Atraumatic Extraction of Mandibular Third Molars
Preventing iatrogenic damage to the inferior alveolar and lingual nerves
Loris Prosper | Nicolas Zunica
Inferior alveolar nerve and lingual nerve lesions are feared complications when extracting mandibular third molars. Iatrogenic injury of the inferior alveolar or lingual nerves can lead to legal issues because of sensory disturbances involving the chin, lower lip, gums, and tongue. However, improved diagnostic and surgical techniques have considerably decreased the prevalence of these complications. What follows is a description of a diagnostic and therapeutic methodology aimed at limiting surgical complications of inferior third molars, starting with an accurate diagnosis followed by the use of minimally invasive surgical instruments.
Instruments and Methodology
When removing an impacted or semi-impacted mandibular third molar, the extraction technique is extremely important in order to prevent damage to the surrounding anatomical structures, such as the inferior alveolar nerve, lingual nerve, and periodontium of the second molar. The surgical instruments used are of paramount importance.
In the case that follows, an innovative instrument, the mechanical periotome Luxator LX (Directa Dental, www.directadental.com), was used to perform a mandibular third molar extraction. The instrument cuts the Sharpey’s fibers surrounding the tooth between cement and alveolar bone by luxating the periodontal ligament.
Case Presentation
A 22-year-old woman in good health presented to our clinic reporting pain in tooth No. 17 and spreading through the whole lower arch.
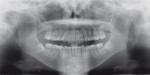
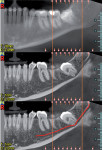
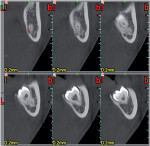
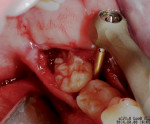
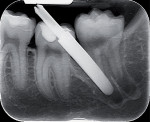
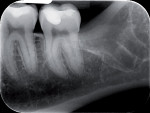
The first panoramic picture shows compression of the mandibular nerve that touches the lower roots of tooth No. 17—physical inclusion of the mucosa and partial bone inclusion in close correlation with the inferior alveolar nerve (Figure 1). Physical examination showed edematous and erythematous mucosa distal to tooth No. 18. No sensibility alteration in the emiarch concerned. A second x-ray showed the position of the inferior alveolar nerve at the distolingual apex as confirmed by CT (Figure 2 and Figure 3).
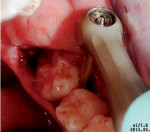
The patient was given anesthesia and a plexus nerve block with a 2% vasoconstrictor. A pouch flap was made. We made an intrasulcular incision at tooth No. 18 and a releasing incision distal to the same. The releasing distal incision must run at a 45º angle to the second molar and in its first part, it is at full-thickness and has a partial-thickness ending. This incision avoids the risk of dissecting the lingual nerve and is the junction of the flap. After skeletonizing the jaw and placing a tongue protection, the Sharpey’s fibers were cut using the mechanical periotome Luxator LX following the tooth circumference and luxating the periodontal ligament (Figure 4 and Figure 5). The tooth was subsequently extracted using an elevator without luxating the surrounding tissues and, above all, with no damage to the mandibular nerve.
Thanks to its controlled reciprocating movement, Luxator LX penetrates the space that lodges the periodontal ligament (0.15 mm to 0.38 mm) and separates the fiber bundle in the least traumatic way for the tooth. The gentle vertical movement applied to the periodont does not cause neural trauma. We managed to perform the extraction with no tissue damage and most importantly, no damage to the mandibular nerve.
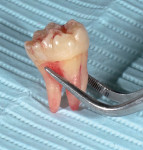
The periapical x-ray (Figure 6) shows how the blade—detached from the contra-angle to facilitate the x-ray—penetrates into the alveolus, facilitating tooth removal. Figure 7 shows the absence of root rests. The extraction was performed without sectioning/dividing the tooth. Figure 8 shows that the tooth was extracted in one piece. No traumatic operations to search for root rests were needed.
The alveolus was cleaned, washed with cold physiologic solution, and sutured with silk thread 4/0. The edge could be sutured, enabling the patient to recover without postoperative pain. The suture stitches were removed 7 days post-procedure. The patient reported a good postoperative recovery with slight pain during the first 3 days mitigated by common pain medication.
It was recommended that the patient use an innovative toothpaste in gel with a mix of humectant and antibacterial substances (ie, cetylpyridinium chloride, triclosan, essential oils) in technologically innovative microcapsules, enabling the patient to significantly lower periodontal plaque and bleeding. Its medium-low RDA (+/-30) is less abrasive on natural tooth and restorative material.
The dental hygienist will focus on reducing plaque close to the postoperative recovery areas, detect poor home hygiene, and promptly intervene to correct them. Professional dental hygiene sessions are extremely important to remove bacteria around the tooth, preferably with glycine powder to preserve the health of gingival tissues (AIR_FLOW®, EMS, https://new.ems-company.com). Final polishing is extremely important to leave a smooth surface, as a rough surface will be more receptive for bacteria. A silica-based polishing paste with a low RDA, such as ProphyPaste CCS Yellow RDA 40 (Directa Dental) is recommended.
Conclusion
Mandibular third molar extractions are undoubtedly associated with neural injury risks that can cause temporary or permanent discomfort for the patient and legal actions for the dentist. A thorough preoperative diagnosis is mandatory and complication factors, such as age and anatomy (ie, depth of impaction and presence of overlying ramus bone), need to be taken into account. The surgical approach used is of paramount importance to minimize tissue damage and neurosensory impairment. The Luxator LX proves to be a valid tool in surgical extractions, allowing minimal trauma and significant reduction of postoperative discomfort.
Loris Prosper
Professor
G. D’Annunzio University
Chieti, Italy
Professor, Dental Prosthetics
Vita-Salute San Raffaele University
Milan, Italy
Nicolas Zunica
Technician/Hygienist
Milan, Italy
For more information, contact:
Directa Dental
203-491-2273