Digitally Driven, Surgically Assisted Orthodontics
Using a 3D printed guide facilitates a less complex, safer corticotomy procedure
Daniel Domingue, DDS, FAAID, DABOI, DICOI | Cory Glenn, DDS | Baron Grutter, DDS
After reviewing the literature on surgically assisted orthodontics, it becomes apparent that there are many different techniques with different trade names that are all centered around the same objectives, including the facilitation of faster tooth movement to shorten treatment times, increase patient compliance, and enhance post-orthodontic treatment stability.1,2 One common fundamental theme found among the varying contemporary clinical techniques is the use of a non-guided surgical protocol (ie, full thickness tissue flaps, grafting, selective decortication,3-6 suturing to obtain primary closure), which requires advanced surgical skills and knowledge of surgical protocols.
Furthermore, moving mandibular incisors can prove to be difficult and has a high rate of relapse in conventional orthodontics.7,8The technique described in this article is intended to reduce the surgical learning curve and lower the cost while also increasing accuracy for any practitioner. This new method helps eliminate relapse, increases the predictability of treatment, and accelerates tooth movement by 2× to 2.5× when compared with conventional methods.
Presentation
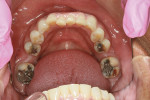
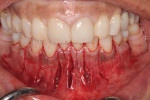
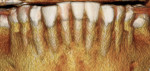
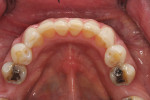
A 54-year-old female patient presented to the office with a chief complaint of wanting straighter teeth (Figure 1). Due to an upcoming familiy function, she wanted the shortest possible treatement time, but could not afford the expense of Invisalign treatment. Her medical and social history were uneventful, and an evaluation confirmed that she had no parafunctional habits (eg, bruxism, tongue trust, lip biting, etc). Following the initial assessment, it was decided that the movement of her crowded lower incisors would be ideally achieved with fabricated clear aligners; however, a supplemental procedure would be needed for the treatment to be completed in time for her event.
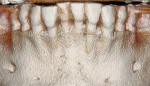
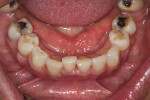
Based on the fact that the literature on surgically assisted orthodontics commonly reports that it is safe, effective, has a low incidence of relapse, and results in shorter treatment times, the decision was made to develop an accurate workup using available digital technology that has not yet been utilized in this manner. Given the close proximity of the roots of the lower incisors (Figure 2), performing this type of corticotomy freehand could lead to irreversible issues and possibly permanently damage the patient's natural teeth. In addition, limited funding prevented the use of advanced surgical grafting required for periodontally accelerated osteogenic orthodontics or the use of the corporate entity Invisalign.
To address these concerns, a new technique was developed using a digitally designed corticotomy guide and a series of custom fabricated clear aligners that could predictably move teeth both quickly and effectively-and all at a lower cost to the patient and dentist.
Obtaining Data
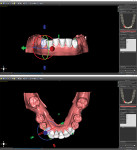
A cone-beam computed tomography (CBCT) scan (PreXion 3D, PreXion, Inc.) of the upper and lower jaws was obtained. This DICOM file was then imported into the treatement planning software (Blue Sky Plan®, BlueSkyBio) as a new project. Next, a vinyl polysiloxane impression was taken of the patients' full lower arch, and a stone model was poured. This model was scanned, and the impression DICOM data was then imported into the planning software and meshed together with the DICOM data of the lower jaw.
Surgical Guide Creation
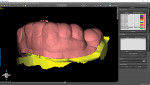
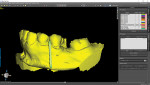
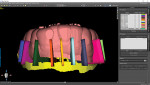
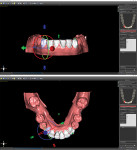
The fabrication of the corticotomy guide was completed by first creating a "generic guide" on the digital model in the planning software. The surgical guide function is typically used for the creation of implant drill guides, but in this case, because no guide tubes were incorporated, the design was just a basic, 3-mm uniform thickness shell that sat over the arch (Figure 3). This provided the foundation for the corticotomy guide. A free 3D modeling application (Meshmixer, Autodesk, Inc.) was then used to create a 15 mm x 15 mm plane measuring 1-mm thick to correspond to the 1-mm width of the piezoelectric surgery tip (Figure 4). After this shape was saved and imported into the planning software, it was duplicated several times and precisely positioned in the surgical guide between the roots of the individual teeth where the corticotomies were to be performed (Figure 5). Because the planes represented the positions where the piezoelectric surgical bone cuts would be made, the plane shapes were checked in all views to ensure that no portion impinged into the tooth roots (Figure 6). Next, the data for the surgical guide and each of the planes were exported and reopened within the 3D modeling application to facilitate a Boolean subtraction. In this manner, the planes were subtracted from the data for the guide, leaving 1-mm slots where the piezo tip could be inserted (Figure 7). Once all of the planes were subtracted, the data was imported back into the planning software to verify the accuracy (Figure 8), and the guide was printed (Objet30 3D printer, Stratasys) (Figure 9).
Aligner Design and Fabrication
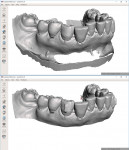
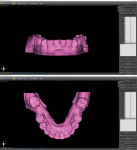
The optically scanned model of the lower arch was opened in the 3D modeling application to evaluate the integrity of the model, trim off any unnecessary data from the border using the cut tools, and repair any flaws using the analysis repair tool. After the model was corrected and smoothed, the teeth were assessed for degree of rotation, alignment, torqueing, and inclination or retraction. To ensure the correct rotation of the teeth, it is best to create "buttons" on the facial aspects of the canines. This facilitates positive seating and helps predict the planned intrusion of the incisors without resulting in unseating of the aligner. The STL file for the newly refined model was then exported to the planning software for aligner design (Figure 10).
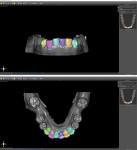
Using the STL file, a new project was started in the planning software's orthodontic module. The positions of the teeth were designated to help the software identify each individual tooth and generate approximate margin tracings. Next, the margins of the teeth were refined, and the software segmented each tooth for individual movement (Figure 11). The teeth were then aligned to their final desired positions, and the rate of movement (ie, weekly, bi-weekly, monthly) was selected (Figure 12 and Figure 13). Using known averages of acceptable tooth movement and sequencing, the software then ran its algorithm and determined the sequential steps of alignment for review. Once approved, the software created individual models for each progressive stage of treatment (Figure 14). After identification labels were digitally embossed onto the models and an orthodontic report for the progressive movement of each tooth was exported and attached to the patient's chart, the STL files for each of the models were ready to be exported for 3D printing.
The progressive models were printed (MoonRay S 3D printer, SprintRay Inc) and then washed for 5 minutes at a time in a series of alcohol baths to remove any uncured resin. Following washing, the models were light cured under a UV light until fully hardened.
To fabricate the aligner trays, the models were individually placed on a positive pressure thermal-forming machine (MiniSTAR®, Great Lakes Orthodontics) with a 1.0-mm (ie, 0.040-in) plastic sheet (ACE® Plastic, Essix). While still on the models, the aligners were trimmed with a tray saw, allowing them to be removed. The edges were then polished smooth with abrasive buff polishers, and the aligners were readied for patient delivery.
Surgical Procedure
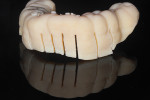
Local anesthesia was achieved by infiltration with septocaine (ie, 1:1,000 epi) in the buccal vestibule around the teeth involved in the osteotomy (ie, teeth Nos. 20 through 29). The surgical guide was seated over the mandibular teeth and checked to ensure that there was no soft-tissue impingement or other interferences that would prevent it from seating fully. Bite blocks were placed to vertically open patient's bite and make sure that the guide was seated evenly on both sides. Using a 15C scalpel blade, vertical incisions were made through the slots on the facial aspect of the guide, sounding to bone (Figure 15). The guide was then removed to check the accuracy of the cuts in between the teeth, ensuring that the soft-tissue incisions went completely through to the bone and that there was no remaining soft tissue attached that would prevent piezoelectric surgical cuts. Once the accuracy was verified, the surgical guide was returned to the mouth with both props and the soft-tissue cuts were used to confirm proper seating. Using a piezoelectric surgery unit (PIEZOSURGERY®, Piezosurgery Incorporated) in the "bone" setting, a titanium nitride-coated principal micro-saw tip (Insert OT7, Piezosurgery Incorporated) was placed in the slots of the surgical guide to initiate cuts between the teeth. The initial cut was made through the cortex, slowly moving the tip up and down until each tooth was segmented. Following this, the guide was removed and each site was checked to verify the depth and length of the cuts. Full thickness flaps were not needed to accommodate the cuts in the soft tissue, and no soft tissue was reflected from the bone in between the cuts. Given the low-level of room for error, a postoperative CBCT image was taken to confirm the accuracy of the cuts and that no damage had been sustained by the teeth (Figure 16).
Orthodontic Tray Delivery and Use
The patient was told to start wearing the trays immediately, switching out each tray every third day. She was given enough trays to self-deliver during this time period and asked to return in 2 weeks to verify that proper tooth movement was occurring. The patient was recalled for several similar follow-up visits until delivery of the final tray. After the final tray appointment, the patient expressed her satisfaction with the results of the treatment.
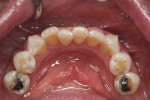
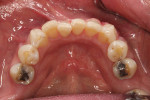
Four months after the surgical procedure, a final CBCT scan was taken and compared to both the initial and postoperative CBCT images to confirm healing and that no bone loss had occurred. Photographs were taken before and at various stages of the clear aligner therapy to monitor tooth movement (Figure 17 through Figure 20).
Conclusion
The initial orthodontic digital workup determined that, without surgical intervention, this patient's treatment would require 16 aligners, switched every other week for a total of 8 months from start to finish. Thankfully, the results confirmed that a shorter treatment time could be achieved with a surgical intervention and that these results are very predictable. In the before and after images, the results of tooth alignment, the speed of alignment, the accuracy of the surgical guide, and the precision of the aligners all speak for themselves. Finally, the lower cost for the patient and doctor, the fast workup and quick turnaround time to initiate treatment, and the ability to alter the course of treatment within a short period of time provide additional reasons to implement this technique into your practice. Given the close proximity of the roots and minimal room for human error in this case, using a digitally designed, 3D printed surgical guide to facilitate the corticotomy prevented damage to the natural teeth and nerves and provided a much easier postoperative recovery time for this patient with a reduced chance of complications. The accuracy of the guide also precludes the need for advanced surgical procedures/techniques, such as those used in periodontally accelerated osteogenic orthodontics,4 thus lowering the level of complexity, which benefits both the patient and the clinician.
About the Authors
Daniel Domingue, DDS, FAAID, DABOI, DICOI
Private Practice
Lafayette, Louisiana
Cory Glenn, DDS
Private Practice
Winchester, Tennessee
Baron Grutter, DDS
Private Practice
Gladstone, Missouri
References
1. Hassan AH, Al-Fraidi AA, Al-Saeed SH. Corticotomy-assisted orthodontic treatment: review. Open Dent J. 2010;13(4):159-164.
2. Cano J, Campo J, Bonilla E, et al. Corticotomy-assisted orthodontics. J Clin Exp Dent. 2012;4(1):e54-e59.
3. Kumar S, Srivastava A, Sharma A, et al. Periodontal intervention in speedy orthodontics-a case report. J Clin Diagn Res. 2016;10(1):ZD15-16.
4. Amit G, JPS K, Pankaj B, et al. Periodontally accelerated osteogenic orthodontics (PAOO) - a review. J Clin Exp Dent. 2012;4(5):e292-296.
5. Alghamdi AS. Corticotomy facilitated orthodontics: Review of a technique. Saudi Dent J. 2010;22(1):1-5.
6. Hasssan AH, Al-Saeed SH, Al-Maghlouth BA, at al. Corticotomy-assisted orthodontic treatment. A systematic review of the biological basis and clinical effectiveness. Saudi Med J. 2015;36(7):794-801.
7. López-Areal L, Gandia JL. Relapse of incisor crowding: a visit to the Prince of Salina. Med Oral Patol Oral Cir Bucal. 2013;18(2):e356-361.
8. Little RM. Stability and relapse of mandibular anterior alignment: University of Washington studies. Semin Orthod. 1999;5(3):191-204.