BruxZir® Solid Zirconia Meets an Anterior Esthetic Challenge
Improvements in translucency create lifelike restorations
This article illustrates recent advancements by Glidewell Laboratories to improve the esthetic properties of BruxZir® Solid Zirconia (www.glidewelldental.com) restorations. As the lab’s research & development department refines its processes, improving the material’s translucency, the esthetics continues to improve.
First Appointment
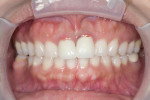
This case will showcase the replacement of porcelain-fused-to-metal (PFM) crowns on tooth No. 8 and No. 9 (Figure 1) with BruxZir Solid Zirconia crowns.
First, the clinician took the shade using the VITA Easyshade® Compact (Vident, https://vident.com), which displays the shade in both VITA Classical and VITA 3D-Master® shades. Next, he compared the selected 2M1 3D-Master shade tab to the tooth, along with the 1M1 3D-Master shade tab for contrast.
Photographs of the shade tabs in the mouth were then taken. Next, the clinician used an Ultradent syringe (www.ultradent.com) to place PFG gel (Steven’s Pharmacy, www.stevensrx.com) into the sulcus of tooth No. 8 and No. 9. The STA Single Tooth Anesthesia System® device (Milestone Scientific, www.milestonescientific.com) was then used to anesthetize tooth No. 8 and No. 9.
Razor® Carbide burs (Axis Dental, www.axisdental.com) can be used for both porcelain and metal substructures. In this case, the burs were used in combination with KaVo’s ELECTROtorque handpiece (www.kavousa.com) to easily cut through the existing PFM restorations. The crowns were then torqued with a Christensen Crown Remover (Hu-Friedy, www.hu-friedy.com).
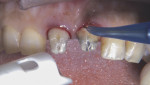
After using a periodontal probe to ensure there was enough biologic width to safely remove some tissue (Figure 2), the NV MicroLaser™ (Zila, www.zila.com) was used to remove 1.5 mm of tissue. With the margins exposed, an 856-025 bur (Axis Dental) and ELECTROtorque handpiece were used to drop the margins to the new gingival level.
The assistant relined BioTemps® Provisionals (Glidewell Laboratories) on tooth No. 8 and No. 9 with Luxatemp® provisional material (DMG America, www.dmg-america.com). Using a thin, perforated diamond disc (Axis Dental), the gingival embrasures were opened to avoid blunting the interproximal papilla and to ensure that the gingival margins were not overextended and the emergence profile was flat. TempBond® Clear™ (Kerr, www.kerrdental.com,) was used to cement the BioTemps provisionals, and loupes were used to inspect around the temporaries and gingival embrasures for excess cement.
Second Appointment
After 2 weeks, the clinician removed the temporaries and cleaned the preparations with a KaVo SONICflex scaler. After trimming the gingival margin with the diode laser, an Ultrapak® cord #00 (Ultradent) was placed and the cord was cut intraorally on the lingual to avoid any overlap. A second cord (Ultrapak cord #2E) was then placed before refining the preparation.
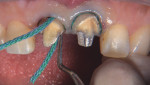
As the clinician packed the top #2E cord on tooth No. 8, the top cord on tooth No. 9 exposed the margin (Figure 3). Finishing the preparations then commenced using a fine-grit 856-025 bur.
Two moistened ROEKO Comprecap Anatomic compression caps (Coltène Group, www.coltene.com) were placed on the preps, and the patient bit down with medium pressure for 8 to 10 minutes. The Comprecaps were removed and the top cords pulled. Medium-body impression material was syringed around the preparations for the impression, and a bite registration was taken. The temporaries were then replaced.
Third Appointment
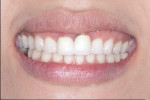
After 2 weeks, the temporaries were removed and the BruxZir crowns were approved. The clinician placed a layer of desensitizer on the teeth (G5™ All-Purpose Desensitizer, Clinician’s Choice, www.clinicianschoice.com). A Warm Air Tooth Dryer (A-dec, https://us.a-dec.com) was used after applying both coats of the G5 while the assistant placed Z-PRIME™ Plus (Bisco) inside the crowns. The crowns were then loaded with a resin-modified glass ionomer cement (RelyX™ Luting Plus Automix, 3M ESPE, www.3mespe.com) and seated using a pinewood stick (Almore International, www.almore.com) to ensure that they are fully seated and the same length (Figure 4).
Final Thought
In this case, a patient with unesthetic anterior PFM restorations experienced an excellent clinical outcome with solid zirconia BruxZir crowns. Although this solution might not work for every case, clinicians may want to consider using BruxZir crowns for patients with parafunctional habits or old PFM restorations, where an esthetic improvement is essentially guaranteed.
For more information contact:
Glidewell Laboratories
800-854-7256
www.glidewelldental.com