Laboratory Communication for Full-Arch, Implant-Supported Prostheses
Occlusal and esthetic considerations to optimize predictability, efficiency, and accuracy
Joe “Ambrose” D’Ambrosia
Restoring a dentate or edentulous ridge with a full-arch, implant-supported prosthesis is a complex treatment modality that presents many challenges for implant surgeons, restorative dentists, and the laboratory. Full-arch restorations can return much needed functionality to patients who may be suffering from multiple dental problems, but these restorations can positively impact the lives of patients in many other ways as well. When excellent esthetics are achieved, a patient's self-image, self-confidence, and overall happiness can be improved, but an analysis of the whole patient is necessary for ultimate success.
In order to work with clinicians on advanced implant-supported appliances, modern dental technicians must have a foundational knowledge of clinical prosthetic implant dentistry and implant surgery. Regarding record-taking and communication, the dental laboratory is responsible for ensuring that the materials received from the clinician are adequate and complete enough to provide successful, high-quality restorations. If laboratory technicians are not provided with the necessary tools to successfully restore a case, it is their job to request the information from the clinician.
It is critical that the esthetics, vertical dimension of occlusion (VDO), available restorative space, and centric relation are determined before planning any full-arch prosthetic restoration case. To optimize the efforts of laboratory technicians in fabricating everything from the surgical guides to the final implant-supported prostheses, this article outlines what information they need from clinicians, including required photographs, and discusses occlusal considerations, methods to confirm the VDO, and esthetic considerations.
Required Photographs
In order to design and deliver the most functionally and esthetically ideal prosthesis for each patient, the laboratory needs a series of photographs that include, at a minimum, full-face repose, natural smile, and exaggerated smile views, as well as profile closed mouth and smile views and views of the bite that show the anterior and posterior relationships.
Full-Face Views
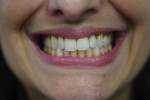
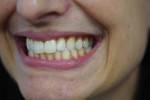
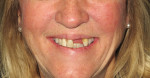
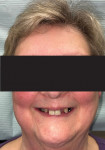
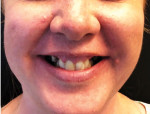
The repose view shows the amount of tooth display that the patient exhibits at rest (Figure 1). The natural smile view, which is of the patient's normal, everyday pleasant smile, is used to make decisions regarding the midline, tooth display, horizontal plane, and the relationship of the incisal edges to the lower lip and pupils of the eyes (Figure 2). To aid in deciding whether an FP1, FP2, or FP3 restoration will be the most appropriate, the exaggerated smile view is a critical photograph because it shows the patient's high lip line and any excessive gum display that might affect a full-arch restoration (Figure 3). Deciding between an FP2 and FP3 prosthesis largely depends on whether or not the transition line between the restoration and gums will be hidden. The decision to deliver an FP1 prosthesis should be informed by whether or not the patient will consider it an acceptable result if resorption occurs and black triangles appear in the interproximal areas. When delivering an FP1 appliance, clinicians should be prepared to perform or refer patients for soft-tissue grafting in the event that resorption occurs.
Profile Views
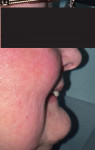
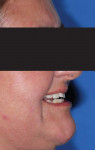
The profile photographs, which include a closed-mouth view with the teeth together and lips touching (Figure 4) as well as a smile view (Figure 5), are used to analyze lip support, anterior-posterior tooth position, and facial incline of the anterior teeth. These views can also be used in an analysis of the VDO.
Bite Views
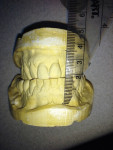
To help determine a starting point for establishing the VDO, bite photographs are compared with a bite model or bite scan. These views should show the anterior relationship, the right posterior relationship, and the left posterior relationship-all with the teeth in maximum intercuspation (Figure 6 through Figure 8).
Occlusal Considerations
When designing the prosthesis and planning the implant positions for a full-arch restoration, there are certain occlusal "red flags" that need to be considered in the decision-making process and included in the laboratory communication. These include a lack of restorative space, a lack of positive centric stops, a deep Class II bite or prognathic bite, and the presence of excessive gingival display, among other considerations. Many of these patients present with deep, collapsed Class II bites for which the VDO must be restored to its original, healthy functional position.
Regarding the restorative space available, when measuring from the top of the implant to the exit position of the screw access hole on the tongue side of the appliance, the minimum restorative space required is 10 mm for FP1 appliances, 10 mm to 12 mm for FP2 appliances, and 13 mm for FP3 appliances. Patients who present with a lack of positive centric stops should be analyzed carefully. In these cases, teeth try-ins or orthotics are options that can be used to confirm the VDO and centric relation. Patients who present with deep Class II bites or prognathic Class III bites, with or without centric stops, should be analyzed to see if the VDO needs to be restored to its most healthy position.
Confirming the VDO
There are several methods that can be used to confirm that the patient's VDO is appropriate or requires further analysis and possibly adjustment. Establishing a proper VDO is essential to delivering a full-arch, implant-supported prosthesis.
Shimbashi Measurement
The Shimbashi measurement, which was developed by Henry Shimbashi, DDS, can provide a very accurate starting point. To obtain the Shimbashi measurement, measure from the cementoenamel junction of an upper central to the cementoenamel junction of the same-side lower central with the teeth in maximal intercuspation (Figure 9). On average, this measurement of the height of the bite should be between 17 mm and 22 mm for the majority of patients. When this measurement is less than 17 mm, the path of closure of the teeth causes unnecessary muscle activity and puts the teeth, jaw, and muscles in conflict, which can create jaw pain, and opening the bite and testing with an orthotic is suggested.
Buccal Fold Measurement
Measuring from the upper buccal fold above a lateral incisor to the lower buccal fold below the same-side lower lateral incisor is another way to confirm a patient's VDO (Figure 10). Typically, the normal range of this measurement is from 35 mm to 38 mm, and it confirms or agrees with the Shimbashi measurement.
Facial Rule of Thirds
A VDO Gauge can be used to establish a patient's VDO using the facial rule of thirds. First, the gauge is used to measure from the middle of the eye to the commissure of the lips, and the set screw is tightened. Next, hold the nasal spine indicator against the nasal spine and check to see if the chin indicator fits properly under the chin. If it does, the VDO is good. If the chin indicator is too high to fit under the chin, then the patient is too open. If the chin indicator is too low to touch the chin, then the patient is overclosed. When the patient is overclosed, use a leaf gauge to open the patient's mouth until his or her chin is firmly against the chin indicator. With the bite stabilized in this position, inject impression material into the space between the teeth to capture the new VDO position and bite registration in centric relation. Sending a centric bite to the laboratory along with the Shimbashi measurement also works as registration. The bite will be mounted on an articulator in centric relation and opened to the Shimbashi measurement to establish VDO.
Orthotic Therapy
An orthotic appliance can be made to test the new VDO. It is worn for a period of time determined by the dentist to confirm that the new jaw position can be tolerated and maintained.
Esthetic Considerations
Regarding esthetic analysis, when planning a full-arch, implant-supported prosthesis, there are several points of importance that must be considered and communicated to the laboratory. These include the midline position and angle, the horizontal plane and relationship of the upper incisal edges to the lower lip, the amount of maxillary and mandibular tooth display, facial features related to the VDO, and the presence of flared teeth or excessive gingival display.
When the patient's midline is not in the center of his or her face, it needs to be corrected. If the lower lip is asymmetric, the horizontal plane needs to be referenced with the pupils of the eyes and how it looks on the face (Figure 11) . In situations in which the patient has excessively long teeth in the maxilla or mandible, the upper or lower teeth can be shortened with the prosthesis as long as enough restorative space exists and the VDO can be adjusted (Figure 12).
In addition to deep Class II overbites, Class III underbites, and Shimbashi measurements less than 17 mm, there are certain facial features that can indicate the presence of a collapsed VDO. These include a C-shaped (Figure 13) or inverted smile profile and smiles in which the upper centrals and cuspids lay on the lower lip (Figure 14). Correcting flared teeth is possible, but it may require the VDO to be opened to reduce the flare, especially for single-arch cases (Figure 15).
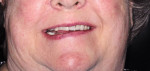
For patients who demonstrate excessive gingival display or "gummy smiles," treatment planning can be challenging if they want less gingiva to show when they smile after restoration (Figure 16 and Figure 17). In these cases, an analysis of the VDO, available restorative space, implant length vs restorative space, and available bone is critical in determining whether an FP1, FP2, or FP3 appliance is most appropriate as well as the need for bone reduction or grafting procedures. There are many factors to consider, including the possibility of resorption in FP1 cases and transition line exposure in FP2 and FP3 cases. Resorption is always a possibility on implant cases, and if resorption occurs in these cases, abutment exposure and open gingival embrasures can occur, causing an esthetic failure. The potential need for soft-tissue grafting to hide black triangles and abutment collars must be anticipated.
Guided Surgery
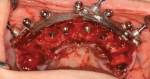
Using a guided surgery technique that leverages a system with a "floating guide concept" (CHROME GuidedSMILE, ROE Dental Laboratory) can improve the delivery of implant-supported, full-arch prostheses. By fitting over the existing teeth or ridge, the pin guide allows the fixation base to be pinned to the bone without touching it. The fixation base has multiple purposes (Figure 18). In addition to serving as the bone reduction guide, it is also the base that is used to attach the other guides, including the osteotomy guide and carrier guide, as well as the rapid pick-up appliance and the final provisional appliance. The system is designed and fabricated using software for the most accurate results.
Conclusion
Full-arch, implant-supported restorations can provide life-changing results for edentulous or partially edentulous patients. The considerations outlined in this article must be analyzed and decided upon before planning implants in software for surgical guide construction. When the establishment of a proper VDO in centric relation and the analysis of any important occlusal and esthetic considerations are emphasized during treatment planning and properly communicated to the laboratory, the need for an FP1, FP2, or FP3 prosthesis can be appropriately determined, and the process of fabrication can be optimized to improve predictability, efficiency, and accuracy.