Simplifying Zirconia Cementation with Glass Ionomer Cement
A successful alternative to PFM restorations
Ara Nazarian, DDS, DICOI
As an alternative to conventional porcelain-fused-to-metal (PFM) restorations, zirconia restorations have grown in popularity among clinicians because they are functional, esthetically pleasing, long lasting, and a good choice for gingival health. Many dental providers choose zirconia because in addition to featuring a metal-free composition, they are also stronger than other restorative materials and cost-effective.
Successful anterior cases typically require high-quality esthetics, strength, and flexibility. Layered zirconia restorations combine these key characteristics with a substructure flexural strength of 1200 MPa, which is higher than most PFM restorations. The fracture toughness and flexural strength are also much higher than alumina or any other all-ceramic materials.1 Layered zirconia does not have the esthetic concerns of metal that shows through or black lines at the gingival margins. Most importantly, clinicians can cement layered zirconia conventionally with glass ionomer and resin-modified glass ionomer cements, which both have excellent biocompatible properties.1 If the primary resistance and retention form of the preparation is not adequate, then the use of bonding agents with resin cements may be suggested for the long-term success of the restoration.2 This case study examines the use of layered zirconia restorations with glass ionomer cement to efficiently and effectively restore the form and function of a patient’s dentition.3
Case Presentation
A man in his late 30s presented to the practice for an esthetic consultation. The patient was not pleased with his smile and did not feel comfortable in social circumstances or in the workforce. In particular, the patient was dissatisfied with the edentulous area of teeth Nos. 10 and 11. According to the patient, these teeth were congenitally missing. In addition, the patient had already undergone orthodontic treatment to create an ideal space for the replacement of these teeth. He had been wearing a temporary acrylic removable partial denture known as a “flipper.”
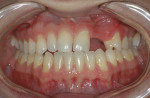
Upon clinical examination, his anterior maxillary teeth exhibited staining and areas of hypocalcification. More importantly, the patient’s midline was skewed to his right with a slight diastema. The patient also exhibited an edge-to-edge position when biting in maximum intercuspation. Lastly, there was a great deal of resorption of the alveolar ridge in the edentulous areas of teeth Nos. 10 and 11 (Figure 1).
The Golden Proportion Rule was used to complete the smile analysis necessary for predesigning the case. The patient’s maxillary anterior teeth were too small, rounded, and short. The patient preferred a more masculine look to complete his smile in addition to filling in the edentulous areas. To satisfy the patient’s request, a squarer tooth shape was selected with smaller embrasures between his teeth. He also needed the teeth lengthened and brought out facially to create a Class I relationship.
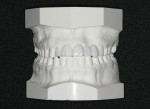
The patient did not want to undergo further orthodontic treatment or grafting procedures for implant treatment. Therefore, a 3D diagnostic wax-up (Arrowhead Dental Lab, www.arrowheaddental.com) helped clinicians visualize the most ideal smile using crown and bridge (Figure 2). All risks, benefits, and alternatives to treatment were discussed with the patient. The treatment would consist of crown restorations on teeth Nos. 7 and 8, while teeth Nos. 9 through 12 would be a fixed partial denture (FPD) with teeth Nos. 9 and 12 being the abutment teeth for the FPD.
Preparation
Once local anesthesia was achieved, a coarse grit diamond chamfer bur (Axis Dental, www.axisdental.com) was used to prepare the teeth for layered zirconia crown and bridge restorations. Utilizing Expasyl® (Kerr Dental, www.kerrdental.com), the author was able to control hemorrhaging and achieve gingival retraction. After approximately 2 minutes in the sulcus, a thorough water rinse removed the Expasyl retraction paste (Figure 3). An impression was taken for the final restoration using a full-arch thermoplastic tray (Instant Custom Tray, Good Fit Technologies, www.goodfit.com) and fast-set impression material (Take 1 Advanced™, Kerr Dental) (Figure 4).
Cementation
Provisional restorations were removed with Pneumatic Crown and Bridge Remover (Dent Corp, www.dentcorp.com). Remaining provisional cement was also removed before trying the definitive restorations to verify the correct fit, color, and shape. The layered zirconia bridge restoration from teeth Nos. 9 through 12 was tried in first followed by the crown restorations on teeth Nos. 7 and 8. After the patient was shown the retracted view for acceptance, the cementation process was initiated.
Riva Luting (SDI, www.sdi.com) conventional, self-curing, glass ionomer luting cement was used for the cementation of these layered zirconia restorations because it can be used without requiring special preparation using cleaning agents and it doesn’t require any bonding agents.
According to the manufacturer, Riva Luting utilizes proprietary ionglass™ filler, a radiopaque, high ion-releasing, reactive glass. Riva Luting releases high levels of fluoride to help with remineralization of the natural dentition, which increases antimicrobial activity against Streptococcus mutans, S. sobrinus, and Lactobacillus species, which are all cariogenic bacteria.4 It also has a low solubility in the oral environment. This increases its ability to resist degradation and wear at the margins, which is typically a result of oral acidity.5
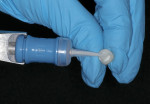
The preparations were washed and dried to the point of being slightly moist. At this time, the cement capsules were depressed consecutively to activate and placed in the Ultramat 2 (SDI) amalgamator for only 10 seconds for trituration. Using the applicator dispenser (SDI), the cement was loaded into the restorations (Figure 5). With a very low film thickness and creamy consistency, the Riva Luting cement was dispensed into the restorations with an easy insertion and seating.
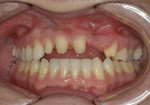
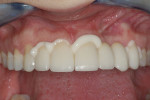
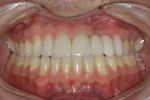
Removal of excess cement was cleaned up in approximately 2 minutes at the gel phase (Figure 6). After the cement was fully set at 5 minutes, the occlusion was verified and adjusted. The soft tissue and restorations were in overall good health and the patient was very pleased with the final results (Figure 7).
Conclusion
It is pivotal that dental professionals now have a legitimate alternative to PFM restoratives in the form of an esthetic and durable all-ceramic. Layered zirconia restorations meet the requirements that dental providers have been looking for in anterior all-ceramic restorations. These restorations allow clinicians to place simple, cosmetic, reasonably priced alternatives with optimal strength, high-quality esthetics, color stability, and biocompatibility. Most importantly, clinical procedures for cementation of these zirconia restorations using glass ionomers and resin-modified glass ionomers are similar to those used when cementing PFM and gold crowns.
References
1. Schrader B. Dental zirconia restorations. Tech Talk. Volume VI. 2011. www.ddslab.com/Content/pdf/DDSLAB-TechTalk-VI-Zirconia-Online.pdf. Accessed December 7, 2015.
2. Christensen GJ. Should zirconia or lithium disilicate be bonded or luted? Dent Econ. 2013;103(3):25-31.
3. Nazarian A. Desired smiles in today’s economy. Dentaltown website. www.dentaltown.com/Dentaltown/Article.aspx?i=304&aid=4153. Accessed November 24, 2015.
4. Waldo B, Zhang P, Bennett J, et al. Antimicrobial Activity of Composite-Resin and Glass-Ionomer Cements [Abstract 0949]. Presented at: IADR/AADR/CADR 83rd General Session; March 2005; Baltimore, MD.
5. Riva Luting product information. SDI website. www.sdi.com.au/en/riva-luting/. Accessed December 8, 2015.
For more information, contact:
SDI
800-228-5166
www.sdi.com.au/en-us