Managing the Technical and Biologic Success of an Implant Abutment
Approaching the challenges presented by implant placement to ensure positive outcomes
Leon Hermanides, CDT
In keeping with the need to deliver biologic harmony as well as esthetics in restorative procedures, the dental laboratory is guided by a series of technical design criteria. What is not always understood in the laboratory, however, is it is the anatomical limitations of the patient that are the best predictors of the successful esthetic integration of the anterior implant restoration.1,2 Therefore, despite the dentists’ and laboratories’ best efforts, as well as the highest levels of surgical and technical competence, some implant restorations may never achieve the esthetic outcome anticipated.
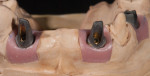
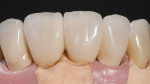
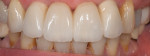
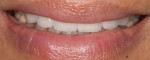
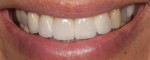
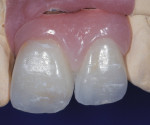
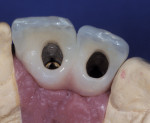
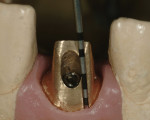
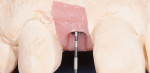
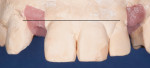
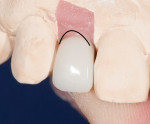
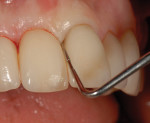
Additionally, considering the challenges posed by implant placement and the design of the implant system, it is understandable why many technicians and restorative dentists have been frustrated by the outcomes they achieve. Although the criteria for implant abutment manufacture will be presented in this article, the esthetic integration with the patient’s smile was determined before the implant was placed, and the role of the abutment in supporting the esthetics was limited by the treatment planning process for the final restoration (Figure 1 through Figure 5).
Cemented vs. Screw Retained Restorations
The first question to consider is: Why would we want to use an implant abutment? There appears to be a significant demand for the manufacture of screw-retained restorations over an abutment and cemented crown. The most obvious reason to use an abutment is to correct an implant placed at an angle that would leave the screw access hole as an esthetic liability. This is most common with maxillary anterior teeth, where the bony architecture tends to create a facial inclination of the implant to avoid apical perforation of the buccal plate. The implant therefore is inclined toward the facial and leaves the screw access hole either through the incisal edge or in the facial of the restoration (Figure 6 and Figure 7).
It has been noted in the literature3, 4 that screw access holes on screw-retained porcelain-fused-to-metal crowns lower the fracture resistance of the ceramic. The screw access hole becomes a liability because it weakens the ceramic enough to increase the occurrence of fractures in the veneering ceramic. Screw-retained implant restorations are at a higher risk of mechanical failure due to their increased risk of ceramic failure.
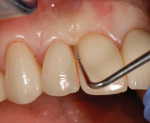
It additionally appears that the choice of either an abutment/cement-retained restoration or a screw-retained restoration has no significant impact on the survival rate of the implant.5,6,7 Although there are articles that would dispute these findings, all the authors agree that accessibility to the restorative margins to remove the excess cement is vital when an abutment is manufactured to create an esthetic outcome (Figure 8).
Processing Distortion
The fit of an implant-supported fixed partial denture is an important issue to consider when choosing between a cemented or screw-retained restoration.8 The data has shown in multiple studies that when evaluating frameworks fitted to implant fixtures manufactured by a variety of methods, there can be measureable distortion.9,10 By cementing the frameworks, the inaccuracies created by casting and bonding ceramic are minimized. Providing an adequate cement spacer mitigates the stresses transferred to the implants from conventional processing distortions. It has been demonstrated that the cement spacer does not compromise the retention of a cemented restoration and, in fact, improves the fit of the seated restoration.11
Adequate Inter-Occlusal Clearance
One of the challenges in manufacturing an implant abutment is creating adequate retention and resistance form to prevent the restoration from dislodging. When assessing the vertical space between the implant fixture surface and the opposing dentition, less than 5 mm would not provide sufficient space for the abutment margin (0.5 mm to 1 mm), adequate resistance form (3.5 mm), and the appropriate thickness of restorative material (1 mm). In these situations, a screw-retained restoration would be a better option, as the hardware required to manufacture the restoration would allow adequate thicknesses for the ceramic materials.
Retained Cement
The amount and accessibility of retained cement after the final delivery of a restoration is a notable argument against the use of a cemented crown and abutment. This can, however, be controlled during manufacture in the dental laboratory through the use of a soft-tissue model to accurately reproduce the soft-tissue profile around the implant. The restoration margin can therefore be predictably placed no more than 1.5 mm below the gingival margin. In fact, for a titanium or metal abutment, margin depths of 0.5 mm on the lingual, 1 mm on the mesial and distal interproximal region, and 1.5 mm on the facial should provide adequate access to the margins for the restorative dentist to clean the cement and hide the junction between abutment and restoration.
Soft-Tissue Model
In order to provide access to the implant replica during the manufacturing process, a soft-tissue model is required for implant restorations. This model uses an addition or condensation silicone material to replicate the soft-tissue contours surrounding the coronal third of the implant replica. Providing a clear view of the interface between the abutment and implant replica to ensure that the components are fully seated and to verify the fit of the restorations is critical during design and manufacture, particularly for fixed partial dentures. Additionally, this allows the dental technician to reproduce or sculpt the ideal emergence profile between the implant fixture and the gingival margin into the silicone material, which can then be replicated during the manufacture of the abutment (Figure 9 through Figure 11).
Material Selection
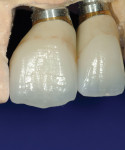
For anterior tooth replacement, material selection is an important factor in achieving esthetic success, depending on the amount of tooth and gum displayed in the smile. It has been shown that, depending on the thickness of tissue over the abutment, a titanium abutment may shadow through the soft tissues.12 When tissue thickness is less than 2 mm, the authors noticed that the human eye could detect the light reflection from the titanium abutment.
Considering the aforementioned observations, any implant placed facial to the adjacent teeth or less than 3 mm below the expected final gingival margin on a patient who shows the cervical of their teeth when smiling may require a zirconia abutment. This will minimize shadowing apical to the gingival margin seen with titanium abutments. Patients who do not show the cervical of their teeth in a large smile give the restorative team more flexibility in material choice, as the risk of the reflection of the metal showing is minimal.
Zirconia abutments are also an excellent option when the accessibility of the restorative margins is of concern, as it is possible to leave the margins closer to the final gingival margin. If there is any future recession, the junction between tooth and restoration is less visible, and there is less likelihood of the shadowing expected with a metal abutment.
Design Parameters
As with any restoration manufactured in the dental laboratory, there is a set of parameters that can be used to determine the outcome of the final result. The abutment needs to fulfill the following criteria:
Provide adequate retention and resistance form to retain the final crown and an appropriate path of insertion
Create an emergence contour that emulates the surrounding dentition
Keep the margins accessible for adequate cleaning of any retained cement
Retention and Resistance
An abutment taper of 6° and a minimum prep length of 3 mm to 4 mm are the ideal parameters for a tooth/abutment.13,14,15 This provides adequate retention and resistance form, assuming the screw access hole does not compromise the facial or lingual wall of posterior abutments or the mesial or distal wall of anterior abutments. The use of proximal retention grooves on posterior teeth can enhance the resistance to dislodging.
Emergence Profile
The emergence profile of an implant abutment is the most important restorative determinant of the facial gingival level, providing the anatomical limitations discussed earlier in this article are favorable. Placement of an implant in an unfavorable position in relation to the final tooth position poses the greatest challenge to the dental technician trying to develop favorable sub-gingival abutment contours.
Ideal placement of an anterior implant would be 3 mm to 5 mm apical to the gingival margin of the contralateral tooth or ideal tooth position. The facio-lingual inclination of the implant should be angled through the incisal edge and with the mesiodistal inclination parallel to the roots of the adjacent teeth.16 A faciolingual placement allowing 2 mm of buccal bone will additionally prevent loss of the facial tissue.17 Creating an appropriate emergence profile when all of these factors are ideal is relatively straightforward; however, the daily reality for the dental technician is that the implant placement usually does not meet one or more of these criteria.
There are three critical dimensions to the emergence profile of the abutment, the combination of which will determine the final position of the gingival margin, the presence of interproximal papilla, and the gingival profile of the restored tooth (Figure 15); they are: the facial emergence profile; the proximal emergence profile and proximity to allow appropriate contact placement; and the lingual emergence profile.
Facial Emergence Profile
It has been demonstrated that a concave profile can increase the volume of tissue17,18 around the abutment, and, conversely, that the convex profile of an abutment will create an apical migration of the soft tissue.17,19 Therefore as the facial profile of the abutment is developed, it is crucial to determine the required final gingival position of the restored tooth.
If the gingival margin of the restored tooth is apical to the contralateral tooth (the restoration would create a longer tooth), the profile of the abutment needs to be flat or concave. This would allow the tissue to drape further down the restoration, thus shortening its visual length. However, when the implant has been facially positioned, placed shallower than 3 mm below the gingival margin, or placed with an excessive facial inclination, the opportunity to correct the visual length of the restoration is compromised.
Conversely, when the gingival margin is coronal to the contralateral tooth (the restoration would create a shorter tooth), the profile of the abutment can be slightly convex in order to displace the soft tissue apically and correct the visual length of the restoration. This can be done by adjusting the gingival level and soft-tissue profile on the soft-tissue model and manufacturing the abutment to this modified profile. However if the implant has not been positioned 3 mm to 5 mm deep relative to the final gingival margin, modification may not be possible. Such an instance is demonstrated in Figure 12 and Figure 13.
Proximal Emergence Profile
The proximal contours of the abutment influence the presence of interproximal tissue by providing adequate emergence for the appropriate crown contour and contact point placement.20,21 For the single-tooth-replacement implant, the bone level and the presence of the interproximal papilla are determined by the adjacent teeth (Figure 14 and Figure 15).22 In adjacent implants, the inter-implant distance appears to influence the height of interproximal bone and corresponding interproximal papilla (Figure 16 and Figure 17).23,24
It is not the abutment that “supports” the tissue, but rather the ability of the abutment and restoration to favorably conform to the anatomy and existing tissue volume, which will in turn create the gingival profile and interproximal papilla. The emergence profile of the abutment in the interproximal regions should therefore begin to approximate the contours of the natural tooth to provide a seamless transition to the restoration.
Lingual Emergence Profile
The lingual profile has little impact on the peri-implant esthetics and can be adapted to form the expected contour of the root of a tooth.
Stock Versus Custom Abutments
As the parameters for emergence profiles and margin accessibility of an abutment are understood, it becomes more difficult to justify the use of stock abutments for anterior teeth. The profiles of stock abutments are developed to a perceived ideal by the implant company, and they allow the technician to adapt the core to the required angulation, length, and taper.
It is possible to differentiate between anterior and posterior teeth in the choice of abutment. As the esthetic requirements for a posterior restoration and the flatter scallop of the interproximal bone provide greater flexibility, the use of a stock abutment is more appropriate for posterior implant restorations (Figure 18).
The relative cost of currently available CAD/CAM options for custom abutments and the quality of the final restorative outcome does, however, support a recommendation for the use of a custom abutment for implant restorations in the esthetic zone.
Conclusion
In summary, a custom-made implant abutment is recommended for anterior implant restorations, particularly for higher-risk esthetic patients. An adequately designed implant abutment will provide the patient a long-term benefit, and the final esthetic outcome of the restoration can be controlled within the abutment by controlling the intra-sulcular profile and material choice. Finally, access to the restoration margin for cement removal can be controlled by margin placement relative to the gingival margin.
References
1. Hermanides LP. Implants in Your Laboratory. Journal of Dental Technology. 2009;26(August-September):16-20.
2. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001; 22(3):199-206.
3. Shadid RM, Abu-Naba’a L, Al-Omari WM, et al. Effect of an occlusal screw-access hole on the fracture resistance of permanently cemented implant crowns: a laboratory study. Int J Prosthodont. 2011;24(3):267-269.
4. Torrado E, Ercoli C, Al Mardini M, et al. A comparison of the porcelain fracture resistance of screw-retained and cement-retained implant-supported metal-ceramic crowns. J Prosthet Dent. 2004;91(6):532-537.
5. Weber HP, Sukotjo C. Does the type of implant prosthesis affect outcomes in the partially edentulous patient? Int J Oral Maxillofac Implants. 2007;22 Suppl:140-172.
6. Vigolo P, Givani A, Majzoub Z, Cordioli G. Cemented versus screw-retained implant-supported single-tooth crowns: a 4-year prospective clinical study. Int J Oral Maxillofac Implants. 2004;19(2):260-265.
7. Nissan J, Narobai D, Gross O, et al. Long-term outcome of cemented versus screw-retained implant-supported partial restorations. Int J Oral Maxillofac Implants. 2011;26(5):1102-1107.
8. Karl M, Taylor TD, Wichmann MG, Heckmann SM. In vivo stress behavior in cemented and screw-retained five-unit implant FPDs. J Prosthodon. 2006;15(1):20-24.
9. Hjalmarsson L, Örtorp A, Smedberg JI, Jemt T. Precision of fit to implants: a comparison of Cresco™ and Procera® implant bridge frameworks. Clin Impl Dent Relat Rest. 2010;12(4):271-280.
10. Karl M, Rösch S, Graef F, et al. Strain situation after fixation of three-unit ceramic veneered implant superstructures.Implant Dent. 2005;14(2):157-165.
11. Olivera AB, Saito T. The effect of die spacer on retention and fitting of complete cast crowns. J Prosthodont. 2006;15(4):243-249.
12. van Brakel R, Noordmans HJ, Frenken J, et al. The effect of zirconia and titanium implant abutments on light reflection of the supporting soft tissues. Clin Oral Implants Res. 2011;22(10):1172-1178.
13. Kaufman EG, Coelho DH, Colin L. Factors influencing the retention of cemented gold castings. J Prost Dent. 1961;11(3):487-502.
14. Maxwell AW, Blank LW, Peulleu GB Jr. Effect of crown preperation height on the retention and resistance of gold castings. Gen Dent. 1990;38(3):200-202.
15. Leong EW, Choon Tan KB, Nicholls JI, et al. The effect of preparation height and luting agent on the resistance form of cemented cast crowns under load fatigue. J Prosthet Dent. 2009;102(3):155-164.
16. JC, Phillips K Kois. Aesthetic peri-implant site development. The restorative connection. Dent Clin North Am. 1998;42(1):57-70.
17. Su H, Gonzalez-Martin O, Weisgold A, Lee E. Considerations of implant abutment and crown contour: critical contour and subcritical contour. Int J Periodontics Restorative Dent. 2010;30(4):335-343.
18. Rompen E, Raepsaet N, Domken O, et al. Soft tissue stability at the facial aspect of gingivally converging abutments in the esthetic zone: a pilot clinical study. J Prosthet Dent. 2007;99(6 Suppl):S119-125.
19. Phillips K, Kois JC. Aesthetic peri-implant site development. The restorative connection. Dent Clin North Am. 1998;42(1):57-70.
20. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996.
21. Kois JC, Kan JY. Predictable peri-implant gingival aesthetics: surgical and prosthodontic rationales. Pract Proced Aesthet Dent. 2001;13(9):691-698.
22. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):563-568.
23. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
24. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4)546-549.
About the Author
Leon Hermanides, CDT
Owner
Protea Dental Studio, Inc.
Redmond, WA
Clinical Instructor
Kois Center
Seattle, WA