Bleeding on Probing Scoring for Patients
How to Enhance the Dental Hygiene Maintenance Visit
Joseph R. Greenberg, DMD, FAGD; Joy Jones, RDH; Wendy Mercaldo, RDH
Many dental practices employ licensed dental hygienists to treat patients at regular intervals for professional monitoring and maintenance. Together, the dentist and hygienist determine the duration of time allotted, the frequency of visits, and the protocol followed for each visit.
An important aspect of a maintenance visit is examination of the patient for inflammatory periodontal disease, which ranks among the most common chronic infections in humans.1 In 2009, Shumaker and colleagues published an article highlighting the importance of the bleeding on probing (BOP) score to detect and evaluate periodontal inflammation around teeth and dental implants.2 They asserted that a BOP score provides evidence-based predictability as an indicator of disease around dental implants and teeth and can be used to determine the frequency of maintenance visits. Patients who presented with high BOP scores (more than 16% of possible sites) were found to have increased attachment loss, whereas patients with BOP scores at < 10% of sites did not. Patients with high BOP scores are recommended for treatment, not maintenance. A single intervention of nonsurgical therapy can be successful in controlling disease activity during the maintenance phase of care. Long-term studies show that after periodontal surgery, recurrent disease that is found during maintenance therapy responds favorably to nonsurgical treatment in 88% of cases.3
The BOP protocol requires a gentle insertion of the periodontal probe tip into the sulcus, followed by a gentle sweep around from proximal surface to proximal surface. The gentle probe insertion can be 1 to 2 mm deep, depending on the nature and character, or biotype, of the gingiva.4 A tapered or parallel-sided probe tip may be used with comparable results.4 Any bleeding seen within 10 to 15 seconds after removing the probe tip should be recorded. Studies have shown that the absence of BOP indicates a state of health that will likely continue for several months after this examination.5 Recent data suggest that chronic inflammation of all types, including periodontal disease, can negatively affect systemic health.6
The BOP procedure is not an attempt to record pocket depth, which is a subsequent, separate process. The BOP procedure should be the first soft-tissue instrumentation performed by the dentist or dental hygienist for that patient on that visit. Any bleeding points that are found should be recorded in the patient's chart for that same appointment. This charting is used for assessment of the patient's personal biofilm control efficacy and for comparisons at subsequent visits. For example, if the bleeding points are found mostly on buccal or lingual surfaces, the likelihood is that the patient's toothbrushing technique needs to be addressed. If bleeding points are mostly interproximal, then the patient's interdental cleansing habits likely need improvement.
Materials and Methods
The following is a report of one dental practice's experience in converting a dental hygiene maintenance visit to a treatment protocol directed by the BOP score. The dentist and dental hygienists were calibrated for assessing BOP by performing this procedure on each other and a few selected patients to regulate the pressure and coverage of the gingival sweep. After approximately 7 years of the BOP-directed protocol, 52 consecutive patients (starting April 25, 2017) who attained a BOP score of 0 (ie, no bleeding on probing) were questioned as to how they personally achieved this desirable score. No single means of achieving success was reported; different patients reported using different types of toothbrushes, different brands of toothpaste, and different types of flossing materials and regimens.
Results
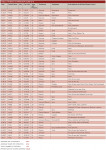
The study was completed on July 6, 2017, after BOP scores of 0 had been tabulated for 52 patients. A total of 172 patients were seen by one of 2 dental hygienists during the tabulation interval (April 25-July 6, 2017). The percentage of patients with zero bleeding was 30.2. The average age of the patients was 64.7 years, and average duration in the practice was 21.4 years. Details and preferences of each of the 52 high-performing patients of the study are shown in Table 1 (available online, see link below).
Conclusions
Dental practices that feature a professional monitoring and maintenance service, with or without licensed dental hygienists as operators, need science-based guidelines to assure ethical and effective treatment protocols. The BOP score (obtained as described in this and other publications) can be an effective tool to assess periodontal disease activity over time and can be an effective motivator for patients' daily personal plaque and biofilm control routines.
About the Authors
Joseph R. Greenberg, DMD, FAGD
Clinical Professor of Restorative Dentistry,
Kornberg/Temple School of Dentistry
Clinical Professor of Periodontics (retired),
University of Pennsylvania School of Dental Medicine
Private Practice
Villanova, Pennsylvania
Joy Jones, RDH
Villanova Dental Group
Villanova, Pennsylvania
Wendy Mercaldo, RDH
Villanova Dental Group
Villanova, Pennsylvania
References
1. Centers for Disease Control and Prevention. Third National Health and Nutrition Examination Survey (NHANES III), 1988-94. Centers for Disease Control and Prevention website. https://wwwn.cdc.gov/nchs/data/nhanes3/3a/VIFSE-acc.pdf. July 1999. Accessed December 28, 2018.
2. Shumaker ND, Metcalf BT, Toscano NT, Holtzclaw DJ. Periodontal and periimplant maintenance: a critical factor in long-term treatment success. Compend Contin Educ Dent. 2009;30(7):388-390, 392, 394 passim; quiz 407, 418.
3. Kaldahl WB, Kalkwarf KL, Patil KD, et al. Long-term evaluation of periodontal therapy: II. Incidence of sites breaking down. J Periodontol. 1996;67(2):103-108.
4. Aldredge WA. Bleeding on probing defined. Dimensions of Dental Hygiene. 2012;10(5):23-26.
5. Lang NP, Adler R, Joss A, Nyman S. Absence of bleeding on probing. An indicator of periodontal stability. J Clin Periodontol. 1990;17(10):714-721.
6. Eke PI, Dye BA, Wei L, et al; CDC Periodontal Disease Surveillance workgroup. Prevalence of periodontitis in adults in the United States: 2009 and 2010. J Dent Res. 2012;91(10):914-920.