Stress-Free Delivery of Restorations for Sleep Apnea Patients
Allow patients to continuously wear their existing appliances during and after treatment
Tony Soileau, DDS
The treatment of sleep apnea by a dentist using a mandibular advancement device as an alternative to treatment by a medical doctor using a continuous positive airway pressure (CPAP) machine is becoming popular. Some patients prefer the convenience of a dental device to a CPAP machine and are being referred by their physicians to dentists for treatment.1-5 The comorbidities of sleep apnea can be life-threatening and debilitating. Oftentimes, this places dentists in the difficult position of having to choose whether to begin sleep apnea treatment prior to restorative care. Obviously, a dental appliance cannot be placed over teeth with severe periodontal issues, but teeth that have fractured cusps and failing restorations can often support a dental appliance. This requires dentists and laboratory technicians to then retrofit crowns and bridges to fit existing sleep apnea appliances. This article discusses techniques to create both temporary and final restorations that fit an existing mandibular advancement device.
Case Report
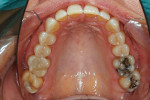
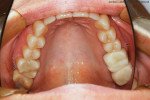
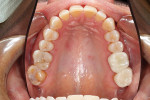
A patient presented to the office who had been prescribed a mandibular advancement device (ProSomnus® [IA] Sleep and Snore Device, ProSomnus Sleep Technologies) 6 months prior to treat her sleep apnea. Although she required posterior restorations, the patient had elected to immediately treat her sleep apnea prior to restoring her posterior teeth because of severe health issues. Once her sleep apnea was under control and she was feeling better, she elected to accept treatment to restore her posterior teeth (Figure 1). After consulting with the patient's medical doctor, it was decided that for the health of the patient, it would be best to provide a treatment plan that included both temporary and final restorations that would accommodate her current sleep device, allowing her to continuously wear it both during and after the restorative treatment.
Temporary Restoration
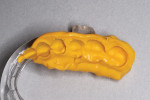
The first step was to fabricate a temporary restoration that fit within the sleep appliance. The existing appliance was used as the tray for the fabrication of the provisional matrix. This ensures that the temporary restoration will fit within the appliance with little to no reduction. To prepare for the impression, the inside of the tray was lightly roughened with an acrylic bur. If needed, the rough surface can later be repolished to make cleaning the appliance easier for the patient. A light body vinyl polysiloxane impression material (Honigum Pro Light, DMG America) was injected into the sleep appliance, and both the maxillary and mandibular components were seated on the teeth. The patient was instructed to bite for 2 minutes as the material set. The light body material creates an extremely thin liner that will act as the matrix for the creation of the temporary restorations, ensuring that the provisional material will not adhere to the appliance during fabrication (Figure 2). The light body impression material also allows for the accuracy needed for the lingual contours of the teeth to be restored. It should be noted that the original sleep appliance was designed and fabricated to be lingual-less to ensure maximum room for the patient's tongue.6,7
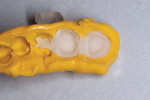
After preparing the teeth, the final impressions were taken with a heavy body and a light body material (Honigum Pro, DMG America) using impression trays.8 Next, a temporary restorative material (Luxatemp Ultra, DMG America) was injected into the mandibular advancement device that had been lined with the light body material (Figure 3). It was inserted into the mouth along with the opposing appliance, and the patient was told to bite while the material set.
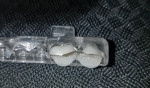
If a traditional matrix from a model is preferred, start by injecting light body impression material into the sleep appliance and taking an impression, then inject bite registration material (O-Bite, DMG America) into the impression. This provides an accurate model to fabricate a wax-up and provisional matrix chairside in minutes without having to mix and pour stone and then wait for it to set (Figure 4).
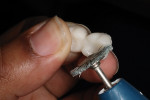
Once the temporary material had set, the excess material was quickly trimmed to ensure that the temporary restoration fit within the sleep appliance (Figure 5). In this case, the cusp tips, which may cause lateral interferences, were slightly shortened.
The temporary restoration was then polished (Figure 6) and cemented into the mouth using a transparent temporary cement (TempoCemID, DMG America) for optimal adhesion and ease of cleanup (Figure 7).
In the event that an acrylic appliance or an appliance with a rubber lining, such as a Herbst appliance, is used in the making of the provisional restorations, the lingual aspects of the teeth are already covered. For these cases, a denture pressure spray should be used as a releasing agent so that the temporary material does not stick to the appliance.
Final Restoration
For the fabrication of the final restorations (Figure 8) and for any cases that require the provisional restorations to be sent to the dental laboratory, other considerations may need to be taken into account. When creating the temporary restoration, the appliance can be used during the appointment and then sent home with the patient. However, the laboratory does not have this advantage. How this is best handled will be determined by the type of sleep appliance used by the patient. Some sleep appliances, including the one involved in this case, come with several arches to be used in the therapy. This means that there is always a mandibular and maxillary tray that is not being used. The tray that is not being used can be sent to the laboratory along with the final impressions. This allows the laboratory to ensure that the final restorations fit within the appliance. If a single sleep appliance with a mechanical advancement mechanism is used (eg, dorsal appliance, Herbst appliance), then the model used to make the sleep appliance is sent to the laboratory. From this model, the laboratory can make a stent to ensure that the final restoration fits the internal shape of the sleep appliance. If the initial treatment plan is to deliver a sleep appliance prior to performing restorative treatment, it is suggested that the initial impressions taken for the sleep appliance be used to immediately pour models to create a wax-up showing the final plan for restoring any broken cusps or missing teeth, which can then be sent to the laboratory for future reference. Care must be taken to avoid changing the shape of the original model too much because this reduces the intimate contact between the sleep appliance and the existing dentition, which can result in a loose-fitting sleep appliance.
Conclusion
Providing treatment for sleep apnea is both rewarding and profitable, but it can also become frustrating if a successful sleep appliance fails because it no longer fits after restorative care has been provided. Insisting that patients have all restorative care done prior to making a sleep appliance can (and often does) result in poor patient acceptance and reduced referrals from physicians. However, with a little planning, restorative care after sleep appliance fabrication can be successful and stress free.
About the Author
Tony Soileau, DDS
Private Practice
Lafayette, Louisiana
For more information, contact:
DMG America
dmg-america.com
800-662-6383
References
1. Young T, Palta M, Dempsey J, et al. The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med. 1993;328(17):1230-1235.
2. Ramar K, Dort LC, Katz SG, et al. Clinical practice guideline for the treatment of obstructive sleep apnea and snoring with oral appliance therapy: an update for 2015. J Clin Sleep Med. 2015;11(7):773-827.
3. Hoffstein V. Review of oral appliances for treatment of sleep-disordered breathing. Sleep Breath. 2007;11(1):1-22.
4. Ferguson KA, Cartwright R, Rogers R, et al. Oral appliances for snoring and obstructive sleep apnea: a review. Sleep. 2006;29(2):244-262.
5. Schmidt-Nowara W. Recent developments in oral appliance therapy of sleep disordered breathing. Sleep Breath. 1999;3(3):103-106.
6. Burns J, Palmer R, Howe L, et al. Accuracy of open tray implant impressions: an in vitro comparison of stock versus custom trays. J Prosthet Dent. 2003;89(3):250-255.
7. Mitchell JV, Damele JJ. Influence of tray design upon elastic impression materials. J Prosthet Dent. 1970;23(1):51-57.
8. Boksman L. Eliminating variables in impression-taking. Ont Dent. 2005;34:22-25.