Treating Traumatic Oral Injury: A Personal Account
Part 3 of one dental technician’s personal restorative journey
By Kyle Swan, CDT
This is Part 3 of an article originally published in the September 2012 issue of Inside Dental Technology (dentalaegis.com/idt/2012/08/treatment-of-traumatic-oral-injury-a-personal-account). The patient suffered an array of dental issues as the result of a fall after his heart stopped during a marathon. Fractured, avulsed, and impacted teeth were all in need of treatment. After the heart issue was dealt with, the path was cleared for the necessary dental restorative plan. The full process was lengthy and methodical, even though the patient was hoping for a “quick fix.” Multiple specialists and an exceptional restorative dentist were involved to give the patient the best possible result, starting with oral surgery, then endodontics, orthodontics, periodontics, and, finally, bonded ceramics.
What makes this case a little more out of the ordinary is the fact that the patient was a ceramist and laboratory owner. His experiences with patients and other people’s cases did not prepare him for the unique insight he gained from his own case. As mentioned in an earlier article, he had to follow his own advice or “put his money where his mouth is.” He learned that even with the best clinical support and restorative plan, it is easy to misjudge vanity biases, home care issues, material limitations, and the transitory nature of “success” in the oral environment. The following illustrates the technical steps involved to restore the patient’s teeth, but also offers personal insight gained by the dental technician-as-patient.
Starting Conservatively
At this point in the process, orthodontics had already been utilized and the teeth were properly aligned for restoring. After doing a diagnostic wax-up and establishing new sizes and shapes for the teeth involved (Nos. 7-10), it was determined that the best restorative choice would be feldspathic veneers. After much deliberation—and taking the endodontic access holes and remaining enamel into consideration—the dentist and patient decided to take the most conservative approach. The move to full-coverage crowns would always be an option for the future, but was not the best first choice for the patient. Although the clinician believed both options were reasonable, he understood the patient’s decision for the least invasive option.
Knowing that it was a unique situation—as the patient was making his own restorations combined with a great working relationship with the restorative dentist—made it easier for the patient to decide against full crowns. Any result that was less than favorable could be redone with less hassle than under most circumstances. Waxing the teeth was an invaluable exercise as the sizes, shapes, and proportions were worked out in advance. Proper function and esthetics were achieved on the wax model after analyzing photographs.
Preparation and Temporization
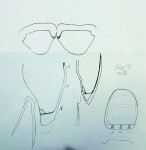
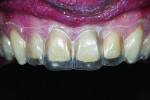
Using the diagnostic as a guide, a preparation “road map” was created (Figure 1). Composite had been added to the teeth as an interim esthetic solution earlier in treatment, and it was decided to leave areas necessary for added support and even preparations instead of total removal.
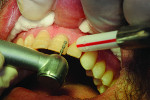
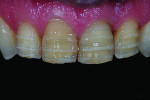
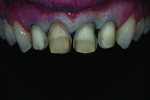
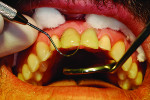
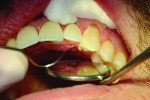
A depth-cutting bur was used to get an even starting depth of the facial surface enamel (Figure 2 and Figure 3). This was followed by removing the remaining raised areas with a diamond carbide bur, leaving large areas of bondable enamel. The preparations were then finished with a flexible disc. This created a very smooth surface and eliminated any irregularities that would be unfavorable to bonded porcelain veneers. Cord was packed using the double cord technique and the margins were adjusted and finalized. This allowed for the veneer margins to be right at the crest of the gingiva or slightly beneath (Figure 4).
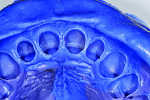
A provisional matrix, or “suck-down,” created in advance of the procedure from a stone duplicate of the diagnostic wax-up, was filled with acrylic and transferred to the mouth (Figure 5 and Figure 6). After setting, it was removed and adjusted in the office laboratory, eliminating flash, etc, and prepared for insertion.
It was suggested that a clear silicone matrix created from the diagnostic wax-up would work well for the provisional matrix. It would capture more detail than a suck-down and need fewer adjustments. The clinician believed this would achieve good results. He was correct. His temporary was very well done, thus legitimizing the seeming concession. As with technicians, the same applies to clinicians: defer to what works best in their hands.
During this process, the final impression and bite registrations were taken using a polyvinyl material. It was verified that all of the margins were completely captured in the impression before continuing (Figure 7).
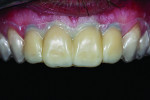
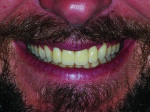
The acrylic one-piece provisional restorations were spot-bonded in place and adjusted for fit and function. The dentist and patient were pleased with tooth display in both repose and smile poses (Figure 8 and Figure 9). An impression of the seated provisionals was taken for reference.
Provisionals for veneers can be challenging. Patients are encouraged to be very careful with them. Depending on the amount of material used and tooth structure involved, they are more prone to breaking or coming loose than conventional full-coverage provisional restorations, especially if they don’t wrap around the lingual. The patient was fully aware of this and was given very specific home care instructions: don’t bite directly into anything with them, eat soft foods, etc. In his laboratory, the patient had fielded many calls and requests to expedite veneer cases because the patient kept breaking their provisionals. He hadn’t had quite the appropriate compassion for these situations until it happened to him. With all the best intentions, thinking a piece of dark chocolate would be safe, he was stunned when, during chewing, it moved to the front of his mouth and snapped off his No. 10 provisional tooth. Too embarrassed to contact the dentist on his case, as it was the day of delivery, he asked another dentist friend to help him reapply the broken temp. He was a little more careful after that.
Veneer Fabrication
Feldspathic veneers built on refractory dies were the restorations of choice. After the stone models were poured and the dies trimmed, they were duplicated and replicated using refractory material (G-CERA VEST, GC America Inc., gcamerica.com) and ceramic pins.
The patient’s shade had been taken previously and he fell in the 2 to 3 range using the VITA 3D-MASTER shade guide (VITA North America, vitanorthamerica.com). He had bleached prior to restoring, so the decision was made to go with 2M1, transitioning to 2M2 and 2M3 towards the cervical third.
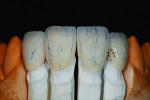
Vita’s VM13 porcelain was chosen for the build up, utilizing a variety modifiers and a fairly standard stratified layering technique (Figure 10). A bluish tint to the incisal translucency was applied due more to patient preference than to existence of translucency in adjacent teeth.
As any technician and cosmetic dentist knows, there is an inherent bias when picking shades. Most patients, when given the choice, pick a shade lighter than their own. They choose to ignore the real value and chroma of their adjacent teeth. The patient certainly knew this. He had cautioned people against it for over 20 years but made the same mistake himself. Thinking he would continue to bleach or, in his words, just choosing to ignore what could be clearly seen, he went with a shade that was too light. He fell victim to vanity and thereafter realized he should have stayed in the 3M shades. He had never liked the idea of setting oneself up for continuous bleaching to match restorations, and yet he put himself in that position. Also, the translucency chosen may have been a favorite but was arguably too strong for this case; looking back, the patient admits he should have chosen less blue and more gray coloring to match adjacent teeth.
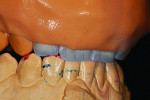
The veneers were built and shaped following the provisional matrix. The surfaces were contoured to create natural surface texture and undulations for optimal light reflection (Figure 11). Ergamix 70 Basic Lab Putty (anaxdent North America, anaxdentusa.com) was used to brace the refractory dies during finalization of function, thus allowing for thorough adjustments without needing to worry much about die breakage (Figure 12).
Function is often neglected in veneer fabrication. So much emphasis is placed on esthetics that often consideration of how the teeth come together is overlooked. This is especially true in the purely protrusive movement. Frequently this is ignored, causing material failure. Not wanting a bite guard or any other “protective appliance,” the patient took great care allowing freedom and harmony in all functional movements. Using putty allows for greater die stabilization so a more aggressive approach may be used. He also used this technique to brace individual crowns on the working models.
The patient, due to bone loss and trauma caused by avulsing and impacting teeth, had fairly blunted papillae. The decision was made to not bring the contact point high enough to close the gingival embrasure between the two central incisors. The esthetic concern was that the veneers would look like one piece instead of two individual teeth, which was undesirable to the patient. So the possibility of a “black triangle” was the preferred risk given the circumstances.
The choice of a black triangle versus a blocky look ended with a mixed result. Food collection in the area was minimal, but the darkness or shadowing caught the eye. A more creative solution using color and contour may have been more favorable, but it was ultimately a choice of preference. He didn’t like the “one mass” look achieved in the provisionals. Initially the plan was to create veneers that were as realistic and faithful to his natural teeth prior to the accident using imperfections and characteristics similar. This would have entailed making highly definitive internal mamelon effects. Although the mamelon porcelains were used, a less defined amount was applied because of lessening commitment to “natural.” Frankly, this was an unexpected and surprising decision, according to the patient. When push came to shove, he wanted them a little less “natural” than he thought.
The veneers were glazed, divested, and fit to the individual stone dies. The proximal contacts and final fit were verified on a solid stone cast (Figure 13).
Fitting veneers to the solid cast is so very important. The fit was just the way they were on the model as in the mouth. As obvious as this may seem, skipping this step is not uncommon and asks a lot of the dentist. Veneers are delicate. Having to adjust the proximal contacts chairside can be unnecessarily tedious and unfavorably alter the shapes and surface glaze. Limiting chairside adjustments and polishing is good for everyone involved.
Delivery
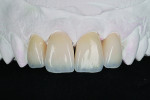
On the day of delivery, the provisional restorations were removed and the preparations were cleaned. The veneers were tried in one at a time and then all together. Both dentist and patient examined them for favorable esthetics (Figure 14). The veneers were etched and bonded into place, starting with the two central incisors seated simultaneously (Figure 15 and Figure 16). The lateral incisors were then bonded in place. After all were fully cured and cleaned, function was checked and any adjustments were made. The patient had an excess amount of space between teeth Nos. 10 and 11. The decision was made to add direct composite to the mesial of tooth No. 11 as opposed to veneering with porcelain or the mesiodistal width of tooth No. 10 disproportionate (Figure 17 and Figure 18).
The patient can confirm that the composite has held up very well with great color stability and no staining around the margins. Direct composite can be a great complement to indirect restorations, and helps reduce the need to prep virgin teeth.
Completion
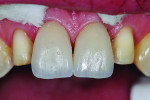
The patient left the office very pleased with the final result. A conservative permanent solution was applied to fix his teeth after severe trauma. He felt like his display in repose was where he wanted it and he found the bigger, more dominant look of his central incisors to be esthetically appealing (Figure 19). Bonding of feldspathic veneers achieved the functional and esthetic goals without having to reduce the teeth for full crowns, saving that as an option for the future if needed.
After dealing with the accident, tooth impaction, fracture, avulsing, and ankylosis; after oral surgery, endodontics, interim restorations, and orthodontics; after bleaching, bone shards, and bonding—it was finally over. Like for so many patients, it seemed the end of a long journey. The patient credits the case’s success on taking his own advice, having an exceptional interdisciplinary team, being patient, and setting the case up properly. The dramatic before-and-after photographs are a testament to this accomplishment (Figure 20 and Figure 21).
The patient was really surprised at how natural everything felt. Although he certainly doesn’t bite into whole apples for instance, everything feels solid and strong. It was refreshing, he admits, and gave him confidence that he didn’t realize he was lacking. The patient is still glad he went with veneers, but maybe not completely.
As time progressed after treatment, his endodontically treated teeth got significantly darker. He’d known this was a possibility, but did not allow for this. Grayish show-through occurred near the margins, exposing flaws in his build-ups. He now believes he should have carried the porcelains he was using to block out the color all the way to the margins. At the time, he was more concerned that they would look too opaque. He is glad he did not over-close the gingival embrasures because the papilla between the two central incisors has filled in slightly and any food impaction has been minimal. He has not bleached since the veneers were seated, yet clearly needs to if he wants a better transition to his natural teeth.
Going Forward
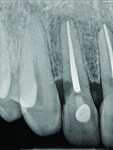
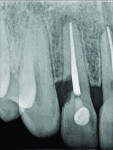
The oral environment is a system and not a static entity. When treating traumatic oral injury, one should follow all the best protocols for the best outcomes, of course, but even then success can be transitory. Permanence or completion can be fleeting, and most patients will be dealing with the after-effects of their trauma in some respect for the rest of their lives. Not even a year later, x-rays showed concern on the patient’s No. 10 tooth—external root resorption. It was watched, but just became more pronounced (Figure 22 and Figure 23). It is only a matter of time before that tooth is lost, and an alternative solution will be needed. So the process continues.
Not exactly back to square one, the patient realizes he’s at another crossroad made unique by his circumstances. So now the questions will be, “What implant system? Guided or not? Screw retained or cementable? Who will do it? Should one tooth be done or more?” He is glad to work with so many great clinicians and be exposed to so much information. His dental journey will most certainly continue, and the choices he makes will be based on the thousands of cases he has worked on over the years.
As far as his other health matters, after coming to grips with his cardiac emergency and running five more marathons, the patient feels like his heart issues are resolved, but he’ll be following it closely the rest of his life. He will continue to seek the advice of talented professionals, and if something changes he will deal with it. But he says he’s not concerned, joking that being in the dental laboratory business may kill him faster than his heart ever will.
The author/patient would like to thank Matthew Miller, DDS, of Plano, Texas for all of his exceptional work and his open mind, and Tracy McCuen for her patient photography, because it’s hard to take pictures of oneself.
About the Author
Kyle Swan, CDT
Owner/President
Functional Esthetics, Inc.
Lewisville, Texas