A Game-Changing Test for Tuberculosis Could Save Millions of Lives
Dental assistants can help reduce transmission with a dose of education
A fairly new rapid test could potentially revolutionize tuberculosis (TB) care and control by providing a quick diagnosis and may save several million lives every year. The combination of funding and rapid testing could make a significant impact on diagnosis, care, and prevention of disease transmission. Educating communities about TB is also critical for the success of any new project initiated to utilize technological advancements. To help with eradicating this disease, World TB day was established on March 24 to raise public awareness about TB, which is one of the deadliest public health threats in the world. This article discusses the healthcare challenges presented by TB and how this new test can help be a “game-changer” that could save millions of lives.
How Common Is TB?
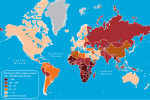
About one-third of the world’s population, or 2.3 million, has been infected with TB, and new infections occur at a rate of one per second. According to the World Health Organization (WHO), TB is the leading cause of death from a single infectious disease agent in adults worldwide. More than 95% of these cases occurs in developing countries. The areas of the world with the highest incidence of TB include southeast Asia (such as India, which had the highest incidence in 2007), Africa, eastern Europe, Latin America, and Russia (including children adopted from these areas). TB also tends to be prevalent among certain high-risk groups, such as immunocompromised individuals (ie, HIV, AIDS, pregnancy, cancer), homeless people, prisoners, people living in nursing homes, and immigrants. Approximately 400,000 immigrants and refugees legally immigrate to the U.S. each year, and an estimated 23,000 arrive with TB conditions.
In the U.S., the incidence of TB has declined slightly; however, four states—California, Florida, New York, and Texas—reported having more than 500 TB cases each for 2009. Combined, these four states accounted for 50.3% of all cases reported that year in the U.S. Statistics gathered regarding TB cases in the U.S show a higher rate of TB among racial/ethnic minorities. Foreign-born Hispanics and Asians together accounted for 48% of the total U.S. cases. A new interactive website by the Centers for Disease Control and Prevention (CDC) division called the National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention (NCHHSTP) was recently activated and provides interactive maps, graphs, tables, and figures showing geographic patterns and time trends for HIV, AIDS, viral hepatitis, sexually transmitted diseases, and TB.
Transmission
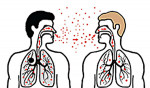
The mobility of travelers has been a major concern regarding contracting TB because of the ease of transmission, which is airborne. In fact, a single sneeze can release as much as 40,000 infectious droplets. TB has a very low infectious dose, meaning that the inhalation of fewer than 10 bacteria may result in an infection. With this mobility in mind, dental assistants must be mindful of where TB is prevalent when considering mission work and when treating patients from countries with a high incidence of TB. Healthcare workers need to review and establish office policies regarding identification of patients who may have infectious TB and protection of themselves and other patients.
The New Test for TB
A key point for the successful control of TB is the early diagnosis and immediate initiation of treatment. Many countries still rely solely on the sputum smear microscopy, which can take 3 months for results. Unfortunately, this smear microscopy test, which was developed more than 125 years ago, is slow and provides false-negative results for more than half of all TB cases. The test involves collecting sputum, dyeing it with a substance that colors only Mycobacterium tuberculosis (the bacteria that causes TB), and examining the sample under a microscope. The older sputum smear test could not be used to help diagnose TB if a patient was co-infected with HIV nor could it be employed to help diagnose drug-resistant TB. The new “while you wait” 2-hour test incorporates modern DNA technology that can be used outside of conventional laboratories and can be used to accurately diagnose TB, the TB/HIV co-infection, and drug-resistant TB. The older sputum smear test could not be used to help diagnose TB if a patient was co-infected with HIV nor could it be employed to help diagnose drug-resistant TB. This new test is also self-contained and does not require specialized training, which makes this test especially valuable in countries such as Kenya, where delays in laboratory diagnosis for TB lead to less patient follow-up and the continuing spread of the disease.
Affordability for the test has proven a major barrier to the introduction and widespread use in low- and middle-income countries where TB is endemic. Three subsidized funding sources for the test are guaranteed until 2022 by the U.S. government, the Bill & Melinda Gates Foundation, and the health-financing mechanism UNITAID. Forty-five developing countries and those with high TB burdens will benefit from the funding and collectively have the potential to save many of the 1.5 million to 2 million lives lost every year to TB.
A Global Health Emergency
WHO declared TB a “global health emergency” and began a “Stop TB” partnership that has aimed to save 14 million lives between 2011 and 2015. WHO is releasing recommendations and guidance for countries to incorporate the new test into health programs and includes testing protocols to optimize the use and benefits of this state-of-the-art technology in areas where it is needed most. Because 60% of all cases in the U.S. are from foreign-born persons, the CDC collaborates with other countries that have high TB rates and aims to improve TB control activities along the border between the U.S. and Mexico.
Treatment Challenges
The recommended treatment for TB uses several drugs, usually for 6 to 9 months. Effective TB treatment has been difficult to render in remote areas and underdeveloped countries due to lack of compliance among patients (especially when patients stop taking the medications because they feel better) or lack of understanding by patients about the importance of completing medication treatment. WHO has now recommended direct observed therapy, in which a healthcare provider watches the patient take the medications to ensure proper dosage compliance. This ensures effective treatment and keeps the patient from developing a resistant strain of TB. Drug-resistant TB, also referred to as multidrug-resistant tuberculosis, is a serious public threat and requires longer and more expensive treatment. Totally drug-resistant TB (resistant to all currently used TB drugs) was first described in 2003 and was widely reported in 2012.
Prevention in the Dental Office
Some basic measures that a dental office could establish are:
1) Modify the health history form to help identify possible TB symptoms. Questions may include: A) How long has your cough been present? B) Have you traveled internationally within the past 6 months? C) Where did you travel? If a patient responds positively to any of these questions, then asking about additional TB symptoms is in order. Symptoms include weight loss, night sweats, fatigue, bloody sputum, hoarseness, shortness of breath, and fever.
2) Establish a referral policy to a facility that can evaluate and treat a patient who you suspect might be infected
with TB. This will typically be a hospital equipped with an airborne-infection isolation room. Be aware of any media coverage of recent outbreaks, too. You can also call your local health department for confirmed current-year cases or go to an Internet site for your state (eg, Texas Department State Health Services), which can provide a history of cases by county. Please go to www.cdc.gov/tb/links/tboffices.htm.
3) Isolation of a suspected patient with possible symptoms of active TB is imperative to reduce the risk for transmission. Because dental offices are not equipped with isolation rooms that have reverse airflow/negatively pressured ventilation relative to the corridors and air either exhausted to the outside or HEPA-filtered if recirculation ventilation is employed, then getting that patient out of the office as quickly as possible is critical. In addition, the healthcare worker and patient should wear a mask during the medical history review. The standard dental masks are not respirators and do not offer the level of protection needed to protect dental team members from TB. The N95 particulate respirator offers the minimal amount of filtration efficiency required. So purchasing N95 particulate respirators might be a dental team’s wisest investment for initial prevention of TB.
4) Postpone any nonemergency dental care for a patient who may have TB. A dentist is not obligated to treat new patients who may have active TB infections. Only after the patient has been cleared by a medical doctor and is confirmed to no longer be infectious should any elective dental treatment be considered.
5) Employers should consider TB testing upon initial hiring of an employee and after a possible exposure to TB has occurred either at the office or in public. The CDC recommends that dental offices perform an annual risk assessment. This includes determining the office’s classification risk (low, medium, high), which might be according to location or recent community outbreaks.
6) Provision of an annual training program is the best prevention for any dental office to ensure dental healthcare workers understand how TB disease transmission occurs, how to recognize potential hazards, and how to handle a situation appropriately.
Conclusion
There is no doubt that the combination of global funding, development of a rapid TB test, and public awareness can result in a “game changing” outlook for treating and eradicating TB in the U.S. and save countless lives worldwide. This author will join in the fight against TB by supporting the “Stop TB Partnership” by building public awareness all year long, but especially on March 24, the anniversary of when Dr. Robert Koch astounded the scientific community in 1882 by announcing that he had discovered the cause of TB.
Acknowledgment
The author would like to thank Garry Woo, MD, Medical Director, Dallas County Health and Human Services TB Control.
About the Author
Ronda V. Lane, BS, CDA, RDA, FADAA
Irving, Texas