A High-Strength, Metal-Free Alternative to Traditional Denture Prostheses
Innovative techniques provide long-term and patient-pleasing results.
Implant-supported fixed prostheses have gained acceptance among dentists and laboratory technicians alike for their ability to deliver proven and dependable functionality in combination with desired esthetics.1 The advent of new implant materials and techniques affords dentists, technicians, and the growing edentulous population opportunities for more comfortable, stable, and natural-looking treatments. When four or more implants are placed to support a full-arch prosthesis, for example, patients experience enhanced support and comfort, as well as decreased bone loss.2 However, the forces placed on such prostheses as a result of the support provided by implants mandate the use of more durable, odor-free substructures as well as denture teeth that can withstand wear and deformation.2,3
High-strength zirconia substructures that are designed and fabricated with CAD/CAM processes represent strong and durable alternatives to conventional denture prostheses. CAD/CAM technology can be used in the office or laboratory to fabricate inlays, onlays, crowns, veneers, implant abutments, fixed partial dentures, and full-mouth restorations.4 Simultaneously, all-ceramic restorations provide immeasurably better esthetic results compared to their porcelain-fused-to-metal (PFM) counterparts—which have been the traditional crown restoration of choice for dentists over the years. Zirconia-based, all-ceramic restorations with layered porcelain are increasingly used as a dependable and esthetic alternative. However, they have been known to chip.
Because zirconia exhibits thermal diffusivity and heats at a different rate than porcelain, it has the propensity to separate from the substructure and chip or crack.5 Research has indicated that porcelain stress and the stress between the porcelain/zirconia interface is minimized when the porcelain-layered, zirconia-based substructure is slowly heated, then subjected to a slow-cool thermal cycle.6,7 Prepared accordingly, the risk of failure for the porcelain overlay has been reduced to less than 6%, and less than 1% for the zirconia core.7
Such results indicate that the preparation technique for porcelain-layered, zirconia-based substructures becomes essential to the success of the restorations. There are laboratory ceramists experienced in the successful preparation of zirconia substructures and the application and use of layering ceramics. The secret to strong, reliable zirconia-based restorations is the firing technique. The zirconia restoration layering procedure is much the same as for regular porcelain.8 However, when layering zirconia, firing the first layer at a temperature hotter than recommended by the manufacturer produces the characteristics of a bonding agent, ensuring a long-lasting and reliable restoration.9 Life-like esthetics can be achieved using porcelain shades and stains that appropriately diffuse light, creating the illusion of depth by incorporating varying opacities to replicate the appearance of natural dentition.
As a result, when zirconia substructures are fitted with customized, pressed all-ceramic restorations instead of prefabricated resin denture teeth, edentulous patients have a predictable and highly esthetic fixed prosthetic that will serve them for the long term.
Case Presentation
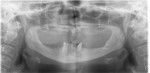
A 68-year-old woman presented with an existing maxillary denture and missing lower teeth. Diagnostic radiographs were taken, along with other records (Figure 1). It was determined that the remaining lower teeth would be extracted and an All-on-4 (Nobel Biocare, www.nobelbiocare.com) prosthesis would be designed. To facilitate a more ideal ridge width at the implant head, occlusal planning of the alveolar ridge would be performed.
Clinical Protocol
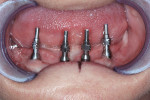
An implant surgical guide was fabricated to guide placement of the four RP NobleActive™ (Nobel Biocare) implants, in addition to multi-unit transmucosal abutments to facilitate tissue level emergence (Figure 2). Following implant placement, implant impression copings were placed after they were luted together using clear-pattern resin (GC America, www.gcamerica.com) (Figure 3). An impression was then taken for use in fabricating the master cast.
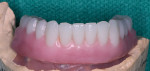
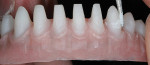
To guarantee the passive and accurate fit of the final prosthesis substructure, a laboratory verification jig was made from the master cast. Then, an occlusal wax rim was created to set up the mandibular tooth arrangement and function. The implant anterior–posterior spread allowed for basic tooth set-up from teeth Nos. 19 through 30 (Figure 4).
At the doctor’s office, the set-up was screwed in and the bite was verified. Phonetics, function, and esthetics were approved. A silicone matrix was formed after the mandibular denture was processed with metal temporary abutments in place that were used as a long-term temporary.
Laboratory Protocol
The substructure that would be scanned or copy-milled for the CAD/CAM zirconia substructure was created to accommodate IPS e.max® (Ivoclar Vivadent, www.ivoclarvivadent.com) pressed restorations and pressed gingival ceramics (Figure 5). This substructure would restore the lost vertical of the alveolar bone process and teeth.
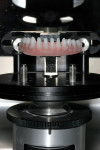
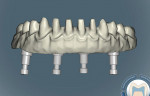
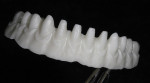
The copy mill substructure was then scanned for the CAD/CAM designing process using the NobelProcera™ Scanner (Nobel Biocare) (Figure 6). The zirconia substructure was then designed using the CAD/CAM software (Figure 7) after the zirconia framework was CAM-milled (Figure 8). A full-contour wax-up of 12 single IPS e.max Press restorations was then performed (Figure 9). To prevent damage to the zirconia surface, the framework was not blasted with aluminum particles.
A specialized bonding liner material, IPS e.max Ceram ZirLiner was mixed to a creamy consistency, and a thin layer was applied to the substructure to ensure a predictable bond and depth of color. The esthetics of the gingival areas were enhanced with berry and rose IPS e.max gingival stains (Figure 10) after the liner was dried and then fired.
A silicone matrix of the denture tooth set-up was used to inject wax onto the zirconia substructure in order to copy the vertical, midline, and tooth arrangement. The exact dimensions would then be incorporated into the final IPS e.max Press tooth restorations. In order to use the full 400-MPa strength of lithium disilicate, a slight cutback and ceramic layering technique was used on the anterior teeth only.
Seating
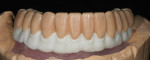
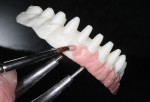
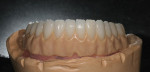
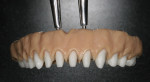
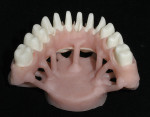
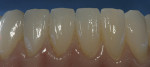
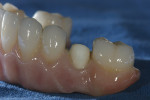
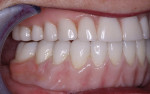
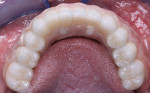
The single-unit IPS e.max crown restorations were stained and glazed, then seated back on the zirconia substructure, and a final hand-waxing of the tissue architecture was completed (Figure 11). The crowns were removed, and the case was then sprued, invested, and pressed with IPS e.max ZirPress gingiva 3 (Figure 12). It was divested, cleaned, and separated from the sprues and prepared for staining and glazing in order to mimic nature through form, function, and tissue textures (Figure 13). Ten of the restorations were then carefully bonded into place, resulting in an amazingly esthetic final prosthesis (Figure 14 and Figure 15). The case was cleaned and polished for final delivery, where it was torqued to the implants (Figures 16, Figure 17 and Figure 18). The final two bicuspid crowns were then bonded to the substructure.
Conclusion
CAD/CAM technology and pressable and milled ceramics enable dentists and laboratories to provide highly esthetic, durable, and stable treatments to edentulous patients.4 The development of new implant structures and materials provides edentulous populations with innovative longer-term alternatives that provide more comfort and are esthetically advanced compared to conventional options. Because implant-supported prostheses require stronger substructures and more durable tooth formations, materials such as zirconia and IPS e.max ZirPress provide prostheses with superior characteristics.2,3 The case presented here demonstrates the manner in which a high-strength zirconia substructure, in combination with state-of-the-art implant techniques, can satisfy patient demands for esthetics, strength, and comfort.
Acknowledgements
The author would like to acknowledge Dr. Charley Varipapa of Alexandria, Virginia, and Dr. Chris Mazzola, AACD, of Sun Valley, Idaho, who helped him develop much of this technique 15 years ago using metal castings and porcelain-fused-to-metal restorations. He would also like to thank Dr. Brandon Williams for treating this case. And finally, special thanks to Jordan Lott for the photography, as well as Jason Boyce, Brian Smith, and Jordan Lott for their everyday collaboration which makes these types of cases such a joy to fabricate.
References
1. Vogel RC. Implant overdentures: a new standard of care for edentulous patients current concepts and techniques. Compend Contin Educ Dent. 2008;29(5):270-278.
2. Henry K. Q&A on the future of implants. Dental Equipment and Materials. 2006; September/October.
3. Rossein KD. Alternative treatment plans: implant-supported mandibular dentures. Inside Dentistry. 2006;2(6):42-43.
4. Davidowitz G, Kotick PG. The use of CAD/CAM in dentistry. Dent Clin North Am. 2011;55(3):559-570.
5. Roediger M, Gersdorff N, Huels A, Rinke S. Prospective evaluation of zirconia posterior fixed partial dentures: four-year clinical results. Int J Prosthodont. 2010;23(2):141-148.
6. Kahng L. Understanding zirconia backgrounds for custom shade matching. J Cosmet Dent. 2009;24(4):94-100.
7. McLaren EA, White SN. Survival of In-Ceram crowns in a private practice: a prospective clinical trial. J Prosthet Dent. 2000;83(2):216-222.
8. Vichi A, Louca C, Corciolani G, Ferrari M. Color related to ceramic and zirconia restorations: a review. Dent Mater. 2011;27(1):97-108.
9. McLaren EA, Giordano RA. Zirconia-based ceramics: material properties, esthetics, and layering techniques of a new veneering porcelain, VM9. Quintessence Dent Technol. 2005;28:99-111.
About the Author
Stan Lott, CDT, AACD
Owner
Precision Dental Arts
Twin Falls, Idaho
For tips on producing photos just like Stan’s, log onto: aegisdentalnetwork.com/go/idt21