You must be signed in to read the rest of this article.
Registration on AEGIS Dental Network is free. Sign up today!
Forgot your password? Click Here!
Treating Dental Trauma
Managing the esthetics and protecting pulpal vitality
Mark L. Cannon, DDS, MS
For the patient, the experience of dental trauma can be both distressing and costly. The most immediate concern is always esthetics, usually followed by financial considerations and time constraints. Because treatment only repairs the damage (ie the dentition does not heal and enamel does not grow back), the financial costs will continue to escalate over time. Trauma to the dentition may also result in pulpal pathology, the onset of which can potentially occur years after the initial event. Endodontic procedures may be time consuming and are considered by many patients to be a major unplanned expense. Unfortunately, exposed pulp from fractured teeth can be extremely uncomfortable, and patients typically require immediate pain relief. For the dental practitioner, emergencies rarely time themselves to fit within the schedule, but the treatment rendered still needs to be of the highest standard. The advent of resin-based light-cured calcium silicate materials has significantly improved the outcomes, both esthetic and pulpal, for dental trauma patients. The ease of placement and quick application provided by these new materials allows the dental practitioner to treat even the most complicated trauma with ensured success.
Case Presentation
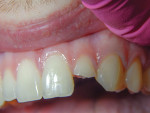
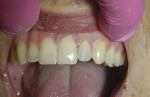
A 19-year-old male patient presented for emergency treatment after sustaining a hockey stick injury to his upper left lateral incisor (Figure 1). The trauma had occured approximately one week earlier, but due to academic time constraints and the patient’s apparent pleasure with his “red badge of courage,” treatment was delayed until maternal influence was brought to bear.
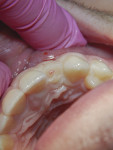
After radiographic examination, anesthesia was administered (20% benzocaine topical and 1.8 cc Septocaine infiltration), and the loose tooth fragment was removed. At this time, a diagnosis of complicated crown root fracture was confirmed. The exposed pulp had grown into a pulp polyp, which is a sign of continued vitality and an indicator of functional pulpal stem cell activity (Figure 2).1
Placement of a rubber dam was attempted, but the palatal tang of the clamp repeatedly intruded into the fracture area and could have impeded proper restoration. An alternative placement onto the palatal tissue pulled the tissue over the fracture area, also impeding complete restoration, so the rubber dam could not be used.
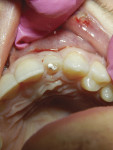
The pulp polyp was surgically amputated with a sharp spoon excavator and then refined with a No. 330 carbide bur in a high-speed handpiece using gentle application. Next, a 3% sodium hypochlorite (VistaDent) dampened cotton pellet and the application of TheraCal LC® (BISCO) were used to obtain hemostasis and disinfection (Figure 3). TheraCal LC is a light-cured, resin-based, hydrophilic dicalcium and tricalcium silicate material that promotes pulpal vitality and dentin bridge formation.2
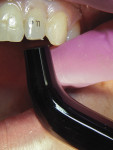
After the TheraCal LC was cured, the tooth was etched using 32% Uni-Etch® with BAC etchant (BISCO) and thoroughly rinsed. Next, ALL-BOND UNIVERSAL® adhesive (BISCO) was applied in two coats and light-cured. A pre-fitted incisor clear crown form was filled with a suprafilled resin composite (Estelite Sigma Quick, shade A1) and then placed on the fractured tooth (Figure 4). After light curing, the crown form was removed and the restoration was polished ((Figure 5).
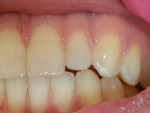
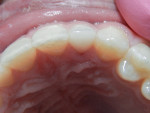
The patient attended standard preventive follow-up visits, and the tooth has remained asymptomatic (Figure 6 and Figure 7). Although the restoration has been performing quite well, the patient and guardian were informed that further treatment would be necessary for the fractured incisor, especially considering the circumstances involving the game of hockey. In addition, the necessity of mouth guards and facial protection was repeatedly discussed.
Several studies have reported that TheraCal LC can induce apatite formation by releasing calcium ions and by maintaining an alkaline pH that is inductive for mineralization.3-5 Although there are other calcium-releasing, silicate-based dental materials, they all require significantly more time to apply and fail to provide the minimum mechanical properties necessary to support the restoration. Previously recommended procedures, such as the placement of MTA or calcium hydroxide pastes, left the restoration totally undermined because the pastes offer no adhesive qualities or mechanical resistance to occlusal forces. All of these pastes also demonstrated a propensity to dissolve, leaving a space for microleakage and bacterial invasion.6
This case presentation provides an excellent example of a clinical situation, which could arise for any dental professional at any time, that is best treated with the use of a light-cured, resin-based dicalcium and tricalcium silicate, such as TheraCal LC.
References
1. Attar A, Eslaminejad MB, Tavangar MS, et al. Dental pulp polyps contain stem cells comparable to the normal dental pulps. J Clin Exp Dent. 2014;6(1):e53-e59.
2. Cannon M, Gerodias N, Viera A, Percinoto C, Jurado R. Primate pulpal healing after exposure and TheraCal application. J Clin Pediatr Dent. 2014;38(4): 333-337.
3. Gandolfi MG, Siboni F, Prati C. Chemical-physical properties of TheraCal, a novel light-curable MTA-like material for pulp capping. Int Endod J. 2012;45(6): 571-579.
4. Gandolfi MG, Siboni F, Taddei P, et al. Apatite-forming ability of TheraCal LC pulp capping material. Oral presentation at: International Association of Dental Research (IADR); March, 2011; San Diego, CA.
5. Menon NP, Varma BR, Janardhanan S, Kumaran P, Xavier AM, Govinda, BS. Clinical and radiographic comparison of indirect pulp treatment using light-cured calcium silicate and mineral trioxide aggregate in primary molars: A randomized clinical trial. Contemp Clin Dent. 2016;7(4):475-480.
6. Hilton TJ. Keys to clinical success with pulp capping: a review of the literature. Oper Dent. 2009;34(5): 615-625.
About the Author
Mark L. Cannon, DDS, MS
Founder, Senior Partner
Associated Dental Specialists of Long Grove
Long Grove, Illinois
Diplomate, American Board of Pediatric Dentistry