Fixed Prosthodontic Procedures Step By Step
Following a proven process ensures predictable success.
Keeping track of the multiple tasks needed to complete a procedure can create frenzy. “Chunking out” each step of a complex, multistep procedure can alleviate some of the stress. Crown or bridge procedures usually require multiple steps over three office visits. For the pretreatment visit, the dental assistant needs to prepare for and make a preliminary impression. For the preparation visit, the dental assistant needs to prepare for the application of topical and local anesthesia, shade selection, crown preparation, tissue management, mixing of final impression and bite registration materials, fabrication of provisional restorations, temporary cementation of provisional restorations, and removal of excess cement. For the final cementation visit, the dental assistant needs to set up for the removal of the provisional(s), removal of remaining temporary cement, isolation of the preparation, and cementation of the final restoration.
Dental assistants, who are credentialed, depending on their state, can perform most of these procedures except for the administration of local anesthesia and the preparation of the teeth. It looks like a laundry list of duties but, as this article demonstrates, by examining each step individually the assistant can accomplish the patient’s treatment with ease.
Pretreatment Visit Steps
Preliminary Alginate Impression
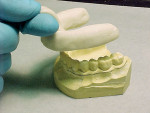
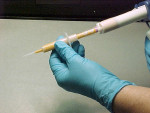
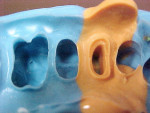
After a patient has been examined and treatment planned for a crown or bridge procedure, a preliminary alginate impression for study models can be made. Subsequently, working casts can be created from the preliminary impression, which will be used to fabricate custom trays (Figure 1 and Figure 2). The philosophy behind making the final impression with custom trays is to provide a well-fitting impression tray that is comfortable for the patient, contains an adequate amount of impression material to obtain an impression that reproduces fine details, minimizes waste of expensive impression materials, and assures proper intraoral seating of the impression tray during the impression process.1
Anesthetic Application
Applying topical anesthetic to the injection sites after drying the mucosa will provide patient comfort during the injections. For patients, the administration of the local anesthetic injection is probably the most nerve-racking part of the dental visit, no matter what procedure will be performed.
Shade Selection
Shade selection can be done while the dental team is waiting for the local anesthetic to take effect. Using a shade guide under natural lighting conditions, the dentist, dental assistant, and the patient should determine which shade matches the adjacent teeth best.2
Preparation and Evacuation
After the teeth to be prepared have been anesthetized, the dentist will use burs in a high-speed handpiece to reduce and shape the teeth. Simultaneously, the dental assistant will use the high-velocity evacuation system and the air/water syringe to keep the oral cavity clear of debris and maintain a clear path of vision for the dentist. When tooth preparation is complete, the dental assistant will examine the patient’s oral cavity to verify that it is clear of debris.
Tissue Management
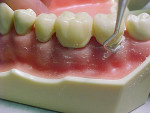
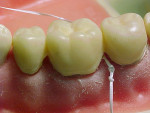
There are various methods available for tissue management (Figure 3), the most common being the use of retraction cord. Retraction cords may be twisted or braided and are available in different sizes to accommodate various depths of sulcus. Using a Balshi packer or another of gingival cord-packing instruments available, gently push the end of the gingival retraction cord under the gingival margin. Continue advancing around the prepared tooth, packing the gingival retraction until arriving at the beginning end of the cord. Leave a piece of the cord sticking above the gingival margin for removal immediately proceeding placement of the wash or light- final impression material (Figure 4 and Figure 5). Some retraction cords are treated with a chemical agent to enhance the contraction of the tissue it contacts. Aluminum chloride, potassium aluminum sulfate, ferric sulfate, or zinc chloride cause the collagen fibers in the tissues around the capillaries to swell. The expansion of the collagen around the capillaries induces pressure on them, which causes them to constrict.3,4 This contraction of the tissues allows the impression material to enter the sulcus to capture the margins of the tooth preparation. Astringedent®, Astringedent® X, ViscoStat®, ViscoStat®Wintermint, ViscoStat® Clear (Ultradent Products, Inc, www.ultradent.com), Gingi-BRAID+ (DUX Dental, www.duxdental.com), and Hemodent™ Cord, (Premier Dental Products Co, www.premusa.com) are examples of tissue management products. Make sure you are familiar with the patient’s medical history before selecting a gingival retraction method. Astringedent X should be used on patients who are on the anticoagulant warfarin or aspirin therapy, or who are hemophiliacs to control bleeding.3 Also, gingival retraction cord should not be left in the sulcus for an extended period of time as this may cause gingival recession, especially if a periodontal condition is present.
Generally, chemically treated retraction cord can be left in place for 5 to 7 minutes and untreated cord for 10 to 15 minutes. Gingival retraction products containing epinephrine should be avoided in patients who have hypertension, heart disease, diabetes, or hyperthyroidism.2 In addition to the use of cords for gingival retraction, retraction caps (Roeko Comprecap, Coltène Whaledent Inc, www.coltenewhaldent.com; GingiCap™, Centrix, www.centrixdental.com), retraction gel (GelCord® Tissue Management Gel, Pascal International, Inc, www.pascaldental.com), and gingival retraction paste (Expasyl™, Kerr Corporation, www.kerrdental.com; Traxodent® Hemodent®, Premier Dental Corporation, www.premusa.com) can be used. Roeko Comprecaps should be used in conjunction with an expanding polyvinyl siloxane material to press the gingival tissues away from the margins of the preparation.5 If the gingival tissues are too bulky and esthetics will not be compromised, the dentist can create a trough around the preparation using electrosurgery to open the sulcus.4
Final Impression
After the tissues have been managed, the final impression materials can be prepared. The selection of the impression material depends on the dentist’s preference. A single-viscosity, monophase impression material is favored by many dental professionals because there is only one material to mix and it can reproduce fine details. A combination of medium-, heavy-, or putty along with a wash-type impression material can be used with a two-step technique (Figure 6 and Figure 7). When selecting an impression technique and materials, consider how many hands will be available for mixing the materials and loading them into a syringe and/or impression tray. An option is to use materials that are prepared using an automixer.6
After the master impression is removed from the patient’s mouth, the impression should be disinfected and then examined by the dentist to ensure all necessary details were captured (Figure 8).7 A clear reproduction of the margins is needed because the dental laboratory technician must be able to read the margins on the dies produced from the impression to fabricate a well-fitting permanent prosthesis (if the necessary anatomic features were not reproduced, the impression would have to be repeated; this also may include reapplication of the gingival retraction method).
Immediately after the impression is completed, a bite registration should be recorded with a high-viscosity elastomeric impression material. The bite registration also needs to be disinfected before packaging to be sent to the laboratory.6
Provisional Restoration Creation/Delivery
After the final impression has been completed, provisional coverage is provided.8 Options available for provisional coverage are: custom-made, preformed polymer, preformed polycarbonate, and aluminum. Stainless steel crowns also can be used as a form of provisional coverage in adults.9 Another possible option requires sending the working cast to the dental laboratory a week before the preparation visit. Provisional restorations can be fabricated by the dental laboratory technician from the pretreatment cast. These provisionals are reinforced with orthodontic wire or Kevlar fiber. Using laboratory-fabricated provisionals can save chair time, but adds an expense. This option is especially useful if the provisional restorations are expected to be worn for an extended time.10
Provisional Restoration Cementation
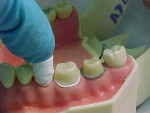
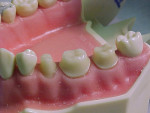
Regardless of the type of provisional used, it will be cemented onto the prepared teeth using a temporary luting agent. A well-fitting provisional needs a minimal amount of temporary cement (Figure 9). An excessive amount of cement inside a crown or bridge may prevent proper seating onto the prepared tooth/teeth. After the cement has set, the gingival margins should be examined and any excess cement removed (Figure 10). A piece of knotted dental floss should be carefully passed interproximally to remove residual cement (Figure 11).9 If the provisional is a bridge, floss should be passed under the pontic areas as well.1
Patient Instruction
After the provisional is in place, the patient should be instructed about the importance of plaque control and any modifications to his or her oral hygiene routine. Diet modifications while the provisional restoration is in place should be discussed. Equally important is informing the patient to notify the dental office immediately should the provisional restoration come off the preparation before the next scheduled appointment.8
Final Cementation Visit Steps
Removal of Provisional Restoration
The next visit is scheduled to permanently cement the prosthesis onto the prepared tooth/teeth. When the patient arrives, the dental assistant will remove the provisional restoration (Figure 12). The prepared tooth/teeth should be examined and any remaining temporary cement removed. The preparation is carefully rinsed and dried.
Restoration Cementation
The permanent restoration is tried in. If the dentist and patient are satisfied with the fit and appearance of the prosthesis, it can be cemented with the permanent cement designated by the dentist. After isolating the preparation, the dental assistant will need to mix the permanent cement according to the manufacturer’s directions and then coat the inner surface of the abutment teeth of the prosthesis with enough cement to ensure adequate adhesion of the prosthesis to the patient’s teeth. Again, excessive amounts of cement may prevent proper seating. The prosthesis is seated onto the preparation by the dentist and the patient is instructed to bite continuously until the cement has hardened. After the cement is set, the dental assistant should examine the area and remove any excess cement as was done with the provisional restorations.
Conclusion
Treatment sessions for fixed prosthodontic procedures are busy. An organized dental assistant will keep track of the multiple tasks involved in the multistep procedure and store instruments and materials so they are easily accessible and ready for use. By chunking out the multiple, coordinated procedures, the dental assistant can keep chair time to a minimum and help reduce stress for the patient and the dental team.
References
1. Bird DL, Robinson DS. Torres and Ehrlich Modern Dental Assistingth ed. St. Louis, Mo: WB Saunders; 2005.
2. Phinney DJ, Halsted JH. Delmar’s Dental Assisting: A Comprehensive Approach. 2nd ed. Clifton Park, NY: Delmar Learning; 2003.
3. Tissue management procedure for making impressions. Ultradent Web site. Available at: https://www.ultradent.com/products/instructions/viscostat.pdf. Accessed Nov 5, 2007.
4. Dental Product Spotlight, Gingival Retraction. J Am Dent Assoc [serial online]. 2002;133(5):653. 2002. Available at: https://jada.ada.org. Accessed Nov 11, 2007.
5. Magic FoamCord. Coltène Whaledent Web site. Available at: https://www.magicfoamcord.com/pdf/MFC_UK.pdf. Accessed Nov 5, 2007.
6. Craig R, Powers JM, Wataha JC. Dental Materials: Properties and Manipulation. 9th ed. St. Louis, Mo: Mosby; 2007.
7. Kugel G, Perry RD, Ferrari M, et al. Disinfection and communication practices: a survey of US dental laboratories. J Am Dent Assoc [serial online]. 2000;131(6):786-792. Available at: https://jada.ada.org. Accessed Nov 12, 2007.
8. Edwards DE. Temporary crowns: materials and techniques. Contemporary Dental Assisting. 2007;4(6):34-39.
9. Hatrick CD, Eakle WS, Bird WF. Dental Materials: Clinical Applications for Dental Assistants and Dental Hygienists. St. Louis, Mo: WB Saunders; 2003.
10. Bird DL, Robinson DS. Torres and Ehrlich Modern Dental Assisting. 8th ed. St. Louis, Mo: WB Saunders; 2005:840.
About the Author
Karen Kulikowski, DMD, Professor, Department of Allied Dental Education, School of Health Related Professions, University of Medicine and Dentistry New Jersey, Scotch Plains, New Jersey.