Ideal Restoration of Proximal Contacts in Complex Class II Lesions
A successive composite reconstruction technique with careful G-ring selection
Direct posterior composite restorations are a routine procedure in dental practices all over the world. Even though many improvements have been made in restorative materials and different techniques have been tested, Class II restorations are still not successful long term. In complex Class II cases, it is difficult for the clinician to restore the proximal contacts to ideal contour and tightness. In this clinical report, the authors present a technique that combines the successive composite reconstruction technique and the use of two G-rings with different ring tine lengths so that neighboring teeth with approximated proximal boxes can be restored successfully in one clinical appointment.
Background
Improvements in the physical properties of resin composite and advances in enamel and dentin bonding have made clinical use of these materials routine. Nonetheless, amalgam restorations are still used successfully in posterior teeth and are indicated for complex Class II restorations because amalgam can be effectively condensed against a traditional matrix band to recreate proximal contacts.1
One of the greatest challenges encountered by even the most experienced clinicians when placing Class II resin composite restorations is creating tight proximal contacts and obtaining anatomically correct proximal contours.2 To achieve a predictable result, dentists must overcome challenges, including the thickness and elastic displacement of the Tofflemire matrix bands,3,4 polymerization shrinkage, and the lack of condensability of composite resin materials.4,5 Research has shown that pre-contoured matrix bands in combination with a separating ring achieve superior contours when compared to flat matrix bands.3,6-8 Through in vitro and in vivo studies, sectional matrix systems and rings have proven to generate proximal contacts with a reliable tightness due to the interdental separation the ring generates during the restorative procedure.9,10 The various sectional matrix systems now available on the market differ mainly in the height, width, and shape of the ring tines, which makes it difficult for one system to work on all clinical cases. The selection of the ideal system should be made according to the bucco-lingual width of the proximal box. Horizontal (bulk) and oblique (layered) restorative techniques have been developed for the restoration of posterior teeth. The greatest advantage of the layered technique is that minimal shrinkage takes place within each increment because of a low C-factor, as the large free surface permits the resin to flow during polymerization.11 This is important to consider at the time of reconstruction of the proximal wall in a Class II preparation, because a high C-factor can lead to an open margin at the base of the box and lead to the imminent failure of the restoration.
Case Presentation
A 25-year-old woman complaining of gingival inflammation and difficulty in flossing between teeth Nos. 4 and 5 presented to the clinic. After her medical history was reviewed, she was determined to be healthy and low risk for treatment (ASA I classification). Intraoral and radiographic examination revealed the presence of defective restorations, including an occlusal restoration on tooth No. 4 with a cavitated carious lesion that extended into dentin (ICDAS code 5) on its mesial surface and an occlusal distal restoration on tooth No. 5 with an over-contoured proximal wall. Periodontal examination revealed bleeding upon probing with normal sulcus depth.
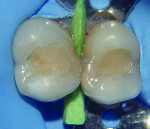
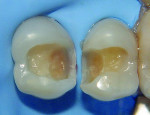
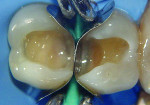
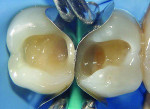
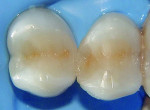
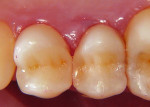
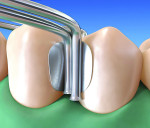
The patient was offered direct and indirect restorative options. The advantages and disadvantages of each option were discussed, and a decision was made based on time and economic factors. After local anesthesia, rubber dam isolation, and pre-wedging was achieved (Figure 1), the existing restoration was removed using a high-speed handpiece and a #4 round carbide bur under constant water cooling. Infected dentin was removed using #2 and #4 round carbide burs on a slow-speed handpiece under water irrigation to prevent increase in pulp temperature and possible pulpal insult. Finished cavity preparations with rounded internal line angles, occlusal cavosurface margins with no bevel, and margins on enamel can be seen in Figure 2.
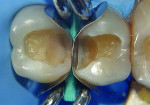
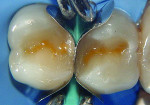
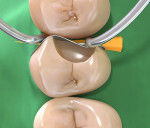
After placement of a new rubber dam (the first one was torn while placing the wedge), two pre-contoured sectional bands (Composi-Tight® Sectional Matrix System, Garrison Dental, www.garrisondental.com) were placed and secured by a wooden wedge (Hawe Sycamore Interdental Wedges, Kerr Corp., www.kerrdental.eu) followed by two G-rings (Garrison Dental) with different tine lengths (Figure 3) so that one ring was on top of the other and both preparations could be restored at the same time. This technique and matrix system will ensure that adequate proximal contours and embrasures are achieved.
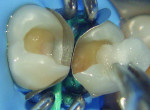
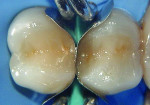
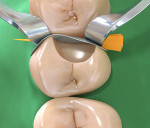
Enamel and dentin were acid etched with 35% phosphoric acid (Scotchbond™ Echtant, 3M ESPE, www.3mespe.com) for 15 seconds. The acid etchant was then rinsed for 30 seconds, gently air dried, and 2% chlorhexidine gluconate Cavity Cleanser™ (BISCO, www.bisco.com) was used for 60 seconds (Figure 4). Two coats of a one-bottle adhesive system (Adper™ Single Bond 2, 3M ESPE) was placed until a uniform layer covered the preparation. A gentle stream of air was applied for approximately 15 seconds to help remove the solvent from the adhesive, which was then light-cured for 20 seconds (Figure 5). A nano-filled A3 body shade composite resin (Filtek™ Z-350, 3M ESPE) was inserted using a technique called successive composite reconstruction,12 starting with the proximal walls of both preparations (Figure 6). Using an incremental composite placement technique to restore these walls results in less volumetric shrinkage because the number of free walls results in less stress buildup during polymerization. Using the same technique, the occlusal portion was also restored; small amounts of composite were layered and light cured incrementally to reconstruct the anatomical forms up to the dentino-enamel junction.
Ochre color intensifier (Tetric®, Ivoclar Vivadent, www.ivoclarvivadent.com) was placed in the central fossa using a #15 endodontic file to create a feeling of depth (Figure 7). A final layer of A3 body shade composite was placed and light cured for 40 seconds (Figure 8). Excess adhesive and composite were removed from proximal areas using thin sand paper strips (Sof-Lex™ finishing strips, 3M ESPE) and a #12 surgical blade (Figure 9). Occlusal anatomy was enhanced using a #OS3 12 blade carbide (Brasseler, www.brasselerusa.com). Minor occlusal adjustments were made as needed (Figure 10).
Discussion
Complex Class II composite restorations present many challenges during clinical procedure. The longevity of these restorations can be compromised by polymerization shrinkage at the resin-tooth interface of the proximal box and the lack of tight and anatomical proximal contacts. This clinical report illustrates a predictable technique to help dentists overcome these common problems.
Pre-wedging is an important step in creating separation between adjacent teeth, as it will help in preventing iatrogenic damage to the neighboring tooth during the preparation phase. The selection of the correct G-ring design is also an important step when restoring a large Class II preparation. Smaller diameter G-rings may impede on the matrix as the bucco-lingual width of the proximal box increases (Figure 11). In this case, a wider flat G-ring is more appropriate, as a portion of the broader flat tine is able to engage tooth structure properly, thus preventing the tine from encroaching on the matrix (Figure 12).
In the clinical case presented, the bucco-lingual width of the proximal boxes had completely eliminated the contact areas between adjacent teeth. This lack of tooth-to-tooth contact presented more of a challenge, as it can be difficult to generate enough pressure with the wedge to compensate for the thickness of both matrices. G-rings have been found to generate enough pressure, but the correct G-ring design selection is important when restoring two neighboring teeth with proximal boxes facing one another. By having two G-rings with different tine lengths, they can fit on top of each other without displacing one another (Figure 13). They will also exert mesial and distal pressures, respectively, and thereby assist the wedge in compensating for the thickness of the matrices. The wedge also displaces the interdental papilla apically as well as seating the matrices more intimately with the adjacent teeth. This method of isolation affords the operator a clearer view of the composite/tooth interface at the gingival wall of the box. Starting the restorative procedure in the proximal box using an incremental technique like the successive composite recontruction reduces the effects of polymerization shrinkage and creates a favorable bonded-to-unbonded wall ratio, thus reducing the C-factor. The final anatomical contours and contact tightness were enough to eliminate the patient’s chief complaint and the surrounding tissues returned to normal health in a few days.
References
1. Cho SD, Browning WD, Walton KS. Clinical use of a sectional matrix and ring. Oper Dent. 2010;35(5):587-591.
2. Saber MH, Loomans BA, El Zohairy A, et al. Evaluation of proximal contact tightness of Class II resin composite restorations. Oper Dent. 2010;35(1):37-43.
3. Loomans BA, Opdam NJ, Roeters FJ, et al. The long-term effect of a composite resin restoration on proximal contact tightness. J Dent. 2007;35(2):104-108.
4. Keogh TP, Bertolotti RL. Creating tight, anatomically correct interproximal contacts. Dent Clin North Am. 2001;45(1):83-102.
5. El- Badrawy WA, Leung BW, El Mowafy O, et al. Evaluation of proximal contacts of posterior composite restorations with 4 placement techniques. J Can Dent Assoc. 2003;69(3):162-167.
6. Dörfer CE, Steinhausen J, Staehle HJ. Messung approximaler kontaktstärken von komposit- und amalgamfüllungen im seitenzahnbereich in vitro. Deutsche Zahnsctzliche Zeitschrift. 1996;51:335-338.
7. Loomans BA, Roeters FJ, Opdam NJ, Kuijs RH. The effect of proximal contour on marginal ridge fracture of Class II composite resin restorations. J Dent. 2008;36(10):828-832.
8. Loomans BA, Opdam NJ, Roeters JF, et al. Influence of composite resin consistency and placement technique on proximal contact tightness of Class II restorations. J Adhes Dent. 2006;8(5):305-310.
9. Peumans M, Van Meerbeek B, Asscherickx K, et al. Do condensable composites help to achieve better proximal contacts? Dent Mater. 2001;17(6):533-541.
10. Loomans BA, Opdam NJ, Roeters JF, et al. A ramdomized clinical trial on proximal contacts of posterior composites. J Dent. 2006;34(4):292-297.
11. Yoshikawa T, Sano H, Burrow MF, et al. Effects of dentin depth and cavity configuration on bond strength. J Dent Res. 1999;78(4):898-905.
About the Authors