Strategic Treatment for the Atrophic Ridge
Narrow diameter implants offer a new solution to limited bone volume in the horizontal dimension
Todd B. Engel, DDS
Historically, patients who were facing the daunting reality of losing most or all of their teeth had few options for dental rehabilitation, and many avoided seeking treatment. In more recent years, much of this perception has changed due to the tremendous amount of clinical advancement within the field of implant dentistry as well as the ever-growing public awareness of the availability of "same-day tooth replacement therapy."
One of the major reasons for the avoidance of implant therapy was (and still is) the "staged" portion of this lengthy treatment in which patients must wear a traditional denture. However, with the awareness of the availability of immediate implant procedures, many of those very same patients who were otherwise holding off on treatment are now considering committing to care. A procedure that previously could have spanned an 8- to 10-month timeframe can now be completed in less than 4 months total with just one surgical procedure instead of multiple ones. In most cases, this eliminates the dreaded interim phase when patients need to wear a removable appliance as they heal.
Now that dental practices are seeing more of these hopeful candidates than ever before, in most cases, the limiting factor is no longer the patients themselves or even their finances but rather nuances of their clinical presentations that compromise their hopes of receiving this modernized therapy. For example, the quantity and/or quality of bone that patients present with is often insufficient for implant placement and requires preemptive grafting procedures. With the increasing demand for same-day immediate implant therapy among these patients, the profession has seen a tremendous rise in the use of smaller or "mini" dental implant fixtures as an alternative strategy to ridge augmentation procedures.1
Case Report
A 65-year-old female patient with a complete maxillary denture, 8 remaining mandibular teeth that demonstrated grade 2 or greater mobility, and an ill-fitting, nonfunctional mandibular partial denture presented to the dental practice seeking a more permanent and definitive solution.2 Her desire was to begin by attending to her mandibular arch and then ultimately proceed to her maxilla in due time based on her budget. After the initial consultation, which included a thorough health history review, intra- and extraoral examinations, cone-beam computed tomography (CBCT) imaging, and a discussion to help the clinician understand the patient's desires, treatment options were provided. The treatment plan selected by the patient was a single-visit surgical solution that included the placement of narrow diameter, one-piece tissue-level implants to retain a full lower removable denture with an immediate load option. This would avoid the multiple preemptive bone and soft-tissue grafts that would be needed to accommodate the future placement of standard size implants.
Diagnostic Phase
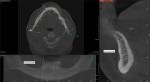
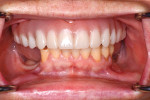
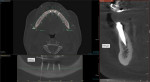
A large field of view CBCT scan was acquired to assess the surgical and prosthetic needs of the candidate (Figure 1). In addition, the patient's phonetics, esthetics, function, vertical dimension of occlusion, smile, and transition lines, among other clinical characteristics, were evaluated and documented (Figure 2). Upon completion of the examination, it was determined that rehabilitation with a full-arch fixed removable denture with narrow platform implants was a viable and acceptable option.3
Surgical Phase
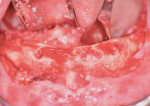
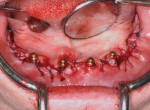
At the surgical appointment, profound anesthesia was achieved using a peripheral block with supplemental infiltration using a combination of articaine HCL 4% with epinephrine (Septocaine®, Septodont) and lidocaine 2% with epinephrine. Next, the elevation of bilateral full-thickness flaps with posterior release was initiated. This permitted full access to the bony architecture and facilitated the removal of the teeth. After extraction of the natural teeth, a small alveoloplasty was performed to ensure uniform bone height and even platform positioning of all of the implants (Figure 3).
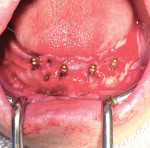
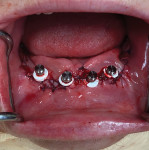
Following the alveoloplasty, four 2.4 mm × 10 mm tissue level implants (RidgeFit System, Straumann) were surgically placed in strategic positions, taking into consideration all of the anatomical landmarks and prosthetic load demands, and torqued to 35 Ncm (Figure 4). These "self-tapping," dual-thread implants were selected because they require a minimum ridge width of only 4.4 mm, a minimum height of 10.0 mm, and a soft-tissue depth of 2.0 mm, while also being conducive for type I, II, or III bone. In addition, the system's prosthetic connection allows for an angulation divergence of up to 40 degrees between implants to facilitate the most challenging cases.
Immediately following placement of the final implant, complete soft tissue closure was accomplished with continuous interlocking and interrupted sutures (Figure 5). The focus was placed on ensuring adequate connective tissue attachment circumferentially to prolong the life of each implant fixture.
Prosthetic Phase
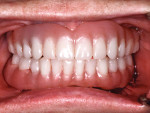
Because an initial stability of at least 35 Ncm of torque was achieved for each implant, immediate loading could be accomplished at the time of surgery. The matrix housings were placed over each implant (Figure 6) to achieve a successful and functionally correct prosthetic result, and then the remaining steps to fabricate the implant-retained prosthesis were performed chairside (eg, block out procedures, resin polymerization, necessary occlusal adjustments, etc). This process was uneventful, and the patient was elated with the final result (Figure 7). A low-dose CBCT scan (Green CT 2, Vatech) was acquired immediately postoperatively to visualize the positions of all of the implants (Figure 8).
Conclusion
The addition of narrow diameter implants to the armamentarium of dental healthcare providers has given many partially and fully edentulous patients renewed hope for a more expeditious solution to their immediate oral rehabilitation needs. This affordable, single surgery approach to a new healthy smile has been very well received and will continue to provide an alternative to ridge augmentation procedures for years to come.4
About the Author
Todd B. Engel, DDS
Diplomate
International Congress of Oral Implantologists
Founder and Clinical Director
Engel Institute
Private Practice
Charlotte, North CarolinaReferences
References
1. Dhaliwal JS, Albuquerque RF Jr, Murshed M, Feine JS. Osseointegration of standard and mini dental implants: a histomorphometric comparison. Int J Implant Dent. 2017;3(1):15.
2. Bulard RA, Vance JB. Multi-clinic evaluation using mini-dental implants for long-term denture stabilization: a preliminary biometric evaluation. Compend Contin Educ Dent. 2005;26(12):892-897.
3. Goiato MC, Sônego MV, Pellizzer EP, et al. Clinical outcome of removable prostheses supported by mini dental implants. A systematic review. Acta Odontol Scand. 2018;76(8):628-637.
4. Griffitts TM, Collins CP, Collins PC. Mini dental implants: an adjunct for retention, stability, and comfort for the edentulous patient. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100(5):e81-e84.
For more information, contact:
Straumann
straumann.com
800-448-8168