Today’s Popular All-Ceramic Materials: Tips for Success
Understanding the limitations and strengths of the materials prescribed makes the selection process much easier
Dental assistants can play a crucial role in helping their dentists select the best restorative material for their patients. Managing a patient’s esthetic expectations, choosing the correct material for their occlusion, considering the preparation shade, and matching the overall look of the natural dentition can seem daunting at first glance but, with some basic tips for success, this process will be greatly simplified.
Understanding the limitations and strengths of the materials prescribed makes the selection process much easier. In this article the author will discuss the most popular all-ceramic materials requested by the dentists who send their cases to the author’s laboratory: IPS e.max® Press (Ivoclar Vivadent, https://www.ivoclarvivadent.us/) and full zirconia, and provide information and tips to dental assistants to help them get the best results for their patients.
Selecting an All-Ceramic Material
Years ago, before there were many strong and natural-looking all-ceramic materials on the market, the decision of which material to choose was much easier to make—a dentist chose either a porcelain-fused-to-metal (PFM) or a full-gold crown. Many times this selection process was based on tooth location, with PFMs selected for anterior restorations where the ceramic matches the natural dentition fairly well, and full-gold crowns selected in the posterior region where occlusal clearance is more limited, occlusal forces are stronger, and the gold alloy is soft and very gentle on the opposing dentition. Even with the more limited choices in restorative materials in the past, the patient’s esthetic expectation was always a factor. In this author’s experience, given the choice between a full-gold crown and a PFM crown, the majority of patients would choose the PFM crown because it blends more with the natural dentition and is less detectable.
Fast-forward to today, and there are now all-ceramic materials that rival or even top the strength of alloy-based restorations while providing amazingly natural esthetics. Does this mean that PFMs and full-gold crowns are going away for good? Are they inferior to these newer all-ceramic options? Not at all. Although the perception of dentists, staff, and patients alike tends to be that all-ceramic materials are the best choice to achieve an esthetically pleasing result, this is not always the case. There are factors that can and do negatively affect the final shade and appearance of all-ceramic materials. The key to success is understanding how to achieve the best results for your patients, and what information the dental laboratory needs from the clinical staff to provide those excellent results.
To understand shade matching and how all-ceramic materials are unique, it is important to think about the three principal characteristics that make up the color or shade of a patient’s teeth: hue, chroma, and value. Hue is generally described with words we associate with color: red, blue, yellow, etc. Chroma can be defined as the strength or dominance of the hue, or how intense the color appears. Value describes how light or dark a color is, and value is the factor that is most commonly associated with all-ceramic restorations not matching the natural dentition accurately. Have you ever seen an all-ceramic restoration that looks too bright in comparison to the natural dentition? When this happens, it is said that the restoration is too high in value compared to the natural dentition and not an accurate shade match. What about a restoration that appears too gray? This would be an example of a restoration that is lower in value than the natural dentition. An interesting observation this author has made is that a patient will accept a crown that is higher in value when compared with the natural dentition more often than they will accept one that is too low. The perception is that higher value (brighter/whiter) looks better and that lower value looks darker and worse. That being said, the goal should be a very accurate shade match, every time.
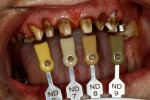
Why don’t all-ceramic restorations match perfectly every time? The value of an all-ceramic restoration can be affected by the color of the preparation underneath, more commonly referred to as the “stump shade” (Figure 1). With all-ceramic material, light passes through its surface and bounces off the underlying preparation and, depending on how translucent the material is, allows more or less of that underlying stump color to show through the restorative material, possibly affecting the value by either lowering it (too dark or grey) or raising it (too bright or light).
In comparison, with a PFM restoration the stump is completely covered by a metal coping that is opaqued (or painted) the exact color of the desired shade of the restoration. When light passes through the layered ceramic, it hits this painted coping instead of the stump and bounces off it; therefore, the stump cannot affect the final appearance of the restoration. There are instances in the author’s laboratory where PFM restorations are chosen over all-ceramic options in the anterior region if the patient’s stump color is very dark. As amazing and natural looking as today’s all-ceramic materials are, this author tells his dental clients that if a patient has a stump that is very dark (for example, one with an amalgam tattoo or a metal post), often the best solution is to cover it up completely with a metal coping.
All-Ceramic Option #1: IPS e.max Press
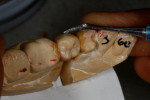
IPS e.max Press restorations are most commonly fabricated by producing a wax-up of the tooth being restored, either by hand or using computer-assisted design (CAD) software and a mill or 3-dimensional (3D) printer (Figure 2). The wax-up is invested in a ring (Figure 3), and the ring is placed in an oven where the wax is completely burnt out (Figure 4). Once the wax pattern has been eliminated from the ring, an empty mold remains. The ring is then placed into the pressing therm (Figure 5), the e.max ingot is placed into the ring (Figure 6), and the oven heats the ingot until it is liquefied. Next, a press motor inside the therm pushes the plunger down, and the liquefied lithium disilicate is pushed into the hollow mold. Once the ring and restoration inside it are cool, the restoration can be cut out of the ring, divested, and finished (Figure 7 and Figure 8). Finishing involves fitting the contacts and occlusion properly on the model if one is used, final shading with surface stains or porcelain, and glazing to seal the restoration and give it a glossy appearance.
Many assistants and dentists do not realize that e.max ingots are only available in the Classic Vita® (Vident, www.vident.com) shades (A through D) and not in the Vita 3D shades (1M2, 2M3, 3R1.5, etc.) so when any shade other than a Classic Vita shade is selected, the technician needs to convert to the proper ingot for the desired shade and then possibly use surface stains to achieve an exact match (Figure 9). Knowing this helps the clinical team to realize the constraints the technician is operating under when producing IPS e.max Press restorations, and could help to ease frustrations if Vita 3D shades do not come back every time as a perfect match.
Technicians can also select from four different translucency levels: high translucency (HT), low translucency (LT), medium opacity (MO), and high opacity (HO). The translucency level affects how clear or opaque the material is. When you provide the stump shade to your laboratory, the technician can choose the ingot that will provide the best result based on the color of the stump. Technicians can also fabricate a stump shade die from material that is the same color as the stump, allowing them to see how the restoration will appear when placed over the patient’s preparation. If the stump shade is darker or lighter than the selected shade of the restoration, the technician may choose a lower translucency ingot to mask the stump, and if the stump closely matches the desired final shade, the technician can use a higher translucency ingot for a less opaque and more natural-appearing restoration. You can use your regular shade guide to give your laboratory the stump shade. Remember, the more information you give your laboratory technician, the better result they can achieve for you.
All-Ceramic Option #2: Full-Zirconia Restorations
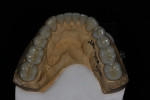
The other very popular material requested by clinicians sending restorative work to the author’s laboratory is zirconia. Zirconia is very versatile and can be used as an understructure (eg, a framework for a multiple-unit layered bridge or a coping for a single-unit layered restoration) or it can be milled to full contour (Figure 10). Zirconia is very strong, typically in the realm of 1,100 MPa to 1,400 MPa, so it is fast becoming the “go-to” all-ceramic restoration for posterior applications, especially for patients with bruxism because other ceramic materials may be susceptible to chipping or fracturing.
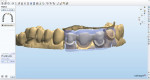
The process of fabricating a full-zirconia crown is very different than an IPS e.max Press restoration. Zirconia restorations are designed with CAD software (Figure 11) and milled in a prefinished state, then fired in a sintering furnace where the material shrinks slightly and achieves its final high strength (Figure 12). There are many different brands of zirconia on the market; some are available preshaded and some are pure white; the coloring/staining process varies depending on the particular zirconia. After sintering, the restorations are finished by fitting them to the models (if the case originates from a digital impression, it is possible to fabricate CAD/CAM restorations without a model) where the proximal contacts, occlusion, and margins are all verified. Surface stains are then applied to the restoration to achieve the final desired shade, and glaze is applied to seal the restoration and give it a shiny appearance. If a layered zirconia restoration is prescribed, veneering ceramic can be layered on and fired.
Because zirconia is very strong, it is well suited for multiple-unit, all-ceramic bridges. In this application the framework is fabricated and then porcelain is layered and fired over the framework, or a pressable ceramic is pressed over it. Earlier in the article the author discussed how stump color can affect the final shade of an all-ceramic restoration, and how masking the dark stump is sometimes necessary with a metal coping. Zirconia can be used for this same purpose and, although it is translucent, depending on the amount of preparation reduction it can be shaded and used effectively to completely mask or mute a dark stump and provide an all-ceramic restoration versus a metal-based one. This is beneficial when restoring multiple-unit anterior cases where most of the patient’s stumps are lighter in color but one is very dark, as all-ceramic restorations can be provided with the same veneering material for a very uniform result on all of the teeth being restored.
Is full zirconia damaging or overly abrasive to opposing natural dentition or restorations? While full zirconia restorations are very strong, the general consensus is they are not overly abrasive to opposing natural dentition or porcelain restorations as long as they are polished and smooth. If you adjust a full zirconia restoration at seating and leave the adjusted area unpolished, that area can be abrasive. Make sure to polish smooth any area you adjust that will contact the opposing tooth or crown.
Conclusion
The role of the dental assistant in helping dentists and patients navigate the all-ceramic options available on the market today is a crucial one. Your dental laboratory should be an indispensable resource in providing information on the all-ceramic options available to you, as well as describing their potential limitations, and assisting your decisions on complex cases. Once you acquire the basic knowledge, you can make well-informed choices and rest assured that your patients are getting the best possible result.
About the Author
Jamie Stover, CDT
General Manager
Ziemek Laboratories, DAMAS
Olympia, Washington