Full-Arch Restorations on CAD/CAM-Milled Titanium Bars—Part II
When fabricating an implant-supported screw-retained hybrid prosthesis, bar design, injection processing, and finishing techniques need to be considered.
In this continuation of “Full-Arch Restorations on CAD/CAM-Milled Titanium Bars,” which appeared in the September 2011 issue of Inside Dental Technology, the author addresses the second stage of this process, beginning with the criteria for proper bar-design selection.
TO READ TOM WADE’S FIRST ARTICLE ON FULL-ARCH RESTORATIONS, PLEASE VISIT:
The two basic “styles” of CAD/CAM-milled bars include the more popular screw-retained hybrid (SRH)—ie, fixed detachable—and the attached overdenture bar. Within those two categories are subcategories. For screw-retained hybrid prostheses, the two main design style subcategories are the “full-wrap” and “Montreal.”
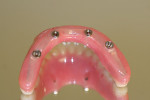
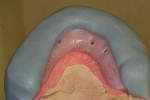
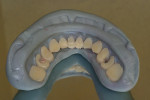
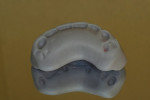
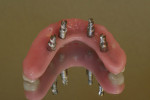
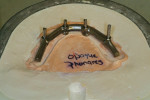
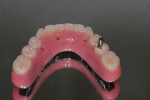
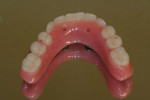
The full-wrap design (Figure 1) is probably the most common because it is generally the fastest and easiest to create. However, sometimes the full-wrap design is overused for that same reason—most often on mandibular prostheses. The real advantage of this design, other than its ease, is the fact that acrylic can be added or removed from the intaglio surface on cases where ongoing tissue management is an issue. This concurrently relieves the technician of the daunting task of creating an undulating and convex, highly polished intaglio surface that either lightly impinges on the tissue or maintains a constant 0.5-mm to 1-mm distance from it—especially in the maxilla, where air escape and phonetic considerations often exist.
A disadvantage of the full-wrap design is that it leaves the technician with a series of “circular finish lines.” If care is not taken to provide a true butt-joint finish line, the “lapping” of acrylic over the polished titanium surface can become a point of seepage, allowing infiltration of bacteria and smaller particles that can cause the area immediately encircling the implant to become a source for difficult hygiene. Such seepage also results in staining, which eventually causes a breakdown of the bond between the bar and the acrylic. Neither scenario is desirable.
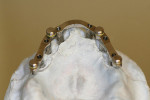
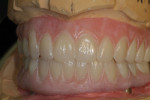
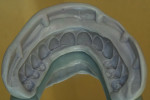
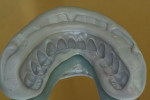
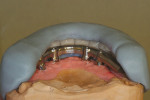
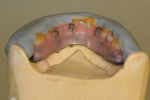
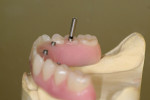
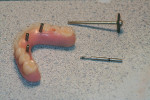
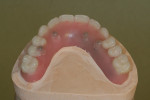
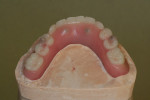
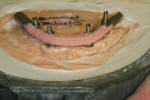
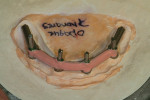
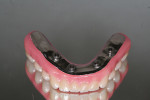
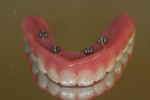
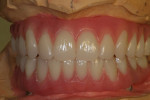
Highly polished medical-grade titanium is very biocompatible and hygienic, which is why the Montreal-style bar (Figure 2 and Figure 3) is desirable for use in implant-supported overdenture cases whenever possible. This design allows for mirror-polished titanium to extend up from either the implant interface or abutment and “splay” out to complete a mirror-polished titanium intaglio surface up and away from the tissue and implant interfaces to a mono-linear finish line. For many years—long before CAD/CAM technology and titanium were used—this was the way hybrid prostheses were fabricated out of cast gold. It should be noted that a properly designed Montreal-style bar could be modified by a skilled technician to accept a full wrap of acrylic to meet receded tissue if needed.
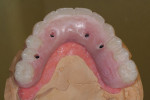
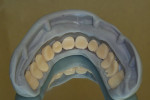
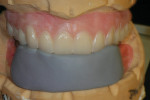
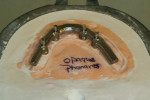
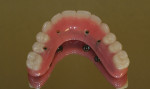
Using NobelProcera™ CAD software (Nobel Biocare, www.nobelbiocare.com), one of the primary designs for attached overdenture bars is the “free-shape milled bar” (Figure 4). This bar design is a simple, highly polished, rectangular bar that can accept attachments, and the walls can incorporate a specific degree of taper from 0º to 10º in increments of 2º. Another excellent choice for overdenture bar design is the “Paris” bar (Figure 5). This design is basically a Montreal-style hybrid bar that has been modified to accept attachments and also has controlled tapered walls. This bar design allows the bar—rather than the attachments—to absorb most of the vertical and lateral forces, therefore relegating the attachments to being only retentive elements as intended. It also has the mirror-polished convex intaglio surface, which is very hygienic and works in harmony with floss. The lingual 90º “inset” also allows room to incorporate the precision cast chrome reinforcement mesostructure required for this type of prosthesis to avoid ongoing breakage issues.
Note: due to space restrictions, the aforementioned mesostructure and the completely different processing procedures of attached overdentures will not be addressed at this time in order to allow the authors to focus on processing more widely prescribed screw-retained hybrids.
Initial Processing
Once the hybrid bar has been received from the milling center, the previously approved and scanned wax tooth setup is reseated (Figure 6 through Figure 8), and a Sil-Tech® (Ivoclar Vivdent, www.ivoclarvivadent.com) silicone matrix is fabricated to fully encompass the entire facial, incisal/occlusal area as well as the buccal land area of the cast (Figure 9 through Figure 12). The denture teeth are then removed from the wax-up and carefully placed and secured accurately into the matrix (Figure 13 and Figure 14). Any stone surfaces on the ridge should be lubricated, the titanium bar should be screwed back on the cast, and the matrix should finally be placed back on the cast (Figure 15). It is important to carefully check that none of the denture teeth are prematurely contacting the bar and are seated properly around the guide pins (Figure 16). If it is a case with tight vertical space and the bar was designed close to the teeth, it is advisable to check each tooth individually to ensure there is no contact with the bar as they are placed into the matrix. Once this is achieved, well-molten wax is used to flow accurately around all of the teeth to bond them to the bar (Figure 17). Although this “jumping” method is a good way to set teeth on the titanium bar in the same position and occlusion as previously approved on the LC resin basebar, it will result in only 90% to 95% accuracy. For complete accuracy, a separate anterior incisal-edge matrix must be used (Figure 18 and Figure 19). This will ensure absolute accurate replacement of the anteriors. It is also important to check and re-tighten the posteriors to ensure tight occlusion before doing a final esthetic wax-up to accommodate the final clinical try-in so that bar passivity—as well as esthetics, occlusion, and contours—is confirmed.
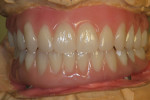
Some clinicians prefer to try in the bar as received from the milling center (Figure 20 and Figure 21). However, there should still be a final try-in with the teeth and wax-up completed on the bar (Figure 22).
It is highly recommended to process screw-retained hybrids on a separate processing model that has been created with an additional set of analogs and guide pins (chimney screws) to create perfect screw shafts. Although the bar is already milled, the best practices call for the use of a near-zero expansion Type IV die stone for creating any model that has analogs—especially any cast that is to be scanned. There are several major advantages to maintaining the unscathed mounted master cast. The first advantage is that in the unlikely case something should go wrong with the acrylic or teeth in processing, the bar can be stripped and the case can be started over. Second, it allows for very accurate final milling and occlusal scheme fine-tuning and makes for a nice presentation to the clinician for review before the prosthesis is placed in the mouth. Should any future maintenance issues arise—such as a tooth failure or the need to completely “re-tread” the teeth and acrylic—it offers a simple and time-efficient method for doing so, requiring only retraction and reseating by the clinician without an impression.
Although some designers use the titanium cylinders on the bar to create the screw access shafts, the author believes this presents too much bulk and interrupts the polymethylmethacrylate (PMMA)—especially when it is under a tooth. The amount of pink base acrylic is so minimal with many of these devices that, other than obtaining the minimum dimensions required to achieve reliable bar strength and integrity, there should be no more metal than necessary because it is better to have as much base acrylic as possible for overall strength and bonding to the denture teeth.
Final Processing Steps
The final processing phase begins by selecting the proper guide pins and seating them, marking about 2 mm above either the pink wax or tooth occlusal, depending on its exit point (Figure 23). The pins are then retracted and cut with a disc. The heads of the pins are “slotted,” making sure care is taken to avoid using a disc that is too thick and centering the slot in a fashion that will not weaken the side walls (Figure 24 and Figure 25). Once this has been completed for all the fixtures, they are seated into the analogs (Figure 26 and Figure 27) and the processing cast is poured. Note: If the design is a full-wrap, it is highly recommended that the technician make sure the wax is in the proper place with regard to the abutment cylinders or “legs” of the bar, preferably to the defined finish lines. If the implants are supergingival, the wax must be at least 1 mm to 2 mm away from the interface because it is much more difficult and dangerous to clear it back in the acrylic.
Once the processing patty is set up, the technician should then flow a “thin skin” of wax over the tops of each guide pin (Figure 28 and Figure 29). This makes it possible to flask the arch in the same manner as any full-arch restoration. After processing, the thin skin—now in acrylic—can be easily removed with a new No. 11 stiff bristle brush without harming the slotted screw head.
At this point, the hybrid is ready to be invested into the injection flask (SR Ivocap® Injection, Ivoclar Vivadent). Once fully invested and boiled clean (Figure 30 and Figure 31), all of the normal preparations are made. However, we want to avoid creating diatorics when using Phonares® nanohybrid composite teeth (Ivoclar Vivadent), but rather roughen the surface and clean thoroughly with monomer.
Prior to closing for injection, it is critical to ensure that there is absolutely no wax residue on the bar side of the flask. If the bar is removed from the cast during any of the preparation procedures—eg, while applying separator or applying metal bond or opaque to the bar—each guide pin must be “mapped” to ensure it is reassembled correctly.
It is paramount to maximize the bond between all of the components, especially the PMMA resin to the teeth as well as to the bar. Using GC Primer Metal Bond (GC America, www.gcamerica.com) on all clean, raw titanium surfaces is recommended—whether they are to interface with acrylic or a light-cure opaque such as Telio (Ivoclar Vivadent) or GC Gradia® (GC America) in the esthetic zone. The author recommends coating only the necessary esthetic zone areas (Figure 32 and Figure 33), because he believes that the bond is somewhat compromised with a layer of opaque and not as effective as it is with acrylic processed directly to titanium with metal bond primer. Also, extreme care must be taken when applying opaque. It is recommended that it be applied in two thin, well-cured layers. Note that sometimes uncured, unbonded opaque can be “blown off” the bar under injection pressure and rolled into the acrylic, which will lead to issues with the final prosthesis. It is likely that soon most bar manufacturers will offer pink and perhaps even tooth-colored titanium and chrome cobalt surfaces via an anodizing process that will eliminate the need to add any layers of opaque and allow for maximum bond; however, currently, Cagenix™ (www.cagenix.com) is the sole manufacturer offering pink titanium-milled implant bars.
Sealing the circular area where the guide pin enters into the bar with a small amount of either pink or tooth-colored self-cure acrylic is also recommended. This will ensure that the injected, processed acrylic cannot enter the area and work its way to the bottom of the shaft near the screw seat, where it could adversely affect the seating of the final screw.
After all preparations are carefully made, the flask is closed and the normal injection process occurs. While the injection technique has been around for a long time, it greatly improves the precision of fit and occlusion as well as the density, strength, and hygienic quality of any device—properties that have never been more important to the overall success and longevity of prostheses than with these multiple-implant, full-arch restorations.
After proper cooling and de-flasking, the prosthetic device is retracted from the processing patty. To remove it from the processing model for finishing, the thin skin of the acrylic encasing the screw heads must first be removed, using a new stiff bristle brush (Figure 34). To facilitate screw removal from the tightly processed acrylic, use a wood-burning tool to contact the screw head (Figure 35) for a couple of minutes to heat the encompassing acrylic slightly—taking care not to overheat and damage the surrounding acrylic. To facilitate the breaking of the initial seal, slowly and carefully unthread the screw, which will also lift the screw until it “jumps thread,” indicating that it is no longer engaged. At that point, the screw will be protruding far enough to be grasped with small pliers and extracted.
The device is then returned to the master cast and the articulator for normal milling and excursion tuning. At this juncture, it is important to point out that it has been established that well-osseointegrated implants of proper diameter and length can successfully withstand and support the forces of cuspid-rise occlusal schemes. However, even highly advanced components—specifically premium denture teeth and their bond to the base acrylic—oftentimes cannot achieve this. Therefore, it is recommended that heavy anterior guidance and cuspid rise be avoided, especially in light of the fact that patients fitted with these implant-supported dentures have no propriaception and cannot really tell whether they are biting down on a spaghetti noodle or the tip of a fork tine.
To achieve a desirable esthetic result, after grinding the mounting is maintained to touch up any areas where pink acrylic processed into the “slop” space that was ground into a denture tooth to properly fit around a guide pin. If that procedure is necessary, the technician should precisely grind out whatever pink is in the tooth body, clean it with monomer, replace the guide pin into the hole, and add tooth-shade acrylic to fill in the discrepancy. After it is fully cured in the pressure pot, the technician should remove the pin, re-mill into centric and excursive movement, add a small amount of secondary anatomy, and finely re-polish, using small bristle brushes for light pumice and high shine to restore to a “new” occlusal condition (Figure 36).
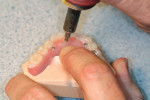
To finish and polish the entire prosthetic device, the technician should follow normal acrylic and metal finishing procedures. However, additional care must be taken to ensure that the implant interfaces are protected and remain absolutely untouched. Nobel Biocare manufactures “protection caps,” which are nothing more than slightly oversized analogs that will protect the interfaces so that they remain unscathed during the entire finishing process. It is far more tedious and dangerous to finish a full-wrap device with a series of circular finish lines around the bar leg/implant interface than the mono-linear finish line that is well away from the interfaces on the Montreal-style bar (Figure 37). Where finishing procedures are performed near the metal-acrylic junction, the author recommends using a rubber point or wheel, rather than a bur, when touching the titanium, as doing so will reduce the time and effort required to restore the high luster to the titanium.
Once the prosthetic device has been properly milled, finished, and polished, it is then ready to be steam-cleaned and finally seated back to the master cast and articulator for presentation to the clinician for final insertion in the mouth (Figure 38 through Figure 42).
Conclusion
Although it is indeed a long tedious process to methodically plod through the many steps necessary to reverse engineer one of these devices, it is very rewarding to the entire restorative team when the clinician seats the device with predictable, successful results.
About the Author
Thomas Wade, CDT
Owner
New Horizons Dental Laboratory
Broomfield, Colorado
To sign up for Tom Wade's courses on "Master Dentures on Implants," please visit:
dentalaegis.com/go/idt26