Programmed Treatment Planning in the Digital Environment
The pathway to functional and esthetic predictability
Michael C. Verber, DMD
There is no greater stress in dental practice than a failed complex restorative case. Because these failures often occur in the planning phase, having a systematic approach to treatment planning and restorations reduces mistakes and increases predictability. Protocols based on the principles of complete dentistry and the evaluation of the entire masticatory system allow for the management of biologic and functional etiology.1 Proper diligence and the use of checklists can eliminate tendencies to short cut the process and the need for guesswork.2
Distinct treatment phases are critical when cosmetic or occlusal issues call for a change in the size, shape, or position of the teeth. Described here as the “Five Ds of Complete Dentistry,” the phases are as follows:
- Discover: Comprehensive Exam and Records
- Diagnose: 2D Treatment Planning
- Design: 3D Treatment Planning
- Debug: Provisional Restoration
- Deliver: Final Restoration
Working with the copious data relevant to these steps can be a challenge. The Dawson Diagnostic Wizard (The Dawson Academy, www.dawsonwizard.com) is cloud-based dental treatment planning software. The software includes tools that facilitate the collection, organization, analysis, and communication of such information.
Case Presentation
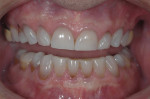
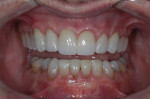
A 51-year-old man was referred for evaluation of esthetic concerns and worn dentition. The patient presented with severe anterior wear, mild to moderate tetracycline staining, and recurrent decay under existing maxillary posterior restorations. His chief complaint was the shortened and discolored appearance of his anterior teeth attributed to bruxism and tetracycline stain (Figure 1). He also expressed a desire to address diastemata between the maxillary canines and lateral incisors. His medical history was unremarkable and there was no indication of sleep apnea or gastroesophageal reflux disease.
Discover: Comprehensive Exam and Records
The Diagnostic Wizard guided a thorough comprehensive exam of the soft tissues, airway, muscles, teeth, and joints. The temporomandibular joints (TMJs) were seated in centric relation (CR) and able to be comfortably loaded with bimanual manipulation.3 Posterior interferences causing a displacement from the CR position into maximum intercuspation (MI), as characterized by a Dawson Type II occlusion, were identified.4 Doppler auscultation revealed a click in the right TMJ upon translation and lateral excursions, indicating a reduced displacement of the disc at the lateral pole.5
Records were taken with the intent to mount the models on a semi-adjustable articulator while transferring proper maxillary relationships. The verifiable CR position included polyvinyl siloxane (PVS) impressions, a face-bow transfer, and a wax bite in CR. Using a digital SLR camera, 21 photos of the face and dentition were taken. The photos were uploaded to the Diagnostic Wizard.
Diagnosis: 2D Treatment Planning
Using the articulated models and a summary report of the exam findings, treatment planning began with a functional-esthetic analysis. The process was expedited by the Diagnostic Wizard’s automated display of pertinent information and photos related to each component of the analysis. Advanced interpretation was accomplished using digital measurement and design tools.
The case was first examined to determine if corrections were necessary to meet the requirements of occlusal stability, including equal intensity stable stops, posterior teeth that do not rub, and anterior contours that do not restrict the envelope of function.5,6 The patient’s occlusion failed to meet all criteria, offering an explanation for the bruxism.
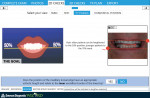
Tying form to function, elements of global esthetics were examined. The maxillo-mandibular relationship was acceptable because of digital analysis incorporating Arnett’s True Vertical Line, Ricketts’ E-plane, and the nasolabial line angle.7 However, the maxillary plane was not perpendicular to the facial midline and the mandibular plane deviated from the Curve of Spee. A deficiency in the vertical position of the maxillary central incisors was also identified. Evident while making the “E” sound, the teeth lacked the appropriate esthetic length related to the lower lip (Figure 2).
The final portion of 2D treatment planning focused on fulfilling macro esthetic criteria. A 100% width-to-length ratio of the central incisors, insufficient incisal embrasures, and unacceptable axial inclinations all called for correction. In addition, gingival contours and positions were unbalanced. Proper dimensions for the maxillary anterior teeth were mapped on the software (Figure 3).
Design: 3D Treatment Planning
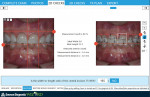
The global position of the teeth was visualized and communicated to the laboratory technician for diagnostic wax-ups using a 3D checklist on the Diagnostic Wizard. With the presence of stable joints and a disharmony between CR and MI, the condylar position was set at CR. Possible treatment modalities were highlighted throughout the digital workup. Options included equilibration, orthodontics, restoration, and orthognathic surgery. The need for an additive equilibration to open vertical dimension of occlusion and replace lost enamel dictated a restorative solution (Figure 4). An illustrated summary report from the software was sent to the dental lab as a prescription for the wax-ups. The workup was also shared with a local periodontist to plan for gingival display correction.
Debug: Provisional Restoration
Treatment was initiated after the receipt and approval of the diagnostic wax-ups. The entire upper arch was prepared for crowns and temporized with a self-curing bis-acryl composite material (Telio CS C&B, Ivoclar Vivadent, www.ivoclarvivadent.us) from a matrix of the wax-ups (Figure 5). To accommodate the patient’s budget and desire for phased treatment, the lower occlusal plane was corrected with limited reshaping of the posterior teeth and transitional incisal composite resin (IPS Empress® Direct, Ivoclar Vivadent) restorations on the anteriors. The maxillary gingival heights were raised and contoured with a diode laser to the desired marginal position. The patient was seen the following day by the periodontist for crown lengthening to re-establish healthy biologic width.
The temporaries remained in place for approximately 3 months while the soft tissues matured. The healing time also provided an appropriate “test drive” to confirm a stable occlusion and acceptable esthetics.
Deliver: Final Restoration
Final restoration began with PVS impressions of the temporaries and the preparations. The temporaries were face-bowed and bites were taken to allow for articulation and cross-mounting of the temporary and master models. At the lab, wax patterns were fabricated with the use of CAD/CAM technology and refined with the aid of an anterior guide table and photographs of the temporaries.
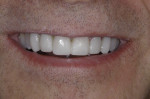
IPS e.max® lithium disilicate crowns (Ivoclar Vivadent) were cemented with the Variolink® II dual-curing composite adhesion system (Ivoclar Vivadent) (Figure 6).
Discussion
A diagnostic software application can offer numerous advantages. In addition to disciplining the practitioner, time spent evaluating and planning cases is drastically reduced. Communication with the interdisciplinary team, including laboratory technicians, is also improved.
Perhaps the greatest benefit of the Dawson Diagnostic Wizard is its interactive visual platform that draws both auxiliary team members and patients into the complete exam and treatment planning process. Exposing patients to the Wizard helps them identify and understand their dental issues while motivating them to proceed with a comprehensive plan.
About the author
Michael C. Verber, DMD
Faculty
The Dawson Academy
St. Petersburg, Florida
Private Practice
Camp Hill, Pennsylvania
For more information, contact:
The Dawson Academy
800-952-2178
https://thedawsonacademy.com
References
1. Dawson PE. The concept of complete dentistry. In: Dawson PE, ed. Functional Occlusion: From TMJ to Smile Design. New Edition. St. Louis, MO: Mosby; 2007:3-9.
2. Gawande A. The Checklist Manifesto: How to Get Things Right. 1st ed. New York: Metropolitan Books; 2010.
3. McKee JR. Comparing condylar positions achieved through bimanual manipulation to condylar positions achieved through masticatory muscle contraction against an anterior deprogrammer: a pilot study. J Prosthet Dent. 2005;94(4):389-393.
4. Dawson PE. Classification of occlusions. In: Dawson PE, ed. Functional Occlusion: From TMJ to Smile Design. New Edition. St. Louis, MO: Mosby; 2007:107-109.
5. Piper MA. Piper’s Classification of TMJ Disorders. Piper Education and Research Center website. www.pipererc.com. Accessed September 12, 2015.
5. Dawson PE. Requirements for occlusal stability. In: Dawson PE, ed. Functional Occlusion: From TMJ to Smile Design. New Edition. St. Louis, MO: Mosby; 2007:345-348.
6. Williamson EH, Lundquist DO. Anterior guidance: its effect on electromyographic activity of the temporal and masseter muscles. J Prosthet Dent. 1983;49(6):816-823.
7. Arnett GW, Jelic JS, Kim J, et al. Soft-tissue cephalometric analysis: diagnosis and treatment planning of facial deformity. Am J Orthod Dentofacial Orthop. 1999;116(3)239-253.