Optimizing Anterior Implant Pink Esthetics
Creating a custom impression coping with an easy and predictable technique
The final esthetics of an implant restoration in the esthetic zone is dependent not only upon the appearance of the crown, but also equally on the position and appearance of the surrounding gingival tissues. The "pink esthetics," as it is called, is the difference between exquisite results and something merely acceptable.1 Achieving top-notch results requires attention to detail in a three-pronged approach that includes treatment planning, surgical management, and restorative management.
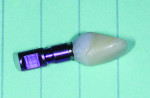
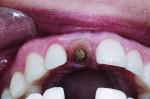
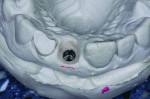
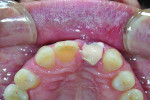
Control of the emergence profile of the abutment—the shape between the head of the fixture and the gingival margin (Figure 1)—finalizes the position of the free gingival margin and papilla. There are many techniques for developing the emergence profile using both custom healing caps (Figure 2) and provisionals.2-5 The author's preference over time has been to use a custom provisional to be able to adjust the emergence profile and watch the tissue response, and also to allow tissue maturation against a shape that encourages optimal soft-tissue esthetics. An initial fixture-level impression (Figure 3) makes it possible to carve the stone (Figure 4) and develop an emergence profile that is a "first guess" at the necessary shape for positioning of the free gingival margin and papilla. Straight or concave facial emergence profiles encourage a more incisal position of the free gingival margin as compared to a convex or facially prominent shape positioning the free gingival margin more apically.6
After the emergence profile of the provisional has been perfected, the next restorative challenge is transferring this key piece of information to the laboratory, where an exact copy of the emergence profile of the provisional can be made. Even slight changes to the shape of the abutment due to tissue slumping during the impression process can cause changes that negatively affect the final esthetics. After trying numerous approaches7-9 and refining them over the years, the author developed the described technique, which works predictably for capturing an accurate soft-tissue impression. Once the emergence profile has been perfected with a provisional restoration and adequate time has elapsed for tissue maturation, the provisional will be used to create a custom impression coping and separate soft-tissue model.
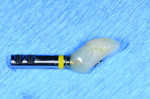
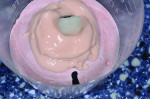
The custom provisional is removed from the patient's mouth, and Mach-2® Die-Silicone (Parkell Inc., www.parkell.com) is injected over the top of the fixture up to the crest of tissue (Figure 5). This does not prevent tissue slumping completely, but it holds the space well enough for the custom impression coping to be seated without blanching or discomfort for the patient. An analog is attached to the custom provisional (Figure 6). Statstone® (Heraeus Kulzer, www.heraeus-kulzer-us.com) is mixed and placed in a plastic pill cup approximately high enough to cover two thirds of the analog. The analog/provisional is then seated into the stone (Figure 7). Once the stone has set, Mach 2 Die Silicone is injected around the top of the analog and over the emergence profile of the provisional, and the facial surface is marked with a sharp permanent marker on the stone for reference (Figure 8). The provisional is then unscrewed and placed in chlorhexidine prior to being reseated in the mouth.
An impression coping is then screwed into the analog in the medicine-cup impression. Flowable composite is injected around the impression coping in the silicone soft-tissue impression in small increments. The author cures after each 1.5 mm layer to ensure the material is adequately polymerized, building up height incisally until reaching the top of the silicone. The facial of the custom impression coping is marked with a sharp permanent marker before being unscrewed from the analog and placed in chlorhexidine (Figure 9).
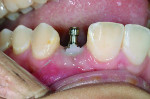
Using an explorer, the author next removes the silicone plug over the fixture intraorally, seats the custom impression coping, and tightens the screw (Figure 10). Full seating is verified with a periapical radiograph. A full-arch final impression that is an exact soft-tissue replica of the mouth is then captured with vinyl polysiloxane impression material.
The custom impression coping—along with the medicine-cup soft-tissue impression and full-arch final impression—is sent to the author's laboratory (Gold Dust Dental Lab, www.golddustdental.com). The laboratory will not need to do any carving of the model to create the soft-tissue shape and can fabricate the emergence profile of the final abutment to exactly duplicate the shape of the provisional. The laboratory uses both the full-arch soft-tissue model and the medicine cup to fabricate the final restoration to duplicate the emergence profile.
The author has tried this same technique with only stone in the medicine cup, which made seating the impression coping challenging and necessitated use of a separating medium prior to placing the flowable. Eliminating the stone and using only silicone, both with heavy-body tray material and bite registration, enabled the analog to spin and move, and there was inadequate accuracy around the provisional to create the impression coping. The combination of stone and a highly flowable, rapid-setting silicone has made this technique easy and predictable.
References
1. Gehrke P, Lobert M, Dhom G. Reproducibility of the pink esthetic score--rating soft tissue esthetics around single-implant restorations with regard to dental observer specialization. J Esthet Restor Dent. 2008;20(6):375-384.
2. Bain CA, Weisgold AS. Customized emergence profile in the implant crown--a new technique. Compend Contin Educ Dent. 1997;18(1):41-45; quiz 46.
3. Azer SS. A simplified technique for creating a customized gingival emergence profile for implant-supported crowns. J Prosthodont. 2010;19(6):497-501.
4. Stumpel LJ, Haechler W, Bedrossian E. Customized abutments to shape and transfer peri-implant soft-tissue contours. J Calif Dent Assoc. 2000;28(4):301-309.
5. Neale D, Chee WW. Development of implant soft tissue emergence profile: a technique. J Prosthet Dent. 1994;71(4):364-368.
6. Son MK, Jang HS. Gingival recontouring by provisional implant restoration for optimal emergence profile: report of two cases. J Periodontal Implant Sci. 2011;41(6):302–308.
7. Elian N, Tabourian G, Jalbout ZN, et al. Accurate transfer of peri-implant soft tissue emergence profile from the provisional crown to the final prosthesis using an emergence profile cast. J Esthet Restor Dent. 2007;19(6):306-314; discussion 315.
8. Ntounis A, Petropoulou A. A technique for managing and accurate registration of periimplant soft tissues. J Prosthet Dent. 2010;104(4):276-279.
9.Paranhos KS, Oliveira R. An impression technique to accurately transfer soft tissue contours for implant-supported restorations: three case reports. J Oral Implantol. 2001;27(6):317-321.
Learn this technique hands-on at:
Clinical Mastery Series
480-489-5551
www.clinicalmastery.com
About the Author
Lee Ann Brady, DMD
Director of Education,
Clinical Mastery Series
Editorial Board,
Journal of Cosmetic Dentistry
Founder of www.leeannbrady.com
Private Practice
Glendale, Arizona