Biomimetic Tooth Repair
Using bulk-fill, resin-based composite for the enamel component
Theodore P. Croll, DDS, Joel H. Berg, DDS, MS
Although restoration of a permanent molar or premolar with a Class I caries lesion is not complicated from the perspective of having a compromised proximal wall, it can otherwise be challenging in view of preparation design, removal of infected tooth structure, protection of the pulp to promote healing and reduce postoperative sensitivity, and replication of the form and function of lost dentin and enamel. According to Merriam-Webster, the definition of the word restore is "to bring back to or put back into a former or original state." Therefore, a workable definition of restoration, as it relates to direct application tooth repair, is "to return the tooth to the state it was in or should have been in." The simple replacement of dentin and enamel with a single material can function well, as has been the case for more than a century with silver amalgam and various dental gold materials. However, current dental restorative science using adhesive repair materials has become more complex. Resin-based composites and glass-ionomer restorative systems, especially the resin-modified glass-ionomer (RMGI) cements, have become the most prominent direct application tooth repair materials, and understanding them is important to ensure that they are used to their best advantage.
Tissue-Specific Restoration
Dentin and enamel are both calcified tissues, but they originate from distinct embryologic layers and have completely different physical and mechanical properties. Enamel is overwhelmingly inorganic; therefore, any material used to replace it must have high resistance to occlusal and masticatory impact and substantial physical strength to resist wear, fracture and fracture propagation, and erosion, whereas dentin has a large organic component and pathways to the pulp that make it vital tissue. In addition, there are morphologic differences between these substrates that create complex challenges regarding their ability to bond to different materials.
The so-called "sandwich technique" or stratification method of tooth restoration serves to accommodate the need for replacing dentin and enamel independently, using separate materials that more closely mimic each of these natural tooth structures. This has been referred to as "biomimetic" or "tissue-specific" tooth repair.1-6 Just as the orthopedic surgeon replaces a destroyed knee with a prosthesis that duplicates the form and function of the original joint, the dentist uses the best materials available to replicate and thus "restore" the original tissues, respectively.
Material Selection
Repairing teeth using a direct application stratification technique requires dentin replacement with a material that mimics dentin, usually a glass ionomer or an RMGI. Previous research demonstrates the appropriateness of using a hydrophilic glass-ionomer material to replace dentin. The physical properties of glass ionomers closely resemble those of dentin. These properties, combined with the ability to chemically bond to tooth structure, biocompatibility, similar coefficients of thermal expansion, and fluoride content in the glass filler, make glass ionomers ideal to replace dentin.7 Enamel is usually replaced with resin-based composite-a hydrophobic material with physical characteristics that are capable of withstanding the insults of occlusion, mastication, pH and temperature changes, and the microflora of the oral environment. In addition, resin-based composites are tooth-colored and form strong bonds with enamel through the acid-etch method of micromechanical attachment. Just as the dentin biologically fuses to the enamel at the dentinoenamel junction, the resin component of an RMGI chemically bonds to the resin-based composite, joining the materials as one restorative mass. Ideally, this fusion of specific materials will completely and indefinitely seal the interface of the restoration and tooth structure from microleakage. This is where the coefficients of thermal expansion of the respective materials will play an important role as the restoration ages.
The following clinical case illustrates a Class I occlusal restoration of a carious permanent second molar using stratified repair and specific pulp protection. An RMGI-type material is used to replace the dentin, which is then overlaid with a new bulk-fill, resin-based composite to restore the anatomical surface of the enamel.
Clinical Case
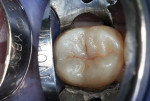
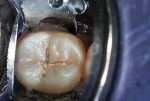
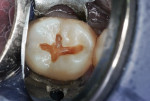
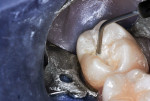
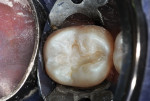
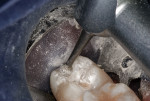
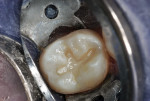
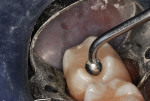
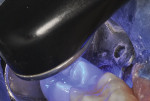
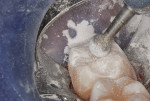
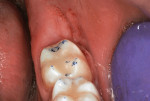
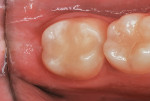
A 16-year-old girl presented with a caries lesion on the occlusal surface of her mandibular left second molar (Figure 1). The concept of stratification restoration was explained to the patient and her mother, and photographs were shown to enhance the description. Following treatment acceptance, anesthesia was achieved with a left mandibular block using one carpule of articaine HCl 4% with 1/200,000 parts epinephrine, and the molar region was isolated using the "slit dam" method.8 Initial preparation of the enamel and dentin was accomplished with a water-cooled, thin tapered, No. 170L diamond bur (Figure 2 and Figure 3). In order to consider the location and three-dimensional extent of the caries lesion, the same bur was carefully moved laterally and more deeply, following the course of the carious dentin. As usual in a Class I preparation design, the outline and retention form were determined by the morphology of the tooth and the extent of the lesion. After creation of the outline form, the carious dentin was debrided using a round No. 6 bur at slow speed. In several areas, the lesion had penetrated the tooth more severely, requiring deeper preparation.
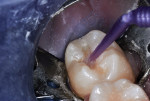
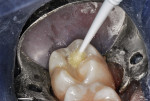
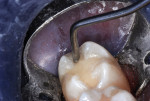
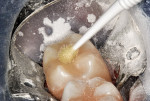
After direct visualization of the preparation from all angles, indirect evaluation using a dental mirror, and an assessment of the tactile feel with a small spoon excavator, the cavity preparation was washed with two 60-second lavages of 5% glutaraldhyde/35% HEMA aqueous solution (Gluma® Desensitizer, Kulzer) using a micro-applicator and then dried with a stream of air (Figure 4). This aids in desensitization of the dentin and disinfection of the preparation.9,10 Next, a thin layer of a resin-modified calcium silicate liner (TheraCal LC®, Bisco) was injected and spread into the deep regions of the preparation (Figure 5).11,12 The liner was hardened with a 20-second exposure to a curing light. To act as a dentin replacement base, an RMGI-type material (ACTIVA™ BioACTIVE-RESTORATIVE™, Pulpdent) was carefully injected (C-R Syringe®, AccuDose® Low Viscosity Tube; Centrix®) to cover the entire surface of the remaining dentin on the pulpal floor as well as on all four axial walls.13,14 After the RMGI-type material was light cured, excess was trimmed away with an inverted cone carbide bur used at slow speed (Figure 6). A large diamond bur was then used at slow speed to roughen the enamel surfaces peripheral to the cavosurface margins (Figure 7). This step enhances the enamel/resin bond.
Next, the preparation and peripheral enamel surfaces were painted with a self-etching resin bonding agent (Adper™ Prompt™ L-Pop™, 3M). The liquid agent was then agitated for 30 seconds with a small tipped applicator (Figure 8). There was no need to be concerned about over-etching the dentin because it had already been replaced with the RMGI-type material. After agitation, the bonding agent was thinned out using a gentle air stream and light-cured for 10 seconds (Figure 9). Alternatively, a traditional etch/rinse/dry/apply bonding agent protocol can be used instead of a self-etching material.
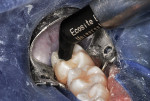
A resin-based composite bulk-fill material (Ecosite Bulk Fill, DMG) was then expressed onto the tooth surface and into the preparation (Figure 10). This new nanofilled, resin-based composite bulk-fill material was chosen because of its unique strengths, high filler load, and easy-to-handle viscosity. In addition, bulk filling saves time when compared with incremental filling, and in a systematic review and meta-analysis, Veloso et al demonstrated "similar clinical performances of bulk-fill and conventional resin composites over a follow-up period of 12 to 72 months."15 Using a non-serrated condenser, the resin-based composite was pressed into all of the corners of the preparation (Figure 11). Next, the bulk of the material was firmly compressed with a large ball burnisher and spread over all aspects of the restorative surface, ensuring that there were no air bubbles incorporated that would become voids after light curing (Figure 12). All of the cavosurface margins were purposely overfilled. The occlusal surface was then photopolymerized for two 20-second exposures (ie, 1,000 mW/cm2) (Figure 13). Because this resin-based composite is a bulk-fill material, it is possible to cure a single increment of up to 5 mm.
After curing, a large, round diamond bur was used at slow speed to sculpt the anatomical form, taking care not to remove all of the bonded material at the overlapping cavosurface margins (Figure 14). The same self-etching resin bonding agent used earlier was then painted over the sculpted, restored surface as a finishing glaze (Figure 15). The mesiolingual cusp of the opposing maxillary second molar was quite pointed, so it was smoothed down with an aluminum oxide finishing disk to prevent "jackhammer-like" impact on the newly restored surface and better distribute the forces during mastication. To complete the restoration, the occlusion was checked to verify that there were no interferences (Figure 16). The patient returned for a 3-month postoperative follow-up appointment and after viewing the photograph, expressed her satisfaction with the result (Figure 17).
Summary
Stratification tooth repair, also known as the "sandwich technique," is a proven, effective, biomimetic method that utilizes "tissue-specific" materials to complete the restoration. In this case, a high-viscosity, resin-based composite bulk-fill material was used as the enamel component. This material was considered to be ideal for this restoration because of its easy handling and exceptional physical characteristics as well as the research that supports successes of resin-based composite bulk-fill materials.
About the Author
Theodore P. Croll, DDS
Cavity Busters
Doylestown, Pennsylvania
Adjunct Professor
Pediatric Dentistry
University of Texas Health Science Center
San Antonio, Texas
Clinical Professor
Pediatric Dentistry
Case Western Reserve School of Dental Medicine
Cleveland, Ohio
Joel H. Berg, DDS, MS
Professor Emeritus
Department of Pediatric Dentistry
University of Washington School of Dentistry
Seattle, Washington
Disclaimer
The authors have no financial interest in any product or company cited in this article and will not receive any remuneration for its preparation or publication.
References
1. Croll TP. Replacement of defective class I amalgam restoration with stratified glass ionomer-composite resin materials. Quintessence International. 1989;20(10):711-716.
2. Bugliarello G. Biomimesis: the road less traveled. The Bridge. 1997;27(3):2-3.
3. Reddy R, Reddy N. Biomimetic approaches for tissue engineering. J Biomater Sci Polym Ed. 2018;26:1-19.
4. Croll TP, Cavanaugh RR, Pedly RD. Posterior resin-based composite restorations: A second opinion. J Esthetic and Restorative Dentistry. 2002;14:(5)303-312.
5. Croll TP. The "sandwich" technique. J Esthet Restor Dent. 2004;16(4):210-212.
6. Croll TP, Cavanaugh RR. Tissue-specific direct application Class II tooth repair: a case report. Compend Contin Educ Dent. 2009;30(9):608-614.
7. Berg JH, Croll TP. Glass ionomer restorative cement systems: an update. Pediatr Dent. 2015;37(2):116-124.
8. Croll TP. Alternative methods for use of the rubber dam. Quintessence Int. 1985;16(6):387-392.
9. Clinicians Report Foundation. Disinfection of tooth preparations-why and how?
Clinicians Report. 2009;2(11):1-2.
10. Christensen R. Dental caries 2018: New insights. Dentistry Today. 2018;37
(11):122-128.
11. Gandolfi MG, Siboni F, Taddei P, et al. Apatite-forming ability of TheraCal pulp-capping material. J Dent Res. 2011;90(Spec Iss A):abstract number 2520.
12. Gandolfi MG, Siboni F, Prati C. Chemical-physical properties of TheraCal, a novel light- curable MTA-like material for pulp capping. Int Endod J. 2012;45
(6):571-579.
13. Ruiz JL, Mitra S. Using cavity liners with direct posterior composite restorations. Compend Contin Educ Dent. 2006;27(6):347-351.
14. Croll TP, Lawson NC. ACTIVA™ BioACTIVE-RESTORATIVE™ material in children and teens. Inside Dentistry. 2018;14(2)(suppl):1-8.
15. Veloso SRM, Lemos CAA, de Moraes SLD et al. Clinical performance of bulk-fill and conventional resin composite restorations in posterior teeth: a systematic review and meta-analysis. Clin Oral Investig. 2018. doi: 10.1007/s00784-018-2429-7.