximately 28% of the respondents indicated that they use cone-beam computed tomography (CBCT). For those in practice 5 years or less, this number jumps to 47%. "Everybody needs some sort of panoramic radiograph, so when a dentist is considering that purchase, a standalone digital unit is often less appealing than one that includes CBCT at just a slightly higher cost," Duplantis says.
Approximately 18% of respondents indicated that they have integrated some artificial intelligence (AI) modules into their workflows. Another 19% reported that they are monitoring the developments and considering adding AI, 47% reported that they may be open to it, and 16% reported that they do not believe AI is a fit for their practice. "The opportunities for AI in dentistry are endless," Duplantis says. "Currently, the CAD applications are growing exponentially, and the time savings for digital design are incredible. More manufacturers are incorporating more AI into their software applications, and it will continue to reach different areas of the dental practice."
The sources for purchasing supplies are evolving as well. About 22% of the total respondents and 31% of those in practice for 10 years or less reported that they participate in a group purchasing organization or buying group for purchasing dental supplies. In addition, 82% of respondents indicated that they utilize dealer websites for purchasing, 64% use manufacturer websites, 44% use Amazon, and 30% use other e-commerce websites. Comparatively, among those in practice 10 years or less, 50% reported that they use Amazon and 39% use other e-commerce sites.
"Especially now with inflation as high as it is, we will see more and more dentists looking for ways to decrease their overhead, and one of the primary ways is to save on supplies," Duplantis says. "The majority of distributors do have some sort of formulary that dentists can use for discounts. I believe that trend will absolutely continue, and there will be many new avenues for dentists to purchase discount supplies and dispensable goods."
What's Next?
As the pandemic shows no signs of abating, uncertainty will likely remain. Increased amounts of disposable income among patients have in many cases been accompanied by lower overall patient volume, but which of those conditions is likely to last longer? "Many patients have not come back yet from the pandemic, and whenever patients leave the system, some of them stay out," Levin says. "Staff shortages also complicate the issue, and although a majority of practices have figured out infection control, it has slowed down many."
At the same time, manufacturers are continuing to produce innovative new technologies that offer a lucrative enough ROI that dentists are investing in them. "Some of this technology investment can be attributed to stimulus money," Duplantis says. "The other likely factor is that we need to get creative and find ways to help our patients in a more cost-effective manner."
No matter how uncertain the times, how unusual the circumstances, or how unconventional the strategies, the goal remains the same: to do what is best for the patient.