The Cannabis Conversation
Is your practice having it?
Jackie Syrop
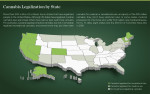
As the number of states that have legalized cannabis (ie, marijuana, weed, pot) for medical and/or recreational purposes continues to grow, the topic is surfacing in conversations at dental practices across the country. The 30 states (see Cannabis Legalization by State) in which cannabis is currently legalized contain a majority of the US population,and 12 additional states will have some form of cannabis legalization on the ballot during 2018.1-3 Nearly 55 million US adults claim to be current cannabis users, which is close to the number of US cigarette smokers (ie, 59 million).3 Attitudes about cannabis are quickly changing: a 2017 Gallup poll showed that 64% of Americans support its legalization-nearly double the figure that did in 2000.1-4 With more states legalizing cannabis, more people are using it. In fact, the population of "heavy users" of cannabis has not only become larger, it has also become older.5
As a result of this phenomenon, nearly all dental professionals can expect to encounter more patients who regularly use cannabis. Therefore, it is more important than ever to understand how cannabis affects oral health as well as its impact on other important areas of dental practice, including treatment planning, taking complete patient medical histories, and obtaining informed consent.
State and Federal Cognitive Dissonance
Despite the fact that most of the states and the District of Columbia have legalized cannabis in some form, US federal law continues to classify marijuana alongside heroin and LSD as a Schedule 1 drug-the most restrictive category, reserved for substances that have "no currently accepted medical use" and a high potential for abuse.5 The federal prohibition of cannabis and its classification as a Schedule 1 drug has led to a critical lack of clinical data about the health effects of cannabis because these designations make it extremely difficult to get approval and funding for cannabis research.5,6 The dearth of reliable data regarding the health effects of cannabis is the main reason why no medical guidelines have been issued by national health organizations. In 2017, The National Academies of Sciences, Engineering, and Medicine concluded that this lack of data is "a significant impediment not only to the scientific understanding of cannabis but also to the advancement of public policy and the nation's overall public health."
As long as cannabis remains classified as a Schedule I drug, cannabis users and clinicians will continue to be part of what TIME magazine terms, "the great pot experiment," in which 1 in 8 adults are conducting their own, mostly recreational, research.6 Because clinicians are largely left to educate themselves about their patients' use of cannabis, dental practitioners around the country have vastly different levels of knowledge and experience regarding its effects.
But dental practitioners can't afford to wait for official guidance on cannabis. "There isn't a dentist in the country who hasn't seen patients who have cannabis in their systems," says Alan S. Budd, DMD, a former assistant professor of restorative dentistry at the Tufts University School of Dental Medicine, who maintains a general and cosmetic dentistry practice in Boston, Massachusetts. People post stories online about smoking cannabis before dental appointments. "By and large, at least among the younger generation, cannabis is increasingly seen as a harmless substance, and if the perception of something is that it's harmless, the freedom to use it is going to continue," notes Budd.
"Cannabis is on the radar, but we are struggling as a profession to establish guidelines," says JoAnn Gurenlian, RDH, MS, PhD, professor and graduate program director in the Department of Dental Hygiene at Idaho State University. "What are the best protocols? Where do we draw the lines? We have very little literature indicating how long it takes for cannabis to clear the system, or how different that process is for men and women, teens, children, or the elderly," she notes. And it's no longer correct to assume that the users of marijuana are mostly teens and children. "I have older patients, some of whom are in their 70s and 80s, who are using all types of marijuana for aches and pains, autoimmune diseases, cancer treatments, seizure disorders, anxieties, and trauma."
A Balancing Act
Opinions and beliefs about cannabis vary greatly among dental practitioners. Cannabis use and its legalization present complex issues that can be seen as having both positive and negative aspects.
On the positive side, cannabis is being used successfully to alleviate the sequelae of many hard-to-treat, chronic conditions, and many medical cannabis users say access to it improves their lives immeasurably. As far back as 1999, the Institute of Medicine reported that substances in cannabis may have a role in the treatment of pain, movement, and memory, even as the agency cautioned about the possible risks associated with its use.7 Today, pain is the number one reason that cannabis is prescribed-especially for neuropathic and malignant pain and chronic pain syndromes.7 "Research shows that marijuana is a great medication for pain control," says Sanda Moldovan, MS, DDS, a periodontist and nutritionist with a focus on natural health who practices in Beverly Hills, California. "For people who need it, there really isn't a better alternative."
In addition, cannabis, particularly cannabis oil, is used to treat severe epilepsy. In fact, the US Food and Drug Administration (FDA) recently approved Epidiolex, the first agency-sanctioned drug containing cannabidiol (CBD) to treat two rare and severe forms of epilepsy.5-8Beyond pain and seizures, cannabis is being used to treat a variety of medical conditions, including the following:
• nausea and vomiting associated with chemotherapy
• glaucoma
• loss of appetite among HIV/AIDS patients
• disturbed sleep
• spasticity associated with multiple sclerosis
• arthritis
• migraines
• Parkinson's disease
• anxiety, depression, and post-traumatic stress disorder
"We sell CBD oil in the office because it is great for people who experience anxiety, seizures, temporomandibular joint pain, bruxism, and insomnia, and it has anti-inflammatory properties," says Moldovan. Marijuana should not be put in the same category as heroin or cocaine, she states, because it is a medicinal substance that has been anecdotally shown to be effective for certain conditions, and research indicates that it contains hundreds of components that could be beneficial for the human body.
As neurosurgeon and CNN's Chief Medical Correspondent Sanjay Gupta, MD, noted in an article addressing US Attorney General Jeff Sessions, cannabis may also be effective at easing opioid withdrawal symptoms in the same way that it helps cancer patients made ill from the side effects of chemotherapy.9 Researchers recently reported an approximately 20% decline in opioid overdose deaths between 1999 and 2010 in states with legalized medical marijuana and functioning dispensaries, and they concluded that broader access to medical marijuana offers people a substitute for powerful and addictive opioids.10 "Chronic substance abusers are at risk for overdosing on an opiate," says Raymond A. Dionne, DDS, MS, PhD, research professor at the Brody School of Medicine at East Carolina University in Greenville, North Carolina. Dionne's 30-year clinical research career has focused on acute and chronic pain and pain management. "Marijuana would probably be a better alternative to an opioid for chronic, intractable pain in states where it has been legalized," he states. "Better the munchies than an overdose."
Concerns about Cannabis
Any discussion about the health effects of cannabis is frustrated by the lack of rigorous clinical data. "There really aren't studies in which cannabis is separated out from tobacco and alcohol," notes Budd. "Many of the chronic effects of cannabis depend on how much someone is using, with what frequency, and at what intensity." (See A Cannabis Primer.)
Among the most serious concerns about cannabis is its effect on young users. Exposure prenatally or during adolescence may affect brain development, causing changes in the connections between neurons in certain regions.11,15 Among those with genetic predispositions to certain mental illnesses, cannabis use may be associated with an earlier onset of mental illness, including schizophrenia, and it may exacerbate the existing symptoms of bipolar disorder. Some research suggests that the average cannabis user is twice as likely as a nonuser to develop a psychotic disorder.11 Approximately 9% of cannabis users become dependent, but that number is closer to 16% if use starts during the teenage years.16 Research suggests that in addition to having short-term effects on cognition, cannabis could potentially alter developing brains, possibly affecting mental abilities and dispositions. In essence, the earlier a user starts, the greater the potential for negative effects.16
Cannabis smoke contains many of the same toxic compounds found in tobacco smoke, including carcinogenic aromatic hydrocarbons,15,17 Smoking cannabis may be associated with an elevated risk of bronchitis and respiratory symptoms.5 "People who use cannabis may not realize that it can be as damaging to their overall health as cigarettes," says Schallhorn. "The combustion products are not healthy. I've told patients who smoke cannabis to consider using edibles." Notably, although tobacco smoking has been proven to kill more than 480,000 US citizens annually, to date, studies have not been able to definitively link chronic marijuana smoking with head, neck, or lung cancer.18-21
Cannabis use has been associated with cardiovascular issues, such as tachycardia and microcirculation disruptions, that can lead to a number of serious conditions, including (but rarely) myocardial infarction and vascular occlusive diseases.15 These cardiac effects are of particular concern for the dental profession because there is a risk that cannabis-induced tachycardia could be prolonged by the administration of local anesthetics containing epinephrine.15,22-24 "In my continuing education classes, I challenge students to consider whether or not it is safe to inject epinephrine into a patient if a comprehensive health history hasn't been taken," says Gurenlian. "The literature has shown that cannabis can have an effect on blood flow and circulation, increasing the heart rate," agrees Dr. Schallhorn. "It is definitely a concern, particularly if patients are using cannabis before an appointment. I don't see it a lot in our practice, but I can imagine that it might be a greater issue among certain patient populations. For example, patients who believe that they can't afford sedation may decide that they're going to use cannabis before the procedure."
Several potentially serious adverse reactions have been associated with cannabis use, including the following15,23-25:
• prolonging/exacerbating tachycardia and hypertension
• potentiating cardiac arrhythmias and respiratory depression under general anesthesia
• increasing the drowsiness caused by some drugs, such as benzodiazepines, codeine, and some antidepressants
• interacting with sedatives, central nervous system depressants, pain relievers, and analgesics
• increasing the risk of bleeding events when taken with aspirin and other nonsteroidal anti-inflammatory drugs, blood thinners, and/or antiplatelet drugs
• affecting blood sugar levels among patients taking diabetes medications
Variable Levels of THC
One of the challenging issues for dental practitioners is the wide variability in tetrahydrocannabinol (THC) levels across, and even within, different forms of cannabis.6,15 There are no simple, office-based tests that can tell a practitioner how much THC patients have consumed or how recently. Consequently, it is not easy to determine whether a patient has recently used cannabis, and many patients are unwilling to report their use. Most people simply don't know how much THC they have in their systems, whether they are smoking or consuming edible cannabis products.In states where medical marijuana has been legalized, packaged marijuana and store-bought edibles are labeled with their THC content in milligrams, but there is a great deal of confusion among users about what the labels mean as well as a lack of regulation regarding the accuracy of these measurements. "Although I have mixed feelings about the legalization of cannabis, one of the things it may do is give people more control over what they are consuming," says Budd. "People may eventually be able to say, ‘I had this mixture, and it contains Xmg of cannabidiol,' but we're not at that point now."
Oral Health Effects of Cannabis Use
Some studies show that cannabis, particularly when smoked, is associated with poor quality oral health.15,21,22 However, frequent users of marijuana may also have high rates of concomitant tobacco use, alcohol use, and recreational drug use as well as poor oral hygiene practices and a lack of regular dental care. Gurenlian notes that some chronic marijuana users have poorer oral health than the general population, including higher rates of decayed or missing teeth, more plaque, and poorer gingival health. "I worry that people who use cannabis tend not to prioritize their oral health-brushing, interdental cleaning, and eating properly. If you are not taking actions to manage interdental biofilm on a regular basis, you're going to have periodontal health problems."
Whether smoked or ingested, cannabis can cause xerostomia-a factor that contributes to a number of oral health conditions, including caries.15 Because THC is an appetite stimulant, cannabis users may consume more cariogenic snack foods, and research indicates that regular cannabis users can have significantly higher numbers of caries than nonusers.15
Leukoedema is more common among cannabis users than nonusers, but it is unclear whether it is associated with the irritants involved (eg, orally inhaled smoke) or the cannabis itself.15 Smoking cannabis is also associated with gingival enlargement, erythroplakia, and chronic inflammation of the oral mucosa with hyperkeratosis and leukoplakia.15 Studies have found higher rates of candidiasis among cannabis users when compared with nonusers, but Candida colonization may simply be a result of the generally poorer oral hygiene among some cannabis smokers.15
Several studies have suggested a direct relationship between cannabis use and periodontal disease, even after adjusting for confounding factors such as cigarette smoking, alcohol use, social status, and other health issues.15,23-25 When compared with nonusers, significantly higher rates of periodontitis were seen among frequent users of cannabis as well as a significantly higher number of sites with pocket depths greater than or equal to 4 mm and attachment loss.7,15 There's more of a correlation between smoking cannabis and periodontal disease than a causal effect, Budd believes, but if he has a patient who is known to have other risk factors, or who is showing a history of periodontal disease, he will tell them that smoking anything is probably going to make it worse.
"I think it's too early to tell," says Moldovan, "but other than dry mouth, which some patients report, we don't really see oral effects directly related to cannabis in our practice." The mouths of cannabis smokers look different than those of cigarette smokers because nicotine shrinks blood vessels and marijuana doesn't. "Some studies have associated marijuana with periodontal disease and cavities, but I believe that those findings are really about oral hygiene," she says. "I don't think there is a direct link between marijuana use and gum disease or cavities. Rather, the connection has more to do with a demographic of the population using it who are paying less attention to oral healthcare and what they eat."
Schallhorn has not seen a significant change in the oral health of her patients since cannabis was legalized in Colorado, but cautions that it is important to consider the patient population she sees: patients who are coming to the periodontist because they are invested in their oral health to begin with and who are trying to minimize their risk factors. Schallhorn is concerned that smoking cannabis could also affect the healing process, so she counsels her patients not to smoke marijuana during the week prior to and for 2 weeks after any oral surgery to minimize any cardiovascular effects that might be present and promote postoperative healing. "There isn't much research on how marijuana smoking affects the longevity of a dental implant," she says, "but I am concerned that if a patient regularly smokes marijuana, he or she could experience increased bone loss around implants and increased risk of failure in the same manner as someone who regularly smokes cigarettes." She sees some mucosal changes (eg, stomatitis, tissues that look hyperkeratotic or inflamed) in patients who report using cannabis frequently, particularly those who are smoking it, but "these are subtle changes," she notes.
Rethinking the Patient Health History
Patients are often reluctant to tell dental practitioners about their cannabis use, even in areas where it has been legalized. "We have to rethink how we take a patient history," Gurenlian states, ending the practice of segregating questions about cannabis from questions about other medications on patient health forms. "If cannabis use is even on the patient history form, we ask about it lower down with the use of other illegal substances, which can make patients feel nervous about answering the question honestly or feel bad about it." Dental professionals have to stop thinking of themselves as the "second cousins" of healthcare. "In dentistry, we want to be so quick with our patients, asking only, ‘Is there anything different in your health?' and then we're done," says Gurenlian. "We believe that dental patients will only fill out a 1-page form, but when they go to a physician, they fill out 20 minutes of forms or fill them out at home and bring them in."
"Patient health records should consist of a review of the dental and medical history as well as social factors, including questions about cannabis use," says Gurenlian. Patients should be assured that they are in a nonjudgmental environment so they feel comfortable telling dental professionals about their cannabis use. Despite the best efforts to reassure patients and get honest answers, patients who use cannabis may simply flat out state that they don't use it. "I go back to the question more than once, offering many opportunities for patients to say they are using cannabis, and very often, they are more honest than you might imagine," notes Gurenlian. To create an environment that encourages full disclosure, she suggests telling patients that: (1) it doesn't matter to you if they use drugs that are legal or otherwise-you're not judging; (2) the information will be kept strictly confidential; and (3) you need to know about cannabis use so you can provide them with excellent care.
Schallhorn's practice changed its health history forms after the Colorado Dental Association suggested adding two new questions about cannabis use.26: (1) Do you or have you used prescribed medical marijuana? If yes, please indicate the condition being treated. If yes, when was the last time you used medical marijuana (orally or inhalation) and (2) Do you or have you used marijuana recreationally? If yes, when was the last time you used recreational marijuana?
"If patients say that they use cannabis, or if I see changes in their oral exam suggesting its use, I talk with them about the potential harmful effects of cannabis. If I see changes that can be signs of using cigarettes or smoking cannabis that are a little concerning, I tell them," says Schallhorn. She assures patients that they are not going to be judged and explains that she evaluates the oral tissues and screens for oral cancer, so it is important to be aware of a patient's risk factors, including cannabis use.
Moldovan is passionate about changing the current medical history forms. She believes that there should be a line added to the history asking if the patient uses cannabis and in what form. The history forms should ask if patients are using nicotine-containing products separately and specify if the tobacco is chewed or smoked. "These questions should be part of the medical history," she advises. "Because otherwise, patients are not going to tell you."
"Dentists need to start asking about cannabis in the health history, and they need to discuss it with their teams as well," Budd concurs. "I don't know what keeps the forms from getting updated more quickly, but in addition to cannabis use, there are a number of other issues for which questions should be added, including sleep-disordered breathing conditions."
"You're always very concerned about patients who may be taking a medication you're not aware of, because you don't know what the formulation is, what the dose is, or how it might interact with the medications that you're going to give them," notes Dionne. "If a dentist inadvertently gives a standard dose of a sedative-type drug to a patient who has already sedated themselves with recreational drugs, there could be dangerous additive effects, and it would be difficult to know how to treat them."
Concerns about Informed Consent
Determining if a patient is under the influence of cannabis is important when considering treatment options and obtaining valid informed consent for plans and procedures. According to the American Dental Association (ADA), informed consent should be the basis for every treatment that doctors propose to perform on patients (ADA, written communication, July 2018).15 "Dentists must obtain informed consent from each patient or from the patient's legal guardian or decision-maker... The ADA recommends carrying out an informed consent process for every patient and having an office policy in place that is referenced and followed in every case (ADA, written communication, July 2018)." There may be legal implications regarding the validity of informed consent with intoxicated patients, especially with irreversible procedures like extractions.15 According to the ADA, the patient should present the most accurate medical history and information to his or her doctor, including current health status and the use of any medications or other substances, which is critical to providing patients with ethical, personalized, high-quality care that maintains or improves their oral health as well as their overall health and well-being (ADA, written communication, July 2018).
Some patients are intoxicated at the time of their office visit.27 Gurenlian sees this much more often now than in past years. Signs of cannabis intoxication include euphoria, hyperactivity, anxiety, tachycardia, paranoia, delusions, and possibly hallucinations.15 Intoxicated users may present with an increased heart rate and other cardiorespiratory effects of cannabis that make the use of epinephrine potentially life threatening.15,24 "Even if patients say they only use CBD, you should still be mindful of respiratory or cardiovascular side effects," Gurenlian cautions. She evaluates if patients have arrhythmia or tachycardia and determines if it is related to using marijuana. "I want to know whether they used marijuana today before the appointment. And if I am concerned about their ability to understand what we are about to do for that appointment, I may choose to reappoint them."
Moldovan has not seen patients coming into her practice who are noticeably impaired. In California, where medical marijuana is legal, many people use cannabis for pain control. "They have a prescription, and most use it in the evening." She notes that there are already patients who come to her office under the influence of tramadol or hydrocodone for back pain. "How is that different? To be able to give informed consent, the patient must be mentally present. If a patient presents for a consultation and he or she is intoxicated from any medications or natural substances that are mind-altering, we are not able to obtain a valid written informed consent, and we become liable for any treatment rendered."
"Informed consent is a very important issue, and the specific dental procedure that will be performed is highly relevant," says Budd. "The typical form asks what medications the patient is taking, but there's no place on the form for every single thing an individual is using that could affect their decision-making. So ultimately, it's incumbent on the dentist to do due diligence and not make the form the be-all and end-all." As a general/cosmetic dentist, Budd does not typically perform oral surgery, but if a patient is having a tooth extracted, he provides an additional informed consent document to sign. The risks inherent in having a tooth extracted are quite different than those associated with receiving a filling because a wound is being created. "By and large, I'm not too concerned about someone who says they smoke pot once in a while-it doesn't really raise a red flag. But I wouldn't extract a tooth from that person without discussing it with them first and trying to ascertain how recently they used it."
A Teaching Moment
When cannabis use is suspected, in addition to performing a comprehensive oral exam and having the patient complete a thorough dental and medical history, the ADA recommends viewing the moment as an opportunity to discuss the potential health consequences and inform the patient of the importance of fluoride, good oral hygiene practices, and healthy snacking.15 Other recommended actions include the following15:
• Emphasize the importance of regular dental visits and oral care.
• Encourage healthy, nutritious snacks over sweet, cariogenic snacks.
• Consider employing preventive measures such as topical fluorides.
• Consider treatment for xerostomia while avoiding alcohol-containing products.
The nation's current epidemic of opioid abuse may be the issue that finally forces the profession to talk about cannabis and develop evidence-based guidelines regarding its use. "We should welcome the opportunity to start with Step 1: having open conversations about reasonable approaches and safe practices," says Gurenlian. "The time is certainly right to have these conversations, and many dentists and hygienists want to learn more, so why not put it on the agenda?"
A Cannabis Primer
Marijuana comes from plants in the genus Cannabis(eg, Cannabis sativa, Cannabis indica). Cannabis plants contain more than 100 known cannabinoids-the active constituents-which interact with neurotransmitters throughout the nervous and immune systems to modulate pain, appetite, and mood and are also involved in brain development and maturation.5 Studies suggest there is an "entourage" effect in that some cannabinoids are only active in the presence of others.
The main cannabinoids of interest are the psychoactive cannabinoid tetrahydrocannabinol (THC), which is responsible for the "high" associated with marijuana use, and cannabidiol (CBD), a non-psychoactive component. CBD modulates the high that users feel, and its antioxidant and anti-inflammatory properties make it an important component of medical marijuana formulations.7,11 The FDA has approved a few prescription forms of synthetic THC (eg, dronabinol) that are used as antiemetics for chemotherapy patients and appetite stimulants for AIDS patients. These medications should not be confused with the synthetic cannabis formulations (ie, "fake weed," K2, Spice) that have been linked to the deaths of users around the country.
Cannabis takes many forms and is consumed in a variety of ways, including the following:
Smoking
This is still the most common method of use. Cannabis is smoked via joints (ie, marijuana cigarettes), pipes, or bongs (ie, water pipes).
"Vaping"
More recently, this method has become popular. Vaping uses a battery-powered vaporizer to heat cannabis or cannabis concentrates at a low temperature, releasing the active ingredients without combustion. Some research suggests that vapor is associated with lower amounts of harmful tars when compared with smoke, and many consider it healthier than smoking, but there is not enough evidence to support this.12
Eating
Cannabis can be cooked into food or other "edibles," such as brownies, lollipops, gummies, candies, cookies, granola bars, etc.13
"Dabbing"
This increasingly popular method involves inhaling the vapor or smoke produced by a dab of marijuana concentrate, which produces a more intense high than other forms of using cannabis.14 There are concerns that dabbing may expose users to elevated levels of toxins when compared with other methods.
Applying topicals
Cannabis oil has been infused into lotions, sprays, oils, and creams that are absorbed through the skin. Tinctures (ie, alcohol solutions) containing cannabis oil are also available.
References
1. State Marijuana Laws in 2018 Map. Govering the States and Localities Website. https://www.governing.com/gov-data/state-marijuana-laws-map-medical-recreational.html Updated March 30, 2018. Accessed August 20, 1018.
2. Geiger A. About six-in-ten Americans support marijuana legalization. Pew Research Center Website. https://www.pewresearch.org/fact-tank/2018/01/05/americans-support-marijuana-legalization/. Published January 5, 2018. Accessed August 20, 2018.
3. Ingraham C. 11 charts that show marijuana has truly gone mainstream. The Washington Post Website. https://www.washingtonpost.com/news/wonk/wp/2017/04/19/11-charts-that-show-marijuana-has-truly-gone-mainstream/?noredirect=on&utm_term=.b56b3e0ae537. Published April 19, 2017. Accessed August 20, 2018.
4. McCarthy J. Record-High Support for Legalizing Marijuana Use in U.S. GALLUP Website. https://news.gallup.com/poll/221018/record-high-support-legalizing-marijuana.aspx?version=print. Published October 25, 2017. Accessed August 2, 2018.
5. National Academies of Sciences, Engineering, and Medicine. 2017. The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research. Washington, DC: The National Academies Press. https://doi.org/10.17226/24625.
6. Barcott B, Scherer M. The great pot experiment. TIME. 2015;185(19):38-45.
7. Yao SG, Fine JB. Consumption of cannabis and effects on periodontal oral health. California Dental Assoc J. 2017:45(9):475-481.
8. U.S. Food & Drug Administration. FDA approves first drug comprised of an active ingredient derived from marijuana to treat rare, severe forms of epilepsy. FDA Website. www.fda.gov/newsevents/newsroom/pressannouncements/ucm611046.htm. Updated June 25, 2018. Accessed August 19, 2018.
9. Gupta S. Dr. Sanjay Gupta to Jeff Sessions: Medical marijuana could save many addicted to opioids. CNN Website. https://www.cnn.com/2018/04/24/health/medical-marijuana-opioid-epidemic-sanjay-gupta/index.html. Updated April 24, 2018. Accessed October 4, 2018.
10. Powell D, Pacula RL, Jacobson M. Do medical marijuana laws reduce addictions and deaths related to pain killers? J Health Econ. 2018;58:29-42.
11. Lawton G. Medical cannabis: What you really need to know. New Scientist Website. https://www.newscientist.com/article/2174448-medical-cannabis-what-you-really-need-to-know/ Updated July 27, 2018. Accessed September 19, 2018.
12. Loflin M, Earleywine M. No smoke, no fire: what the initial literature suggests regarding vapourized cannabis and respiratory risk. Can J Respir Ther. 2015;51(1):7-9.
13. Barrus DG, Capogrossi KL, Cates SC, et al. Tasty THC: promises and challenges of cannabis edibles. Methods Rep RTI Press. 2016;2016:10.3768/rtipress.2016.op.0035.1611.
14. Nir SM. Chasing bigger high, marijuana users turn to "dabbing." New York Times Website. https://www.nytimes.com/2016/05/13/nyregion/chasing-bigger-high-marijuana-users-turn-to-dabbing.html. Published May 12, 2016. Accessed September 19, 2018.
15. American Dental Association.Cannabis: Oral Health Effects. ADA Website. www.ada.org/en/member-center/oral-health-topics/cannabis. Updated January 22, 2018. Accessed August 20. 2018.
16. National Institute on Drug Abuse. Is marijuana addictive? National Institute on Drug Abuse website. https://www.drugabuse.gov/publications/research-reports/marijuana/marijuana-addictive. Updated June 1, 2018. Accessed October 9, 2018.
17. Barcott B. Weed the People. The Future of Legal Marijuana in America. New York, NY: Time Books, 2015.
18. Rosenblatt KA, Daling JR, Chen C, et al. Marijuana use and risk of oral squamous cell carcinoma. Cancer Res. 2004;64(11):4049-4054.
19. Aldington S, Harwood M, Cox B, et al. Cannabis use and cancer of the head and neck: case-control study. Otolaryngol Head Neck Surg. 2008;138(3):374-380.
20. The Oral Cancer Foundation Staff. Study: Smoking marijuana found non-carcinogenic. OCF Website. https://oralcancernews.org/wp/study-smoking-marijuana-found-non-carcinogenic/ . Published November 2014. Accessed August 21, 2018.
21. Meier MH, Caspi A, Cerdá M, et al. Associations between cannabis use and physical health problems in early midlife. A longitudinal comparison of persistent cannabis vs tobacco users. JAMA Psychiatry. 2016;73(7):731-740.
22. Cho CM, Hirsch R, Johnstone S. General and oral health implications of cannabis use. Aust Dent J. 2005;50(2):70-74.
23.Legalization of marijuana. What dentists need to know. CDA Essentials. 2017;4(6): 29-32. https://www.cda-adc.ca/en/services/essentials/2017/issue6/29/#zoom=z. Accessed August 20, 2018.
24. Feuerstein JB, Reimers N, Lerman MA, et al. What every dentist should know about cannabis. J Massachusetts Dental Soc. 2017:66(3)20-23.
25. Portillo KM, Sanderson TR, Gurenlian JR. Oral health care for marijuana users. Decisions in Dentistry.2018;4(3): 41-44.https://decisionsindentistry.com/article/oral-health-care-marijuana-users/. Accessed August 20, 2018.
26. Pereira M. Colorado Marijuana Law-time to adjust your health history questions! Colorado Dental Association Website. https://cdaonline.org/news/latest-news/coloradomarijuanalawhealthhistoryquestions. Published February 19, 2014. Accessed August 18, 2018.
27. Grafton SE, Huang PN, Viera AR. Dental treatment planning considerations for patients using cannabis. J AM Dent Assoc. 2016;145(5):354-361.