What Are the Indications and Contraindications for Use of SDF in Anterior Teeth?
Theodore P. Croll, DDS | Travis M. Nelson, DDS, MSD, MPH | Jeanette K. MacLean, DDS
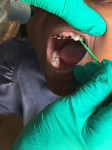
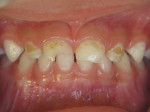
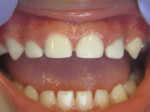
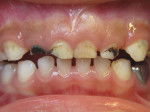
Theodore P. Croll, DDS: Hermann Prinz cited the use of silver nitrate or “lunar caustic” dating back to 1846, because it “practically stops the progress of the carious process.” Today, the question of how to use 38% silver diamine fluoride (SDF) to treat anterior teeth in children is easy to answer: SDF is the best way to manage anterior caries lesions in some children and a cosmetically terrible way to treat certain other children.
Considerations for the use of SDF include the parents' preference (Some parents have no objection to the black discoloration whereas others are horrified by it and sometimes suggest they would prefer extractions.); the child's age, medical status, comfort, and safety (Would traditional restorative treatment require sedation or anesthesia?); the child's ability to cooperate; and the severity of the caries lesions (Is there pulpal involvement precluding SDF?).
The use of SDF can function as a delaying tactic, followed by traditional restorative measures when the child is better able to safely and comfortably tolerate such care. For example, in cases of early childhood caries in babies and toddlers, SDF can be an ideal, albeit unattractive, stopgap measure. Another consideration is the age of a patient. Children whose primary teeth exhibit radiographic evidence of impending exfoliation can certainly benefit from SDF. When finances are a concern, SDF applications can provide rapid, pain-free treatments that are much less expensive when compared with traditional restorative treatment.
All of these considerations result in the need for complex decision-making for dentists and parents when treatment planning. To optimize success, each child's treatment should be formulated by factoring in all of these influences and perhaps others.
Sociological considerations are also important. In parts of the world where dental caries is endemic and oral hygiene care is lacking or non-existent, SDF can be a blessing for patient populations that have no other type of routine dental treatment available to them.
Personally, I had not given much thought to the use of SDF in my pediatric dentistry specialty office until several years ago, and since then, I have discovered many indications for its use both in primary and permanent teeth.
Travis M. Nelson, DDS, MSD, MPH: SDF provides an effective method for treating caries in teeth that do not have symptoms of irreversible pulpitis or infection. Primary anterior teeth are easily isolated, so caries arrest is more predictable there than in any other area. This makes SDF a great option for the treatment of early childhood caries. My skillset includes the use of SDF, interim therapeutic (ART/glass ionomer) restorations, pharmacologic behavior guidance, and definitive esthetic restorations. Under the right circumstances, all of these treatments have their place. My approach is to provide families with options and allow them to make the decision. For example, I rarely recommend the option of sedation/general anesthesia to the parents of a child with only a few caries lesions. Similarly, when a child presents with a badly broken dentition or abscessed teeth, I frequently recommend definitive restorative care.
Patients and caregivers need to know that: (1) although SDF treatment can be quite effective, teeth that have been treated with SDF can still continue to decay, develop pulp pathosis, and become abscessed; (2) rather than restoring form and function, SDF only stops disease progression; (3) teeth treated with SDF can have a compromised appearance and may fracture; (4) the accompanying stain that indicates arrest can be very noticeable in anterior teeth; and (5) SDF must be reapplied at least twice a year until the tooth exfoliates or is restored.
In our clinic, we require that every parent sign a detailed consent form, which includes color photographs of SDF treated lesions, before their child receives SDF treatment. Although some proponents claim that most caregivers readily accept the dark discoloration, many parents want no part of it. Today's parent often prefers more esthetic restorative options. As evidence to this trend, consider the dramatic growth in composite and zirconia options for primary teeth.
I have found that some parents are very opposed to treatment with sedation or general anesthesia, so they are quite happy with SDF. Others can't stand the idea of the SDF staining, so they opt for anterior crowns or fillings, which may necessitate some form of sedation. It's not an easy choice, and I am often surprised by what the family decides. Consider for yourself: if it was your child or grandchild, what would you want?
Jeanette K. MacLean, DDS: To put it simply, the only time SDF cannot be used in the anterior is when there is pulpal involvement. The answer to the question of when it should be used is more complicated. Circumstances and reasons for why parents in my practice choose SDF in the anterior for their children (which is frequently) include an understanding of the benefits of treatment with medicine versus surgery; a desire for quick, easy, and painless treatment; the need to avoid or delay sedation, general anesthesia, or a traditional restoration; concerns related to the costs and risks of traditional treatment; lack of concern regarding esthetics; appropriate age and exfoliation timing; and interest in a silver modified atraumatic restorative technique (SMART).
Often, the greatest barriers to SDF treatment are the dentists themselves. While we focus on esthetics, we can lose sight of the underlying disease—caries—and its etiology. The more that I study caries, the more I am reminded that health comes before beauty—and that healthy is beautiful.
Furthermore, there is beauty in the simplicity of minimally invasive treatment modalities, such as SDF and SMART, especially when working with young children.
I do educate patients that, even with SDF, it may still be necessary to restore the tooth. However, SDF manages the bacteria that contributed to the decay, and it is an excellent option when combined with SMART. Multiple studies have shown that bonding is not negatively affected by SDF treatment.
After 12 years in practice, I can honestly say that having the ability to provide effective minimally invasive treatment options to my patients has renewed my passion for the profession and given me hope for its future.
Theodore P. Croll, DDS, maintains a private practice in Doylestown, Pennsylvania, and is an affiliate professor in the Department of Pediatric Dentistry at the University of Washington School of Dentistry.
Travis M. Nelson, DDS, MSD, MPH, is a clinical associate professor in the Department of Pediatric Dentistry at the University of Washington School of Dentistry and an attending dentist at Seattle Children's Hospital.
Jeanette K. MacLean, DDS, is a diplomate of the American Board of Pediatric Dentistry and a co-owner of Affiliated Children's Dental Specialists in Glendale, Arizona.