Facial Analysis for the Digital Planning of a Full-Mouth Implant Rehabilitation
Collaborative benefits of a detailed diagnostic approach
By Ryan Tak On Tse, BDS, and Edward Tam, BDS
Historically, implant rehabilitation was driven largely by bone location. Eventually, prosthetic design began to play a greater role.1 More recently, the trend has been toward a dentofacially driven approach2 based on incisal edge position and preoperative lip dynamics.3-5 The use of the patient's natural head position, facial reference glasses, a dentofacial analyzer, and digital photography facilitates an acceptable preoperative analysis.6
This case report discusses the case of an elderly gentleman who desired a fixed implant prosthesis to replace his failing dentition and tooth-supported fixed and removable appliances. The combined use of a Kois dentofacial analyzer, Kois facial reference glasses, intraoral scans, and cone-beam computed tomography (CBCT) scans enabled the dental team to plan and complete the implant case digitally and fulfill the patient's desired outcome.
Clinical Case Overview
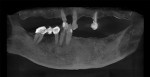
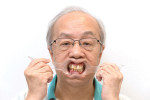
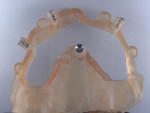
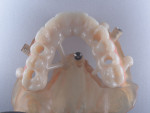
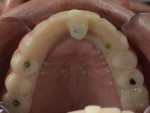
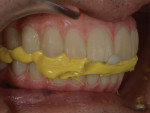
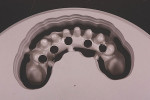
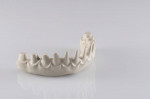
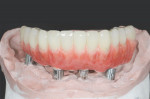
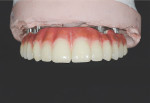
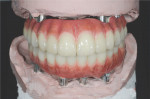
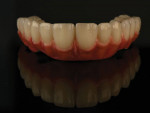
A 65-year-old man presented with concerns about quality of life with regard to his oral condition. Due to deterioration of his maxillary and mandibular fixed and removable appliances and remaining supporting teeth (Nos. 6, 8, 12, 27 through 29, and 31), he was unable to eat adequately (Figure 1 and Figure 2). His chief desire was to have a fixed prosthesis.
Medically, the patient reported a history of hypertension, elevated cholesterol, and type II diabetes. His hypertension and elevated cholesterol were controlled with blood pressure medication and statins, and his diabetes was well controlled, with his Hb1Ac below 7.
Diagnosis and Risk Assessment
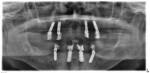
Radiographic evaluation revealed attachment loss or bone loss in the remaining dentition. Bleeding on probing was evident on the lingual side of the mandibular teeth. Several teeth had 1 mm to 3 mm recession, and tooth No. 31 had a 5 mm mesiolingual pocket. The patient reported that his missing teeth were lost more than 10 years prior due to severe caries. Considering the numerous extractions surrounding his surviving dentition and the lack of severe periodontal pocketing, the clinician surmised that periodontal disease likely was not the main factor in the failure of the dentition. This was encouraging news to the clinician, as previous tooth loss from periodontal disease is a significant risk for implant success.7 The patient was diagnosed as American Academy of Periodontology (AAP) stage II, grade B. As such, the periodontal risk was assessed as low to moderate, and the periodontal prognosis was moderate.
From the laboratory's perspective, the primary periodontal issue with a full-arch prosthesis is whether the patient can clean underneath the fixed implant bridge. In some cases, a removable option such as an overdenture may need to be considered. In this case, a high-performance polymer was chosen, partly because of its biocompatibility and ability to maintain periodontal health.
The patient's biomechanical risk was assessed as high and his prognosis poor, as he presented with multiple carious lesions. His missing teeth were lost because of caries.
Functionally, the patient did not have adequate natural dentition for mastication, and because of the failing restorative appliances his chewing was gradually becoming compromised. There were no detectable neuromuscular or joint pathologies or complaints at the time of examination. Although his function was diagnosed as acceptable, the potential for loss of function due to his dentition and restorative treatment failing over time was notable. The functional risk was assessed as moderate, and the prognosis was poor.
With the functional diagnosis, the laboratory needs to consider:
• the likely loading requirement on the framework and therefore the choice of material of the framework and crowns;
• the amount of occlusal clearance so the type of prostheses and material are suitable;
• the anterior guidance and the cuspal incline of the crown;
• the possible wear if the patient has paranormal function;
• and the opposing dentition and materials.
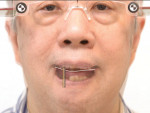
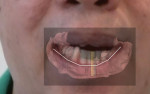
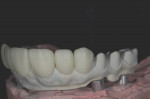
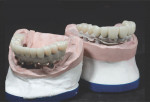
Dentofacially, with the patient smiling, the maxillary gingival margins were not visible. However, the patient's mandibular teeth Nos. 27 through 31 (No. 30 being a pontic) were supererupted and fully visible in the patient's smile (Figure 3). The dentofacial risk was assessed as high and the prognosis poor.
From the laboratory's perspective, the position of the incisors particularly affects where the access holes of the implant connection may come out, so that should be considered at the planning stage. It is also important to determine and communicate the vertical dimension of occlusion (VDO) and anterior occlusal plane (ie, the incisors' vertical and horizontal positions in relation to the lips).
The team planned the case from the position of the incisal edge and lip dynamics. This is significantly different from the old "bone-driven" approach; conversely, the "restorative-driven" approach allows the team to plan the esthetics from the beginning. This helps to decide how much bone to reduce, where the transition zone is, whether/how much pink porcelain is required, and what material is best for the final prosthesis.
In order to optimize treatment outcomes, the clinician should be well-informed regarding laboratory procedures and materials, including limitations, advantages, and disadvantages. Similarly, technicians need to understand the clinical situation well to alert dentists to potential problems and address them while the case is still being planned. When technicians are only involved after implant placement, the restorative options are limited. By using the approach detailed above, the entire restorative team can plan the case together; in this case, the prosthodontist was also the surgeon, and two laboratories were involved (one for the fabrication of the surgical guide and temporary prosthesis, and one for the final prosthesis).
Treatment Plan
Because of the patient's high biomechanical risk on his few remaining teeth, it was determined that the existing dentition would be a hindrance to ideal treatment. The clinician, therefore, recommended the removal of the remaining teeth and the utilization of maxillary and mandibular implants for a full-mouth implant rehabilitation.
Phase 1: Dentofacial Analysis
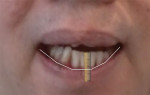
Five extraoral photographs were taken to establish the dentofacial midline, proper incisal edge position, smile curve, and smile design. These photographs, some of which were taken with the patient wearing a pair of facial reference glasses (Kois Facial Reference Glasses, Kois Center) comprised a retracted view (Figure 4), smile view, lips in repose view, Duchenne smile view (Figure 5), and overhead, or 12 o'clock, view.
As established in the literature, the natural head position is a critical factor in locating the esthetic plane.8-10 Utilizing the patient's natural head position, facial reference glasses provide visual reference points on facial photographs of the same focal length distance from the camera. Photographs can then be superimposed for diagnostic and treatment planning measurements. In addition, the facial reference glasses are used to locate the dental midline and natural head position, which are recorded by the Kois Dento-Facial Analyzer™ (Panadent). The dentofacial analyzer was used to record and then communicate the essential functional and esthetic parameters for mounting the maxillary cast.6
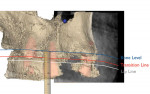
The clinician used a calibrated digital ruler utilizing digital smile design technology to determine maxillary incisal edge position. Normally, the canine cusp tip should be approximately at the same level as, or have up to 1 mm showing below, the upper lip line in repose.11 In this case, the canine was shown to be 2 mm above the upper lip line. By superimposing the smile image and the repose image, the desired canine position was determined; adding 3 mm to the canine would provide an appropriate esthetic result (Figure 6).
Upper lip mobility was measured by superimposing the repose and Duchenne smile photographs and was found to be 6 mm (Figure 7), which is within normal limits.12
The clinician used a video recording of the patient speaking and captured a screenshot with maximum gingival display. Lower lip mobility was measured at 8 mm (Figure 8). The mandibular incisors showed 4 mm in repose, therefore the clinician determined the mandibular incisor position should be reduced in height by 3 mm, leaving a normal 1 mm reveal of the incisal edges in repose.
With the steps above completed, the position of the maxillary and mandibular incisors was established and the upper and lower lip mobility was documented. These measurements allowed the clinician to determine where the gingival tissue-to-restoration interface would be; this is labeled the "transition zone" in the photographs.
Phase 2: Data Gathering and Digital Planning
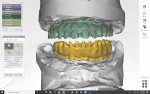
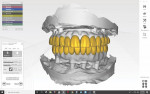
For the digital treatment plan, four image layers were superimposed (ie, merged). The DSD Planning Center provided the digital merging of the layers.
The first image layer included the digital smile design photograph smile view (Figure 1), retracted view (Figure 4), lateral view, and 12 o'clock view.13 The lateral view was used to assess the "E line" (ie, the tip of the nose to soft-tissue pogonion)14 and nasolabial angle.
The second image layer was the intraoral scan (STL file) of the maxilla and mandible. The third image layer comprised the scan of the entire denture with a radiographic marker, and, finally, the fourth image layer consisted of the CBCT scan with the radiographically marked denture placed intraorally.
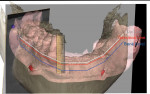
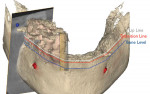
After all the layers were merged by the planning center, the clinician could perform bone contouring and implant planning. For the maxilla, to hide the transition zone, bone needed to be reduced in height. As depicted in Figure 9 through Figure 11, reduction of bone height in the area of tooth No. 8 would enhance implant placement as this would also increase bone width. The blue line in Figure 11 indicates bone level was around 13 mm from the incisal edge of tooth No. 8. For the mandible, to hide the transition zone, the bone needed to be reduced to approximately 18 mm from the incisal edge of tooth No. 27 (Figure 12 through Figure 14). The maxillary and mandibular All-on-4® implant rehabilitation was enabled via adequate restorative space in this patient (Figure 12 through Figure 14) and would replace the missing hard and soft tissues and hide the transition zone behind the lips.15-17
Phase 3: Guided Implant Surgery and Immediate Prostheses
Clinical guides were manufactured by the DSD Planning Center according to the digital plan and consisted of four parts: the base guide (Figure 15), pin guide, implant guide (Figure 16), and hybrid provisional guide (Figure 17). The clinician positioned the base guides for both the maxillary and mandibular prostheses intraorally. The base guides were stabilized over the remaining teeth and pins were used to anchor the base guides to the maxillary and mandibular bones. The remaining teeth were then extracted, and the base guide was used as a bone reduction guide to remove the prescribed amount of bone. The implant guide was placed over the base guide and pin guide for accurate placement of four implants each in the maxilla and mandible. Astra Tech® EV implants (Dentsply Sirona) were placed in the anterior, while Astra Tech® Profile implants (Dentsply Sirona) were chosen for the posterior to avoid having to trim extra bone and to minimize bone resorption (Figure 18). Finally, SmartFix® abutments (Dentsply Sirona) and temporary abutments were placed, and light-cured acrylic was used to attach the hybrid provisional. The patient was instructed to wear a provided soft nightguard and have a soft diet for 8 weeks.
Phase 4: Provisional Prostheses
After 6 months of osseointegration, the patient was satisfied with the appearance and function of the provisional restoration (Figure 19). A Kois deprogrammer platform (Kois Center) was made directly in the mouth on the palatal surfaces of teeth Nos. 8 and 9 (Figure 20). The patient was deprogrammed for 1 hour and a bite record (Harvard Bite, Harvard Dental International) was taken for the laboratory to mount the final prosthesis (Figure 21). An open-tray PVS impression (Imprint™, 3M Oral Care) was taken with splinted impression copings.
The functional pathways were adjusted by positioning the patient in an upright seated position.18He was asked to bite on 200-µm-thick articulating paper (Bausch) and bring the posterior teeth together to maximum intercuspation. The lingual contours of the maxillary incisors were adjusted until the marking ink no longer showed surface streaks during biting. The laboratory would utilize the lingual surfaces of the provisional restoration as an aid in the design of the final restoration.
Phase 5: Final Prostheses
The framework chosen for the base of the final prostheses was made of milled PEKK, a high-performance polymer (Pekkton®, Anaxdent North America), which has elastic modulus similar to natural teeth and bone and is designed to provide stress distribution and shock absorption.19 Milling the framework involves significant amounts of digital design work, which was beneficial in this case because information from the initial planning and other stages could be transferred to the design. Additionally, the temporary implant bridges could be used as templates, as the clinician had adjusted them.
The laboratory needed to make individual crowns that fit over the framework, so they opted to "split" the whole design into crowns and base in the design software (Figure 22 and Figure 23). Even in the gingiva, cutback could be pre-determined.
Once the framework design was finalized, it was precisely milled with a 5-axis machine (Figure 24 and Figure 25). After milling, the margins were carefully refined and the prosthesis was re-scanned using pre-recorded implant positions so the crown height and shape would not change and all the components could be bonded together precisely when ready.
Full-contour zirconia crowns (Katana™, Kuraray Noritake Dental) were selected for the posterior, and layered lithium disilicate crowns (IPS e.max®, Ivoclar Vivadent) were used for the anterior teeth (Figure 26 through Figure 33).Strength and esthetics must be considered for all tooth-colored materials, and sometimes those factors are inversely related. The full-contour zirconia offered high strength (850 MPa), providing durability in the posterior. Lithium disilicate crowns, meanwhile, offer even more natural-like esthetics, so they were chosen for the less mechanically demanding anterior. Both materials bond similarly to the PEKK framework.
As the crowns were designed together with the framework, the final shape had already been determined. Once they were adapted to the final framework, the STL files were sent to the CAM software for milling. The zirconia crowns were milled with 5-axis dry milling, and the lithium disilicate crowns were wet-milled. The zirconia crowns were sintered in a furnace (Dekema) and the lithium disilicate crowns were crystallized in a ceramic oven (Ivoclar Vivadent). Stains and even thin layers of porcelain were added according to the desired shade and esthetic requirements such as surface textures and translucency.
The final crowns were cemented onto the framework according to bonding protocols from the PEKK manufacturer (Cendres+Metaux).
Conclusion
This case illustrates a method to systematically diagnose, plan, and stage treatment for a full-mouth implant rehabilitation. The use of facial analysis with reference glasses and digital smile design imaging and measurements allowed the team to preoperatively plan the incisal edge, lip mobility, and transition zone. The All-on-4 implant treatment offered immediate function and an esthetic appearance without grafting, which helped to minimize pain and swelling. The patient was satisfied with the excellent esthetics as well as the function.
About the Authors
Ryan Tak On Tse, BDS, MFGDP, MClinDent (Prost), MSc (Implant Dent) (HK), MGD
Private Practice
Hong Kong
Edward Tam, BDS
Director
Vanguard Computer Assisted Laboratory
Hong Kong
References
1. Morton D, Phasuk K, Polido WD, Lin WS. Consideration for contemporary implant surgery. Dent Clin North Am. 2019:63(2):309-329.
2. Orphanos ES. Facial esthetic considerations with all-on-4: a report on two cases. Int J Periodontics Restorative Dent. 2019;39(1):57-64.
3. Spear F. The maxillary central incisor edge: a key to esthetic and functional treatment planning. Compend Contin Educ Dent. 1999;20(6):512-516.
4. Kois JC. Diagnostically driven interdisciplinary treatment planning. Seattle Study Club J. 2002;6(4):28-34.
5. Roe P, Rungcharassaeng K, Kan JYK, et al. The influence of upper lip length and lip mobility on maxillary incisal exposure. Am J Esthet Dent. 2012;2(2):116-125.
6. Tak TO, Kois JC. Digital smile design meets the dento-facial analyzer: optimizing esthetics while preserving tooth structure. Compend Contin Educ Dent. 2016;37(1):46-50.
7. Levin L, Ofec R, Grossmann Y, Anner R. Periodontal disease as a risk for dental implant failure over time: a long-term historical cohort study. J Clin Periodontol. 2011;38(8):732-737.
8. Solow B, Tallgren A. Natural head position in standing subjects. Acta Odontol Scand. 1971;29(5):591-607.
9. Lundström F, Lundström A. Natural head position as a basis for cephalometric analysis. Am J Orthod Dentofacial Orthop. 1992;101(3):244-247.
10. Lundström A, Lundström F, Lebret LM, Moorrees CF. Natural head position and natural head orientation: basic considerations in cephalometric analysis and research. Eur J Orthod. 1995;17(2):111-120.
11. Misch CE. Guidelines for maxillary incisal edge position - a pilot study: the key is the canine. J Prosthodont. 2008:17(2):130-134.
12. Roe P, Rungcharassaeng K, Kan JYK, Patel RD. The influence of upper lip length and lip mobility on maxillary incisal exposure. Am J Esthet Dent. 2012;2:116-125.
13. Coachman C, Van Dooren E, Gürel G, et al. Smile design: from digital treatment planning to clinical reality. In: Cohen M, ed. Interdisciplinary Treatment Planning, Vol. II, Comprehensive Case Studies. Chicago, IL: Quintessence Publishing; 2012:119-174.
14. Ricketts RM. Esthetics, environment, and the law of lip relation. Am J Orthod. 1968;54(4):272-289.
15. Maló P, de Araújo Nobre M, Lopes A, et al. The All-on-4 concept for full-arch rehabilitation of the edentulous maxillae: a longitudinal study with 5-13 years of follow-up. Clin Implant Dent Relat Res. 2019;21(4):538-549.
16. Maló P, de Araújo Nobre M, Lopes A, et al. The All-on-4 treatment concept for the rehabilitation of the completely edentulous mandible: a longitudinal study with 10 to 18 years of follow-up. Clin Implant Dent Relat Res. 2019;21(4):565-577.
17. Di P, Lin Y, Li JH, et al. The All-on-Four implant therapy protocol in the management of edentulous Chinese patients. Int J Prosthodont. 2013;26(6):509-516.
18. Bakeman EM, Kois JC. The myth of anterior guidance: 10 steps in designing proper clearance for functional pathways. J Cosmetic Dent. 2012;28(3):56-62.
19. Han KH, Lee JY, Shin SW. Implant- and tooth-supported fixed prostheses using a high-performance polymer (Pekkton) framework. Int J Prosthodont. 2016;29(5):451-454.