Complete Treatment Planning: Meeting Patients’ Needs
A systematic approach to treating occlusal dysfunction
Treatment planning in today’s environment can be very confusing for both the patient and the dentist. Patients can present with a myriad of problems, some obvious and others not so. Tooth decay, periodontal disease, endodontic issues, gingival recession, tooth wear, mobility, migration, esthetic issues, muscle soreness and temporomandibular joint (TMJ) problems are but a few of the potential issues facing our patients. Creating a complete treatment plan that addresses the patient’s needs and communicating that plan to the patient can be especially challenging.
Whether dentists realize it or not, they treat two populations of patients within their dental practices. In the first patient population, the issues are chiefly bacterial in nature. The second population may also present with bacterial issues, but the size, shape, or position of the teeth is also unacceptable, potentially leading to functionally based breakdown. The functional issues can result in excess force applied to the masticatory system, leading to potential breakdown of teeth, muscle, or the TMJ. Dr. Peter Dawson describes this as occlusal disease.1
Occlusal disease is the most common and the most undiagnosed problem facing patients. These problems only get more complicated as the destructive nature of occlusal disease progresses. For the dental practitioner, these issues pose a diagnostic and treatment planning challenge. If the treatment goal is to correct all of the bacterial and functional problems of patients, satisfy their esthetic concerns, and do so with the least amount of dentistry, then knowing when and how to treat is of utmost importance. In addition, sequencing care becomes important; some problems requiring immediate care, whereas others may be deferrable.2
The long-term goal of complete treatment is elimination of disease from all masticatory structures, creating a healthy periodontium, healthy teeth, stable TMJs, and stable occlusion and function as well as optimal esthetics. Ideal function decreases potential negative effects of excessive forces being applied to the dentition, restorations, and supporting structures.1 The starting point is an orthopedically and repeatable TMJ position-centric relation.3,4 Simultaneous tooth contacts with anterior guidance in eccentric movements creates a peaceful neuromusculature.5 The position and contours of the anterior teeth are not arbitrary and affect proper esthetics, function, and speech.1 When dysfunction in the masticatory system and problems with teeth, muscle, or the TMJs are present, the dentist must find the cause. Failure to do so and treating just the effects will most likely lead to unsuccessful outcomes. Successful long-term solutions are attained by visualizing the end result before any definitive treatment is completed.
Although this may seem like a time-consuming task for the busy practitioner, it is actually an effective and efficient process. It is through this process that predictable success is possible. Unsuccessful restorative results cost the dentist time and money and can damage the doctor-patient relationship.
The four-pronged approach of complete dentistry presented below enables the dentist to identify solutions, prioritize treatment, and communicate this plan to the patient. An honest economic discussion with patients will allow the dentist to create a treatment plan that may better fit within a patient’s budgetary constraints. Creativity in treatment planning and the use of today’s materials can serve as an interim stage prior to definitive restorations.
Following a protocol allows the dentist to visualize a treatment plan for predictable long-term health. This patient-centered approach provides solutions for all potential masticatory problems: bacterial, functional, and esthetic. Treatment planning is not about selling services but rather about helping patients achieve long-term sustainable health. Treatment plans should be customized to the patient’s needs for both mandatory and deferrable treatments. Deferrable, elective, and sequenced treatment can be discussed, allowing patients to decide on treatment that best meets their needs. Following this process allows the dentist to be the patient’s advocate for dental health.
The Process of Complete Dentistry
The starting point of this 4-part process is a complete examination identifying any and all problems in the masticatory system—bacterial, functional, and esthetic. It is also important to connect with the patient’s wants and concerns during the examination process. The dentist is responsible for the interpretation of this data. In a co-diagnostic process, signs and symptoms of dental disease along with treatment options are discussed. Relating the dental needs and treatment options to the patient’s wants is paramount to case acceptance.6
It is important to mention that the mere presence of an occlusion that is not ideal is not a reason for treatment. Many patients adapt to a lack of ideal occlusion and function asymptomatically. It is only when lack of functional ideal is linked to cause and effect that treatment is indicated. The only way to differentiate one from another is to perform a complete exam that evaluates the entire masticatory system.
1. 2D Functional-Esthetic Analysis
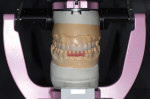
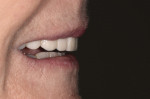
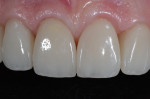
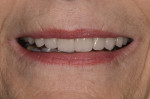
This stage is the foundation of the evaluation process. Bacterial, functional, and esthetic issues are identified, along with possible solutions. Starting with TMJs that are verified as healthy and stable, functional and esthetic corrections are addressed. Five factors of a stable occlusion are analyzed and then smile analysis is completed. The smile analysis begins with a global esthetic analysis and then progresses to macroesthetic principles (Figure 1). Microesthetics are that last esthetic factor that can be communicated between the dentist and ceramist to give teeth a natural appearance.7-9 Form and function go hand in hand, resulting in restorations that are esthetically pleasing and provide the stability needed for functional harmony. Face-bow mounted centric relation articulated models (Figure 2) and a full series of photographs are necessary for the 2D functional-esthetic analysis.
2. 3D Treatment Planning
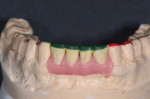
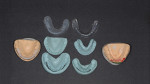
Using the mounted models and the photographs, the visualized 2D solutions are created on the models in wax. This occlusal analysis allows the dentist to evaluate and create solutions on an articulator, which reflects how a patient currently functions. The mounted diagnostic models are done in duplicate, one set to make the desired changes and the other to serve as the unchanged originals. The functional and esthetic changes are made in tooth position, size, and shape, as well as incisal edge position. At this point, the doctor has visualized changes twice, first in the 2D work up and then in 3D diagnostic wax-up (Figure 3 and Figure 4). Despite this work-up, the changes must be verified in the mouth through the use of the provisional prototypes. Treatment guides and stents are utilized for tooth preparation and for creating the provisional prototypes (Figure 5). The 3D treatment plan allows for the creation of a definitive treatment plan. Visualizing ideal care and then communicating this vision to the patient is the key element to case acceptance.
3. Provisional Prototypes
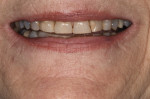
Actual treatment begins in this stage with the diagnostic wax-up being used as a guide for tooth preparation and development of the prototypes. Functional and esthetic corrections are verified with the prototypes in the mouth. This is the only way to truly be sure that the planned changes are correct. If alterations are needed, it is an easy step to make changes while the patients are still in prototypes. Verified prototypes are copied and used by the lab for fabrication of the definitive restorations, further eliminating guesswork. This step also provides the dentist with a means to verify that the lab has accurately reproduced definitive restorations based on the parameters established in the prototypes.10 Not completing this step and rushing to definitive restorations may result in unsatisfactory restorations that may need extensive alteration or may even need to be redone. Predictability comes from following this process along with a series of checklists for each step. This protocol increases the predictability of successful outcomes (Figure 6 through Figure 11).
4. Definitive Restorations
Through approved provisional prototypes, the laboratory and technician now have everything they need to create ideal restorations that are functionally accurate with the best esthetics possible. Cross-mounted models of the prototypes along with photographs allow the lab to create an incisal guide table and an incisal edge matrix. The incisal guide table allows the lab to create lingual contours of the definitive restorations to replicate those of the prototypes that were proven to be accurate. The incisal edge matrix ensures that the maxillary anterior vertical and horizontal position of the prototypes are also replicated in the definitive restorations (Figure 12 and 13).
The Dawson Diagnostic Wizard
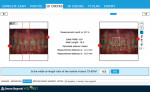
In an effort to make implementing the treatment planning process easier, more predictable, and time efficient, The Dawson Academy created the Diagnostic Wizard. It is a cloud-based program that encompasses the entire process described above, from the complete examination to definitive restorations. It is organized in an easy-to-follow stepwise format and prevents skipping any steps in this systematic treatment planning process. The photographic series is uploaded and auto populated into the Wizard program with just a few keystrokes on the computer, and each photograph is automatically placed into the correct treatment planning step for evaluation. The Dawson Diagnostic Wizard helps the dentist develop an ideal treatment plan in a more timely and efficient manner (Figure 14). It is also a powerful tool for patient case presentation as well as communication with the interdisciplinary team.
Sequencing Treatment
Despite the desire to correct patient’s problems with the least amount of dentistry, often patients present with multiple problems that require extensive dentistry. This type of dentistry can be expensive and may not possible for many patients. Sequencing care and utilizing less expensive interim restorations can create a pathway for a patient to achieve the same successful outcome but over a longer time interval. Definitive restorations can be staged over time on a schedule that works best for the patient. Regardless of whether a patient is able to complete treatment immediately or sequence treatment over time, the process of visualizing a complete treatment plan is the same. Only when that treatment plan is created can the dentist begin to formulate a plan of sequenced care.
Goals of sequenced care include techniques that are readily available to most practitioners, are time efficient in delivery, and can control costs. They are not meant to be replacements for the definitive restorations but rather solutions that will buy time until the definitive restorations can be completed. These interim restorations may be in place for months or in some cases a few years.11
As a general rule, bonded restorations seem to be a better solution when interim restorations may be in place for longer than a few months due to decreased risk of microbial leakage. Cemented restorations are a good option for shorter time periods or when retrievability of the restoration may facilitate interdisciplinary care.12 It is important to remember that the 3D diagnostic wax-up and establishment of the complete treatment plan is an important initial step.
Conclusion
Starting with a complete examination, interpreting the results of that examination, and proceeding through the four stages of complete dentistry allow for predictable outcomes that address the patient’s bacterial, functional and esthetic needs. Treatment plans can be idealized to address the patient’s immediate and deferrable needs as well as provide options for sequenced care. Long-term predictable success is likely when following a proven protocol. Following this process will result in fewer failures, which will save the dentist both time and money. The real benefit is a long-lasting beautiful and functional result for the patient.
References
1. Dawson PE. Functional Occlusion: From TMJ to Smile Design. 1st ed. St. Louis, MO: Mosby; 2007.
2. Christensen GJ. Elective vs mandatory dentistry. J Am Dent Assoc. 2000;131(10):1496-1498.
3. Dawson PE. Position paper regarding diagnosis, management, and treatment of temporomandibular disorders. J Prosthet Dent. 1999;81(2):174-178.
4. McKee JR. Comparing condylar position repeatability for standard verses nonstandardized methods of achieving centric relation. J Prosthet Dent. 1997;77(3):280-284.
5. Williamson EH, Lundquist DO. Anterior guidance: Its effect on electromyographic activity of the temporal and master muscles. J Prosthet Dent. 1983;49(6):816-823.
6. Murphy MT. Improving case acceptance: A new paradigm for treatment plan presentations. J Am Dent Assoc. 2006;137(12):1724-1726.
7. American Academy of Cosmetic Dentistry. AACD guide to accreditation crieteria: Contemporary concepts in smile design. AACD website. www.aacd.com/guides. Accessed June 19, 2015.
8. Rufenacht CR. Fundamentals of Esthetics. Chicago, IL: Quintessence; 1990:77-85.
9. Morley J, Eubank J. Macroesthetic elements of smile design. J Am Dent Assoc. 2001:132(1):39-45.
10. Helvey GA. Provisional material considerations: creating a blueprint of the final restorations. Compend Contin Educ Dent. 2014;35(1):56-60.
11. Lodding DW. Long-term esthetic provisional restorations in dentistry. Curr Opin Cosmet Dent. 1997;4:16-21.
12. Spear F. An interdisciplinary approach to the use of long-term temporary restorations. J Am Dent Assoc. 2009;140(11):1418-1424.