Direct Composite and Finishing/Polishing Systems for Esthetic Anterior Restorations
Selecting complementary materials for freehand restorative work in the esthetic zone
Placing direct composite restorations in the anterior region requires build-up steps similar to those for fabricating a layered ceramic restoration that will replace dentin, enamel, dentin lobes, and characteristic colors. Mastering direct composite build-up techniques enables dentists to create lifelike restorations based on their artistic abilities and imagination. This is especially true when undertaking the procedure using freehand bonding methods.
Direct restorations require knowledge of and astute attention to the various optical and anatomic variances of natural teeth. For clinicians to create an accurate reproduction of a natural tooth, they must layer composite materials of different opacities to replicate the tooth structure that was either removed during preparation or lost as a result of disease or trauma.1 Realistic direct composite restorations can only be achieved through a combination of correct anatomic form and creative color layering concepts.2
Creating Proper Esthetics
To build a direct restoration, a detailed shade diagram is developed. Then teeth are minimally prepared and etched, after which an appropriate bonding agent is applied, and composite is incrementally layered, contoured, and light cured. After all increments have been placed and cured, the restoration is then finished and polished.3
Imperative to this process is using and properly handling materials that interplay with light and recreate the hues, chromas, and values inherent in the natural tooth structure being replaced.4 Whether on facial, cervical, or interproximal surfaces, the manner in which composite materials are handled influences the ultimate appearance of composite restorations.3,5
Precise and appropriate composite placement facilitates esthetic recreation of adjacent tooth characteristics, in addition to contributing to the finishing and polishing process.3,6 After composite restorations have been anatomically layered, the finishing and polishing sequences then allow dentists to achieve harmony and balance in terms of facial contours, texture, and tertiary anatomy.6 For example, line angles, secondary anatomy, and tertiary anatomy can be more well defined using a logical, sequential, and predictable finishing and polishing method.3 This will ultimately enable dentists to produce restoration surfaces that accept and reflect light, without voids, defects, stains, or pits.3
Equally significant, when dentists incorporate a finishing and polishing system into their protocol that graduates from coarse to fine discs—as well as includes a variety of tools that complement the chemistry of the selected composite—the final restorations can demonstrate the desired luster and polish. Such systems should include finishing discs, polishing paste, points, cups, and wheels.3
This article demonstrates the manner in which a freehand composite placement technique was used to restore severely damaged anterior maxillary central incisors. A simplified composite system with an advanced filler technology was selected based on its bioactive benefits, optical properties, esthetics, and ideal handling. Additionally, the finishing and polishing protocol necessary to complete the restorations to the desired outcome are demonstrated.
Case Presentation
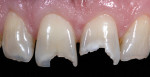
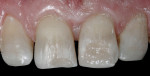
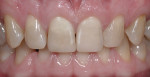
A 42-year-old woman presented with severe destruction of her maxillary central incisors from long-time biologic damage due to sugar and soda consumption, as well as disease. She would not smile, and she cried emotionally with embarrassment about how she presented herself to the world (Figure 1).
During a comprehensive examination, repairing the damaged teeth was correlated to restorative materials, since successful esthetic and functional outcomes in restorative dentistry require envisioning the restorations prior to initiating treatment.3,7 By first envisioning the direct composite restoration in the mind, it could then be created in the patient’s mouth.
In this case, an indirect restoration was not indicated. Rather, the dentist discussed how the patient’s teeth could be restored easily with direct composite restorations based on her expectations. These included restorations that resembled natural teeth and would be reversible and cost-effectively repairable. Advantages of direct composite restorations also included future options for more durable indirect restorations should conditions in her oral cavity worsen.
Based on an esthetic evaluation of the patient’s teeth, it was determined that an uncomplicated palette of nano-hybrid composite (Beautifil® II, Shofu Dental Corporation, www.shofu.com) could be used. This fluoride-releasing and recharging composite features enhanced thixotropic properties for excellent marginal adaptation and efficient contouring without slumping or sticking. Additionally, the composite’s “Giomer” chemistry and surface pre-reacted glass technology (ie, S-PRG filler particles) could be clinically beneficial to the patient given the acidic nature of her oral environment. These fillers uniquely release six ions (ie, fluoride, sodium, strontium, aluminum, silicate, and borate), all of which are known to demonstrate bioactive properties. These fillers have been shown to inhibit plaque formation and neutralize acid for a stable oral pH.8
The material’s high flexural strength of 130 MPa, whether placed in the anterior or posterior region, was also ideal for this case for long-term functional stability in the oral environment. Long-term clinical stability and resistance to wear of posterior teeth also were material characteristics beneficial for this case.8
The patient’s teeth demonstrated some translucency and not much high value with fairly medium chroma. The hallmarks of the case would be light reflection zones on the mesial transition line angles, as well as creating the incisal and distal edges. There would be some light transitions and depth of color in the restorations, but not a very complicated color scheme.
The universal shades in the selected composite system enabled straightforward use and excellent shade reproduction with a chameleon effect by simulating the internal structure of the patient’s natural teeth. The composite provided appropriate depth of color without being overly opaque and also produced appropriate light transmission and optical characteristics. The moderate translucency and light transmission of enamel, combined with the light-diffusion of dentin, would demonstrate predictable esthetics. Additionally, the composite exhibits shade stability prior to and following curing.
Freehand Composite Placement
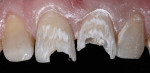
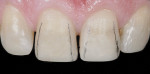
The teeth were prepared with a very conservative, minimally invasive design, with only unsupported enamel removed (Figure 2). A starburst bevel was created and incorporated into the long bevels using a staccato approach.3 This enabled more hydroxyapatite to be incorporated into the restoration, helping to create the illusion of imperceptible color blending.
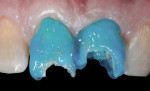
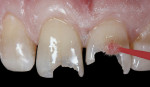
The preparations were etched with phosphoric acid using a total-etch technique (Figure 3), rinsed, and dried. A bonding agent was then carefully applied (Figure 4) and light cured for 10 seconds with an LED curing light.
The first increment of deeper colored composite (ie, shade A3) was placed to block any unsupported enamel in the preparation design. This facilitated an imperceptible blend with the final contour composite layer (Figure 5). This composite is not recommended for placement in increments thicker than 2 mm. This layer was light cured for 10 seconds in a fanning motion with an LED curing light according to the manufacturer’s instructions.
Shade A2 composite was then placed in a striated fashion to demonstrate abstract undulations that would diffuse light rather than reflect it (Figure 6). This also was blended and light cured for 10 seconds with an LED light source.
The third and final composite layer placed was shade A1, which was blended on top of the A3 and A2 composite layers and light cured for 10 seconds in a fanning motion. This resulted in a uni-body, monoblock construction of the restorations’ anatomy (Figure 7).
The decision was made to open the embrasure between teeth No. 8 and No. 9, since the patient desired a natural appearance. Further, closing the diastema and midline would have resulted in disharmony with the adjacent teeth No. 7 and No. 10 (Figure 8).
Finishing and Polishing
An artisan’s approach was taken to prepare the restoration surfaces during the finishing and polishing sequence. A system of discs, polishers, points, and cups with decreasing coarseness (Super-Snap®, Dura-Green stone, Dura-White stone, T & F Hybrid Points®, Direct Dia Polishing Paste, and Super-Snap® Superbuff® Discs, Shofu Dental Corporation) was used to create a unified surface free of voids, imperfections, and signs of delamination between layers.
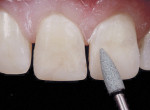
The primary anatomy was redefined by marking the mesial/distal triangular transitional line angles with pencil lines. Then, green discs (Fine Super-Snap) were used to create the secondary anatomy (Figure 9). Slight concavities were created in the interproximal embrasures to prevent light reflection. In particular, a green stone (Dura-Green Stone) was used in areas of the restorations where light-diffusing zones were needed.
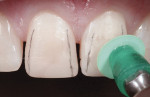
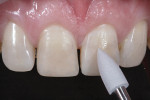
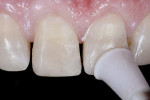
Other components of the finishing and polishing system were employed to create higher luster for light-reflecting zones (Figure 10). The transitional line angles, certain aspects of micromorphology, and the center third of tooth No. 9 (Figure 11) were properly managed and optimized to best mimic the characteristics of the adjacent teeth. Using water spray and very low torque, larger volumes of composite material were then carefully and lightly buffed (Figure 12).
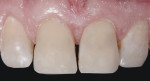
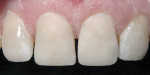
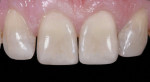
The proper value of the adjacent teeth was achieved in the restorations; today, value is the most important determinant of the shade selection in esthetics. The primary outline, which was very realistic, resulted from not closing the diastema or midline (Figure 13). The light reflection patterns necessary to create the illusion of natural esthetics also were achieved (Figure 14), as demonstrated by the three composite shades mirroring the appearance of teeth No. 7 and No. 10.
Conclusion
In this case, the dentist employed freehand composite placement techniques, in which concepts of “polyrhythmic abstractionist art” were incorporated. This artistic style incorporates many textures and visual sensations without following a model. Rather, the brain is used intuitively to guide color and form throughout the process, helping the final composition to come together. A simple, three-composite buildup was used based on a vision of what the final esthetic result should represent. Because of the uncomplicated nature of the universal composite system selected, no pre-planning or shade mockup was required. Additionally, due to the dentist’s experienced knowledge of and skills with the fundamentals of composite placement, the restorations could be completed freehand, without the use of putty stents.
The patient was very pleased with the esthetic results and could not believe that her smile could look that way following so many years of destruction. During a follow-up appointment, she commented that the restorations had added value to her personal life. She had confidence to present herself to the world. Rather than disguise her smile, she smiled in a natural way.
Of paramount importance to creating a natural-appearing smile were the finishing and polishing sequence and related armamentarium. All of the components necessary for establishing macro and micro esthetics (eg, discs, stones, mini buffers, buff discs, polishing paste) were available and used. Selecting complementary systems of composite and finishing/polishing tools facilitated the predictable creation of esthetic and functional anterior restorations.
Disclosure
Frank Milnar, DDS, AAACD, received material support from Shofu Dental Corporation.
References
1. Blank JT. Simplified techniques for the placement of stratified polychromatic anterior and posterior direct composite restorations. Compend Contin Educ Dent. 2003;24(2 suppl):S19-S25.
2. Terry DA. Restoring the incisal edge. NY State Dent . 2005;71(5):30-35.
3. LeSage B, Milnar F, Wohlberg J. Achieving the epitome of composite art: creating natural tooth esthetics, texture, and anatomy using appropriate preparation and layering techniques. Journal of Cosmetic Dentistry. 2008;24(3):42-51.
4. Jackson RD. Understanding the characteristics of naturally shaded composite resins. Pract Proced Aesthet Dent. 2003;15(8):577-585.
5. Terry DA, Leinfelder KF. An integration of composite resin with natural tooth structure: the Class IV restoration. Pract Proced Aesthet Dent. 2004;16(3):235-242.
6. Peyton JH. Finishing and polishing techniques: direct composite resin restorations. Pract Proced Aesthet Dent. 2004;16(4):293-298.
7. Small BW. Pretreatment wax-ups and provisionals for restorative dentistry. Gen Dent. 2005;53(2):98-100.
8. Gordan VV, Mondragon E, Watson RE, et al. A clinical evaluation of a self-etching primer and a giomer restorative material: results at eight years. J Am Dent Assoc. 2007;138(5):621-627.
About the Author
Frank Milnar, DDS, AAACD
Private Practice
St. Paul, Minnesota