Minimally Invasive Treatment with a 940-nm Diode Laser
Photocoagulation of a lingual hemangioma
Michael K. Koceja, DDS
Laser use continues to expand into the medical and dental fields, and patients are increasingly seeking out such treatment because it is perceived as less invasive and less traumatic than traditional methods. Laser surgical treatments have also shown fewer postoperative complications and faster, uneventful healing when compared to traditional surgical techniques.1
Within dentistry, diode lasers have become common for use as soft-tissue surgical devices. As these tools are used more frequently, their functions and utility continue to expand in the dental clinic. Besides soft-tissue surgical applications, some diode lasers can also be used for teeth whitening,2 biostimulation,3 reduction of gingival inflammation as an adjunct in the management of periodontal disease,4 temporomandibular joint treatment,5 and photocoagulation of vascular lesions.6 Diode lasers also have a high affinity for hemoglobin, which makes them suitable for the treatment of vascular malformations and pigmented lesions.7 Photocoagulation results in no bleeding, fewer postoperative symptoms, and a safer approach to treating these types of lesions and providing relief to the patient.8
In this clinical case report, a unique diode laser was used to treat a hemangioma of the tongue. While not common in the oral cavity, hemangiomas can occur in the lips, tongue, buccal mucosa, and palate. Their appearance can vary from a round, bluish-red, raised lesion, to a pedunculated, irregular shaped mass. Most hemangiomas of the oral cavity are classified as capillary hemangiomas, which are formed by small capillaries surrounded by a layer of endothelial cells in a connective-tissue stroma. Hemangiomas can become quite large, are unsightly, and can bleed if traumatized. Some can affect swallowing, speech, or breathing, though most do not. Traditional methods of treatment include surgical excision, x-ray therapy, sclerotherapy, and embolization; however, clinical guidelines for these procedures are not uniform and exhibit deficiencies.9 These techniques can result in excessive bleeding, postoperative complications, and slower healing, all of which can lead patients to avoid treatment.10
Clinical Case Presentation Diagnosis and Treatment Plan
A 59-year-old man presented with a raised bluish-red lesion on the left central surface of the tongue. The patient said he had had the lesion for a number of years, that it seemed to fluctuate in size and shape, and that he was uncertain of its etiology.
Approximately 2 years prior, the patient attempted to have the lesion surgically treated. According to him, the procedure resulted in “moderate bleeding for 2 hours,” creating a very stressful situation for both the patient and the medical practitioner that provided treatment. While the procedure did slightly decrease the size of the lesion, the patient was unwilling to undergo another surgical procedure based on this experience. Seeking another treatment modality, he was referred for evaluation and possible laser treatment. The thought of using a laser to treat the lesion in a less invasive, bloodless procedure appealed to the patient.
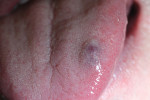
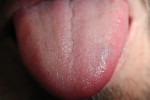
Upon further examination, the raised bluish-red lesion was identified as 9 mm x 12 mm in size with regular-shaped borders (Figure 1). The patient reported no pain or bleeding at the time of the evaluation but did report episodes of bleeding following trauma in the past. Other than the lesion being unsightly and bothersome, it posed no breathing, swallowing, or speech problems. The patient’s health was excellent with no systemic problems or conditions that would impact the treatment of the hemangioma.
Clinical Protocol
The patient was advised of the treatment, and informed consent was obtained. Both the patient and clinician wore wavelength-specific safety eyewear during the entire procedure.
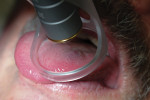
The actual treatment consisted of using a 940-nm diode laser (EPIC™, BIOLASE, www.biolase.com) with an adjustable pain therapy handpiece capable of creating diffuse laser energy patterns ranging from 15 mm to 30 mm in size. The handpiece was set at a spot size of 15 mm for this treatment. Power output was set at 4.0 W continuous wave. The pain therapy handpiece was slowly moved over the lesion (Figure 2) while emitting laser energy for two 3-minute intervals, with a 30-second interval between the actual laser treatments. Total laser time on tissue was 6 minutes. The patient said he “felt warmth” on the tongue, but not to the point of pain, and no local anesthetic was used during the procedure.
Immediately following the procedure, there was little visible change to the targeted tissue and the patient stated the warm sensation dissipated. The patient was given postoperative instructions for care that included nonprescription NSAIDs, warm salt-water rinses, and a soft diet.
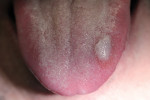
The patient was also instructed to report any adverse conditions such as swelling, fever, signs of infection, or difficulty swallowing or breathing. He was also asked to return the following day for a 24-hour postoperative check. In a phone call to the patient the evening of treatment, he revealed slight discomfort and an increased, whitish discoloration to the lesion. The 24-hour postoperative check (Figure 3) revealed a raised whitish lesion, with the patient reporting mild discomfort similar to a burn in the mouth caused by hot food, and nodule-like tissue in the tongue at the site of the hemangioma.
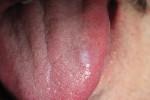
The patient returned for a 1-week postoperative appointment (Figure 4), reporting no complications, a lessening of the whitish area, and a decrease in the size of the nodule in the tongue. He was surprised at the decrease in the size of the lesion, saying, “it was almost gone.” Subsequently, at a 1-month postoperative appointment (Figure 5), the lesion was visibly gone and no nodule or firmness was noted in the tongue where the lesion had previously been located.
Discussion
Past treatment modalities for oral hemangiomas usually involved medication (eg, systemic steroid treatment), sclerotherapy, embolization, x-ray therapy, or excisional surgery. These treatment methods carry several unwanted side effects, including bleeding, risk of infection, and systemic complications as the patient in the present case discovered from an earlier attempt to treat his lesion. Bleeding was a major factor in his previous treatment, as was postoperative discomfort. Using photocoagulation with a diode laser eliminated the need to incise the lesion, which greatly increased the patient’s acceptance of treatment and overall perception of care.
Other than the patient reporting a feeling of warmth, the minimally invasive procedure had no visible or reported adverse effects on him. Postoperative symptoms were mild, and other than the lesion hardening slightly into a nodule due to photocoagulation of the lesion site (which dissipated with time and eventually disappeared over a 1-month period), the healing was uneventful. Variables that could affect the outcome of diode-laser photocoagulation include:
Size of the lesion.
• Type of handpiece used to disperse the laser energy into the targeted tissue.
• Wavelength of the diode laser (810 nm, 940 nm, 980 nm, 1060 nm).
• Time of laser interaction with the targeted tissue.
• Distance of the laser from the targeted tissue.
• Number of applications and time interval.
Further research and clinical studies are needed to help standardize this approach to provide the most efficient and effective treatment to the patient.
Conclusion
Through the successful resolution of a lingual hemangioma using a 940-nm diode laser and special handpiece attachment, this case report demonstrates the potential advantages of innovative laser photocoagulation treatment as an alternative to more invasive, surgical methods. No injectable anesthetic was used. Because no incisions were made, no bleeding was reported. This less invasive nature of treatment averted complications involved with incising a vascular lesion such as the need for suture placement and resulting scarring. Additionally, due to the bactericidal effect of the laser, the chances of postoperative infection and discomfort to the patient were reduced.
The use of a 940-nm diode laser offers an alternative, less-invasive treatment modality for patients presenting with hemangiomas of the oral cavity. While there are a few previously published clinical studies demonstrating this procedure, further case studies and clinical research are needed to standardize a treatment protocol using the 940-nm diode laser.
Disclosures
Dr. Koceja has no relevant financial relationships to disclose.
References
1. Coluzzi DJ. Fundamentals of dental lasers: science and instruments. Dent Clin North Am. 2004;48 (4):751-770.
2. Dostalova T, Jelinkova H, Housova D, et al. Diode laser-activated bleaching. Braz Dent J. 2004;15 spec no:SI3-SI8.
3. Walsh LJ. The current status of low level laser therapy in dentistry. Part 1. Soft tissue applications. Aust Dent J. 1997;42(4):247-254.
4. Qadri T, Miranda L, Tunér J, Gustafsson A. The short-term effects of low-level lasers as adjunct therapy in the treatment of periodontal inflammation. J Clin Periodontol. 2005;32(7):714-719.
5. Pinheiro AL, Cavalcanti ET, Pinheiro TI, et al. Low-level laser therapy in the management of disorders of the maxillofacial region. J Clin Laser Med Surg. 1997; 15(4):181-183.
6. Deppe H, Horch HH. Laser applications in oral surgery and implant dentistry. Lasers Med Sci. 2007;22 (4):217-221.
7. Genovese WJ, dos Santos MT, Faloppa F, de Souza Merli LA. The use of surgical diode laser in oral hemangioma: a case report. Photomed Laser Surg. 2010;28(1): 147-151.
8. Fekrazad R, Am Kalhori K, Chiniforush N. Defocused irradiation mode of diode laser for conservative treatment of oral hemangioma. J Lasers Med Sci. 2013;4(3):147-150.
9. Donnelly LF, Adams DM, Bisset GS III. Vascular malformations and hemangiomas: a practical approach in a multidisciplinary clinic. AJR Am J Roentgenol. 2000;174(3):597-608.
10. Buckmiller LM, Richter GT, Suen JY. Diagnosis and management of hemangiomas and vascular malformations of the head and neck. Oral Dis. 2010;16 (5):405-418.
About the Author
Michael K. Koceja, DDS
Private Practice
Camas, Washington