Creating Synergy with Conventional and Small-Diameter Implants
Planning for success with maxillary and mandibular overdentures
Brian J. Jackson, DDS
The demand for implant-supported dentures is projected to increase in coming years, and it is important for clinicians to be aware of the variety of options for patients. In many cases, a patient’s bone quality, quantity, and biomechanics, as well as financial means, may call for a blended approach that utilizes conventional-diameter implants (CDIs) and small-diameter implants (SDIs) or mini dental implants (MDIs). When the proper attention is paid to site preservation and careful implant placement, clinicians can achieve both functional and esthetic success for patients.
Oral reconstruction supported by osseointegrated endosseous implants has improved the quality of life for thousands of patients. The demand for implant therapy in the max-illary and mandibular arch is projected to increase as the number of edentulous or partially edentulous patients rises in the future.1 Research has demonstrated long-term success of an implant-retained overdenture prosthesis within the range of 85% to 99%, depending on the specific arch involved.2 Predictable outcomes have been demonstrated when bone quality, quantity, and biomechanics have served as the foundation of treatment planning.3,4
Frequently, clinicians must develop treatment plans for teeth with a poor prognosis, and extraction with site preservation through socket grafting has become a routine procedure.5 Site preservation allows for the development of adequate bone, enabling conventional implant placement while establishing bone density for initial fixation for SDIs.6
CDIs are considered when adequate bone and significant occlusal loads exist or bone-grafting procedures demonstrate a favorable long-term prognosis. However, SDIs are an alternative modality when patients present with diminished bone quality, quantity, and reduced biomechanical loads.7 Utilizing a variety of implant designs and diameters based on the patient’s existing anatomy, medical conditions and monetary constraints can provide a multitude of treatment options. In this case presentation, a thought-provoking treatment plan focusing on bone quality, quantity, age, and biomechanical loads served as the primary considerations in resolving the patient’s chief complaint.
Case Presentation
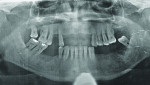
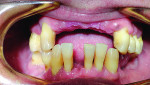
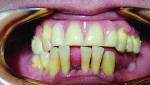
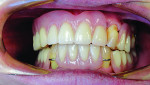
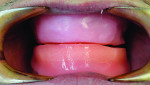
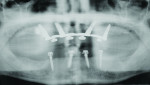
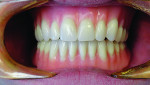
A 41-year-old man presented to the office stating that he did not want to wear partials anymore because they were not comfortable. The patient’s medical history exhibited no significant findings except that he smoked one pack of cigarettes per day. A radiographic survey demonstrated severe horizontal bone loss associated with his maxillary and mandibular teeth (Figure 1). A diagnosis of severe periodontitis was established. The intraoral dental examination revealed a total of 16 remaining teeth in the maxillary and mandibular arches (Figure 2). Class II and III periodontal mobility was exhibited by 9 teeth. The patient was wearing a maxillary transitional removable partial denture (Figure 3).
At consultation, various treatment plans were presented, including saving specific teeth or full-mouth extraction. In addition, the treatment plans included CDIs and SDIs to enhance support, stability, and retention in prosthetic reconstruction. The agreed-upon treatment plan was maxillary and mandibular overdentures. A screw-retained superstructure supported by four CDIs would retain the maxillary overdenture. The mandibular overdenture prosthesis would be retained by four SDIs. The treatment would be performed in a staged approach with extraction and grafting followed by implant placement. Consent, time frame for treatment completion, and provisionalization were reviewed.
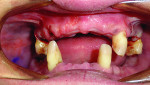
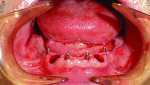
The pre-implant surgical stage consisted of extraction with site preservation. The mandible was anesthetized and teeth Nos. 23, 25, 26, 28, and 30 were removed. The sockets were debrided with a double-ended curette and grafted with a mineralized irradiated cancellous allograft (Puros®, Zimmer Dental, www.zimmerdental.com) and contained with a d-polytetrafluoroethylene (Cytoplast™, Osteogenics Biomedical, www.osteogenics.com) barrier. The extractions of the maxillary arch consisted of teeth Nos. 1, 4, 6, 12, and 13, and the procedure and grafting materials employed in the maxilla mimicked the mandibular arch (Figure 4). Maxillary and mandibular removable partial dentures (RPDs) were placed, occlusion adjusted, and polished (Figure 5).
Surgical Stage
The maxillary implant surgical procedure was initiated 3 months after the extractions and socket grafting. The patient was prepped, draped, and asked to rinse with a 0.12% chlorhexidine mouth rinse for 30 seconds. The blood separation process to develop platelet-rich plasma was initiated. The patient was anesthetized, and a midcrestal incision with a 15c blade was made and a full mucoperiosteal flap reflected with a periosteal elevator. A surgical guide was placed and four osteotomy “dimples” were made with a surgical long shank No. 4 round bur. The implant surgical protocol drill sequence was 1.3, 2.0, 2.5, and 3.1 mm to a depth of 12 mm for the future 3.8-mm diameter implants. The 4.8-mm diameter implant required two additional drills, 3.8 and 4.1 mm, to complete the osteotomy. Three 3.8-mm x 12-mm RBC Tapered Laser-Lok (BioHorizons, www.biohorizons.com) implants were placed at the crest using a fixture mount and a 2.5-mm hex driver. The cover screw was secured to the fixture via a 1.25-mm hex tool. The mucoperiosteal flap was closed using 4.0 vicryl sutures in a horizontal mattress manner.
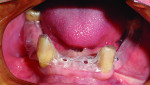
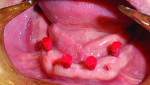
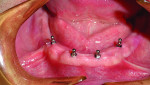
The mandibular implant surgery was initiated 3 months after the maxillary implants were placed. The preparation and anesthesia of the patient were similar to the maxillary implant surgery. A full mucoperiosteal flap was established with a 15c blade penetrating midcrestally and reflected with a periosteal elevator. A surgical template was placed to aid in the mesial-distal location of the future implant sites (Figure 6). The partial osteotomies were prepared with a 1.1-mm drill to a depth of 6 mm. The four 2-mm x 13-mm O-ball collared MDIs (MDI Mini Dental Implants, 3M Oral Care, www.3mespe.com/implants) were auto-advanced with a finger driver, thumb wrench, and ratchet to final position (Figure 7). The transitional RPD was relieved where the transgingival aspect of the o-ball was located and the occlusion was adjusted.
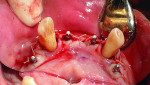
Second stage surgery for the maxillary arch consisted of the exposure of the conventional implants and extraction of all remaining teeth. This procedure was initiated 6 months post implant placement. Three 3.8-mm x 5-mm and one 4.8-mm x 5-mm titanium healing collars were placed during the surgical uncovering procedure. In addition, teeth Nos. 3, 11, 14, 19, 22, 27, and 30 were extracted (Figure 8). The transitional RPDs were modified to incorporate additional prosthetic teeth and relined with a soft temporary material. The soft tissues healed for 6 weeks prior to prosthetic reconstruction.
Prosthetic Reconstruction
The prosthetic reconstruction stage was unique to the specific type of implant design utilized in the treatment plan. The primary objective of the impression stage was to capture the position and angulation of the implants. The maxillary arch employed an open-tray impression technique to capture an abutment level impression (Imprint™ 3 VPS Impression Material, 3M Oral Care) (Figure 9). The mandibular MDIs were impressed after placing “red” transfers onto the o-ball aspect of the implant (Figure 10). A polyvinylsiloxane impression material (Imprint 3) was utilized within a border molded custom tray for both arches.
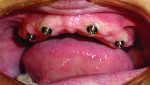
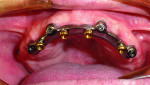
The intraoral impressions were sent to a commercial laboratory where a final working model was established. The maxillary superstructure with locator attachments was designed and manufactured with CAD/CAM technology (Figure 11). The mandibular unibase with o-ring housings was made using standard dental laboratory procedures (Figure 12). The passivity of the maxillary superstructure was confirmed intraorally using the Sheffield test and a panoramic radiograph. A maxillary/mandibular relationship utilizing baseplates and wax rims, as well as a mold and shade, were taken (Figure 13). A try-in of the final prosthesis was used to confirm vertical dimension of occlusion, phonetics, esthetics, and patient acceptance. The final superstructure was fixated to the implants with retaining screws, torqued to 30 Ncm and locator inserts placed with a cumulative retention value of 7.5 lbs (2 pink and 1 blue). The final maxillary and mandibular overdentures were placed 1 week thereafter (Figure 14 and Figure 15).
Discussion
Creating synergy with CDIs and SDIs can provide a multitude of treatment alternatives for oral rehabilitation. The size of the implants used depends on various factors of the quality and quantity of bone, as well as biomechanical stress. Site preservation has become a predictable method to optimize bone dimensions and density for future implant sites.8,9
Conventional implants (3.4 to 6.0 mm) are the primary type of endosseous implants used for long-term predictability in implant-retained or supported therapy.10 They can be utilized when the facial-buccal or facial-lingual dimension exhibits a minimal bone of 6 to 8 mm. Conventional size implants remain the primary option for patients who have adequate bone or who accept bone grafting procedures, and who also have financial means.
SDIs (1.8 to 2.9 mm) are an alternative to CDIs when specific criteria are met.11 The major reason for utilizing SDIs is minimal width of bone or space between adjacent teeth in a mesio-distal dimension. In addition, SDIs are indicated for patients who are not candidates for invasive bone grafting procedures due to medical reasons, limited finances, or time. SDIs demonstrate high success in the mandibular arch when retaining removable overdentures.12
The maxilla has demonstrated lower success rates than the mandible in regards to implant therapy. Protocols have been established to enhance success rates as they relate to the mandible.13 These protocols have centered around minimizing stress to the crestal bone, where bone loss is often seen. A critical consideration is utilization of implants with a diameter size greater than 3 mm, which reduces stress at the crest of the alveolar bone due to increased surface area. In addition, increasing the number of implants from four to six demonstrates higher success rates via an increase in cumulative surface area. Implant lengths of 12 mm or greater have exhibited two to three times greater success versus 10-mm lengths. Superstructure design without a cantilever component has demonstrated higher overdenture retention with less resultant crestal bone loss. The elimination of cantilevers in the maxillary superstructure bar reduces stress on the distal terminal implants.
Research has demonstrated positive long-term outcomes with the utilization of SDIs in the mandible.14 Rigid fixation of the implant body at the time of placement is crucial for the osseointegrative process to ensue.15 Secondarily, the auto-advanced technique coupled with a partial osteotomy enhances bicortical stabilization.16 Flapless surgery and immediate load are considerations when utilizing a one-piece SDI.17 However, a full mucoperiosteal flap with a 3-month osseointegrative time period was utilized in this case.
In the case report, the decision to utilize conventional implants in the maxilla was based on diminished bone quality and significant biomechanical load. Research has exhibited guarded success rates with maxillary overdentures.18 SDIs were employed in the mandible because excellent success rates have been demonstrated in similar cases.19 The patient made a treatment decision based on personal finances, as well as an understanding of bone density and biomechanics and how they relate to long-term outcomes.
Conclusion
Oral implantology has become a major discipline in the field of dentistry. Clinicians must evaluate the patient’s existing condition and develop thought-provoking treatment plans based on a variety of factors. The utilization of CDIs and SDIs should be considered in regards to bone, biomechanics, age, and finances. A synergy of different implant modalities can provide alternative approaches to resolve patient concerns in a predictable, less invasive, and more economical way.
Disclosure
Brian J. Jackson, DDS, has previously lectured for 3M, but did not receive compensation for this article.
Acknowledgments
The author wishes to acknowledge Tatyana Lyubezhanina, DA, and Caitlin Carparelli, DA, for their assistance in the preparation of this paper, and Matt Weigand, CDT, of Utica Dental Laboratory in Utica, New York, for his dental technical expertise.
References
1. Douglass CW, Shih A, Ostry L. Will there be a need for complete dentures in the United States in 2020? J Prosthet Dent. 2002;87(1):5-8.
2. Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications with implants and implant prostheses. J Prosthet Dent. 2003;9(2):121-132.
3. Jemt T, Chai J, Harnett J, et al. A 5-year prospective multicenter follow-up report on overdentures supported by osseointegrated implants. Int J Oral Maxillofac Implants. 1996;11(3):291-298.
4. Bergendal T, Enquist B. Implant-supported overdentures: a longitudinal prospective study. Int J Oral Maxillofac Implants. 1998;13(2):253-262.
5. Sclar AG. Preserving alveolar ridge anatomy following tooth removal in conjunction with immediate implant placement. The Bio-Col technique. Atlas Oral Maxillofac Surg Clin North Am. 1999;7(2):39-59.
6. Nevins R, Mellonig JT. Enhancement of the damaged edentulous ridge to receive dental implants: a combination of allograph and GORE-TEX membrane. Int J Periodontics Restorative Dent. 1992;12(2):207-217.
7. Sendax V. Mini Dental Implants: Principles and Practices. St Louis, MO: Mosby; 2013.
8. Jackson BJ, Morcos I. Socket grafting: a predictable technique for site preservation. J Oral Implantol. 2007;33(6):353-364.
9. Irinakis T, Tabesh M. Preserving the socket dimensions with bone grafting in single sites: an esthetic surgical approach when planning delayed implant placement. J Oral Implantol. 2007;33(3):156-163.
10. Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):11-25.
11. English CE, Bonie GC. Diagnostic procedural and clinical issues with the Sendax mini dental implants. Compend Cont Educ Dent. 2003;24(11 suppl 1):3-25.
12. Shatkin TE, Shatkin S, Oppenheimer BD, Oppenheimer AJ. Mini dental implants for long-term fixed and removable prosthetics: a retrospective analysis of 2514 implants placed over a five-year period. Compend Contin Educ Dent. 2007;28(2):92-99.
13. Hutton JE, Heath MR, Chai JY, et al. Factors related to success and failure rates at 3-year follow-up in a multicenter study of overdentures supported by Branemark implants. Int J Oral Maxillofac Implants. 1995;10(1):33-42.
14. Christensen GJ. The ‘mini’-implant has arrived. J Am Dent Assoc. 2006;137(3):387-390.
15. Balkin BE, Steflik DE, Naval F. Mini-dental implant insertion with the auto-advance technique for ongoing applications. J Oral Implantol. 2001;27(1):32-37.
16. Bulard RA, Vance JB. Multi-clinic evaluation using mini-dental implants for long-term denture stabilization: a preliminary biometric evaluation. Compend Contin Educ Dent. 2005;26(12):892-897.
17. Flanagan D. Flapless dental implant placement. J Oral Implantol. 2007;33(2):75-83.
18. Smedberg JI, Lothigius E, Bodin I, et al. A clinical and radiological two-year follow-up study of maxillary overdentures on osseointegrated implants. Clin Oral Implants Res. 1993;4(1):39-46.
19. Griffitts TM, Collins CP, Collins PC. Mini dental implants: an adjunct for retention, stability, and comfort for the edentulous patient. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100(5):e81-e84.