More CAD/CAM Options Than Ever
Bars and abutments form the backbone of the laboratory
Josh Marotta, CDT, MDT, and Justin Hayes
CAD/CAM bars and abutments are integral parts of laboratories' digital offerings. While digital dentistry is a term thrown around to cover everything from intraoral scanners to computerized shade taking, bars and custom abutments were one of the earliest ways laboratories entered the digital market. Titanium was a mainstay of the earliest prostheses; today, there are numerous options, from zirconia to high-performance polymers. Each comes with pros and cons, but the foundation of restoration has not changed. With the increased demand for esthetic outcomes comes even more need for specialized planning and designing to ensure a proper-fitting, long-lasting restoration.
Abutments
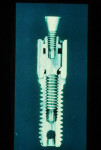
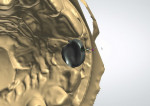
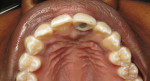
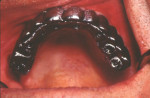
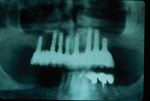
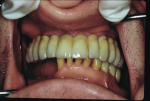
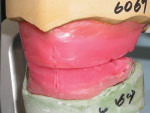
As one of the original foundations of CAD/CAM restorations, custom abutments are standard in many laboratories' armamentarium. When the first implant protocols were introduced by Per-Ingvar Brånemark, everything was screw-retained on stock components. The standard abutment formed the foundation of any restoration, with the intention that in a worst-case scenario, the prosthetic screw would break (Figure 1 through Figure 3). Over time, the strict protocol that guided implant placement was lost, and cementable restorations came to fruition.
Cementable restorations emerged because at times implant placement was not ideal for screw-retained restorations. Screw-access holes coming through the facial or severely off-angle implants necessitated the use of cementable restorations and ushered in the first use of CAD/CAM custom abutments. For cases needing deep implants, stock components would have sub-subgingival finish lines. This feeds into today's concern about excess cement being left after insertion and the risk of peri-implantitis as well as potential bone loss and implant failure. Custom abutments help to avoid this issue by being patient-specific products that bring the cementoenamel junction of the restoration to the proper tissue height, facilitating better hygiene and avoiding deep sockets where cleaning the excess cement would be impossible.
With today's CAD/CAM systems, technicians have even greater control of their ability to design custom abutments. Utilizing today's leading design software, they are able to control every facet of the abutment within specified parameters from the manufacturer. This results in even greater precision in creating a restoration for each specific patient. Laboratories can ensure that abutments are parallel and accommodate any contouring needed by the patient. They can control exactly where the finish line will be for achieving the best esthetic outcomes and desired results of the dentist (Figure 4).
Dental professionals are no longer limited to just titanium; zirconia custom abutments have long been a restorative option for numerous implant platforms. They allow for the fabrication of metal-free restorations for patients. With zirconia, more options are available to provide highly esthetic all-ceramic crowns and avoid metal show-through on thin biotypes. When designed properly to manufacturers' specifications, these custom abutments have shown themselves to offer "excellent technical and biological results over 10 to 11 years of function."1 Of course, with zirconia, extra consideration must be paid to material thickness and angulation. With leading design software, there are minimum constraints that must be met to ensure a proper restoration and avoid potential complications.
Even with custom abutments, there has been significant headwind against cementable restorations. Today custom abutments are being utilized as custom titanium bases. Taking all the best from custom abutment design, technicians can design abutments with ample support for the final crown. Instead of being cemented intraorally, the crown is cemented to the abutment outside the mouth, with a screw-hole in the crown so it can be screwed into the mouth. Another new approach is utilizing angulated screw channels for custom abutments. They allow the technician to change the screw chimney, offering the option to use a screw-retained restoration in areas where it once wasn't possible (Figure 5 through Figure 7).
Bars
Beyond single units, full-arch restorations benefited from CAD/CAM technology. The original restorations from Brånemark were all screw-retained, including full-arch restorations and bars. The hybrid restoration—a milled titanium bar wrapped in acrylic with denture teeth—was the original restorative option for patients. The basic titanium bar overdenture continues to be a mainstay of full-arch restorations with its proven reliability.2 Nonetheless, the titanium bar is limited by the kind of restorative outcomes that can be built upon it. Restorative teams are often limited to acrylic and denture teeth or a patient-removeable overdenture utilizing snap attachments. Ceramo-metal restoratives have been tried, but they require technique-sensitive titanium porcelains, as regular veneering porcelains to do not adhere to titanium (Figure 8 through Figure 10).
As technology has progressed, so have restorative materials. Full-arch zirconia has become common in restorative procedures. It allows most laboratories to easily produce predictable restorations with high strength and esthetics. Zirconia full-arch reconstructions are new, but the initial research indicates full-arch monolithic zirconia frames were a therapeutic option in 2- to 7-year follow-ups.3 It is wise to note that monolithic zirconia is virtually a solid rock; there is no layering to it. Compared to titanium or porcelain fused-to-metal restorations, all the force is transferred right through to the implant. Proper design must consider force and leverage materials to avoid the transfer of undue force over the implants.4
Milled cobalt-chrome frameworks are another restorative choice to consider for full-arch restorations. Traditionally cobalt-chrome was relegated to partial frameworks and attachment bars. Today's milled cobalt-chrome pucks allow for a porcelain-fused-to-metal framework utilizing traditional feldspathic porcelain without the additional costs of a gold-palladium alloy or expensive parts. Cobalt-chrome is a stiffer, stronger alloy than titanium that reduces stress on implants.5 In addition, today's milled cobalt-chrome alloys are much purer than what was traditionally available, with no trace elements of nickel or beryllium. This ensures even expansion and oxidation compared to the mixed alloys of cast frameworks. If fabricated properly, the chrome-cobalt restorations show significantly less deviation compared to cast frameworks.6
Some materials generating the most interest today are high-performance polymers. These relatively new restorative options are being promoted both for ease of fabrication and their reduced cost profile. There are numerous design options available, from full-arch bar overdentures to direct screw-retained frameworks with composite veneering. Initial studies claim to show positive biomechanical properties.7 Long-term studies are still evaluating the longevity of these restorative materials. There is hope that high-performance polymers will show proven benefits for esthetic outcomes and implant and prosthesis longevity as such research is completed.
There are more restorative options than ever for fabricating custom abutments and full-arch implant-retained frames. With full-arch cases utilizing modern materials, even more attention should be paid to setting up each case properly to avoid complications. Traditional denture workflows can help support ideal esthetic outcomes. Bite rims, setups, and verification jigs are necessary to establish vertical dimensions of occlusion and allow patients to get a preview of the final esthetic outcome (Figure 11 through Figure 13). By verifying the model, we reduce the chance of putting undue force on the implants or needing to section and weld the frameworks.
With ever more proliferation of CAD/CAM technology, it will be even easier for laboratories and clinicians to produce restorations in-house without relying on implant companies or third parties to mill materials. This helps retain quality control and puts more onus on the technician to ensure the clinical acceptability of the restoration. For any restoration, from single-unit abutments to full arches, it is critical to ensure that the patient knows what to expect—anything from the chance of tissue recession around a metal abutment to not having enough A-P spread to accommodate second molars. Communication is key in providing both clinically acceptable restorations and ensuring patient satisfaction. Today's technology allows even closer communication among the clinical team, surgeon, restorative dentist, technician, and patient. With proper planning, single-implant and full-arch restorations are predictable and cost effective for the laboratory, clinician, and patient.
About the Author
Josh Marotta CDT, MDT, is a Manager/Partner at Marotta Dental Studio, a full-service laboratory in Farmingdale, NY. Justin Hayes is the Operations Director at Marotta Dental Studio.
References
1. Ekfeldt, Anders, et al. “Zirconia Abutments for Single-Tooth Implant Restorations: A 10- to 11-Year Follow-up Study.” Clinical Oral Implants Research, vol. 28, no. 10, Oct. 2017, pp. 1303–1308. EBSCOhost, doi:10.1111/clr.12975.
2. Corsalini, Massimo, et al. “Maxillary Overdenture Retained with an Implant Support CAD-CAM Bar: A 4 Years Follow Up Case.” The Open Dentistry Journal, vol. 11, no. 1, 2017, pp. 247–256., doi:10.2174/1874210601711010247.
3. Vizcaya, Fernando Rojas. “Retrospective 2- to 7-Year Follow-Up Study of 20 Double Full-Arch Implant-Supported Monolithic Zirconia Fixed Prostheses: Measurements and Recommendations for Optimal Design.” Journal of Prosthodontics, vol. 27, no. 6, 2016, pp. 501–508., doi:10.1111/jopr.12528.
4. Corsalini, Massimo, et al. “Maxillary Overdenture Retained with an Implant Support CAD-CAM Bar: A 4 Years Follow Up Case.” The Open Dentistry Journal, vol. 11, no. 1, 2017, pp. 247–256., doi:10.2174/1874210601711010247.
5. Bhering, Cláudia Lopes Brilhante, et al. “Comparison between All-on-Four and All-on-Six Treatment Concepts and Framework Material on Stress Distribution in Atrophic Maxilla: A Prototyping Guided 3D-FEA Study.” Materials Science and Engineering: C, vol. 69, 2016, pp. 715–725., doi:10.1016/j.msec.2016.07.059.
6. Paniz, Gianluca, et al. “The Precision of Fit of Cast and Milled Full-Arch Implant-Supported Restorations.” The International Journal of Oral & Maxillofacial Implants, vol. 28, no. 3, 2013, pp. 687–693., doi:10.11607/jomi.2990.
7. Keilig, Ludger, et al. “Does the Material Stiffness of Novel High-Performance Polymers for Fixed Partial Dentures Influence Their Biomechanical Behavior?” The International Journal of Prosthodontics, 2016, pp. 595–597., doi:10.11607/ijp.4940.