Treatment of a Miller Class II Gingival Recession Defect
Use of double-layer acellular dermal matrix: 5-year results
Douglas H. Mahn, DDS
Gingival recession presents when the gingival margin is located apical to the cementoenamel junction (CEJ), resulting in exposure of the root surface. One or more sites of gingival recession can be found in 50% of persons aged 18 to 64 years.1 Gingival recession severity increases with age.1 In people 65 years or older, the prevalence is approximately 88%.2
The use of a subepithelial connective tissue graft (SCTG) in conjunction with a coronally advanced flap (CAF) is a successful method of gaining root coverage and augmenting gingival thickness.2-4 Using SCTGs with a thickness of 2 mm or greater is reportedly more successful in achieving complete root coverage than using thinner SCTGs.4 Palatal masticatory mucosa reportedly has an overall mean thickness of 3.83 mm ± 0.58 mm.5 This tissue thickness permits harvesting palatal connective tissue grafts of 2 mm or greater.
An acellular dermal matrix (ADM) is a connective tissue allograft derived from the skin of an organ donor.6 ADMs are supplied with a uniform thickness from 0.89 mm to 1.65 mm. Studies and case reports have shown the efficacy of ADM in the treatment of gingival recession defects.7-9 However, a report from Esteibar and colleagues shows lower success rates in root coverage with ADM compared to SCTGs.4 Given the thickness of the palatal masticatory mucosa, harvested palatal SCTGs may have greater thickness than that of a single layer of ADM. To address the difference in graft tissue thickness, a double layer of ADM has been used with a CAF to treat gingival recession defects.10,11
This case report demonstrates and discusses the use of a double layer of ADM in the treatment of Miller Class II12 gingival recession defects. Long-term (5-year) success was achieved in this case.
Case Management
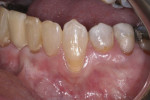
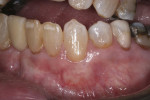
A 67-year-old female non-smoker was referred for treatment of a progressive gingival recession defect. The facial aspect of tooth No. 22 was found to have 4 mm of gingival recession (Figure 1). There was no attached keratinized gingiva on the straight facial aspect of the tooth. The straight facial probing depth was 2 mm. The root appeared prominent and visible through the translucent mucogingival tissues. A facial noncarious cervical root lesion was present.
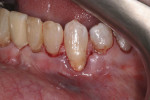
Local anesthesia was administered using 2% lidocaine with 1:100,000 epinephrine. Initial intrasulcular incisions were made using a Bard-Parker No. 15 blade from the distofacial of tooth No. 21 to the mesiofacial of tooth No. 23 (Figure 2). A full-thickness flap was carefully elevated using a Kirkland knife. Beneath the mucosa, a split-thickness flap was created. Adequate tension-free coronal advancement that permitted full root coverage was verified. Root surface irregularities were reduced using sharp hand instruments until they were smooth.
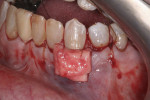
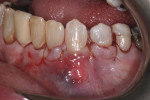
Two pieces of ADM (AlloDerm®, BioHorizons, www.biohorizons.com) were trimmed to approximately 10 mm in width and 8 mm in height. They were layered on top of one another with the connective tissue side of both ADMs positioned toward the facial. Approximately 2 mm of the ADM lay over the wound bed on either side of the root. A continuous 4.0 chromic gut suture was secured to the interdental facial gingival between teeth Nos. 20 and 21. The double layer of ADM was secured over the buccal root surface by weaving the suture around the lingual of the teeth and engaging the double layer of ADM on the facial. This suture held the double layer of ADM in a coronal position (Figure 3). Once secured, the double layer of ADM was tucked beneath the gingival flap. The gingival flap was coronally advanced to completely cover the double layer of ADM and root surfaces. The gingiva was secured into position by weaving the suture distally. The final suture knot was tied over the original suture knot (Figure 4).
Along with being given postoperative instructions, the patient was prescribed ibuprofen (600 mg) for discomfort as well as amoxicillin (875 mg) twice per day for 10 days. The patient was instructed not to brush or floss the surgical site for 7 days. Instead, she was instructed to rinse with 0.12% chlorhexidine gluconate (Peridex®, Procter & Gamble, www.pg.com) and expectorate twice daily. After 7 days, the patient was to discontinue the rinse and begin gentle toothbrushing and flossing. Toothbrushing was to be in a coronal direction only. After 6 weeks, the patient could resume normal toothbrushing and flossing.
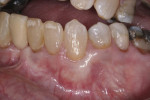
At 12 weeks, tooth No. 22 was healed with complete root coverage (Figure 5). The mucogingival tissues appeared thicker, and the overall gingival architecture had a natural appearance and contours. No observable increase in the zone of keratinized tissue was noticed. The straight facial probing depth was 2 mm.
At 5 years (61 months), the gingival margin position had remained stable with complete root coverage (Figure 6). The mucogingival tissues continued to appear thick, and the overall appearance looked natural. No increase in keratinized tissue was observed. The straight facial probing depth continued to be 2 mm.
Discussion
The combination of a SCTG and CAF has been found to be successful in the treatment of gingival recession defects.2-4 SCTGs with a thickness of greater than 2 mm were reported to have a higher rate of complete root coverage than SCTGs that were less than 2-mm thick.4 The use of an ADM has also been shown to be successful in the treatment of gingival recession defects.7-9 An ADM used with a CAF was shown to increase gingival thickness when compared to a CAF alone.9 In most studies, a single layer of ADM was used.7-9
In this case report, a double layer of ADM with a CAF was used and 100% root coverage was achieved. This root coverage remained stable from 12 weeks to 5 years (61 months). This result compares well with findings from a systematic literature review in which several types of root coverage procedures were evaluated.3 Chambrone et al3 reported that an ADM (single layer) with a CAF ranged from 50.7% to 96% root coverage, and complete root coverage 7.7% to 91.6% of the time. For a SCTG with a CAF, those same authors3 reported a range of 64.7% to 97.3% root coverage, and complete root coverage 53% to 89% of the time.
The results in this case report are consistent with findings of studies evaluating the use of a double layer of ADM with a CAF.10,11 In those studies, complete root coverage was found in 80% of the teeth after 1 year and 69.2% after 4 to 5 years.
Harris13 evaluated the short-term and long-term results of root coverage using an ADM (single layer) and a SCTG. A specially designed scalpel with parallel blades spaced 1.5 mm apart was used to harvest the palatal SCTGs.14 No measurements comparing the thickness of the ADMs or SCTGs were made. The short-term results using the ADM (mean 12.3 weeks) was 93.4% while the long-term (mean 48.1 months) was only 65.8% root coverage. The short-term (mean 13.2 weeks) results using a SCTG were 96.6%. However, the results using a SCTG remained stable with long-term results (mean 49.2 months) with 97% root coverage. Harris concluded that the results with the SCTG held up better than the mean results with an ADM.
In contrast to the study by Harris,13 a double layer of ADM was used in this case report. This may be an important difference. Mahn10 reported that using a double layer of ADM with a CAF in 50 consecutively treated teeth with 94.7% stable root coverage was maintained from 12 to 52 weeks. In another study, Mahn11 reported 95% root coverage between 6 to 8 weeks and 92.5% root coverage at 48 to 66 months (4 to 5 years). These results may indicate the long-term benefits of using a double-layer of ADM verses a single-layer of ADM.
The lack of increase in keratinized tissue was not unexpected in this case. SCTG, being cellular, has the ability to increase the keratinized tissue when it is left partially exposed.15 ADMs are a noncellular scaffold and must be completely covered. Exposed portions of ADM will disintegrate due to a lack of revascularization. Therefore, the potential of ADM to increase keratinized tissue is limited.16
Conclusion
The use of a double layer of ADM with a CAF can yield long-term success in the treatment of Miller Class II gingival recession defects. Further investigation of this treatment modality would be useful.
Disclosure
Douglas H. Mahn, DDS, has no relevant financial relationships to disclose.
References
1. Kassab MM, Chaen RE. The etiology and prevalence of gingival recession. J Am Dent Assoc. 2003;134(2):220-225.
2. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
3. Chambrone L, Sukekava F, Araújo MG, et al. Root-coverage procedures for the treatment of localized recession-type defects: a Cochrane systematic review. J Periodontol. 2010;81(4):452-478.
4. Esteibar JR, Zorzano LA, Cundin EE, et al. Complete root coverage of Miller Class III recessions. Int J Periodontics Restorative Dent. 2011:31(4):e1-e7.
5. Song JE, Um YJ, Kim CS, et al. Thickness of posterior palatal masticatory mucosa: the use of computerized tomography. J Periodontol. 2008;79(3):406-412.
6. Scarano A, Barros RR, Iezzi G, et al. Acellular dermal matrix graft for gingival augmentation: a preliminary clinical, histologic, and ultrastructural evaluation. J Periodontol. 2009;80(2):253-259.
7. Harris RJ. A comparative study of root coverage obtained with an acellular dermal matrix versus a connective tissue graft: results of 107 recession defects in 50 consecutively treated patients. Int J Periodontics Restorative Dent. 2000;20(1):51-59.
8. Aichelmann-Reidy ME, Yukna RA, Evans GH, et al. Clinical evaluation of acellular allograft dermis for the treatment of human gingival recession. J Periodontol. 2001;72(8):998-1005.
9. Woodyard JG, Greenwell H, Hill M, et al. The clinical effect of acellular dermal matrix on gingival thickness and root coverage compared to coronally positioned flap alone. J Periodontol. 2004;75(1):44-56.
10. Mahn DH. A double-layer technique using an acellular dermal matrix for the treatment of Miller Class I and II gingival recession defects: 1-year results of 50 consecutive cases. Int J Periodontics Restorative Dent. 2015;35(2):257-262.
11. Mahn DH. Use of a double-layer technique with an acellular dermal matrix to treat Miller Class I and II gingival recession defects: 4- to 5-year results. Clinic Adv Periodontics. 2016;6(1):44-49.
12. Miller PD Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
13. Harris RJ. A short-term and long-term comparison of root coverage with an acellular dermal matrix and a subepithelial graft. J Periodontol. 2004;75(5):734-743.
14. Harris RJ. A comparison of two techniques for obtaining a connective tissue graft from the palate. Int J Periodontics Restorative Dent. 1997;17(3):261-271.
15. Han JS, John V, Blanchard SB, et al. Changes in gingival dimensions following connective tissue grafts for root coverage: comparison of two procedures. J Periodontol. 2008;79(8):1346-1354.
16. Wei PC, Laurell L, Lingen MW, Geivelis M. Acellular dermal matrix allografts to achieve increased attached gingival. Part 2. A histological comparative study. J Periodontol. 2002;73(3):257-265.
Douglas H. Mahn, DDS
Private Practice limited to Periodontics and Implantology
Manassas, Virginia