A Future-Proof Digital Denture Workflow
Making digital dentures make sense
Andrew C. Johnson, DDS, MDS, CDT
Despite the many years of development so far, we are still on the front end of an active revolution in removable prosthetic dentistry. Even with the many advantages in terms of strength, durability, fit, biocompatibility, and reproducibility, digital dentures are still relatively rare in comparison to traditionally fabricated prosthetics. While digital denture design and production technology has advanced tremendously over the past decade—from scanning to milling to 3D printing, etc—it seems to have had relatively little impact so far on the customary clinical workflow.
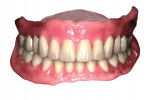
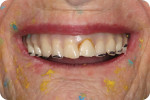
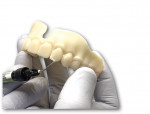
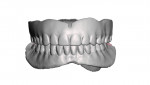
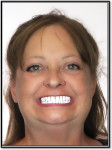
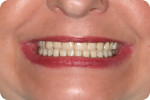
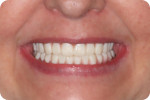
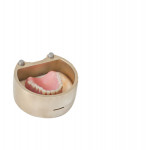
Clinically, most denture providers are still following the same basic steps, in the same basic order. First, dentists meet the patients in person, at which time they examine, diagnose, and prescribe appropriate treatment options. If and when these patients opt for new dentures, the dentist begins with primary and/or master impressions, followed later by bite registrations and initial tooth/arch arrangements, usually after creating a record base and wax rim. Dentists are taught to then validate their clinical efforts and confirm patient acceptance with a wax try-in. In the traditional workflow, this try-in step was done directly with the actual final prosthetic teeth set in wax, allowing for accurate, natural visualization and easy adjustment of anything requiring correction in order to achieve satisfactory results in the end (Figure 1). As a culmination of all preceding steps, this traditional wax try-in was the first and only opportunity to visualize a new human smile and allow for both patient and provider approval before the point-of-no-return laboratory processing steps.
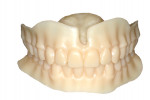
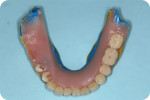
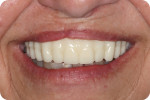
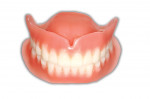
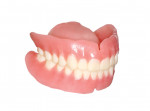
For nearly a century, this well-established procedure sequence helped maintain patient confidence in the dentist and the dentist's confidence in the laboratory throughout the treatment process. Now that we are seeing digital dentures grow in popularity, we often find ourselves at a crossroads. Whether dentists admit it or not, they are often forced to choose between the efficiency and profitability of a digital workflow, OR the predictability and control of the conventional process. The clinical speed with which a digital denture product can now be delivered is no better demonstrated than when the patient's existing dentures are used as both a custom impression tray and a wax rim/try-in—the "reference denture" technique (Figure 2).
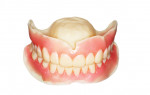
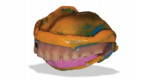
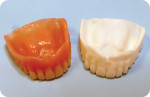
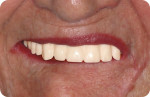
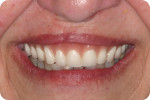
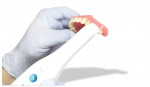
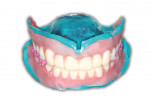
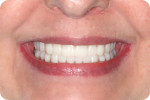
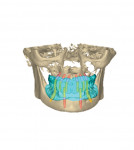
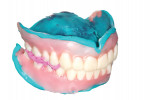
However, existing dentures often require significant modification in order to make space for good impression materials and techniques as well as to capture proper interarch relationships and represent optimal esthetics (Figure 3 and Figure 4). Using this technique, we often find that esthetic and functional displacement of teeth is something to be corrected in the digital design process in order to achieve optimal final results. If the dentist then wishes to validate all of the necessary laboratory guesswork, they go back to the patient with some sort of digitally produced prototype (printed or milled) for final clinical try-in (Figure 1). However, that additional validation is increasingly omitted entirely due to the additional chairtime and laboratory service cost it demands. Moreover, because the majority of patients intend on wearing their existing dentures throughout the new denture fabrication process, sending their in-use prostheses to the laboratory as physical records and/or irreversibly modifying them is not always acceptable to the patient.
One solution to these problems is to simply replicate the existing dentures with flask/acrylic duplication or to scan and mill/print a physical copy of the denture so that any irreversible changes made do not affect the serviceability or availability of those old dentures while patients still depend on them. However, when the starting dentures are simply duplicated, we are no farther along the redesign process than had we used the existing dentures directly (Figure 5 and Figure 6). Furthermore, considering that these solid plastic denture prototypes can only be amended additively and/or subtractively, any modifications to these substitute starting points are often more time-consuming, messy, and expensive than a traditional wax try-in (Figure 7).
For all these reasons, it is more sensible to have a digital denture try-in that represents the anticipated final result rather than the known problem starting point; therefore, the contemporary "monoblock" digital denture try-in is something many providers are now adopting to keep pace with the technology while still following the original denture checkpoints (Figure 1). While they can be a much better attempt at previewing optimal prosthetic results, because they are both monolithic and monochromatic, these digital try-ins offer hardly the same opportunity to visualize (much less modify) the anticipated treatment results (Figure 8 and Figure 9). Their main appeal appears to be that because they are a result of an accelerated digital design and production process, they are assumed to be a more profitable alternative to the conventional means of clinical validation (Figure 1). However, in many cases, this modern substitute for a denture wax try-in is outright skipped due to an imbalance in production cost vs clinical value.
However advantageous the digital denture product, the digital denture process is often less efficient, less predictable, and less profitable in terms of acquiring, transmitting, interpreting, processing, and actualizing all of the case data in a way that meets or exceeds both patient and provider expectations. This often leads to increased problems, and contributes to lower patient satisfaction, higher remake rates, and slow industry adoption of what could be a groundbreaking solution for an enormous population of patients in serious need of higher treatment standards.
Proposed here is the author's complete reinventing of the entire approach to this basic dental service as laid out in the following steps:
1. At the initial patient consultation, digital smile photographs and existing denture scans are acquired and submitted to a preferred dental laboratory for the initial smile-guided digital denture design and production of the author's proprietary try-ins (Omnismile Try-Ins, omnismile.com) (Figure 10 through Figure 13).
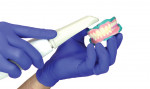
2. The try-ins are then used to capture direct master impressions and bite registrations all during the same records appointment, where full smile visualization and clinical validation occurs highly consistently with the actual final prosthetic results (Figure 14 through Figure 19).
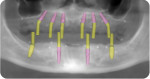
3. The finalized try-ins not only can be scanned locally using an intraoral scanner for final denture design, but they also serve as radiographic scanning templates if dental implants are indicated in conjunction with the prosthetic treatment (Figure 20).
4. Digital data is sent to a preferred dental laboratory to act as a highly detailed, 3D blueprint of the ideal final digital denture design, from which the final dentures are then fabricated per whatever denture material and/or production modality is requested. Additionally, if the case includes dental implants, then surgical guides and any implant componentry can be provided at this same step (Figure 21 and Figure 22).
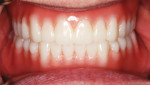
5. Now, the clinician can simply insert final digital dentures per normal denture delivery protocols, and enjoy the mutual satisfaction of completing a predictable digital denture after just one clinical records appointment (Figure 23 to Figure 25).
6. Furthermore, if a quick economy denture (eg, backup denture or transitional/healing denture) is desired, simply processing the try-in per usual relining/rebasing laboratory steps can produce another cost-effective denture without any additional clinical effort (Figure 26 to Figure 29).
In this way, efficient, attractive, reproducible dentures are finally a predictable and profitable reality, both now and long into the future, with an economy solution built right into the standard workflow. No longer is the value of the denture service carried solely by the resulting prosthesis alone. Now, the process itself creates upfront value by preserving clinical resources as well as the integrity of the original dentures and retains it indefinitely as the opportunity to remake that same prosthesis lives on in the digital database.
This process takes a fraction of the clinical time normally required for traditional complete dentures, without needing to skip or compromise any of the clinical steps. Furthermore, by streamlining the acquisition of initial patient data and jumping straight to the smile-guided digital design steps, the dental team can condense the patient experience to the point of starting the clinical records process with the final wax try-in itself. Lastly, because complete visual and functional evaluation can finally occur all in the course of the first and only clinical records appointment, neither the clinician nor the technician need worry about the problems ordinarily encountered with faster, more profitable denture workflows, such as esthetic deficiencies, functional misalignments, phonetic disturbances, and any other complication relating to compromising or omitting the traditional wax try-in. Now, the final denture production laboratory can produce a high-quality final denture with confidence using best-in-class digital prosthetic materials and processes simply by aligning the final denture design to the perfected, approved try-in scans without needing to interpret any additional setup changes or do any guesswork in the absence of adequate laboratory prescription information. In this way, the laboratory, the clinic, and the patient all benefit from the enhanced value of a reproducible denture product that also fits better, looks better, and lasts longer than traditional materials/methods. With the additional benefits of preserving the integrity and functionality of the existing denture along with the built-in processed economy denture option as well as the radiographic guide/surgical planning functionality, there are now multiple upfront opportunities embedded in this otherwise basic-level dental service. Ultimately, this process saves all parties the most precious resource of all—time—while having fun and ensuring success for now and for the future.
About the Author
Andrew C. Johnson, DDS, MDS, CDT, FACP
Surgical Prosthodontist
Fayetteville, AR
Adjunct Faculty, University of Tennessee Advanced Prosthodontics
Diplomate, American Board of Prosthodontics
Member, American Academy of Restorative Dentistry