Veneering a Resin-Based Composite Crown
Improve color without transitioning to full-coverage porcelain
Theodore P. Croll, DDS
A patient whose diminutive maxillary left lateral incisor was built up to full natural coronal dimensions and appearance using bonded resin-based composite (RBC), unexpectedly whitened her teeth using carbamide peroxide bleaching strips.1,2 As a result, the color of the resin-based composite no longer matched that of the newly whitened adjacent teeth. Rather than replace the entire crown, the decision was made to apply a veneer with a lighter shade RBC.
Treatment
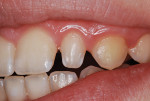
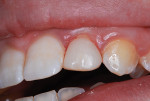
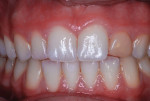
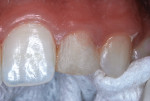
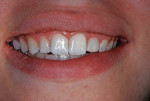
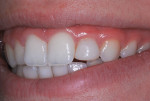
In March of 2011, the diminutive maxillary left lateral incisor in a 14-year-old girl was restored to normal contours with a bonded resin-based composite crown, using the method reported by Croll and Bond (Figure 1 and Figure 2).3 Filtek™ Supreme Ultra Restorative in A2 Body shade (3M ESPE) was used for the coronal “build-up.” Approximately 30 months later, the patient presented for her usual 6-month recall appointment with generalized whitening of her teeth. She had successfully used over-the-counter carbamide peroxide whitening strips; however, the RBC crown had retained its original shade, which appeared yellower than the rest of the anterior teeth (Figure 3).
Rather than removing the bonded crown, the decision was made to reduce the labial surface and place a veneer of lighter-colored RBC. Without the need for local anesthesia, treatment was rendered using the following eight steps:
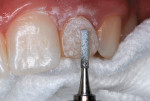
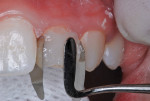
1. A surface layer of 1 mm to 1.5 mm of resin-based composite was cut down using a cylindrical coarse diamond bur at slow speed (Figure 4).
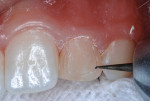
2. An area in the gingival region of the labial surface was denuded of bonded RBC to expose new enamel for acid etching (Figure 5).
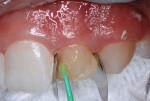
3. Using an inverted cone bur, two semi-circular grooves were cut in the RBC surface (Figure 6).
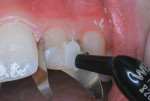
4. Strip-T stainless steel anterior matrices (DENOVO Dental) were placed, secured only by the tight contacts (no wedging was required), and the entire labial surface was saturated with Adper™ Prompt™ L-Pop™ Self-Etch Adhesive (3M ESPE). The liquid adhesive was agitated with a small brush for 30 seconds, but the curing light beam was not applied until the first layer of RBC was compressed upon the surface (Figure 7).
5. A thin layer of Filtek™ Supreme Ultra in White Body shade was expressed upon the tooth surface and compressed into place with a flat metal instrument. Care was taken to ensure that the retentive grooves were completely filled with RBC. After the first layer was photopolymerized, an additional, thicker layer of RBC was applied (Figure 8) and pressed into place (Figure 9). The RBC was then hardened with a total of 60 seconds of light exposure (1,200 mW/cm2).
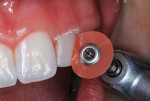
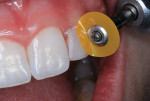
6. The surface was sculpted using high speed finishing burs, followed by additional finishing and polishing using aluminum oxide disks (Figure 10 and Figure 11).
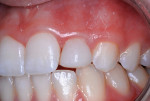
7. The resurfaced RBC crown is shown immediately after treatment (Figure 12) and 7 months later (Figure 13).
8. The patient was photographed 32 months after renewed labial veneering with whiter material, which was 61 months after the original resin-based crown was placed (Figure 14).
Discussion
The RBC crown was originally designed to be out of contact with the mandibular incisor and canine tooth. This position matched the bite relationship of the right lateral incisor and did not influence the appearance of her smile. Unlike ceramic crowns used to restore diminutive lateral incisors in older teenagers and adults, RBC crowns are more prone to fracture, especially under the constant incisal impact of mastication and bite closure. Therefore, the less contact experienced by the crown, the better the outcome. In retrospect, the mesio-incisal corner could have been made slightly longer without risking excessive incisal impact during function. The patient was exceptionally pleased with the new lighter shade of the tooth and had no concerns about the tooth length discrepancy when she was shown photographs.
Aged-cured RBC does not bond well to newly placed resin-based composite, so grooves were cut for mechanical retention, and some enamel in the gingival third of the crown was exposed for new acid etch resin retention. It was not necessary to remove all of the A2 Body shade RBC because the White Body shade was opaque and thick enough to mask the residual material left from the original layer.
Although the best long-term treatment for diminutive lateral incisors in the adult years is precision-fit, full-coverage with porcelain, in the author’s experience, well-placed RBC crowns can last a decade or more.4,5 The patient and her parent were advised that, when this RBC crown required replacement, a ceramic crown would be the next type employed.
An important lesson learned from this case is that patients and parents should be queried about their desire to bleach teeth before resin-based composites are placed on permanent anterior teeth.
Disclaimer
Dr. Croll has a merchandising agreement with Denovo and receives royalties for Strip-T sales.
References
1. Donly KJ, Donly AS, Baharloo L, Rojas-Candelas E, Garcia-Godoy F, Zhou X, Gerlach RW. Tooth whitening in children. Compend Contin Educ Dent. 2002;23 (1A):22-28.
2. Donly KJ. The adolescent patient: special whitening challenges. Compend Contin Educ Dent. 2003;24 (4A):390-396.
3. Croll TP, Bond J. Resin-based composite coronal augmentation of diminutive lateral incisors: an update. Compend Contin Educ Dent. 2006;27(10):546-550.
4. Croll TP. Bonded composite resin crown restoration without enamel reduction. Quintessence Int. 1987;18 (11):753-757.
5. Croll TP, Bullock GA. Bonded resin-based composite crown restoration of diminutive lateral incisors. Compend Contin Educ Dent. 2002;23(6):550-559.
About the Authors
Theodore P. Croll, DDS
Private Practice
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry UW School of Dentistry
Seattle, Washington
Adjunct Professor
Department of Pediatric Dentistry, UT Health Science Center
San Antonio, Texas
For more information, contact:
Denovo Dental
800-854-7949
https://www.denovodental.com