Outcome-Based Preparation Design for Anterior Veneers Using Specific Depth-Cutting Burs
Sound preparation design guidelines help clinicians achieve a highly predictable result.
The predictability of the esthetic outcome in restorative dentistry is dictated by the degree of change expected by the patient or clinician. The preferred or required change may be in tooth morphology, color, or value. The greater the change needed, the more extensive the required tooth reduction. The primary goal of any procedure that requires tooth reduction is to preserve natural tooth structure while achieving the desired esthetic outcome. The amount of tooth preparation needed to accomplish the established goals is based on the degree and location of the underlying tooth discoloration, the expectation of the outcome, and the space requirements of the restorative material. The amount of relative translucency and/or opacity determines the esthetic success or failure, so if the clinician’s goal is to mimic natural tooth structure and translucency, there are specific guidelines that should be followed. The labial depth-cutting burs described in this article were designed based on average labial enamel thickness to provide the proper space needed for the ceramic material chosen.
Tooth Morphology Considerations
Whether it is a crown or veneer, 0.5 mm of space for enamel ceramic is required over the dentin or opacified layer of ceramic to mimic the depth and translucency of a natural tooth. If the underlying tooth structure is of normal color and value, a conservative preparation can be considered. If it is discolored or of low value, enough space must be created for the ceramist to correct the problem and eliminate or minimize the influence of the tooth color and the “show through” of the transition line of the preparation. Keep in mind that ceramic veneers have the highest long-term success rate when the restoration is bonded to enamel rather than dentin.1 Relying on the color or opacity of the bonding resin cement to create the desired changes is highly variable and unpredictable, and should be undertaken only if needed to enhance the outcome.
If significant tooth morphology changes are desired, a mock-up based on a diagnostic wax-up is recommended. This preparatory stage helps to determine if a procedure such as the additive restorative technique can help minimize the actual amount of tooth that requires reduction. For example, the additive veneer technique can be used for changing tooth morphology through the use of a mock-up that is placed on the teeth at the time of preparation so that only the necessary amount of natural tooth structure is removed to accomplish the final preferred tooth shape and position. The overall depth of reduction will still be appropriate for the desired value or color changes, because the actual thickness of the restoration allows for the necessary masking while providing additional space to develop the appropriate translucency.
Preparation Design Considerations
There are several important points to consider when designing preparations. First, to have adequate space for the restorative material and conservation of natural tooth structure, the final esthetic outcome should be considered. Clinicians may need to consult with their technicians to discuss the appropriate material and amount of space needed to meet the identified outcome.
The clinician may want to begin tooth reduction after a direct mock-up on the teeth to preserve as much tooth structure as possible.2 It is important to remember that the greater the color or value change, the more the tooth needs to be reduced.
The next consideration is that all corners and edges must be rounded to:
• ensure precisely fitting restorations and less stress on the ceramic; sharper angles provide increased challenges for the laboratory.
• allow a smooth flow of cement for complete seating of the restoration.
• allow for complete milling or fabrication of the restoration, whether in the office or the laboratory.
Lastly, smooth and sharp preparation finish lines allow for more precisely fitting restorations at the margins, as well as more predictable clinical procedures at the time of restoration insertion.
Preparation Design Concepts
Incisal Reduction
The concept of length reduction is based on knowing the definitive incisal edge position of the final restoration. The goal is to create 2 mm to 2.5 mm of space for the restorative material. A reduction of 2 mm is adequate when there are minimal esthetic changes and minimal incisal translucency is desired. The bur that would be used for this type of procedure is RW 2.0. A reduction of 2.5 mm is recommended when there will be a framework (metal, zirconia, etc.) in the crown restoration; greater translucency is desired; or a conventional or extensive veneer is required because significant color or value changes are expected. For this procedure, the RW 2.5 bur would be used.
The protocol for using these burs is to make either 2-mm or 2.5-mm depth cuts from the definitive length of the final restoration. The entire incisal edge is then reduced to this level (Figure 1 through Figure 5).
Labial Reduction
The three recommended reductions for the labial surface of anterior teeth are classified as minimal, conventional, and extensive, depending on the esthetic changes stipulated by the desired outcome. The minimal reduction is for zero to one shade change, the conventional reduction is for one to two shade changes, and the extensive reduction is for two to three shade changes.
The labial depth-cutting bur designed for minimal reduction measures 0.3 mm in the gingival third, 0.5 mm in the middle third, and 0.7 mm in the incisal third of the preparation. This minimal tooth reduction is essentially all within the enamel tooth layer. For this procedure, the RW Min bur is used. The depth-cutting bur for conventional reduction measures 0.5 mm in the gingival third, 0.7 mm in the middle third, and 0.9 mm in the incisal third. The resulting reduction is mostly in enamel, except for possibly the gingival third of the preparation. For this procedure, bur RW Conv is used. When significant color or value changes are needed, or a combination of veneers and crowns will be placed or already exist, a greater reduction is required to achieve a predictable outcome. The depth-cutting bur for extensive reduction measures 0.8 mm in the gingival third, 1 mm in the middle third, and 1.2 mm in the incisal third. This results in the removal of labial enamel unless there is an additive technique planned that will change the labial position of the final restoration. The bur to be used for this procedure is the RW Ext. The suggested procedure for labial reduction is shown in the accompanying photographs and follows the following protocol:
1.Select the appropriate labial depth-cutting bur to accomplish the goals of the case.
2.The bur needs to be used in two planes to follow the curvature of the labial aspect of a natural tooth.
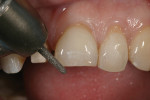
3.The first plane uses the 0.7 mm and 0.9 mm bands of diamonds, sinking these bands into the tooth until the shank of the bur above, in the middle, and below these bands touches the tooth. The shank typically leaves a grey line on the surface of the tooth (Figure 6).
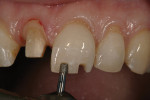
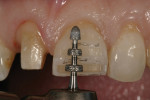
4.The second plane uses the gingival depth-cutting diamond tip of the bur. The bur is placed into the depth of the radius of the round tip. The shank above this band of diamonds will limit the depth in this area. It is possible to over- or under-angle this aspect of the preparation. The goal is to sink the round end of the diamond tip 50% into the tooth (Figure 7).
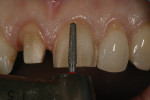
5. Once the depth cuts have been established, reduce the labial aspect with a medium-grit tapered diamond bur (856-016 or 856-018, Brasseler USA)(Figure 8).
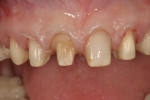
6. The final step in tooth preparation is finish-line refinement so that a smooth and well-defined margin is created with a fine-grit tapered diamond bur (8856-016, Brasseler USA) (Figure 9).
7. Additional preparation design changes needed interproximally are outcome-dependent (Figure 10).
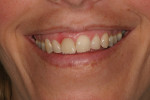
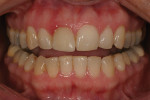
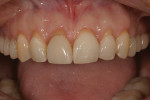
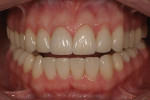
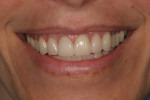
The long-term success of this method can be observed in the 5-year post-treatment photographs (Figure 11 and Figure 12).
Conclusion
By following the presented preparation design guidelines using the Brasseler depth-cutting burs, practitioners can produce a highly predictable result. While dentists strive to do only minimally invasive procedures, in some cases a more significant amount of tooth reduction is in the best long-term interest of the patient if the goal is to create a natural-looking restoration.
Disclosure
The author is the developer of the five depth-cutting burs described in this article, and has received financial compensation for this article.
Acknowledgment
The author wishes to thank the periodontist in this case, Dr. Edward P. Allen of Dallas, Texas; and the Spear Winter Laboratory for fabrication of the final restorations.
References
1. Gurel G, Morimoto S, Calamita MA, et al. Clinical performance of porcelain laminate veneers: Outcomes of the aesthetic pre-evaluative temporary (APT) technique. Int J Periodontics Restorative Dent. 2012;32(6):625-635.
2. Magne P, Magne M. Use of additive waxup and direct intraoral mock-up for enamel preservation with porcelain laminate veneers. Eur J Esthet Dent. 2006;1(1):10-19.
About the Author
Robert R. Winter, DDS
Private Practice Limited to Prosthodontics
Newport Beach, California
Faculty
Spear Education
Scottsdale, Arizona
Founder
Spear Winter Laboratory
Laguna Beach, California
Bur Descriptions
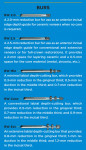
The system described in this article is composed of five burs created for Brasseler USA. The two incisal depth-cutting burs are designed to create adequate space for the ceramist to develop natural internal characteristics and translucency in the incisal edge of the veneer restoration. This reduction is determined based on the definitive length of the final restoration. In addition, a series of three depth-cutting burs was developed so that the labial reduction is tapered and corresponds to the average enamel thickness of anterior teeth. These are used in two planes to follow the labial morphology. The average enamel thickness of anterior teeth is: Please put something in here referencing figure 13
0.3 mm to 0.4 mm in the gingival third.
0.8 mm to 1.0 mm in the middle third.
1.1 mm to 1.2 mm in the incisal third.