Placing Posterior Direct Composite Restorations
Using a compatibly engineered universal adhesive and nanohybrid composite reduces complexity
Mark Kleive, DDS
As the demand for posterior direct composite restorations increases, clinicians will continue to face ongoing challenges to minimize the potential risks of failure associated with these treatment options. From shrinkage stress and marginal leakage to postoperative sensitivity and tooth fractures, many of the complexities associated with posterior direct composite restorations can be resolved when techniques are properly performed using appropriately formulated restorative materials.
Due to the physical properties of available composite materials, placing direct restorations in the posterior region has often involved technique-sensitive protocols, which have affected how clinicians adapt materials to preparation walls, shape and sculpt the materials, and finish and polish them. Fortunately, recently introduced products that have been engineered to work together are enabling dentists to provide highly esthetic, wear-resistant, and strong restorations that will function predictably for many years.
Case Report
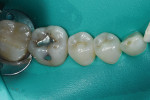
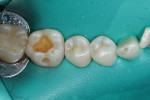
A 55-year-old male patient presented with a failing occlusal amalgam restoration and recurrent decay at the margins of tooth No. 19 (Figure 1). After a local anesthetic was administered, tooth No. 19 was isolated with a rubber dam, and the defective restoration and recurrent decay were removed. The preparation was then cleaned, rinsed, and lightly air-dried (Figure 2).
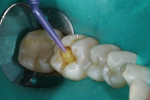
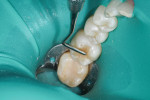
Next, a selective-etch protocol was performed to ensure the highest bond strength to the prepared tooth substrates.1 Following etcing, an 8th generation, one-bottle universal adhesive bonding agent (G-Premio BOND™, GC America) was applied precisely and allowed to wet the preparation for 10 seconds without the need for scrubbing (Figure 3). The adhesive was then air-dried for 5 seconds to quickly evaporate the solvent, after which it was light cured for 10 seconds. This universal bonding agent's compatibility with all etching techniques, extended working time of 5 minutes, low film thickness, and low pH provided maximum versatility.
To line the preparation floor, a layer of flowable composite (G-ænial™ Universal Flo, GC America) in shade A1 was placed and light cured. Highly filled flowable composites such as this have demonstrated comparable clinical effectiveness to conventional composites in posterior restorations.2
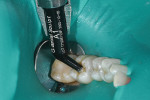
To begin building the restoration, a 2-mm increment of a light-cured, universal nanohybrid composite (G-ænial Sculpt®, GC America) in shade A1 was placed directly into the preparation using a single-dose unitip while maintaining steady pressure (Figure 4). This highly radiopaque, non-sticky, and packable universal nanohybrid composite was selected based on the ease with which it can be shaped and adapted to preparations, as well as its ability to sculpt anatomy without slumping. As this increment was shaped and light cured, care was taken to keep the curing light as close to the composite surface as possible.
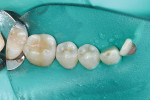
After a second 2-mm increment of the same composite shade was placed, sculpted, contoured (Figure 5), and light cured, the anatomical details of the restoration were finalized. This composite's barium glass nanofillers enhance finishing and polishing; therefore, rough finishing only required the use of a bur, and an ideal polish and highly esthetic luster were easily achieved (Figure 6).3 Due to the composite's self-shining/polishing effect, the initial polish achieved in the restoration would increase in the mouth with daily tooth brushing.4
After the finishing and polishing were completed, the occlusion was checked and the rubber dam was removed. A chameleon effect that blended the restoration with the surrounding tooth structure was observed and attributed to the optical properties of the selected composite.
Conclusion
When dentists are faced with the need to use direct composite in the posterior region, selecting restorative materials that have been specifically engineered to work together can enable them to efficiently and predictably place highly esthetic and wear-resistant restorations.
References
1. Helvey GA. Adhesive dentistry: the development of immediate dentin sealing/selective etching bonding technique. Compend Contin Educ Dent. 2011;32(9):22,24-32,34-5.
2. Kitasako Y, Sadr A, Burrow MF, et al. Thirty-six month clinical evaluation of a highly filled flowable composite for direct posterior restorations. Aust Dent J. 2016;61(3):366-373.
3. Pala K, Tekçe N, Tuncer S, et al. Evaluation of the surface hardness, roughness, gloss and color of composites after different finishing/polishing treatments and thermocycling using a multitechnique approach. Dent Mater J. 2016;35(2):278-289.
4. Lai G, Zhao L, Wang J, et al. Surface properties and color stability of dental flowable composites influenced by simulated toothbrushing. Dent Mater J. 2018. doi: 10.4012/dmj.2017-233.