Identifying and Treating Associated Systemic Factors of Occlusal Disease
Obstructive sleep apnea and gastroesophageal reflex evaluation
DeWitt C. Wilkerson, DMD
The term occlusal disease is used to described excessive tooth wear that has been caused by abrasion (eg, malocclusion, bruxism, toothpaste) and/or erosion (eg, chemical damage, low pH). Some cases of abrasion can be caused by bruxism resulting from airway obstruction, such as sleep apnea.1-3
Tooth erosion is commonly associated with the significantly low pH changes caused by gastroesophageal reflux (Figure 1).4,5 The term laryngopharyngeal reflux (LPR) is used when acids travel to the upper airway. Dentists should ask patients about signs and symptoms of sleep-disordered breathing (such as snoring, tiredness upon waking, excessive sleepiness during daytime hours, and difficulty concentrating) when tooth wear signs of bruxism are present.6 Dentists should ask patients about signs and symptoms of gastric reflux (such as heartburn, regurgitation, excessive burping or nausea, a feeling of stomach fullness or bloating, and upper abdominal pain and discomfort) when tooth wear signs of erosion are present. It is noteworthy that “silent reflux” is also a common finding, where the patient is unaware they have active reflux.7 Clinical identification of bruxism activity and obstructive sleep apnea (OSA) can be evaluated using home sleep testing (HST), which can measure biologic functions such as nasal and oral airflow, respiratory effort, heart rate, and oxygen levels in the blood while sleeping.
Case Presentation
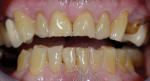
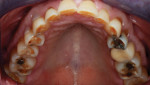
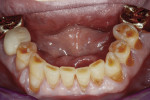
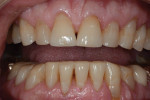
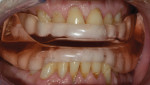
A 67-year-old man presented with severe occlusal disease as a result of advanced abrasion and erosion on all of the teeth (Figure 2 and Figure 3), as well as tired eyes, snoring, and sinus problems. His medical history revealed a high risk for both OSA and gastric reflux. The patient was sent home with a home bruxism/sleep monitor for an evaluation of sleep bruxism, OSA, and central sleep apnea (CSA).
The results of the home testing revealed both severe sleep bruxism and a severe apnea hypopnea index (AHI) of 55.4 (severe > 30). The case was reviewed and diagnosed by a board certified sleep physician.
The Koufman Reflux Symptom Index7 is a useful written questionnaire/tool for screening the presence of GERD. A gastroenterologist evaluated the patient in this case.
The standard protocol for diagnosed severe OSA is the nightly use of a positive-airway pressure (PAP) device. This patient was subsequently entered into a pilot study utilizing an interim trial bruxism/sleep apnea oral appliance. The appliance is designed to disclude all posterior teeth, thus reducing elevator muscle forces, as well as anteriorly reposition the mandible, approximately 60% of maximum protrusive, in an attempt to open the airway in the throat/epiglottis region.
The patient was instructed to wear the appliance every night for 7 days. After one week, the overnight home study was repeated while wearing the oral appliance. The results showed a dramatic reduction in bruxism activity and the AHI dropped from a severe 55.4 to a mild apnea-hypopnea level of 11. These were both remarkable improvements. The heart rate activity was also significantly lower and the oxygen desaturations were markedly reduced.
Intra-thoracic negative pressure created by upper airway occlusion may induce reflux. Although studies to date have not found a specific relationship between such an obstructive event and an episode of gastroesophageal reflux, they have shown that the patients had excessive acid contact time.8 Reflux has also been associated with an acidic diet.7
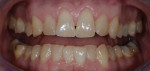
The patient’s definitive occlusal therapy included restoration of the damaged teeth and occlusal equilibration in centric relation, providing appropriate anterior guidance (Figure 4 and Figure 5).
A definitive anterior repositioning sleep apnea appliance was subsequently fabricated and titrated (Figure 6). His bruxism activity has remained minimal and the AHI level has remained below 10. Gastric reflux can be well controlled through a combination of keeping the airway patent during sleep and a modified alkaline diet.7
Conclusion
The focus in dentistry for the clinical diagnosis and treatment of occlusal disease is expanding to identify and treat possible associated systemic factors. Because abrasion can be caused by bruxism resulting from airway obstruction, one of these associated factors that needs closer consideration when patients present with severely worn teeth is sleep disordered breathing or sleep apnea. When the patient’s health history and general examination indicate such, home sleep testing, or a referral for a polysomnogram, should be pursued to ascertain the possible clinical relationship of the patient’s bruxism activity and tooth wear to jaw movements driven by airway obstruction and the primary “flight or fight” effort to obtain oxygen.
Disclosure
The author has no relevant financial relationships to disclose.
References
1. Ohayon MM, Li KK, Guilleminault C. Risk factors for sleep bruxism in the general population. Chest. 2001;119(1);53-61.
2. Lavigne GJ. Sleep Medicine for Dentists A Practical Overview. Chicago, Illinois: Quintessence Publishing Co, Inc. 2009.
3. Oksenberg A, Arons E. Sleep bruxism related to obstructive sleep apnea: the effect of continuous positive airway pressure. Sleep Med. 2002;3(6):513-515.
4. Miyawaki S, Tanimoto Y, Araki Y, et al. Association between nocturnal bruxism and gastroesophageal reflux. Sleep. 2003;26(7):888-892.
5. Ranjitkar S, Kaidonis JA, Smales RJ. Gastroesophageal reflux disease and tooth erosion. Int J Dent. 2012;2012:479850. Epub 2011 Dec 12.
6. The Official STOPBang Tool Website. https://www.stopbang.ca. Accessed June 1, 2016.
7. Koufman J. Dropping Acid: The Reflux Diet Cookbook & Cure. 1487th edition. Delran, New Jersey: Simon & Schuster. 2010.
8. Ing AJ, Ngu MC, Breslin AB. Obstructive sleep apnea and gastroesophageal reflux. Am J Med. 2000;108 Suppl 4a:120S-125S.
About the Author
DeWitt C. Wilkerson, DMD
Private Practice
St. Petersburg, Florida