Treating Nonreducing Disc Displacement
Successful "unlocking" with injection and orthotic relies on patient education
Jamison R. Spencer, DMD, MS
Internal derangements of the temporomandibular joint (TMJ) are not uncommon among those who are asymptomatic and very common among those who present with signs and symptoms of temporomandibular disorders.1,2 In many cases, patients who develop a nonreducing disc displacement pass first from a normal disc/condyle relationship to a reducing disc displacement (ie, disc displacement with reduction or "clicking jaw"), which then, over time, begins to become nonreducing (ie, "catch or lock").3,4 This article describes a simple procedure that was used to help a patient who had developed an acute nonreducing disc displacement (ie, closed, locked) return to her previous state of reducing disc displacement.
Case Report
A 69-year-old female patient with a chief complaint involving jaw pain, limited opening, and inability to protrude her jaw was seen for an initial evaluation. The patient stated that her symptoms began approximately 6 months ago when she realized that she had trouble posturing her jaw forward to whistle for her dogs. She reported that she had a long history (ie, more than 50 years) of her jaw popping and clicking on the left side and that this clicking had abruptly stopped around the time that she began experiencing difficulty whistling.
Her clinical examination revealed a maximum interincisal opening of 35 mm with slight deflection to the left side. A spray and stretch procedure was performed on the left masseter and TMJ, which resulted in a reported reduction of pain but no increase in range of motion. A diagnosis of left-side anterior disc displacement without reduction of the TMJ was suspected.
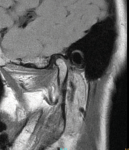
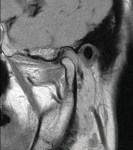
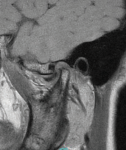
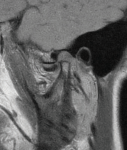
The patient was referred for magnetic resonance imaging (MRI), and both open and closed views were used to investigate the location and condition of the disc. The MRI scans showed that the left-side articular disc was anteriorly displaced in both views, which is consistent with a nonreducing disc displacement (Figure 1 through Figure 4). This diagnosis was discussed with the patient, treatment options were presented, and the patient provided informed consent to be scheduled to proceed with an unlocking procedure.
When the patient returned for the procedure, an ampule of 3% mepivacaine without epinephrine (Carbocaine® 3%, Septodont) was prepared and injected into the joint capsule of her left TMJ. Immediately after the injection, the patient reported feeling a "pop" in her left TMJ. Her maximum opening increased to 46 mm without any deflection or pain. To support the reduction of the articular disc, a temporary mandibular splint was fabricated in a slightly anterior position. The patient was instructed to wear this temporary splint full time for 3 days, including while sleeping, and return for a follow-up in 1 week.
After a week, the patient returned to the clinic. Her maximum opening was measured at 45 mm without deflection or deviation, and she reported a reduction in pain and a feeling of "being unlocked." Impressions were obtained, and the patient returned 1 week later for the fitting of a custom-fabricated, "Farrar-style" maxillary orthotic for nighttime use. At her 1-year follow-up, the patient reported continued nightly use of her orthotic, no further locking episodes, and no pain or dysfunction, and she had retained a maximum opening of 46 mm without deviation or deflection.
Disc Unlocking Treatment
The following procedural synopsis is not intended to be a comprehensive guide or definitive protocol for reducing a nonreducing disc displacement. It assumes that the clinician possesses at least a working knowledge of the diagnosis and treatment of basic internal derangements and some experience administering intra-articular injections. Clinicians who do not possess this basic knowledge should seek out appropriate courses and mentors in order to gain proficiency.
Diagnosis and Informed Consent
The diagnosis of a nonreducing disc displacement is achieved through patient history, examination, and, whenever possible, MRI. Relevant signs and symptoms revealed through history and examination include the following:
• A history of reducing disc displacement (ie, clicking), often for many years
• A history of episodes of catching or locking after which the patient was able to move his or her jaw to cause a click/pop and regain full range of motion
• A history of waking up "locked closed"
• A limited range of motion, which is very often around 26 mm interinsically but may also be 30 mm or slightly more, depending on how long the patient has been locked
• A slight to pronounced deflection of the mandible to the affected side
Unlike the palpable clicking/popping of a reducing disc displacement, nothing is felt upon palpation of a nonreducing disc displacement. Because many conditions can result in limited range of motion, as well as deflection, it is wise to also obtain an MRI scan of the bilateral TMJs in order to definitively confirm diagnosis.5,6 Such a scan should be performed without contrast and include both closed and wide-open views. The dentist is strongly encouraged to obtain the images and review them independently, then speak with the radiologist should there be any questions with regard to the impression.
Once the diagnosis has been made and an unlocking procedure is indicated, it is important to obtain written informed consent. Patients should be educated about the possible side effects, including bruising and/or pain at the site of the injection, a reaction to the anesthetic or one of its components, and partial temporary facial paralysis as well as the potential for failure of the procedure. Consent is usually obtained at least a day before patients are seen for the procedure. It is also important to discuss alternative treatment options that can be pursued should the procedure be unsuccessful. These options include repeating the procedure, arthrocentesis, arthroscopic surgery, open joint surgery with plication, treating "off the disc" with splint therapy, physical therapy, doing nothing, etc.
The Injection
Prepare the injection area with alcohol or iodine solution wipes. If desired, a topical anesthetic, such as a cold spray, may be used to make the injection more comfortable. The injection is performed using 1 ampule of a short acting anesthetic, such as mepivacaine without epinephrine (eg, Carbocaine® 3%, Septodont), or 2 cc of lidocaine (eg, Xylocaine®-MPF, Fresenius USA) in a Luer lock syringe with either a 30 gauge 1 inch or 27 gauge 1 and 1/4 inch needle, depending on the size of the patient.
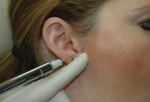
Prior to injection, the joint space is palpated immediately anterior to the tragus with the patient's mouth open as wide as he or she is able to hold it. Injection into the posterior-superior joint space is ideal. The needle should travel anteriorly, medially, and superiorly until it is approximately 1 inch deep, again, depending on the size of the patient. Contact with the posterior aspect of the condyle is not necessary but may occur and help to confirm location (Figure 5 and Figure 6). Prematurely injecting while the needle goes in can result in inadvertent anesthesia of the temporal and/or zygomatic branches of the facial nerve, which will make it difficult for the patient to close his or her eye.
After the injection, ask patients if their bite feels different. They should respond that it does and be unable to close their posterior teeth together on that side. If their bite hasn't changed, it is still likely that anesthesia of the auriculotemporal nerve will occur, which will provide partial anesthesia of the joint. The auriculotemporal nerve provides approximately 75% of the innervation of the joint capsule with additional innervation via the deep temporal and masseteric nerves. If desired, now that the injection site is most likely numb, the clinician could try again to enter the joint capsule. The goal of depositing the anesthetic inside the joint capsule is less about the anesthetic effect and more about the hydraulic effect and its resultant increase in the efficacy of the unlocking treatment.
Unlocking and Education
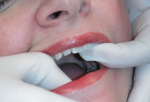
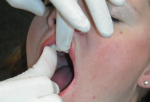
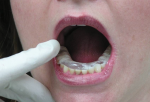
Once a successful injection has been performed, ask patients to start moving their jaw from side to side followed by opening wide. They should continue doing this for the next few minutes. It is common for 30% to 50% of patients to unlock on their own, simply through gentle lateral movements and the opening and closing of the jaw. It is prudent to observe patients for a few minutes after the injection in case they become syncopal or experience another adverse reaction. If patients are unaccompanied, an assistant should stay in the room to monitor their condition. During the few minutes that patients are given to attempt to unlock on their own, a thermal sensitive plastic is prepared for the fabrication of a temporary splint. In cases in which patients do not unlock on their own, simply helping them move their jaw laterally to the opposite side of the lock, followed by helping them open wide, may reduce the disc displacement (Figure 7 and Figure 8).
Once patients unlock successfully, the next step is patient education. This is the most important post-unlocking step. If patients are not able to feel the difference between "being locked" and "being unlocked," it is likely that no matter what is done next, they will walk out of the office and relock within the next 24 hours. To educate patients, have them close on their back teeth and try to make the disc displace again. This is to help them feel the difference between being locked and unlocked and to help them realize that they can unlock on their own if they discover that they have locked again after leaving the office. After patients have performed this exercise a few times, they are shown that they should be able to place three fingers vertically between their incisors if they are unlocked, and they are asked to check their opening every 5 minutes until they go to bed that night. They are also asked to check their opening first thing upon waking the next morning. If they feel they are locked again, they are instructed to get in the shower, let the hot water relax their jaw, and try to unlock again. Patients are asked to call the office the morning after the procedure to report on their status.
After the education session, patients are fit with a temporary mandibular thermoplastic splint. The splint is usually made with an "end-to-end" incisor relationship for Class I and Class II, division 2, patients. However, it is far more important that the position is able to keep the disc displacement reduced, if possible.7 Patients are instructed to wear this splint full time, including during meals, for the next 3 to 4 days and then at night for at least another week (Figure 9 through Figure 13).
Follow-Up and Alternatives
After a week, patients return for a follow-up. If they have locked again, the procedure may be repeated. If they have remained unlocked, they are reminded of the nature of their internal derangement and the likelihood of repeated locking episodes without preventive measures. Those measures will depend on when patients' locking episodes have been most likely to occur historically, but very often include the use of a specialized nighttime oral orthotic designed to reduce the likelihood of locking during sleep.
If several attempts at this conservative approach to unlocking a patient are unsuccessful, the patient is encouraged to proceed with arthrocentesis or arthroscopic surgery or to begin initial splint therapy. Recommendations are based on each patient's diagnosis, pain, dysfunction, and quality-of-life issues. If an unlocking procedure is unsuccessful and an MRI scan has not yet been obtained, it would be highly recommended to obtain one prior to further therapy or referral for surgery in order to confirm the diagnosis.
Unfortunately, arthrocentesis and arthro-scopic surgery only rarely result in the long-term reduction of a nonreducing disc displacement. Fortunately, however, reduction of pain and increased range of motion is common.8,9 The lack of long-term success with surgery may be due to the fact that a stabilization splint is commonly not fit immediately after the procedure, particularly if the patient has been sedated.
Conclusion
It is very common for patients to progress from a reducing disc displacement to a nonreducing disc displacement. Understanding the typical presentation, history, and clinical signs and symptoms and, when indicated, referring for MRI, will allow the dentist to make an accurate diagnosis. Time is of the essence. The longer patients remain locked, the less likely an unlocking procedure will be successful.
About the Author
Jamison R. Spencer, DMD, MS
Director
Center for Sleep Apnea and TMJ
Boise, Idaho, and Salt Lake City, Utah
Adjunct Faculty
University of the Pacific
Arthur A. Dugoni School of Dentistry
San Francisco, California
References
1. Giraudeau A, Cheynet F, Mantout, B, et al. Prevalence and distribution of intracapsular derangement of TMJ in an asymptomatic and a symptomatic population. J Stomat Occ Med. 2008;1:5-15.
2. Paesani D, Westesson PL, Hatala M, et al. Prevalence of temporomandibular joint internal derangement in patients with craniomandibular disorders. Am J Orthod Dentofacial Orthop. 1992;101(1):41-47.
3. Young AL. Internal derangements of the temporomandibular joint: a review of the anatomy, diagnosis, and management. J Indian Prosthodont Soc. 2015;15(1):2-7.
4. Manfredini D, Guarda-Nardini L, Winocur E, et al. Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112(4):453-462.
5. Yang Z, Wang M, Ma Y, et al. Magnetic Resonance Imaging (MRI) evaluation for anterior disc displacement of the temporomandibular joint. Med Sci Monit. 2017;23:712-718.
6. Santos KC, Dutra ME, Warmling LV, Oliveira JX. Correlation among the changes observed in temporomandibular joint internal derangements assessed by magnetic resonance in symptomatic patients. J Oral Maxillofac Surg. 2013;71(9):1504-1512.
7. Liu M, Lei J, Han J, et al. Metrical analysis of disc-condyle relation with different splint treatment positions in patients with TMJ disc displacement. J Appl Oral Sci. 2017;25(5):483-489.
8. Ohnuki T, Fukuda M, Nakata A, et al. Evaluation of the position, mobility, and morphology of the disc by MRI before and after four different treatments for temporomandibular joint disorders. Dentomaxillofac Radiol. 2006;35(2):103-109.
9. Emshoff R, Gerhard St, Ennemoser T, Rudisch A. Magnetic resonance imaging findings of internal derangement, osteoarthrosis, effusion, and bone marrow edema before and after performance of arthrocentesis and hydraulic distension of the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(6):784-790.