Efficient Direct Restorative Quadrant Dentistry
Self-adhesive flowable composite improves predictability and offers bioactive benefits
Jack D. Griffin Jr, DMD
Dentists have been drilling holes and filling them for many decades now. One of our long-standing goals has been to ensure that we do no harm and that our chosen techniques and materials do not have a negative effect on the oral tissues.1 Now, the challenge is not merely to avoid the negative but, instead, to have a positive influence, which has led to the development and popularity of bioactive/regenerative materials.2
Regarding these restorative materials, the goal is to provide a therapeutic environment with a reduction in microbes, the stimulation of secondary dentin, and ultimately, a less sensitive, longer lasting esthetic direct restoration. These durable therapeutic "fillings" help provide an environment where tissues can heal.2
Traditional Composites
When placing direct restorations, most clinicians use phosphoric acid, at least on the enamel, and then place a bonding agent prior to the filling material. A dentin bonding agent lines the dentin and is the intermediary between the tooth structure and the restorative material. The undeniable clinical success associated with using these techniques and materials has been validated by the millions of successful restorations that have been placed by many dentists with relatively few complications.
Unfortunately, postoperative sensitivity, recurrent decay, stained margins, and reduced longevity are just some of the issues encountered by dentists when placing composite restorations. The step that presents the greatest potential for mishap regarding placement and handling is the bonding step; however, the etching technique, etching time, proper rinsing, effective drying, application technique, quality of air thinning, proper curing, and subsequent addition of composite can all also be areas of concern for even the most attentive clinician.
Bioactive Materials
Today, new materials are available that possess exemplary clinical properties and that also have a positive impact on the oral environment through ion release.3 These "bioactive" materials differ from most traditional materials in that they are more biologically tolerant and can influence the dentinal hard tissue to repair itself.4 The ability to stimulate hydroxyapatite formation and other tissue regeneration (ie, pulp, blood vessels, dentin, and bone) has been well studied.5 The ionic release by the material and uptake by the dentin at the material/tooth interface is key to this process.6
When attempting to achieve this therapeutic effect, the application of a dentin bonding agent may impede the desired ionic exchange by forming a physical barrier and reducing the bioavailability of the ions to the tooth. Therefore, a self-adhesive bioactive direct restorative material would have the advantage of being in direct contact with the hard tissues, particularly the dentin, allowing for a greater ionic influence.7 This case report describes the use and benefits of such a material.
Case Report
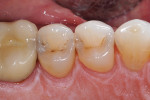
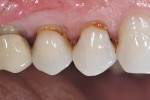
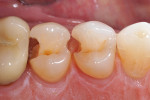
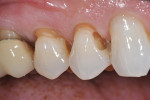
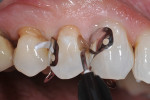
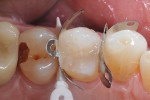
A patient reported for upper right quadrant dentistry. Decay was affecting the occlusal, interproximal, and facial surfaces (Figure 1 and Figure 2). The preparations were performed with a No. 330 carbide bur, and the decay was removed with a No. 2 round bur and spoon, then verified with a caries indicator (Figure 3). After all of the enamel was beveled, the teeth were thoroughly rinsed (Figure 4).
Lip retractors were placed, followed by sectional matrices and wedges (Figure 5). First, the cuspid and first bicuspid were restored. A bioactive self-adhesive light-cure flowable restorative (FIT SA™, Shofu) was placed, covering all dentin and all margins in a layer approximately 0.5-mm thick, and allowed to sit for 20 to 30 seconds before curing. It is important to note that the time that the material is in contact with the tooth before curing helps determine the extent of the self-adhesion and that the clinician should avoid the temptation to begin curing it too quickly.
This bioactive self-adhesive flowable is a regenerative material that offers the performance of a composite without the need for a bonding agent. Its Giomer Technology, which releases six beneficial ions (ie, fluoride, sodium, strontium, silicate, borate, aluminum), results in positive effects, including inhibition of plaque, neutralization of acid, increased mineralization, and others.8 This material both releases and recharges all of the beneficial ions, and it possesses excellent clinical characteristics for long-term success.9 An independent laboratory evaluation reported its shear bond strength to enamel as excellent and to dentin as above average when compared with most self-etching universal adhesives.10 In addition, when compared to other injectable/flowable composites, its clinical performance was above average to excellent in categories such as depth of cure, hardness, flexural strength, compressive strength, shrinkage, and polishability.10
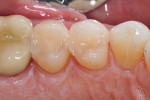
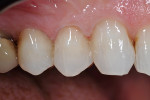
The remainder of the restoration was completed with a bioactive universal composite (Beautifil II LS, Shofu) that was placed in 2-mm layers (Figure 6). The matrices were then moved to the second bicuspid, and the procedure was repeated. After complete polymerization with an LED curing light, the shaping was done with a fine finish diamond and a round bur, the occlusion was checked, and the restorations were polished (Figure 7). All of the margins had the bioactive self-adhesive flowable covering them in a thin layer, and the remainder of the restored surfaces were composed of the universal composite. Both materials polish very well and maintain an excellent long-term luster (Figure 8).
Conclusion
The excellent clinical performance of functional, esthetic, comfortable, and long-lasting restorations is the clinician's goal, and producing a regenerative effect should become the new goal in materials. Clinicians should consider all of the characteristics of materials and techniques to select those that best fit their method of practice and their patients' needs. However, if materials are otherwise similar in clinical performance and esthetics, those that have a positive influence on the oral environment should be preferred over those that do not.
About the Author
Jack D. Griffin Jr, DMD
Private Practice
Lake St. Louis, Missouri
For more information, contact:
Shofu Dental
shofu.com
800-827-4638
References
1. Hench LL, Splinter RJ, Allen WC, Greenlee TK. Bonding mechanisms at the interface of ceramic prosthetic materials. J Biomed Mater Res. 1071;5(6):117-141.
2. Dworkin O, Kugel G, Loo C. What is bioactive dentistry? A review. Dent Today. 2018;37(1):44-46.
3. Sidhu SK, Nicholson JW. A review of glass-ionomer cements for clinical dentistry. J Funct Biomater. 2016;7(3):16.
4. Elsenpeter R. How bioactive materials are changing restorative dentistry. Dental Products Report. https://www.dentalproductsreport.com/dental/article/how-bioactive-materials-are-changing-restorative-dentistry. Published June 21, 2018. Accessed October 28, 2020.
5. Goldstep F. Bioactivity in restorative dentistry: a user's guide. Oral Health Group. https://www.oralhealthgroup.com/features/bioactivity-restorative-dentistry-users-guide/. Published January 11, 2018. Accessed October 28, 2020.
6. Chatzistavrou X, Lefkelidou A, Papadopoulou L, et al. Bactericidal and bioactive dental composites. Front Physiol. 2018;9:103.
7. Jeffries SR. Bioactive and biomimetic restorative materials: a comprehensive review. Part I. J Esthet Restor Dent. 2014;26(1):14-26.
8. Nagafuji A, Shino K, Kimoto K, et al. Acid-neutralizing capacity of resin-based materials containing S-PRG filler. 2010 IADR/PER General Session;89(B):1437.
9. Jyothi KN, Annapurna S, Kumar AS, et al. Clinical evaluation of giomer- and resin-modified glass ionomer cement in class V noncarious cervical lesions: An in vivo study. J Conserv Dent. 2011;14(4):409-413.
10. Cowen M, Powers JM. Laboratory evaluation of FIT SA. Dental Advisor.2019;129.