The Salt-and-Pepper Powder Dentin
Achieving the ideal combination of opacity and color with a milled lithium disilicate coping
By Rafael Santrich, CDT, and Richard Canizares, DMD
Restorative treatment of anterior teeth is an area of dentistry that can still be challenging for many professionals, despite the availability of innovative and advanced techniques and materials.1,2 Careful treatment planning and embracing a multidisciplinary approach are significant factors when undertaking restorative procedures in the esthetic zone, primarily due to the combination of functional and esthetic requirements that are placed on these types of restorations.1,2
In everyday dental practices, it is not uncommon for patients to present with a single chipped or fractured anterior tooth.1,2 In some instances, those cases may have been previously restored with direct composite buildups that, over time, have not provided the esthetics or durability desired by the patient.3,4 Although direct composite restorations may represent a quick and minimally invasive procedure for repairing anterior tooth fractures, they can be subject to discoloration, staining, and failure over time.5
Fortunately, laboratory ceramists can work closely with dentists to identify functional, structural, and esthetic goals and requirements of an anterior case. These may involve preparation parameters that dictate how thin or thick a restoration can be and, therefore, how esthetic characteristics can best be incorporated into the restoration.
When these considerations are applied to material selection and fabrication techniques, dental ceramists can skillfully utilize innovative all-ceramic materials such as lithium disilicate glass-ceramic (eg, IPS e.max system, Ivoclar Vivadent, ivoclarvivadent.com) to achieve optimal strength and esthetics in anterior restorations.6,7,8 Additionally, when a material system is selected that enables different or multiple fabrication techniques to be used (ie, milled with CAD/CAM, wax hot press, milled coping/framework layered with veneering ceramic and characterized with stains and glazes), the most ideal restoration can be created in terms of durability, conservation of natural tooth structure, and lifelike optical properties.7-9
Case Presentation
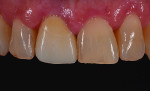
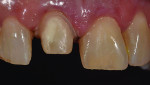
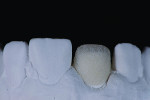
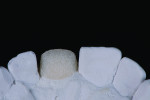
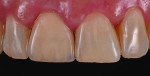
A 56-year-old woman presented with a large fracture and discolored composite restoration on tooth No. 8 (Figure 1). The dentist recommended a full-coverage crown as treatment, and the patient accepted the treatment plan. The old composite restoration was removed and the tooth prepared (Figure 2). A polyvinyl siloxane (PVS) impression was made, and the shade was also identified using the VITA Classic Shade Guide (Figure 3) and determined to be A3. However, it was noted that the patient’s teeth demonstrated greater opacity at the cervical margin. The patient was then provided with a provisional restoration, and all records were forwarded to the laboratory.
Case Analysis
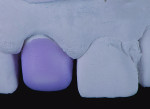
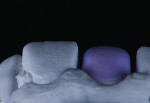
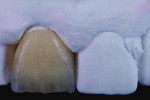
At the laboratory, stone models were made from the PVS impressions provided by the dentist. Analyzing the models from different angles and examining the tooth No. 8 preparation revealed limited buccal space for creating a nice esthetic result (Figure 4 through Figure 6). Although pressable lithium disilicate can be pressed as thin as .3 mm for veneers, because this case required combining the opacity of the patient’s natural teeth at the cervical margin with the tooth’s other optical properties, a combination of a milled lithium disilicate coping (IPS e.max CAD, Ivoclar Vivadent) and veneering ceramics (IPS e.max Ceram, Ivoclar Vivadent) would be used to fabricate the restoration.
Coping Fabrication
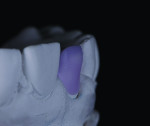
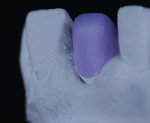
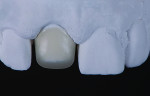
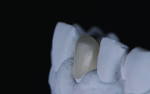
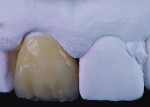
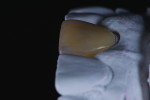
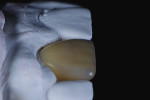
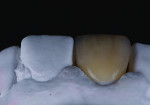
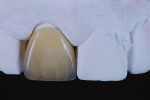
A low-translucency lithium disilicate block (IPS e.max CAD LT, Ivoclar Vivadent) in shade A3 was milled in order to obtain the necessary opacity in the cervical area of the restoration (Figure 7). After milling, the coping was tried on the model and evaluated from multiple angles (Figure 8 through Figure 10). The coping was then crystallized in a programmable oven (Programat, Ivoclar Vivadent) according to the program recommended by the manufacturer.
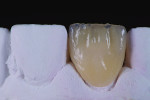
After crystallization, the coping was returned to the model, at which time limitations in its opacity were observed due to the minimal reduction of the buccal preparation (Figure 11 and Figure 12). Therefore, the ceramist determined that the ideal way to opacify the coping would be using a “salt-and-pepper” technique. Using this technique, the coping is moistened with stain liquid, after which dry ceramic powder is dusted on top (Figure 13). In this case, a deep dentin powder (IPS e.max Ceram Deep Dentin, Ivoclar Vivadent) was used to opacify the coping, as well as contribute to light reflection (Figure 14 through Figure 17).
Restoration Buildup
The restoration was built up by first applying IPS e.max Ceram Powder Dentin in shade A3 (Figure 18), which contributed to chroma, saturation, and value. A combination of opacity and color was best in this case, as well as in cases with small areas or over-translucent structures. Internal effects were created by applying IPS e.max Ceram Mamelon Effect Yellow-Orange powder in the incisal third, Enamel Opal 1 around the incisal edge, Opal Violet at the distal corner of the incisal edge, and T blue at the mesial corner of the incisal edge.
Additionally, to close the length of the crown and simultaneously create contrast between translucent areas (Enamel Opal 1) and opaque areas, Incisal Edge porcelain was applied. This resulted in the ideal transition in the incisal third. Then, to create the white band at the end of the cervical third, Enamel Opal 4 was used, while the grey band in the middle third of the crown was created using Opal Violet. Once this buildup was complete, it was baked at 780°C with a hold of 25 seconds (Figure 19 and Figure 20).
The second and final buildup was accomplished using a 1:1 ratio of Enamel Opal 1 and Enamel Opal 5 for the incisal and middle thirds. Cervical Orange was also used for the cervical area. The restoration was then baked and returned to the model, revealing the power of the color and nice value control that was achieved (Figure 21 through Figure 23).
The anterior crown was then glazed, with careful attention given to mimic the patient’s natural tooth effects. Once completed, the crown was fired at 725°C, with a 40-second hold and vacuum. By hand, and using a diamond paste and pumice, the ceramist polished the anterior crown to create the desired surface texture (Figure 24). The restoration was then returned to the dental practice and delivered to the patient.
Conclusion
Creating a natural-looking single anterior restoration requires a blend of artistry, technical skill, and knowledge of how to best utilize the innovative materials that are available today. In particular, every case requires assessment of its own unique parameters, because conventional procedures may not always deliver optimal results. In this case, preparation and space limitations, as well as the opacity in the cervical area, would affect restoration fabrication. However, by understanding the natural nuances of this patient’s tooth shade, opacity, and internal characteristics — as well as how to combine a milled lithium disilicate coping with veneered ceramic — the ceramist was able to deliver a restoration that demonstrated the ideal saturation, chroma, value, intensity, and translucency (Figure 25).
Disclosure
The author had no disclosures to report.
References
1. Krasteva K. Aesthetics and function in anterior restorations. a practical approach. Dent Today. 2004;23(1):52-5.
2. Christensen GJ. Restoring a single anterior tooth: solutions to a dental dilemma. J Am Dent Assoc. 2004;135(12):1725-7.
3. Koora K, Muthu MS, Rathna PV. Spontaneous closure of midline diastema following frenectomy. J Indian Soc Pedod Prev Dent. 2007;25(1):23-6.
4. Fuhrer N, Vardimon AD. Clinical analysis and treatment of spaced dentition. Pract Periodontics Aesthet Dent. 1997;9(5):493-501; quiz 502.
5. Chalifoux PR. Diastema closure: using orthodontics, composite bonding, or porcelain veneers for optimal esthetics. Inside Dentistry. 2010;6(8):62-70.
6. McLaren EA, Phong TC. Ceramics in dentistry: classes of materials. Inside Dentistry. 2009;5(9):94-103.
7. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-13.
8. Reynolds JA, Roberts M. Lithium-disilicate pressed veneers for diastema closure. Inside Dentistry. 2010;6(5):46-52.
9. Helvey GA. Chairside cad-cam. lithium disilicate restoration for anterior teeth made simple. Inside Dentistry. 2009;5(10):58-66.
About the Authors
Rafael Santrich, CDT
President
VM Laboratory Technologies
Aventura, FL
Richard Canizares, DMD
Prosthodontist and Cosmetic Dentist
Dental Esthetic Solutions
San Juan, PR