The Hall Technique: Serious Questions Remain
A hard look at the evidence base raises critical concerns
In the past 15 years, a method of treating carious primary molars has emerged in the United Kingdom that has received little attention in the United States. The “Hall Technique,” named for Norna Hall, a Scottish dentist, involves compressing an oversized, cement-filled stainless steel crown form upon a primary molar infected with dental caries, using no local anesthesia, no removal of carious tooth structure, no cutting the crown margins to natural length, and no marginal crimping or finishing, as opposed to the usual stainless steel crown procedure.1 A brochure by the University of Dundee2 documents the Hall Technique extensively. A number of clinical research reports have also given some perceived legitimacy to the method.3-6
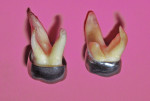
For reference, Figure 1 shows a stainless steel crown form as supplied by the manufacturer (left) and a form adapted for use in the traditional stainless steel crown procedure (right). Figure 2 shows a primary first molar in an unadapted crown form (left) along with an extracted maxillary primary first molar 6 years after it had been restored with a stainless steel crown in the traditional manner (right).
Cause for Concern
There have been several published concerns about the method. Dean questioned the ethics of the method and achieving consent from parents,7 and Nainar pointed out problems with the controls and outcomes assessment in a study by Innes et al5 and questioned the validity and meaningfulness of those findings.8 Now that there has been a study of the technique published in the December 2014 issue of the Journal of the American Dental Association, much more attention has been brought to this method in the United States.6
The measures of success used by the researchers are controversial. Imagine that a research team sets out to test the efficacy of a new skin-tanning device. To measure changes in the skin color of various subjects and judge the success of the equipment, they create a scale of skin color and use standardized before and after photographs for comparison. The research model, however, completely ignores that a risk of skin cancer accompanies treatment results. It is easy to ignore that risk in a published report simply by not mentioning it. One must remember that the darkened skin in question, considered an attractive cosmetic change, is attached to a person, not a research specimen. Likewise, even if a primary molar crown is retained and recorded in the research team’s “success column,” there is still a diseased tooth underneath that crown, and it is attached to a child with an infected mouth who has not been cured.
A clinical “pilot trial” of the Hall technique consisted of a series of questions for children who were treated using the Hall Technique.9 Their parents were also queried. The basis of this “trial” was questions for patients such as, “If you had to have another filling, would you like it done the same way?” and “Was there anything you didn’t like?” Parents were asked, “If your child had to have another filling, would you like it done the same way?”
This subjective “trial” had no controls and did not meet the basic requirements of serious scientific clinical research because it was entirely based on reported opinions and attitudes about the procedure from biased samples (the patients and their parents). One wonders what the parents’ responses would have been had the question read: “If your child had to have another filling, would you like it done the same way even though the tooth decay, which is infected dead and dying tooth structure, was not removed from your child’s tooth and will remain there as long as the crown stays on? Furthermore, do you understand that the research shows the treatment has a one third chance of failing within 5 years?” The results could be compared to asking the subjects of the tanning device trial if they liked the new dark color of their skin, but were still not apprised of the cancer risk.
Due Diligence
With all the above in mind, there are some questions that proponents of the Hall Technique need to answer:
1. What is the medical model for the Hall Technique? Does a surgeon knowingly “wall off” an infected appendix with Gore-Tex® or some other surgically placed barrier and leave the necrotic tissue in situ? In what other circumstances in medical or dental practice did the critical concept of debridement of dead and dying tissue in wound healing become unnecessary?
2. Will normal eruption of a permanent succedaneous tooth be delayed as it engages the overhanging margins of a primary second molar steel crown placed with the Hall Technique, and become at risk for caries? What about the inevitable chronic gingival inflammation associated with over-extended, non-adapted, unfinished stainless steel crown margins?10-12 What, if any, concerns are there about restoring teeth with the Hall Technique for a child at risk for subacute bacterial endocarditis, or for a child who is immunodeficient and requires antibiotic prophylaxis for dental care? A single dose of prophylactic antibiotic before the procedure will not provide long-term protection and this could place such children at risk.
3. When did “no symptoms” become equated with absence of pathosis? Do proponents of the Hall technique believe the caries infection will cease? While sealing off caries has been shown to be successful since the first studies of Handelman,13 it is the seal that is the crucial part of the procedure. Without a Hall crown completely sealing off the caries lesion, a circumstance that is hard to imagine with this technique, the lesion can continue to progress under the crown. At the very least, research should be done to indicate the degree to which crowns seated with the Hall Technique are capable of sealing off caries lesions. The subject of anaerobic pathogens in the infected primary molars has also not been addressed by Hall Technique advocates.
4. Should the measure of “success” in the Hall method be merely crown retention? Should the following not also be considered?
· Pain or discomfort (Dentists who treat children recognize that children are often seen with significant oral disease with no complaints of pain or discomfort).
· Soft tissue pathological alterations.11,12
· Osteomyelitis that could affect development of the underlying succedaneous teeth. (In the 2006 Innes et al study, the writers state under materials and methods, “Radiographs were not routinely taken…”)3 If no periapical or panographic radiographs are recorded for a child whose teeth are to be treated with the Hall Technique, there is no way of knowing if there is a succedaneous tooth forming under the primary molar. If a crown is placed on a primary molar for which there is no permanent successor, that crown may be required to endure for many years, well beyond the typical exfoliation time of the primary molar. Are there any data to support the use of the Hall Technique for treatment of primary molars that will be retained, serving as permanent teeth if there is no successor? Furthermore, in many cases, wouldn’t a conservative adhesively bonded resin-based composite/resin-modified glass-ionomer type of tooth repair be more judicious?
· Other radiographically detectable pathological changes such as internal or external radicular resorption, intraradicular radiolucencies, or ectopic eruption of developing permanent first molars.
· The necessity of additional clinical intervention.
5. What are the short-term and extended histopathological implications of necrotic and necrobiotic tissue left in place within live tissue? Sometimes primary molar stainless steel crowns remain functional for up to 8 years. The mean time for evaluating the 67 crowns in the Ludwig et al6 study is 15 months. Using their own questionable measures of success, Innes et al reported a 73.4% “success rate” after 3 years and 67.6% “success” after 5 years with the method.5 That equates to a 26.6% failure rate after 3 years and 32.4% failures after 5 years. What conscientious dentist would be satisfied with failing to heal an infected child, entrusted to her/his care, a quarter or a third of the time? In reality, the Hall Technique fails to heal a child 100% of the time, if the measure of success is healing, not the tooth remaining in place or the crown being dislodged. Can common sense be trumped by a faulty, artificial, and misleading definition of success? Can research results based on bad definitions be seriously considered “evidence- based?” Can it be that the method is successful in the judgment of the dentist because the treatment is easier for the clinician to accomplish than the proven traditional approach?
6. Would dentists who treat children using the Hall Technique also use it for their own children or young extended family members who develop caries lesions in primary molars? Would they use the method for a child of a dentist, physician, microbiologist, or an attorney?
7. What about ethical, financial, and medico-legal implications of the Hall method? How can a dentist ethically charge or accept a stainless steel crown fee knowing that worthy, proven care for the child not only wasn’t attempted or achieved, but rather was purposely avoided? We recognize that dentists use various means to provide “interim” (ie, “temporary” or “sedative”) restorations for urgent care in certain cases, such as in military settings or emergency care visits. However, the Hall Technique is not characterized by its proponents as “interim,” and there is no separate third-party billing code for crowns placed with this technique.
We cannot imagine third-party dental insurance carriers willing to send payment checks for dentists voluntarily abrogating their responsibility to treat children in a proven, acceptable manner that has been known for more than half a century as the standard of care. How would a dentist explain the Hall Technique when an insurance carrier initiates an audit of patient records? In addition, we wonder how dentists can explain to parents about the inevitable failures when a compromised technique was purposely used knowing that infected tissue was hidden rather than removed prior to crown placement. Medico-legal implications and ethical concerns have yet to be addressed by Hall Technique proponents.
Our Responsibility
We were glad that the Ludwig et al study6 was published, because it exposes the Hall method for scrutiny by dentists in the United States. This is not the first technique, and most assuredly won’t be the last, that was introduced as a way to provide dental treatment in an expedient manner. One recalls the enthusiasm with which the Sargenti endodontic filling method was embraced to make things easier for the dentist. To what end?
We also sincerely hope that publication of the Ludwig et al study and this Viewpoint essay launch a serious soul-searching evaluation of what we do for children, what measures of success we use, and how serious we are about teaching the principles of excellent restorative dentistry in our schools and in the scientific literature of dentistry. It is paramount we remember that attached to that primary molar is an innocent, vulnerable young person whose parents are trusting us to know the science and art of what we are doing, and to do the right thing for their child.
About the Authors
Theodore P. Croll, DDS
Affiliate Professor, Department of Pediatric Dentistry
University of Washington School of Dentistry
Adjunct Professor, Pediatric Dentistry
University of Texas Health Science Center at San Antonio
Private Practice, Pediatric Dentistry
Doylestown, Pennsylvania
Constance M. Killian, DMD
Adjunct Associate Professor of Pediatric Dentistry
University of Pennsylvania
Private Practice, Pediatric Dentistry
Doylestown, Pennsylvania
Richard J. Simonsen, DDS, MS
Dean, College of Dental Medicine
University of Sharjah
United Arab Emirates
References
1. Croll TP. Preformed stainless steel crowns: an update. Compend Contin Educ Dent. 1999;20(2):89-106.
2. The Hall Technique: A minimal intervention, child centred approach to managing the carious primary molar brochure. University of Dundee website. http://dentistry.dundee.ac.uk/sites/dentistry.dundee.ac.uk/files/3M_93C%20HallTechGuide2191110.pdf. Accessed May 22, 2015.
3. Innes NP, Stirrups DR, Evans DJ, et al. A novel technique using preformed metal crowns for managing carious primary molars in general practice - a retrospective analysis. Br Dent J. 2006;200(8):451-454.
4. Innes NP, Evans DJ, Stirrups DR. The Hall Technique; a randomized controlled clinical trial of a novel method of managing carious primary molars in general dental practice: acceptability of the technique and outcomes at 23 months. BMC Oral Health. 2007;7:18.
5. Innes NP, Evans DJ, Stirrups DR. Sealing caries in primary molars: randomized control trial, 5-year results. J Dent Res. 2011;90(12):1405-1410.
6. Ludwig KH, Fontana M, Vinson LA, et al. The success of stainless steel crowns placed with the Hall technique: a retrospective study. J Am Dent Assoc. 2014;145 (12):1248-1253.
7. Dean C. Wholly untested. Br Dent J. 2006;201(2):68-69.
8. Nainar SM. Success of Hall technique crowns questioned. Pediatr Dent. 2012;34(2):103.
9. Evans DJP, Southwick CAP, Foley JI, et al. The Hall technique: a pilot trial of a novel use of preformed metal crowns for managing carious primary teeth. University of Dundee website. www.app.dundee.ac. uk/tuith/Articles/rt03.htm. Accessed May 22, 2015.
10. Croll TP, Epstein DW, Castaldi CR. Marginal adaptation of stainless steel crowns. Pediatr Dent. 2003;25(3):249-252.
11. Webber DL. Gingival health following placement of stainless steel crowns. ASDC J Dent Child. 1974;41(3)186-189.
12. Myers DR. A clinical study of the response of the gingival tissue surrounding stainless steel crowns. ASDC J Dent Child. 1975;42(4):281-284.
13. Handelman SL, Buonocore MG, Heseck DJ. A preliminary report on the effect of fissure sealant on bacteria in dental caries. J Prosthet Dent. 1972;27(4): 390-392.