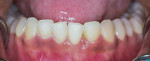
Treatment of Localized Aggressive Periodontitis
Regenerative periodontal therapy offers alternative to extraction/implant placement
Ahmad Soolari, DMD, MS
Due to the effect of implant-related complications, the longevity of implants is often questionable, even when compared with that of compromised but successfully treated natural teeth. This article describes a case of severe, localized periodontal disease in which the patient rejected a recommendation to undergo extraction followed by implant placement and restoration in favor of receiving regenerative periodontal therapy to save the natural tooth.
Case Report
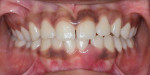
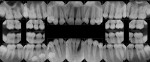
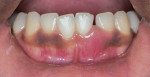
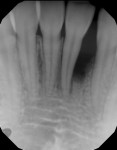
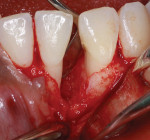
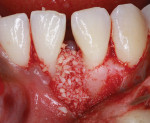
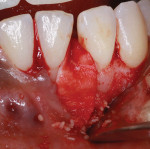
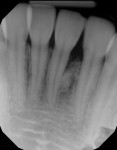
A 17-year-old female patient presented with bone loss associated with tooth No. 24. A clinical examination and periodontal evaluation (ie, assessment of mobility, probing depth, bleeding on probing, plaque score, and clinical attachment loss) revealed severe horizontal and vertical bone loss, deep probing depth with bleeding, class II mobility, a widened periodontal ligament, traumatic occlusion, and the formation of a diastema between the teeth (Figure 1 through Figure 4). In addition, there was bone loss of a lesser magnitude associated with tooth No. 23. The radiograph of tooth No. 24 suggested vertical and horizontal bone loss extending to the apical one-third of the root length. This was an isolated deep intrabony defect with inconsistent margins, which could be measured from the cementoenamel junction or from the crest of the alveolar bone to the base of the defect. A periapical radiograph showed angular bone loss on the distal aspect of tooth No. 24 with an angle of almost 45°. The interproximal space between tooth No. 24 and tooth No. 23 was the only site with severe bone loss throughout the patient's mouth; therefore, the diagnosis was localized aggressive periodontitis. The patient's medical history was unremarkable, but a significant finding was the retention of primary teeth with premolar impaction on the lower right side. The patient was later referred to an orthodontist for consultation.
The goal of regenerative periodontal therapy is to improve a tooth's prognosis by regenerating the supporting structures. In this case, the prognosis for tooth No. 24 was poor, and in such cases, the current trend in the dental community is to extract the tooth and place an implant. However, the patient could not afford implants and wanted to retain her natural tooth for as long as possible. Moreover, the longevity of implants does not surpass that of compromised but successfully treated natural teeth,1 and biologic and prosthetic complications are common as implant cases age.2 Beyond these considerations, the successful placement of an implant and management of the space between teeth Nos. 23 and 24 would require a greater volume of bone and gingiva; therefore, the existing site was not favorable for implant placement. The patient accepted a treatment plan that included surgical regenerative periodontal therapy.
Clinical Treatment
Prior to the surgical appointment, scaling and root planing was performed and occlusal adjustments were made. A reevaluation of the area 6 weeks after scaling and root planing revealed moderate improvements in probing depth, bleeding on probing, and the clinical attachment loss. However, a 6-mm probing depth with bleeding on probing persisted; therefore, regenerative periodontal therapy was planned as an alternative to tooth extraction and prosthodontic treatment. The patient was made aware that the scaling and root planing treatment was only the initial phase of the periodontal therapy and that a surgical phase would follow.
In advance of the procedure, the patient was premedicated with 250 mgs of metronidazole and 500 mgs of amoxicillin 3 times a day for 2 weeks. After anesthesia was achieved, envelope incisions were made from the distal aspect of tooth No. 21 to the mesial aspect of tooth No. 25 using a No. 12 scalpel blade (No. 12 Carbon Steel Scalpel Blades, Benco Dental). This enabled access to the root and osseous defect in the interproximal area between teeth Nos. 23 and 24 via a full-thickness flap that was raised beyond the mucogingival junction to facilitate the ridge-augmentation procedure. The flap elevation enabled access to the granulation tissue occupying the defect, and the subsequent removal of the granulation tissue allowed visualization of the defect, which measured 5 mm × 8 mm. The lack of access to the root and osseous defect resulted in the destruction of buccal and lingual bone plates (Figure 5). The teeth were scaled and root planed again to remove any remaining plaque and calculus. Debridement of all necrotic tissue enabled observation of the bare bone with no bleeding. Once debrided, the osseous defect was filled with a particulate freeze-dried bone allograft (Cortical Bone, Maxxeus Dental) (Figure 6) and covered with a resorbable membrane (Bio-Gide®, Geistlich Biomaterials) that was trimmed and fitted to the interproximal area (Figure 7). The flap was coronally advanced to cover the membrane and was secured into position with simple interrupted 4-0 sutures (Coated VICRYL® [polyglactin 910] Suture, Ethicon). After the periodontal surgery, the patient was advised to return in 3-month intervals for maintenance appointments to prolong the improvements achieved during surgery, which were normal to shallow probing depth, attachment level gain, and no bleeding on probing. The patient's compliance with this recommendation was erratic, but this did not negatively affect attachment gain. The patient was informed that the benefit of periodontal treatment, whether surgical or nonsurgical, can be short-lived without a commitment to regular periodontal maintenance visits.
At a 3-year follow-up appointment, radiographs were taken, and they demonstrated that tooth No. 23 had improved and that tooth No. 24 was fully functional and had no more mobility, no widened periodontal ligament, and no diastema (Figure 8). In this case, regenerative periodontal therapy was able to produce a remarkable regainment of bone (ie, 8 mm) within 3 years. A 3-year postoperative photograph of the lower anterior ridge (Figure 9) demonstrates an improvement in the tissue's color, tone, and texture as well as a lack of edema. There was no bleeding on probing, the probing depth was 3 mm, and there was no tooth mobility or open contact.
Discussion
An advanced surgical reconstruction approach can yield a favorable long-term prognosis, maintain natural healthy dentition, and overcome the need for a prosthesis.3 Biological and technical complications can occur in as many as 50% of implants within 10 years of placement.4 In a discussion of technical factors (eg, occlusion, improper implant placement, angulation of implants, poorly planned prostheses, loading too early, etc) and biological factors (eg, poor oral hygiene, periodontal disease, systemic diseases, smoking, specific microbes causing peri-implantitis) that can affect the success of implants, it was noted that approximately 25% to 30% of the adult population have overt grinding or clenching bruxism and that this could contribute to implant failure if the implant-supported prosthesis has an inadequate occlusal design to address bruxism. 5 Poorly designed implant-supported prostheses are not conducive to the patient's performance of oral hygiene, which can lead to the presence of disease around a dental implant and eventually cause peri-implantitis. Poor personal oral hygiene and periodontal disease are etiologic factors for attachment loss around lateral incisors, and these factors can cause the same problem and even more harm around implant-retained restorations used to replace lateral incisors.3 Because implants are not completely trouble free, can be expensive, and do not necessarily last longer than natural teeth, retaining a patient's natural teeth should be the goal whenever possible. For cost-effective, positive outcomes, periodontists should adopt a balanced approach between placing implants and employing regenerative periodontal therapy in which patients are assessed for the appropriateness of each on a case-by-case basis. Successful regenerative periodontal therapy requires access to the root and osseous defect to enable proper diagnosis and debridement. Reynolds and colleagues suggested that successful outcomes could be expected after early intervention for intrabony defects with regenerative approaches.6 Regenerative materials such as freeze-dried bone allografts, barrier membranes, and growth factors are placed at the site to potentiate the formation of new cementum, bone, and a functional periodontal ligament during the healing process. Prior to finalizing any treatment plan, periodontists should consider the risk of disease progression and subsequent tooth loss as well as which option (ie, implant placement versus preservation of natural teeth) is likely to result in a better prognosis with fewer complications, is preferred by the patient, and is economically justifiable.7
The longevity of implants and of compromised but successfully treated natural teeth should also be considered before finalizing a treatment plan. Several factors must be taken into account. First, the tissues around implants may be more susceptible to plaque-associated infections than the tissues around natural teeth.8 In a study involving beagle dogs, plaque was allowed to accumulate around natural teeth and dental implants to induce periodontal disease. The results from the clinical and histological examinations revealed that tissue destruction was more pronounced at the implant sites than at the sites of the natural teeth. The extent and severity of hard- and soft-tissue breakdown was greater around the implants than the natural teeth, and it even extended into the bone marrow.8 Second, the risk of developing peri-implantitis is higher among patients who are susceptible to periodontitis,5 and the treatment of peri-implantitis is not predictable.8 Third, the cost of maintaining implants can be much higher than the cost of maintaining natural teeth.10 Fourth, approximately 50% of implant cases may experience biological and technical complications within 10 years.4 And finally, compromised but successfully treated natural teeth last longer than implants.1 Implant treatment outcomes are generally positive, but implants do occasionally fail, and this can occur due to a variety of reasons, including metal allergies, occlusal issues, previous periodontal disease, oral hygiene, diet, systemic disease, smoking, inadequate bone, or microbial colonization.5 Another issue that merits consideration is the expertise of the practitioner. A comparison of implant treatments rendered by different types of practitioners found that the survival rate of implants placed by inexperienced practitioners was 73.0% whereas the survival rate of implants placed by implant specialists was 95.5%.11 To aid in the decision of whether or not to extract a tooth and place an implant, Pjetursson and Heimisdottir offer a system to classify teeth as secure, doubtful, or irrational to treat.12 Overall, dentists should attempt to retain natural teeth whenever possible.
The case presented here demonstrates that a tooth with a poor prognosis can be retained using appropriate regenerative periodontal therapy. Not every tooth with a poor prognosis can be saved, but advances in regenerative periodontal therapy can sometimes enable dentists to avoid tooth extraction and implant placement, preserving the natural dentition.
About the Author
Ahmad Soolari, DMD, MS
Diplomate
American Board of Periodontology
Private Practice
Gaithersburg, Potomac, and Silver Spring, Maryland
References
1. Holm-Pedersen P, Lang NP, Müller F. What are the longevities of teeth and oral implants? Clin Oral Implants Res. 2007;18(Suppl3):15-19.
2. Derks J, Schaller D, Håkansson J, et al. Effectiveness of implant therapy analyzed in a Swedish population: prevalence of peri-implantitis. J Dent Res. 2016;95(1):43-49.
3. Kamil W, Al Bayati L, Hussin AS, Hassan H. Recon-struction of advanced bone defect associated with severely compromised maxillary anterior teeth in aggressive periodontitis: a case report. J Med Case Rep. 2015;9:211. doi: 10.1186/s13256-015-0677-6.
4. Lang NP, Berglundh T, Heitz-Mayfield LJ, et al. Consensus statements and recommended clinical procedures regarding implant survival and complications. Int J Oral Maxillofac Implants. 2004;19(Suppl):150-154.
5. Christensen GJ. Why are implants failing? Dentaltown website. https://www.dentaltown.com/magazine/article/7757/why-are-implants-failing. Published October 2019. Accessed January 9, 2020.
6. Reynolds MA, Kao RT , Camargo PM, et al. Periodontal regeneration - intrabony defects: a consensus report from the AAP Regeneration Workshop. J Periodontol. 2015;86(2 Suppl):S105-S107.
7. Donos N, Laurell L, Mardas N. Hierarchical decisions on teeth vs. implants in the periodontitis-susceptible patient: the modern dilemma. Periodontol 2000. 2012; 59(1):89-110.
8. Lindhe J, Berglundh T, Ericsson I, et al. Experimental breakdown of peri-implant and periodontal tissues. A study in the beagle dog. Clin Oral Implants Res. 1992; 3(1):9-16.
9. Lindhe J, Meyle J, Group D of European Workshop on Periodontology. Peri-implant diseases: consensus report of the sixth European workshop on periodontology. J Clin Periodontol. 2008;35(8 Suppl):282-285.
10. Fardal Ø, Grytten J. A comparison of teeth and implants during maintenance therapy in terms of the number of disease-free years and costs -- an in vivo internal control study. J Clin Periodontol. 2013;40(6):645-651.
11. Setzer FC, Kim S. Comparison of long-term survival of implants and endodontically treated teeth. J Dent Res. 2014;93(1):19-26.
12. Pjetursson BE, Heimisdottir K. Dental implants - are they better than natural teeth? Eur J Oral Sci. 2018;126(Suppl 1):81-87.