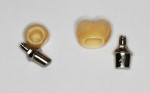
BellaTek® Laboratory-Designed Abutments
Laboratories can have complete control over the design of precisely fabricated, patient-specific CAD/CAM abutments.
Today when debilitated teeth are being rehabilitated with dental implant therapy, patients expect both function and esthetics. For clinicians and laboratory technicians who are fabricating implant-supported prostheses, the ability to fabricate patient-specific abutments is paramount. Computer-aided design and computer-aided manufacturing (CAD/CAM) techniques have been essential to making this possible. Such techniques were first introduced to dentists in 1971, and by 1998, the first customized implant abutments were being created with CAD/CAM technology. Like cast custom abutments, patient-specific abutments created with CAD/CAM technology have the potential to provide customized peri-implant, soft-tissue support. This is essential to achieving an optimal esthetic result. The inherent dimensional inaccuracies of waxing, investing, and casting are eliminated by the CAD/CAM process, as is the subsequent need for finishing the abutments after machining. Such abutments fit more precisely than stock or cast ones.
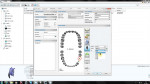
CAD/CAM technology can give dental technicians complete control over abutment design within cleared design parameters (Figure 1). The technician also can select the material (titanium, titanium nitride-coated, or zirconia) that best matches the restorative material and planned function associated with the definitive prosthesis.
The following describes the steps taken by the laboratory technician to design a patient-specific BellaTek® CAD/CAM abutment after receiving
an implant-level impression from the clinician.
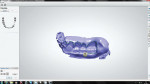
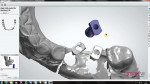
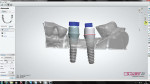
The process begins with the technician mating implant analogs to the impression copings in the impression and fabricating a master cast with soft tissue. The case is set-up in the Order Form of the 3Shape Abutment Designer software by selecting the BIOMET 3i Library. In the software, the dental technician selects the position of the abutments and the materials (titanium, titanium nitride-coated, or zirconia) (Figure 2.) The technician then initiates a series of scans, capturing soft tissue of the master cast and the index of the opposing dentition (Figure 3 and Figure 4). After the initial scans, specific scan caps are attached to the analogs in the cast (Figure 5), the entire assembly is sprayed with an appropriate anti-reflective powder, and then it is scanned.
Once scanning is complete, the design of the abutment(s) is carried out. This process begins by marking the location of the virtual scan cap that is selected from the library and placed in the 3D computer model of the arch (Figure 6). After the scan and alignment of the master cast and opposing dentition are completed (Fig. 7), the software begins the abutment-design process. Then the technician refines the design (Figure 8 through Figure 10).The software’s “Parametric” tool is used to define the margins, establish the emergence curve, create the margin shape, and set the emergence profile. The shape of the abutment occlusal surface is adjusted with the Sculpt Tool; contouring of the abutment’s overall shape is accomplished with the Virtual Wax Knife. The latter enables material to be subtly added, removed, and/or smoothed after the overall shape has been established.
The final step is to check that the abutment’s screw head will not be visible and no breakthrough will be generated during machining. This is accomplished using special tools in the Dental Designer Software.
The completed abutment design is sent electronically to the BellaTek Production Facility (BIOMET 3i) for computer numerically controlled (CNC) milling of the abutment(s) (Figure 11). Use of the CAD/CAM technology eliminates the need for the laboratory technician to physically send the master cast to the production facility. This saves time and serves the greener consciousness that has begun to permeate dental
offices and laboratories worldwide.
While the case presented here began with the laboratory receiving an implant-level impression made using implant impression copings, data may also be acquired from patients for fabrication of patient-specific BellaTek Abutments in two other ways. If the clinician places BellaTek Encode Healing Abutments, the need for impression copings can be eliminated. The healing abutments identify the implant-platform diameter, healing abutment height, hex position of the implant, and diameter of the emergence profile by means of various
arrangements of facets or codes on the abutment occlusal surfaces. Custom BellaTek Abutments are fabricated from supragingival impressions made by the dentist and from the master cast (Figure 12).
More recently, it has also become possible to record the patient’s intraoral geometry (tooth preparations and/or CADCAM healing abutments) with a digital scanner rather than a conventional elastomeric impression. This further simplifies design of the abutment for the laboratory technician, as it eliminates the need for pouring, mounting, and scanning the master cast.
Asa Karner, CDT, is the manager of Dentalgruvan Dental Laboratory in Falun, Sweden.
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dental Technology.
For more information, contact:
Biomet 3i
Phone: 800-342-5454
Web: www.biomet3i.com
E-mail: 3ics@3implant.com