Don’t Get Lost in Translation
Multidisciplinary treatment for congenitally missing teeth
Salvatore Lotardo, DDS, AAACD
It is always important to consider multiple treatment options, as there can be many ways to effectively treat the same case. Clinicians often have a bias toward treatment plans that favor their skill sets or ones for which they have had prior experience. As a general dentist, it is important to develop a wide knowledge base encompassing all of the disciplines so that all options are considered when treatment planning. Even if clinicians decide not to perform certain treatments, they need to know what is possible, including the limitations and advantages of potential alternatives. This allows them to fully inform patients and guide them into making a decision that best meets their needs and desires.
Historically, orthodontic education at the undergraduate level has been minimal. This has led to an underutilization of orthodontics as an adjunct to restorative treatment. Fortunately, the trend toward multidisciplinary dentistry is on the rise, which is leading to less invasive treatments with improved outcomes.
Case Report 1
Presentation
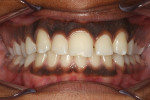
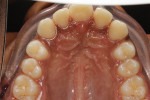
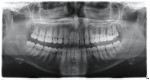
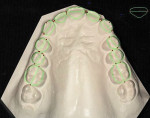
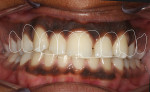
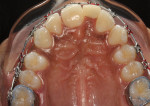
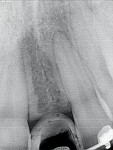
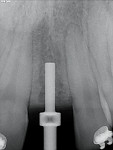
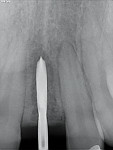
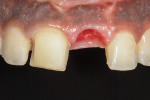
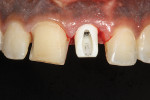
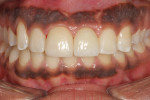
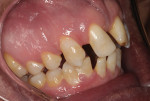
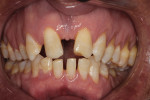
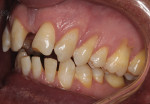
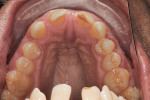
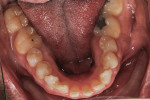
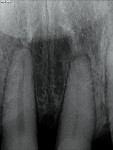
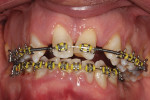
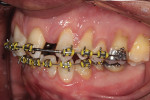
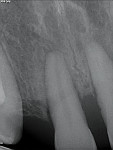
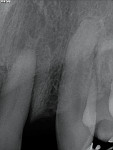
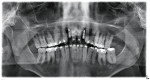
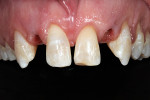
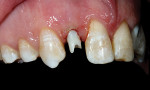
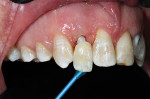
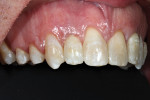
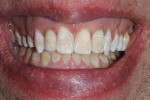
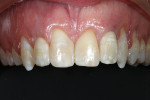
A 19-year-old female patient presented with the chief complaint of not being happy with her smile (Figure 1 through Figure 4). After a comprehensive examination, the patient was found to have a congenitally missing tooth No. 9, macrodontia of tooth No. 8, and a Class II molar relationship on the right side with minor spacing and rotations throughout the arch.
When treatment planning complex cases, dentists should ask themselves: Can this case be treated without preparing or extracting any teeth? If so, how can that be accomplished? Although there are multiple ways that this case could be treated, the most conservative option involves using orthodontic treatment to open space so that the missing tooth can be replaced with a dental implant. To address the patient's goals, any other treatment would require either significant preparation of the teeth or extraction of one or more teeth.
It's one thing to devise a plan and another to know if it is attainable. In orthodontic-restorative combination cases, clinicians need to know the feasibility of moving teeth into the desired positions as well as the potential resultant occlusal and esthetic outcomes. The goal is “translation,” whereby the tooth moves bodily (ie, both crown and root) in the direction of the force applied. When correctly performed, this will not only reposition the teeth within the arch, but also minimize tipping in preparation for implant placement.
Orthodontics offers many techniques and tools to analyze tooth size and arch length (Figure 5).1 Typically, these types of analyses serve as aids in predicting and treating tooth size and arch length discrepancies in adolescent malocclusions. In adult patients presenting with both orthodontic and restorative needs, analyzing and establishing these relationships can be more challenging.
Coming from a restorative perspective, the use of smile design software (Smile Designer Pro, Tasty Tech Ltd.) allows for the incorporation of an orthodontic prediction into the esthetic restorative outcome (Figure 6). Most smile design programs and other photography-based software applications use photographs calibrated with referenced measurements and then manipulate them using templates or custom outlines to determine tooth proportions and positons.2The resulting blueprint can then be used to guide restorations. Similarly, these functions can be used to guide orthodontic treatment and set up teeth and arch forms to maximize restorative outcomes.
The goal of smile design is not to idealize every case, but rather to systematically evaluate a smile and identify elements that would enhance the patient's esthetics if corrected. In this case, important elements to be addressed include symmetry, central dominance, and tooth proportions.
Arguably, one central incisor could fit the criteria for symmetry, as is sometimes done in orthodontic cases on the lower arch, but that obviously will not work in the upper arch for this case.3 Symmetry among the maxillary central incisors is more important than among any other contralateral teeth and therefore, is a primary goal of treatment.4
Central dominance means that the maxillary central incisors are the focal point of the smile. In most cases, lack of central dominance (ie, the centrals do not dominate in size and shape over the adjacent laterals) is the issue. Although this case would be considered to have excess central dominance, correction is still of high importance.
Tooth proportion is twofold, involving both the proportion of the individual tooth in terms of its width-to-height ratio and its relative proportion to the adjacent teeth. A typical unworn central incisor has a width-to-height ratio of 76%, average crown widths ranging from 8.4 to 9.3 mm, and average lengths ranging from 10.4 to 11.2 mm.5,6 In this case, the lone central not only exhibits a larger than average width at 10.5 mm but also a height equal to its width, resulting in a ratio of 100% that makes for a square and less-than-esthetic proportion.
Determining the relative proportions begins with the establishment of an ideal central, and then the proportions of the remaining incisors are derived from that measurement. In this case, because the central is too prominent, the relative proportions must be determined by working backwards from the canines and the laterals. Historically, cosmetic dentists have used a variety of formulas to calculate relative proportions, but the most well-known is the “golden ratio” or “golden proportion.”7Smile design templates are often based on such proportional formulas, but the software allows for customization, which gives the dentist an opportunity to make adjustments by visually determining the desired relative proportions. Because all of the measurements are calibrated, the new goal proportions can be factored into the final treatment plan.
Using the existing size of the canines and laterals as a starting point, the smile design revealed that two 8.5-mm wide centrals would look the most natural. So, if the macrodontic central (ie, No. 8) could be reduced in width to 8.5 mm, and space could be created to allow for a symmetrically sized implant-retained crown in the No. 9 position, an ideal esthetic outcome could be achieved. However, because the tooth size/arch length analysis predicted that only 6.0 mm of space creation was realistic, achieving ideal proportions using this method would be unlikely. Either a compromise in esthetics or a more aggressive tooth preparation would have to be decided upon at that stage of the treatment.
After the findings, limitations, and treatment options were discussed with the patient, she consented to a plan involving orthodontic treatment to open space for the placement of an implant to replace missing tooth No. 9 and a porcelain veneer to narrow the width of tooth No. 8.
Orthodontic Phase
Fixed appliance therapy was initiated to level and align both arches. Correction of the rotated posterior teeth was planned to create space by aligning the narrower dimension of the teeth to the arch form. Along with closing any existing diastemas, this would create the space needed for an implant in the No. 9 position. Utilizing a combination of chains, nickel titanium closing and opening coils, and archwire expansion, space was redistributed to the left central incisor area. For esthetics, a crown shell can be attached to the wire and modified periodically to keep up with the space as it opens (Figure 7 and Figure 8).
Opening space orthodontically may result in crown tipping, which can leave the roots of adjacent teeth converging into the prospective implant site. When this occurs, the resultant clinical inter-crown space may be deceptive and not indicative of pure bodily movement. If the mechanics for translation are correct, the crown and the root move together, and the correct pathway for implant placement is assured.8 When possible, overcorrection of the root angulations by tipping the roots more divergently than necessary allows for an easier and safer implant placement. Once the implant is placed and integrated, the adjacent roots can be moved back into proper alignment.
Surgical/Implant Phase
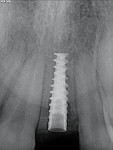
Upon completion of the active phase of orthodontic therapy and confirmation of space and root angulations, an immediately loaded implant was planned. There are many advantages to computer-guided implant placement; however, in this case, the orthodontic appliances were to be left in place, so a freehand technique was planned(Figure 9 through Figure 12).9
Following administration of local anesthesia, a tissue punch was performed, and an osteotomy was created for the placement of a 3.5 x 13 mm implant (Nobel Active, Nobel Biocare). The implant was positioned to maximize the esthetics while respecting the biologic parameters necessary for successful integration.
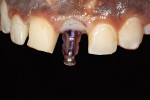
An immediate screw-retained provisional was fabricated using a temporary abutment and an acrylic crown form.10 Even in situations where the screw access would lie outside of the incisal edge or the buccal edge, a screw-retained provisional is still preferred because it improves a clinician's ability to shape the contours necessary to develop a correct soft-tissue emergence profile.11
Restorative Phase
The orthodontic fixed appliances should remain in place until implant integration is confirmed.12 At subsequent visits, the soft-tissue profile is improved by adjusting the contours of the provisional until the proper, final emergence profile is achieved. At 12 weeks after implant placement, the brackets and bands are removed, and the final prosthetic plan is devised.13
At this point, the decision was made to complete the treatment plan despite the fact that there would be a slight size discrepancy between the two central incisors. To make tooth No. 8 and No. 9 symmetrical, the width of No. 8 would have to be reduced by 2.5 mm. However, this amount would encroach upon the cervical width at the osseous crest. One solution to correct this would be to restart orthodontic treatment and extrude the larger tooth. Moving the narrower portion of the tooth incisally in this manner would allow for a narrower overall restoration and a more symmetric gingival outline form relative to the final restoration in position No. 9. Unfortunately, this was not considered earlier, and at this time, the patient would not consent to any additional treatment beyond the originally planned veneer and the subsequent compromise in symmetrical widths.
Tooth No. 8 was prepared for a lithium disilicate veneer (IPS e.max®, Ivoclar Vivadent) while reducing the interproximal width as much as possible. Next, a custom impression coping was created for the No. 9 implant to capture the soft-tissue profile created by the provisional. A simple indirect technique utilizing a stone mounted replica and a transfer of the provisional contour via a polyvinyl siloxane impression material was used (Figure 13 through Figure 16).14 Using the custom, closed-tray impression coping, a definitive full-arch impression was made, ensuring that the soft-tissue profile was transferred accurately to the final model (Figure 17 and Figure 18). The fabrication of the veneer for tooth No. 8 and the zirconia abutment and all-ceramic full crown for the implant in position No. 9 was prescribed. The shade was communicated to the laboratory via photography along with a preparation shade guide and a porcelain shade guide. The screw-retained provisional was replaced, and a bis-acryl provisional was fabricated using a putty matrix technique for tooth No. 8.15
At the seating appointment, the veneer was tried in along with the custom abutment and the implant crown. The esthetics were approved by the patient. After the custom abutment was torqued down to 30 Ncm(Figure 19), the restorations were silanated and bonded with a resin cement (RelyX™, 3M ESPE). Next, final polishing was performed, occlusal adjustments were made, and overlay retainers were fabricated and delivered. The patient was satisfied with the final results of treatment (Figure 20 and Figure 21).
Case Report 2
Presentation
A 41-year-old male patient presented with the chief complaint of “excessive space between his teeth.” After a comprehensive examination, the patient was found to have congenitally missing maxillary lateral incisors and generalized gingival recession (Figure 22 through Figure 27). Additional orthodontic problems identified included an anterior open bite, upper and lower arch size discrepancies, spacing issues, a right side posterior cross bite, and a left side “scissor bite.”
A treatment plan involving comprehensive orthodontics, including orthognathic surgery to fully correct the occlusion and other skeletally related problems, was presented to the patient. He declined any treatment that would involve surgery, so a limited orthodontic compromise solution was developed to address his main esthetic concerns. Although not ideal, compromise treatment can be beneficial and is justified provided that the patient's health, function, and esthetics are not jeopardized by such treatment. For this case, the treatment plan that was presented and accepted involved fixed orthodontics to open space for the congenitally missing laterals, close the midline diastema, and improve the occlusion, followed by implant placement for missing teeth Nos. 7 and 10.
As in the previous case, smile design software was used to determine the proper tooth proportions and subsequently, the space needed to create an esthetic smile. With a width-to-height ratio of 72%, the proportions of the preexisting centrals were deemed too narrow. Therefore, the decision was made to use composite to reshape tooth No. 8 and No. 9 to improve their proportions. Reshaping the mesial contours would also lead to a more natural midline diastema closure at the end of treatment. After translating the teeth and redistributing the space, properly proportioned laterals would become possible through implant restorations.
Orthodontic Phase
Tipping proved difficult to control; therefore, during the course of treatment, adjustments in mechanics were needed to ensure proper root alignment (Figure 28).To counteract the tipping movements associated with space closure via chain or open coil, the brackets were purposely misaligned. Because space opening can be deceptive, root angulation and bodily movement must be confirmed (Figure 29 through Figure 33). After 18 months, the upper and lower teeth were aligned, the occlusion was improved, and the case was set up for implant placement.
Surgical/Implant Phase
Upon completion of the active phase of orthodontic therapy and confirmation of space and root angulations, implant therapy was planned as described in the previous case.
Following administration of local anesthesia, a tissue punch was performed, and osteotomies were created for the placement of two 3.0 x 12 mm implants (Tapered Plus, BioHorizons®) using a free hand approach (Figure 34). A delayed loading protocol was followed in this case. Although immediate loading has been shown to be highly successful, in a case such as this where the benefits of immediate load are not critical to the outcome, delayed loading is preferred.16,17
Restorative Phase
After 12 weeks, the implants were uncovered. Provisionals were fabricated on temporary abutments using hollow crown forms and acrylic. During the next 8 weeks, the provisionals were shaped to mimic the cervical contours needed to develop ideal emergence profiles in the soft tissue(Figure 35 through Figure 36).11When the definitive soft tissue architecture was established, final impressions utilizing customized impression copings were completed.
After the final zirconia abutments were torqued down and the cement-retained IPS e.max crowns (Ivoclar Vivadent) inserted (Figure 37 through Figure 39), composite restorations were completed on teeth Nos. 8 and 9 to improve the proportions and contours and develop midline papilla. The patient expressed satisfaction with the treatment outcome (Figure 40 through Figure 42).
Conclusion
As with most cases, those presented here could be effectively treated using a variety of different treatment plans. The restorative dentist's role in diagnosing and presenting treatment options requires a good understanding of multidisciplinary dentistry. In a time when patients' expectations for esthetic treatment are high, often, restorative solutions alone will be inadequate. When treatment planning, especially in complex cases for which conservative options are desired, orthodontic considerations are vital to success.
Acknowledgment
The author would like to acknowledge LK Dental Studio and Morphology Dental Studio for their work on cases 1 and 2, respectively.
About the Author
Salvatore Lotardo, DDS, AAACD
Bella Smiles
Riverhead, New York
References
1. Schirmer UR, Wiltshire WA. Manual and computer-aided space analysis: a comparative study. Am J Orthod Dentofacial Orthop. 1997;112(6):676-680.
2. McLaren EA, Garber DA, Figueira J. Compend Contin Educ Dent. 2013;34(10):772-776.
3. Kokich VG, Shapirio PA. Lower incisor extraction in orthodontic treatment. Four clinical reports. Angle Orthod. 1984;54(2):139-153.
4. Finlay S. AACD Guide to Accreditation Criteria: Contemporary Concepts Smile in Design. Madison, WI: American Academy of Costmetic Dentistry; 2014.
5. Magne P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89
(5):453-461.
6. Chiche GJ, Pinault A. Esthetics of anterior fixed prosthodontics. Chicago: Quintessence; 1994. p. 97-113.
7. Ward DH. A study of dentists' preferred maxillary anterior tooth width proportions: comparing the recurring esthetic dental proportion to other mathematical and naturally occuring proportions. J Esthetic Restorative Dent. 2007;19(6):324-339.
8. Nanda R, Tosun Y. Biomechanics In Orthodontics. Chicago, Ill.: Quintessence Publishing; 2010:87-88.
9. Dula K, Mini R, van der Stelt PF, Buser D. The radiographic assessment of implant patients: decision-making criteria. Int J Oral Maxillofac Implants. 2001;16(1):80-90.
10. Weber HP, Morton D, Gallucci GO, et al. Consensus statements and recommended clinical procedures regarding loading protocols. Int J OralMaxillofac Implants. 2009; 24(Suppl):180-183.
11. Saito H, Chu SJ, Reynolds MA, Tarnow DP. Provisional restorations used in immediate implant placement provide a platform to promote peri-implant soft tissue healing: a pilot study. Int J Periodontics Restorative Dent. 2016;36(1):47-52.
12. Worthington P, Lang BR, Rubenstein JE. Osseointegration in Dentistry: An Overview. 2nd ed. Hanover Park, Il: Quintessence Publishing; 2012.
13. Buser D, Mericske-Stern R, Bernard JP, et al. Long-term evaluation of non-submerged ITI implants. Part 1: 8-year life table analysis of a prospective multi-center study with 2,359 implants. Clin Oral Implants Res. 1997;8(3):161-172.
14. Polack MA. Simple method of fabricating an impression coping to reproduce peri-implant gingiva on the master cast. J Prosthet Dent. 2002;88(2):221-223.
15. Sneed WD, Knight JS. Simple technique to fabricate provisional restorations for porcelain veneers. J Esthet Restor Dent. 2001;13(2):115-119.
16. Tarnow DP, Emtiaz S, Classi A. Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants. 1997;12(3):319-324.
17. Ostman PO. Immediate/early loading of dental implants. Clinical documentation and presentation of a treatment concept. Periodontol 2000. 2008;47:90-112.